01 July 2022: Articles 
Adalimumab Mitigates Lumbar Radiculopathy in a Case of Ankylosing Spondylitis
Challenging differential diagnosis, Unusual or unexpected effect of treatment, Rare coexistence of disease or pathology
Trevor Persaud1ABCDEFG*, Richard MorganDOI: 10.12659/AJCR.936600
Am J Case Rep 2022; 23:e936600
Abstract
BACKGROUND: Ankylosing spondylitis (AS) is an immune-mediated chronic inflammatory condition grouped under spondyloarthritis (SpA), which is an umbrella term for a group of interrelated inflammatory rheumatic conditions with characteristic radiographic findings such as erosions and ankylosis of the sacroiliac joint. Unfortunately, there is an average delay of 8-9 years between the onset of the symptoms and diagnosis due to infrequent consideration of this disease in the differential diagnosis of patients with low back pain and unusual or incomplete presenting clinical symptoms.
CASE REPORT: We describe the case of a 37-year-old male patient with no significant past medical history and surgical history of bilateral hip arthroplasty secondary to idiopathic aseptic necrosis of the bilateral femoral head and bilateral rotator cuff repaired surgery due to multiple motor vehicle accidents (MVA) with a chief concern of chronic low back pain. In this case of ankylosing spondylitis presenting with low back pain and radicular symptoms, his symptoms were resistant to multiple opioid medications, trigger point injections, and epidural steroid injections. Initiation of adalimumab subsequently relieved the patient’s symptoms and restored his ability to perform daily activities.
CONCLUSIONS: This is an unusual presentation of AS with radiographic evidence of bilateral sacroiliitis. The neurological manifestations in AS are not uncommon, and they can occur during the quiescent stage of the disease. It should be emphasized that early diagnosis is essential to prevent progression of the disease and avoid unnecessary treatment for the patient.
Keywords: adalimumab, HLA-B27 Antigen, radiculopathy, sacroiliitis, Spondylitis, Ankylosing, Accidents, Traffic, Adult, Humans, Low Back Pain, Male
Background
Ankylosing spondylitis (AS) is an immune-mediated chronic inflammatory condition grouped under spondyloarthritis (SpA) with a prevalence of 0.1% to 1.4% worldwide, and males are affected more frequently than females [1,2]. Spondyloarthritis (SpA) is an umbrella term for a group of interrelated inflammatory rheumatic conditions that include sacroiliitis, spondylitis, peripheral arthritis, enthesitis, dactylitis, acute anterior uveitis, associated psoriasis or inflammatory bowel disease, presence of HLA-B27, and no association with rheumatoid factor [3]. The SpA can be subdivided into axial SpA or ankylosing spondylitis (predominant symptoms of spine and sacroiliac joints) and peripheral SpA (predominant symptoms of peripheral arthritis, enthesitis, and or dactylitis) [3,4].
An early diagnosis of AS is critical because effective treatments are available, and they are more efficacious if used in the early stage of the disease [5–7]. Back pain is also the first symptom and most frequent manifestation in the AS [7,8]. Additionally, bilateral sacroiliitis is the hallmark of AS, and detecting radio-graphic sacroiliitis is pivotal for diagnosing AS [9,10]. Moreover, SpA accounts for only about 5% of chronic back pain, which is an extremely frequent symptom in pain management facilities and is widespread in the general population [11,12]. Therefore, subsequent referral to the rheumatologist of those patients with back pain with a higher probability of AS is needed to effectively rule out the disease.
To the best of our knowledge, an L4–5 nerve root radiculopathy associated with AS has not been previously reported. Increased suspicion may lead to earlier diagnosis and treatment, potentially reducing the duration of the symptoms and improving the functional ability of patient with AS.
Case Report
We present the case of a 37-year-old male patient with no significant PMH and a past surgical history of bilateral hip arthroplasty secondary to idiopathic aseptic necrosis of the bilateral femoral head and bilateral rotator cuff repaired surgery due to multiple motor vehicle accidents (MVA).
