10 November 2022: Articles 
A Rare Case of Prosthetic Joint Infection with
Rare coexistence of disease or pathology
Varsha Prasad1ABCDEFG*, Frederic Washburn2CDEF, Baina Barouni3EF, Musab Saeed4ABCDDOI: 10.12659/AJCR.937271
Am J Case Rep 2022; 23:e937271
Abstract
BACKGROUND: Chronic prosthetic joint infection (PJI) is a devastating complication following total joint arthroplasty, resulting in significant morbidity and mortality. The criterion standard of treatment for chronic PJI is two-stage revision arthroplasty consisting of complete hardware removal, thorough irrigation and debridement, placement of an antibiotic spacer, prolonged intravenous antibiotics based on culture sensitivities, and revision total knee arthroplasty once the infection resolves. The most common organism implicated in chronic PJI is Staphylococcus aureus.
CASE REPORT: In this report, we have summarized the case of a 75-year-old woman who developed chronic PJI caused by an unusual organism, Streptococcus gordonii, 1 year after a right total knee arthroplasty. S. gordonii is a gram-positive organism that is an oral flora and a colonizer of human teeth. This organism is known to create biofilm on the human teeth, more commonly known as dental plaque. S. gordonii has the ability to travel to extraoral sites and cause infection. It has been found to be a cause of subacute bacterial endocarditis, but it has been rarely described in the literature as a cause of prosthetic joint infection. Treatment of S. gordonii requires a tailored approach.
CONCLUSIONS: This case report highlights the clinical presentation, diagnosis, and treatment of chronic prosthetic joint infection caused by S. gordonii and identifies a rare cause of PJI that is not well documented in the literature. Streptococcal PJI portends a poorer prognosis, and identification of this organism is crucial for prompt treatment and improved outcomes for PJI.
Keywords: Biofilms, Knee Joint, Reoperation, Streptococcus gordonii, Female, Humans, Aged, Prosthesis-Related Infections, Debridement, Arthritis, Infectious, Arthroplasty, Replacement, Knee, Anti-Bacterial Agents
Background
Prosthetic joint infection (PJI) is defined as an infection of the joint prosthesis and intra-articular soft tissue. It is a devastating complication that affects approximately 1–2% of all total joint replacements [1–4]. Diagnosis of PJI is based on clinical appearance of the joint, laboratory markers, and synovial fluid analysis. Treatment of PJI depends on whether the infection is acute (<6 weeks from index surgery) or chronic (>6 weeks from index surgery). The criterion standard for treatment of chronic PJI is implant removal with thorough irrigation and debridement, placement of an antibiotic spacer, prolonged course of culture-specific intravenous antibiotics, and revision total joint arthroplasty once the infection has resolved [5]. Chronic PJI necessitates this form of orthopedic management because the infection cannot be eradicated with antibiotics alone once biofilm has formed on the orthopedic implants [5]. Even with criterion standard treatment, the morbidity and mortality rates of PJI are extremely high, with complications including poor patient-reported outcomes, disability, persistent infection, need for amputation, sepsis, and death [6]. The 1-year mortality rate for PJI is approximately 5-10%, with a 5-year mortality rate approaching 25% [6].