He came to our clinic for occasional low back pain in early 2018. Initially, he rated the pain as an 8 out of 10 on the numerical rating scale (NRS). It was described as a constant, aching sensation that radiated from his lower back to both feet with associated stiffness, numbness, and tingling in his feet. His pain was mostly concentrated in his lower back and gluteal regions. The intensity of his pain was more significant in the morning and when a posture was maintained for a prolonged duration.
On the initial visit, the physical examination elicited that the patient had limited thoracic and lumbar spinal range of motion throughout the sagittal and coronal planes, most apparent on the left side. As for the special test, the FABER test was positive on the left side, the straight leg raise was negative, and the Schober test was positive (Lumbar flexion difference is 4 cm). There were bilateral lumbar paraspinal spasms. Muscle strength, light touch, sensations, tactile discrimination, and deep tendon reflexes were normal in all extremities (Table 1). His complete blood count, complete metabolic panel, other antibody tests and inflammatory markers were within the reference ranges except for a mildly elevated total complement level and low hemoglobin level (Table 2).
On magnetic resonance imaging (MRI), there was evidence of an L4–5 mild broad-based disc bulge with superimposed small central disc protrusion/herniation and traced bilateral facet joint effusions along with sclerosis, joint space narrowing, and erosions of bilateral sacroiliac joints (Figures 1, 2). In addition, electromyography (EMG) was abnormal for chronic left L5 motor radiculopathy with signs of healing, but the nerve conduction studies were normal (Table 3). Therefore, a diagnosis of lumbar radiculopathy was corroborated based on clinical features, MRI findings, and EMG report.
Over the course of three and a half years, the patient had inadequate pain relief with multiple NSAIDs, pain medications (Oxycontin and Percocet), tizanidine, multiple sessions of osteopathic manipulative treatment (OMT), Physical therapy (PT), and multiple trigger point injections. He also underwent one left Intralaminar lumbar epidural steroid injection (L4/5) with 1-month relief of low back pain and resolution of radiating left leg pain and three bilateral SI joint injections, which provided >50% improvement in his low back pain for 2–3 weeks. In Feb 2021, while the patient was waiting for the insurance approval for another intralaminar L4–5 lumbar epidural steroid injection, he developed bilateral eye redness and pain. At this point, point, we considered his clinical symptoms to be an unusual presentation of AS possibly, and he was referred to an ophthalmologist and a rheumatologist, where he was diagnosed with AS. Adalimumab was initiated, and the patient experienced gradual improvement in his low back pain, radicular lower legs pain, and bilateral SI joints pain, with reduced need of pain medications. In a follow-up visit one month after initiating adalimumab, he rated his lower back and bilateral SI joint pain as 3–4/10 on the NRS. As a result, he could return to work and resume many of his activities.
Discussion
LIMITATIONS OF THE STUDY:
We aimed to present the unusual presentation of AS with lumbar radiculopathy signs and symptoms. However, there are limitations of our study: (1) the patient had previous multiple accidents that could contribute to the lumbar disc bulging, and (2) he should have had follow-up blood work to monitor complement level and MRI imaging to identify the improvement of radiographic sacroiliitis after initiation of adalimumab.
Conclusions
Current evidence demonstrates the beneficial effects of TNF inhibitor (adalimumab) in AS patient with symptoms of radiculopathy. It provides sustained clinical remission with the restoration of normal physical activities. Young patients with chronic worsening low back pain with symptoms of radiculopathy, reduced spine mobility, and minimal relief from opioid medications and epidural steroid injection should be referred to a rheumatologist to rule out AS. HLA-B27 is not a diagnostic feature for AS, and diagnostic delay can lead to unnecessary treatment, with poor quality of life, worse functional impairment, and more significant radiographic progression [40]. As such, physicians should be aware of the features of inflammatory low back pain.
References:
1.. Stolwijk C, Boonen A, van Tubergen A, Reveille JD, Epidemiology of spondyloarthritis: Rheum Dis Clin North Am, 2012; 38(3); 441
2.. Akkoç N, Yarkan H, Kenar G, Khan MA, Ankylosing spondylitis: HLAB*27-positive versus HLA-B*27-negative disease: Curr Rheumatol Rep, 2017; 19(5); 26
3.. Poddubnyy D, Rudwaleit M, Early spondyloarthritis: Rheum Dis Clin North Am, 2012; 38(2); 387-403
4.. Østergaard M, Lambert RGW, Imaging in ankylosing spondylitis: Ther Adv Musculoskelet Dis, 2012; 4(4); 301-11
5.. Braun J, van den Berg R, Baraliakos X, 2010 update of the ASAS/ EULAR recommendations for the management of ankylosing spondylitis: Ann Rheum Dis, 2011; 70(6); 896-904
6.. van der Heijde D, Sieper J, Maksymowych WP, 2010 Update of the international ASAS recommendations for the use of anti-TNF agents in patients with axial spondyloarthritis: Ann Rheum Dis, 2011; 70(6); 905-8
7.. Vastesaeger N, van der Heijde D, Inman RD, Predicting the outcome of ankylosing spondylitis therapy: Ann Rheum Dis, 2011; 70(6); 973-81
8.. S van der L, D van der H, Ankylosing spondylitis. Clinical features: Rheum Dis Clin North Am, 1998; 24(4); 48-52
9.. Lukas C, Cyteval C, Dougados M, Weber U, MRI for diagnosis of axial spondyloarthritis: Major advance with critical limitations “Not everything that glisters is gold (standard).”: Open, 2018; 4; 586
10.. Calin A, Taurog JD, The spondylarthritides Published online 1998;353
11.. Moll JMH, Wright V, New York clinical criteria for ankylosing spondylitis. A statistical evaluation: Ann Rheum Dis, 1973; 32(4); 354
12.. Underwood MR, Dawes P, Inflammatory back pain in primary care: Br J Rheumatol, 1995; 34(11); 1074-77
13.. O’Shea F, Salonen D, Inman R, The challenge of early diagnosis in ankylosing spondylitis: J Rheumatol, 2007; 34(1); 5-7