Case Report
A 75-year-old woman with a past medical history of hypertension and type 2 diabetes mellitus with insulin dependence presented 11 months after a primary right total knee arthroplasty with progressive pain and swelling of her right knee (Figure 1). She was evaluated by her orthopedic surgeon as an outpatient, where samples were taken for laboratory testing and a knee aspiration was performed. Laboratory test results revealed erythrocyte sedimentation rate (ESR) of 55 mm/h, C-reactive protein (CRP) of 12.8 mg/dL, and synovial white blood cell (WBC) count of 5000 K/uL, consistent with chronic PJI. Cultures were taken from this knee aspiration, which did reveal growth of
The patient underwent the first stage of her procedure, which consisted of removal of the right knee total arthroplasty, thorough irrigation and debridement, and placement of a static antibiotic spacer consisting of 2 batches of antibiotic-laden cement with 6 g of vancomycin and 4.8 g of tobramycin (Figure 2). She was initially treated for prosthetic joint infection with intravenous ceftriaxone 2 g daily and intravenous vancomycin 1 gm/D5W 200 mL pb every 24 h. This isolate was noted on the liquid broth media, which was aliquoted onto an agar plate and incubated for a minimum of 18–24 h. On the second reading of the agar plates, there was growth of the isolate, which was tested with a BioMerieux Vitek GPI card. The Vitek MS (MALDI-ToF) system was used for identification of the isolate. The Vitek system uses mass spectrometry, which is highly sensitive for organism identification. In our patient, the Vitek MS system identified the bacterium
Antibiotics were de-escalated to intravenous ceftriaxone 2 g every day according to sensitivities. The organism was pansensitive. Transthoracic echocardiography did not reveal obvious vegetations seen on any valves. Her postoperative course was complicated by an acute kidney injury, which resolved within 2 days of fluid hydration, and acute blood loss anemia, with hemoglobin measuring 6.9 g/dL, which resolved after transfusion with 1 unit of packed red blood cells. The patient was discharged on postoperative day 4 with ceftriaxone 2 g daily for a total of 6 weeks duration via a peripherally-inserted central catheter. Based on the growth of
At 8-week follow-up, the patient demonstrated resolution of infection, with repeat inflammatory markers within normal limits 2 weeks after an antibiotic holiday. One year following her initial total knee arthroplasty, and 8 weeks following PJI treatment, our patient underwent revision of the right knee total arthroplasty (Figure 3). Three intraoperative intra-articular synovial tissue samples were sent to Pathology, which did not demonstrate acute inflammation, confirming resolution of infection and the ability to proceed with the revision total knee arthroplasty. The patient was not continued on long-term suppressive antibiotics after this procedure. She recovered un-eventfully from the right revision total knee arthroplasty and is now doing well over 6 months after surgery. She has not demonstrated any signs or symptoms of recurrent infection and is happy with the functional level of her right knee. She continues to be routinely followed in the orthopedic clinic. There is a plan for continued follow-up with dental studies and colonoscopy.
Discussion
One potential explanation is oral trauma from the initial surgery, though this is unlikely as her infection developed 1 year after her index total knee arthroplasty and she underwent spinal anesthesia with monitored anesthesia care (MAC) during this procedure. Once the organism invaded the knee joint,
Prosthetic joint injection risk factors commonly include intravenous drug abuse, rheumatologic disorders, alcoholism, previous intra-articular corticosteroid injection, and diabetes mellitus. Our patient was diabetic, which may have predisposed her to the risk of prosthetic joint infection. Interestingly, she denied any recent history of routine dental cleaning or invasive dental procedures, which would have predisposed her to PJI caused by this specific organism. Orthopedic surgeons rarely require dental clearance prior to elective joint arthroplasty, but generally advise patients to delay dental procedures until 3 to 6 months after joint arthroplasty and recommend antibiotic prophylaxis for dental procedures indefinitely [8,9].
The
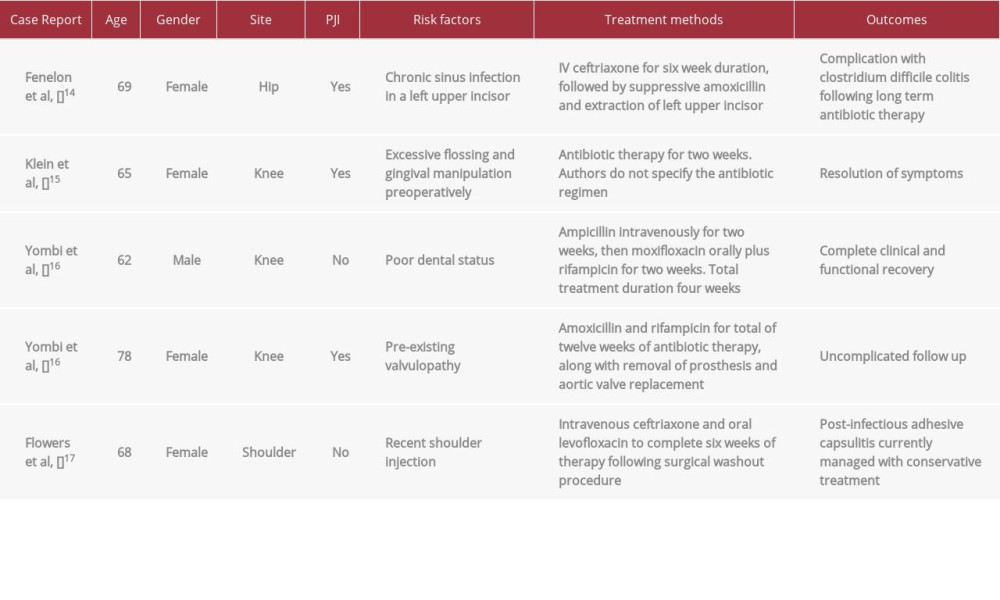
The case report by Yombi et al discussed 2 patients with PJI due to
A case report by Flowers et al described a 68-year-old woman who presented with septic arthritis of her glenohumeral joint following COVID-19 vaccination, with intraoperative joint cultures growing
A single-center case series by Dadon et al presented 15 patients with culture-proven
Although the
Conclusions
PJI is a devastating complication of orthopedic surgery, resulting in significant morbidity and mortality. Diagnosis and treatment of PJI requires a multidisciplinary approach with cooperation among orthopedics, medicine, and infectious disease departments. Our patient presented with chronic prosthetic joint infection caused by the unusual pathogen
Figures
References:
1.. Kurtz SM, Ong KL, Lau E, Prosthetic joint infection risk after TKA in the Medicare population: Clin Orthop Relat Res, 2010; 468; 52-56
2.. Abranches J, Zeng L, Kajfasz JK, Biology of oral streptococci: Microbiol Spectr, 2018; 6; 10.128
3.. Loo CY, Corliss DA, Ganeshkumar N: J Bacteriol, 2000; 182; 1374-82
4.. Tande AJ, Patel R, Prosthetic joint infection: Clin Microbiol Rev, 2014; 27; 302-45
5.. Morgenstern M, Post V, Erichsen C: J Orthop Res, 2016; 34; 1905-13
6.. Lum ZC, Natsuhara KM, Shelton TJ, Mortality during total knee peri-prosthetic joint infection: J Arthroplasty, 2018; 33; 3783-88
7.. Dadon Z, Cohen A, Szterenlicht YM: Ann Clin Microbiol Antimicrob, 2017; 16; 68
8.. McNally CM, Visvanathan R, Liberali S, Adams RJ, Antibiotic prophylaxis for dental treatment after prosthetic joint replacement: Exploring the Orthopaedic Surgeon’s opinion: Arthroplast Today, 2016; 2; 123-26
9.. Lima BP, Kho K, Nairn BL: mSphere, 2019; 4; e00814-19
10.. Svensson Malchau K, Tillander J, Zaborowska M, Biofilm properties in relation to treatment outcome in patients with first-time periprosthetic hip or knee joint infection: J Orthop Translat, 2021; 30; 31-40
11.. Kansara T, Pernia M, Kim Y, Saeed M: Cureus, 2019; 11; e5980
12.. Weber M, Gubler J, Fahrer H: Clin Rheumatol, 1999; 18; 417-21
13.. Blankstein A, Amsallem JL, Rubinstein E, Septic arthritis of the acromioclavicular joint: Arch Orthop Traumatic Surg (1978), 1985; 103; 417-18
14.. Fenelon C, Galbraith J, Dalton D, Masterson E: J Surg Case Rep, 2017; 2017; rjw235
15.. Klein R, Dababneh AS, Palraj BR: BMJ Case Reports, 2015; 2015; bcr2015210695
16.. Yombi Jcyr, Belkhir L, Jonckheere S: BMC Infect Dis, 2012; 12; 215
17.. Flowers RC, Rivera Rodriguez B, Corbitt K: BMJ Case Reports, 2021; 14; e243066
18.. Akgün D, Trampuz A, Perka C, Renz N, High failure rates in treatment of streptococcal periprosthetic joint infection: Bone Joint J, 2017; 99-B; 653-59
19.. Lora-Tamayo J, Senneville É, Ribera A, The not-so-good prognosis of streptococcal periprosthetic joint infection managed by implant retention: The results of a large multicenter study: Clin Infect Dis, 2017; 64; 1742-52
20.. Fiaux E, Titecat M, Robineau O, Outcome of patients with streptococcal prosthetic joint infections with special reference to rifampicin combinations: BMC Infect Dis, 2016; 16; 568
21.. Huotari K, Vuorinen M, Rantasalo M, High cure rate for acute streptococcal prosthetic joint infections treated with debridement, antimicrobials, and implant retention in a specialized Tertiary Care Center: Clin Infect Dis, 2018; 67; 1288-90
Figures
In Press
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943010
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943687
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943070
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943370
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250