14.. Forestier J, Jacqueline F, Rotes-Querol: Ankylosing spondylitis Published online 1956
15.. Matthews WB, The neurological complications of ankylosing spondylitis: J Neurol Sci, 1968; 6(3); 561-73
16.. Khedr EM, Rashad SM, Hamed SA, Neurological complications of ankylosing spondylitis: Neurophysiological assessment: Rheumatol Int, 2009; 29(9); 1031-40
17.. Carman RD, And Fineman S, Harrington SW, Ankylosing spondylitis: (An analysis of 100 cases): CMAJ, 1947; 57(1); 16
18.. Kotil K, Yavasca P, Lumbar radiculopathy in ankylosing spondylitis with dural ectasia: J Clin Neurosci, 2007; 14(10); 981-83
19.. Bowie EA, Glasgow GL, Cauda equina lesions associated with ankylosing spondylitis: Br Med J, 1961; 2; 24-27
20.. Cumming WJK, Saunders M, Radiculopathy as a complication of ankylosing spondylitis: J Neurol Neurosurg Psychiatry, 1978; 41(6); 569-70
21.. Ramos-Remus C, Gomez-Vargas A, Guzman-Guzman JL, Frequency of atlantoaxial subluxation and neurologic involvement in patients with ankylosing spondylitis: J Rheumatol, 1995; 22(11); 2120-25
22.. Lan HHC, Chen DY, Chen CCC, Combination of transverse myelitis and arachnoiditis in cauda equina syndrome of long-standing ankylosing spondylitis: MRI features and its role in clinical management: Clin Rheumatol, 2007; 26(11); 1963-67
23.. Tyrrell PNM, Davies AM, Evans N, Neurological disturbances in ankylosing spondylitis: Ann Rheum Dis, 1994; 53(11); 714-17
24.. Lee JY, Kim J il, Park JY, Cervical spine involvement on longstanding ankylosing spondylitis: Clin Exp Rheumatol, 2005; 23(3); 331-39
25.. Ramos-Remus C, Russell AS, Gomez-Vargas A, Ossification of the posterior longitudinal ligament in three geographically and genetically different populations of ankylosing spondylitis and other spondyloarthropathies: Ann Rheum Dis, 1998; 57(7); 429-33
26.. Takahashi M, Kawanami H, Tomonaga M, Kitamura K, Ossification of the posterior longitudinal ligament – a roentgenologic and clinical investigation: Acta Radiol Diagn (Stockh), 1972; 13(1); 25-36
27.. Tarulli AW, Raynor EM, Lumbosacral radiculopathy: Neurol Clin, 2007; 25(2); 387-405
28.. Siré E, Van Der Heijde D, Rgen Braun J, Deodhar A, Modified stoke ankylosing spondylitis spinal score as an outcome measure to assess the impact of treatment on structural progression in ankylosing spondylitis: Rheumatology (Oxford), 2019; 58(3); 388-400
29.. Friedly J, Standaert C, Chan L, Epidemiology of spine care: The back pain dilemma: Phys Med Rehabil Clin N Am, 2010; 21(4); 659-77
30.. van der Linden S, Valkenburg HA, Cats A, Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria: Arthritis Rheum, 1984; 27(4); 361-68
31.. Mau W, Zeidler H, Mau R, Clinical features and prognosis of patients with possible ankylosing spondylitis. Results of a 10-year followup: J Rheumatol, 1988; 15(7); 1109-14
32.. Rudwaleit M, Khan MA, Sieper J, The challenge of diagnosis and classification in early ankylosing spondylitis: Do we need new criteria?: Arthritis Rheum, 2005; 52(4); 1000-8
33.. Caffrey MFP, James DCO, Human lymphocyte antigen association in anky-losing spondylitis: Nature, 1973; 242(5393); 121
34.. Brewerton DA, Hart FD, Nicholls A, Ankylosing spondylitis and HL-A 27: Lancet, 1973; 1(7809); 904-7
35.. Evans DM, Spencer CCA, Pointon JJ, Interaction between ERAP1 and HLA-B27 in ankylosing spondylitis implicates peptide handling in the mechanism for HLA-B27 in disease susceptibility: Nat Genet, 2011; 43(8); 761-67
36.. Blair HA, Secukinumab: A review in ankylosing spondylitis: Drugs, 2019; 79; 433-43
37.. Shen H, Goodall JC, Hill Gaston JS, Frequency and phenotype of peripheral blood Th17 cells in ankylosing spondylitis and rheumatoid arthritis: Arthritis Rheum, 2009; 60(6); 1647-56
38.. de Koning A, Schoones JW, van der Heijde D, Pathophysiology of axial spondyloarthritis: Consensus and controversies: Eur J Clin Invest, 2018; 48(5); e12913
39.. Zhu W, He X, Cheng K, Ankylosing spondylitis: Etiology, pathogenesis, and treatments: Bone Res, 2019; 7; 22
40.. Zhao SS, Pittam B, Harrison NL, Diagnostic delay in axial spondylo-arthritis: A systematic review and meta-analysis: Rheumatology (Oxford), 2021; 60(4); 1620-28
Figures
Tables
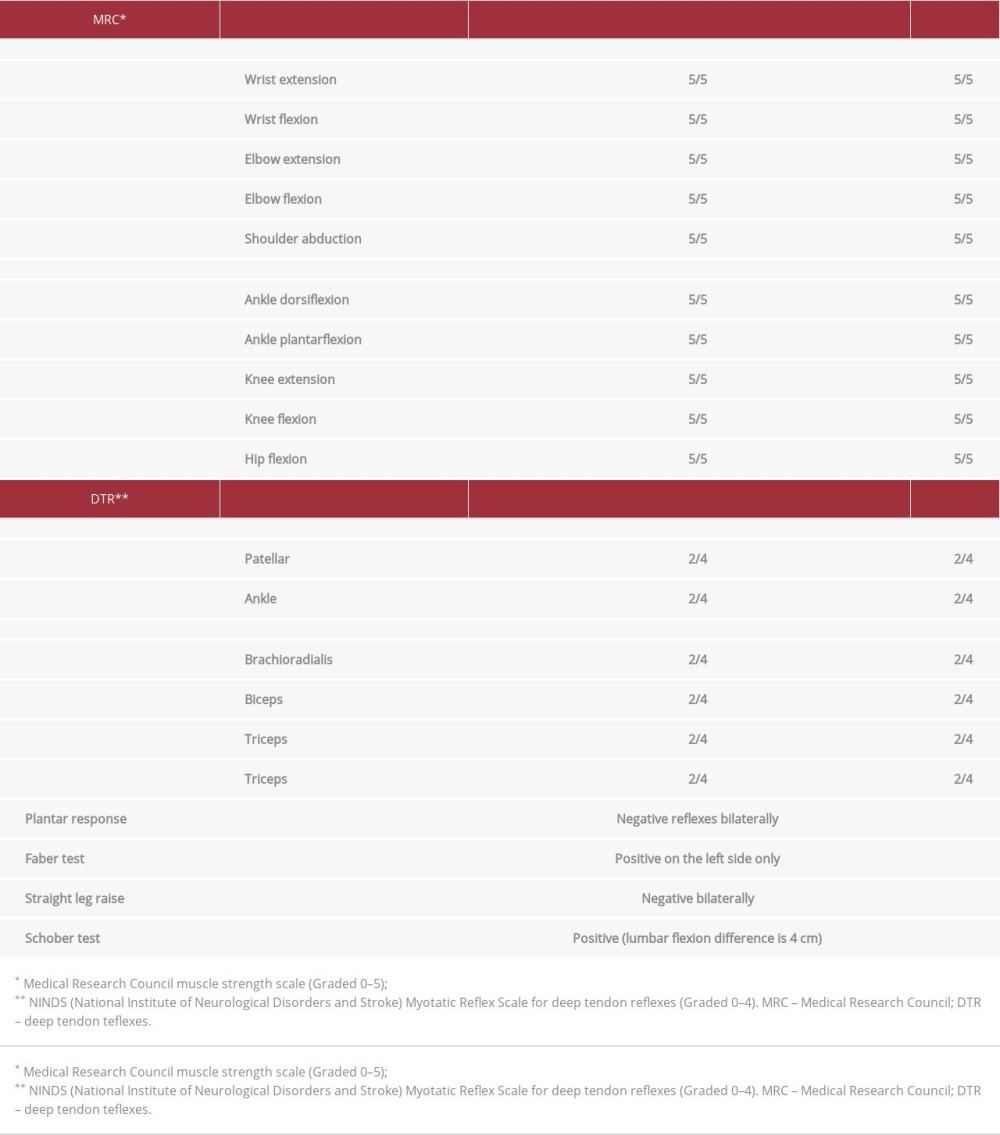 Table 1.. Muscle strength grading and deep tendon reflexes (on last visit).
Table 1.. Muscle strength grading and deep tendon reflexes (on last visit).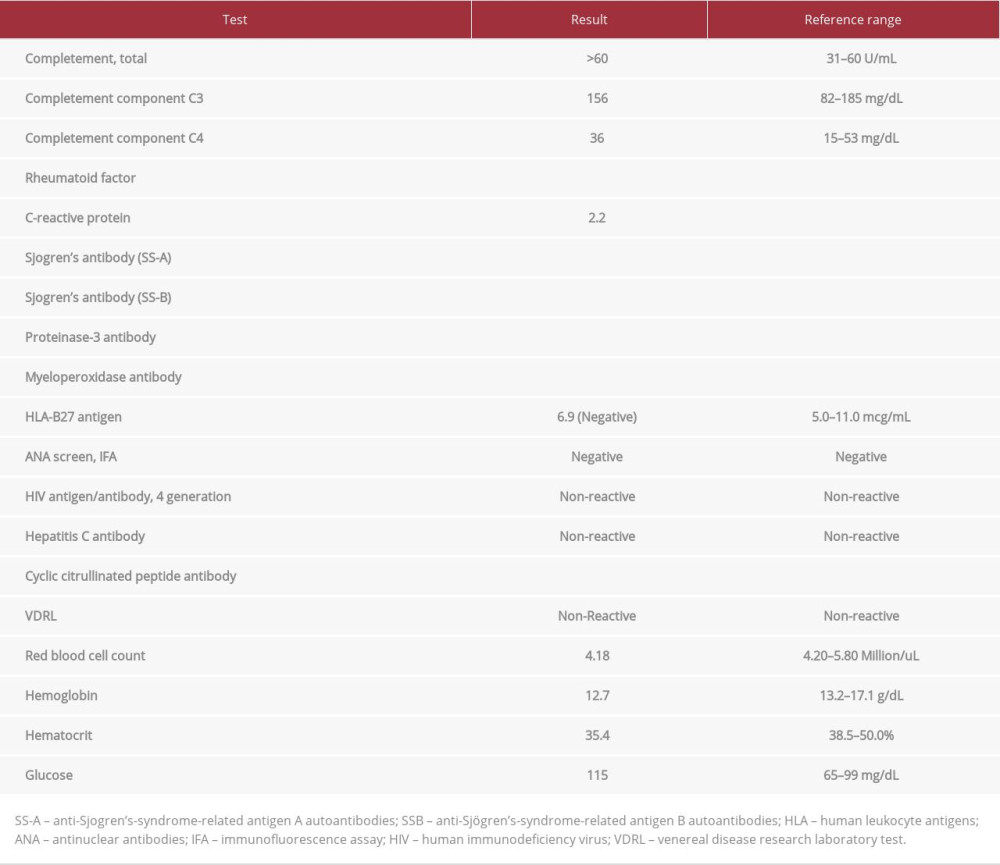 Table 2.. Patient’s laboratory tests summary (obtained on initial visit).
Table 2.. Patient’s laboratory tests summary (obtained on initial visit).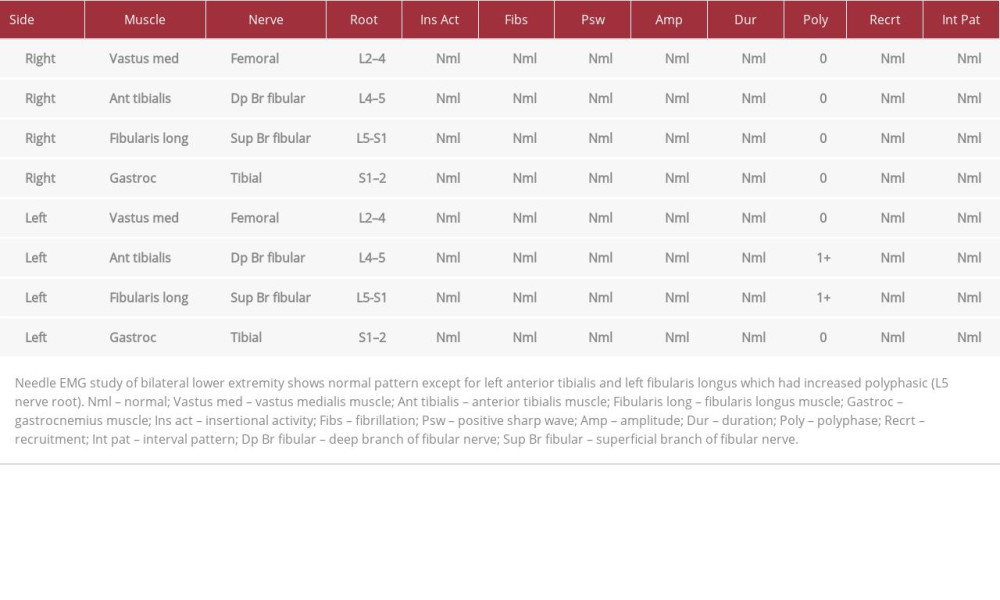 Table 3.. Needle EMG (Electromyogram) results obtained on the follow-up visit.
Table 3.. Needle EMG (Electromyogram) results obtained on the follow-up visit. Table 1.. Muscle strength grading and deep tendon reflexes (on last visit).
Table 1.. Muscle strength grading and deep tendon reflexes (on last visit). Table 2.. Patient’s laboratory tests summary (obtained on initial visit).
Table 2.. Patient’s laboratory tests summary (obtained on initial visit). Table 3.. Needle EMG (Electromyogram) results obtained on the follow-up visit.
Table 3.. Needle EMG (Electromyogram) results obtained on the follow-up visit. In Press
04 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.941835
05 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943042
05 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942578
05 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943801
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250








