02 November 2020: Articles 
Successful Clozapine Re-Challenge After Suspected Clozapine-Induced Myocarditis
Unusual clinical course, Challenging differential diagnosis, Unusual or unexpected effect of treatment, Diagnostic / therapeutic accidents, Adverse events of drug therapy
Seyed Alireza Hosseini1BCDEF*, Brianna Skrzypcak1BEF, Rama Yasaei1ABD, Sara Abdijadid1ADE, Fowrooz Joolhar2DE, Theingi Tiffany Win2E, Leila Moosavi3ADDOI: 10.12659/AJCR.926507
Am J Case Rep 2020; 21:e926507
Abstract
BACKGROUND: Clozapine plays a unique role in the management of treatment-resistant schizophrenia (TRS). Clozapine re-challenge following an episode of myocarditis is controversial, with a very limited literature, although it may be crucial in the recovery of certain patients. To date and to the best of our knowledge, only 10 of 22 studied cases reported successful clozapine retrial after myocarditis.
CASE REPORT: We present the case of a 22-year-old Hispanic man with treatment-resistant schizophrenia and polysubstance use disorder (methamphetamine, cannabis, and alcohol) initiated on aggressive clozapine titration after lack of response to several other therapies. Approximately 16 days after clozapine trial, the patient developed cardiac function impairment, presenting with chest pain, notable elevation in several biomarkers (troponin: 0.72 ng/ml, ESR >100 mm/h, CRP: 20.8 mg/dl, and BNP: 999 ng/ml), and a depressed ejection fraction at 25%. Further assessments also showed positive hepatitis A serology. Following discontinuation of clozapine and providing supportive care, the patient’s physical symptoms resolved. He had a relapse of psychotic symptoms, which were refractory to treatment with other antipsychotic agents. Subsequently, the patient underwent a second clozapine trial under close monitoring, with resolution of his psychosis. Repeated echocardiography demonstrated improved EF to 50%, transaminitis was resolved, repeat blood test results were normalized, and the patient was discharged while he was stabilized and asymptomatic.
CONCLUSIONS: This case adds to the previous case reports and suggests that clinicians may consider clozapine re-challenge following an episode of myocarditis based on clinical judgment, on a case-by-case basis, and under close monitoring. We highlight the need for development of clinical guidelines for clozapine re-challenge.
Keywords: clozapine, Drug-Related Side Effects and Adverse Reactions, myocarditis, Schizophrenia, Antipsychotic Agents, Echocardiography, young adult
Background
At present, clozapine is considered the most effective antipsychotic agent and it is the standard treatment with regulatory approval for patients with treatment-resistant schizophrenia [1]. Despite its beneficial effects, clozapine use is limited due to its adverse effects profile. Clozapine is associated with severe adverse effects, including agranulocytosis, leukopenia, pulmonary embolism, and rare but potentially life-threatening early myocarditis and later cardiomyopathy [2,3].
Myocarditis can be caused by a broad range of infectious and noninfectious etiologies. The most common infectious etiology is attributed to viruses [4]. The noninfectious causes of myocarditis include autoimmune diseases, toxins, use of illicit substances, and hypersensitivity to medications [5]. Incidence rates of clozapine-induced myocarditis (CIM) have been reported from fewer than 0.1% to at least 1% [6]. Clinical manifestations are highly variable, ranging from asymptomatic to sudden cardiac death [5]. ECG and laboratory findings are relatively nonspecific and do not confirm or exclude the diagnosis [3,7]. Echocardiography is one of the most helpful diagnostic tools and it is indicated in the presence of clinical and laboratory findings suggestive of myocarditis. Echocardiography findings may include left ventricular or biventricular dysfunction, reduced left ventricular ejection fraction (LVEF), and global or segmental wall motion abnormalities [3]. Cardiac magnetic resonance imaging (MRI) also has been proposed for the diagnosis of myocarditis; however, endomyocardial biopsy (EMB) is the diagnostic criterion standard [8]. Management of myocarditis is primarily conservative, and if related to clozapine use, immediate suspension of clozapine is indicated [9]. Reintroduction of clozapine in patients who had developed myocarditis is controversial [10]. The judgment to re-challenge clozapine depends on several factors and is typically performed under closely controlled conditions, in an inpatient setting, starting with low and slowly increased doses, and with close monitoring of laboratory and cardiological markers [11].
Case Report
The case described in this article was presented as a poster presentation at the Southern San Juaquin Valley Research Forum in May 2020 [12].
A 22-year-old Hispanic man, with a history of schizophrenia and polysubstance use disorder (methamphetamine, cannabis, and alcohol), was placed on an involuntary hold and admitted to the inpatient psychiatric unit (IPU) secondary to auditory, visual, and tactile hallucination, agitation, and violence. A history of incarceration, sexual and verbal abuse, and a family history of schizophrenia on the maternal side were noted on admission. The patient also had a history of long-term hospitalization in a state hospital, with a discharge diagnosis of schizophrenia. He reported continued use of methamphetamine, marijuana, and alcohol. Urine toxicology was positive on admission for methamphetamines.
During admission and upon further assessment, the patient endorsed hallucinations concurrent with mood symptoms and was started and maximized on olanzapine, which was later changed to risperidone without any noticeable improvement. The patient required multiple seclusions and administration of IM haloperidol and diphenhydramine due to persistent symptoms. The patient was determined to have TRS, and on day 22 of admission, treatment with clozapine was initiated according to the guidelines. Baseline leukocyte count, absolute neutrophil count (ANC), liver enzymes, and ECG were assessed and were found to be normal. Within 13 days, he was receiving clozapine 100 mg in the morning and 200 mg in the evening. With this treatment his symptoms improved, and agitation and psychosis were resolved.
On day 16 of clozapine therapy, the patient reported flu-like symptoms, weakness, sudden-onset chest pain, loose stools, and fever upon examination. Initial electrocardiography (ECG) showed sinus tachycardia with a heart rate of 112 beats/min, no acute ischemic changes, nonspecific T abnormalities in lateral leads, and a prolonged QTc of 482 (Figure 1). Supportive care was started, clozapine was discontinued, and risperidone was initiated. The patient continued to have worsening of his symptoms; therefore, he was transferred to the medical unit for further workup and monitoring. Cardiology and infectious disease were also consulted.
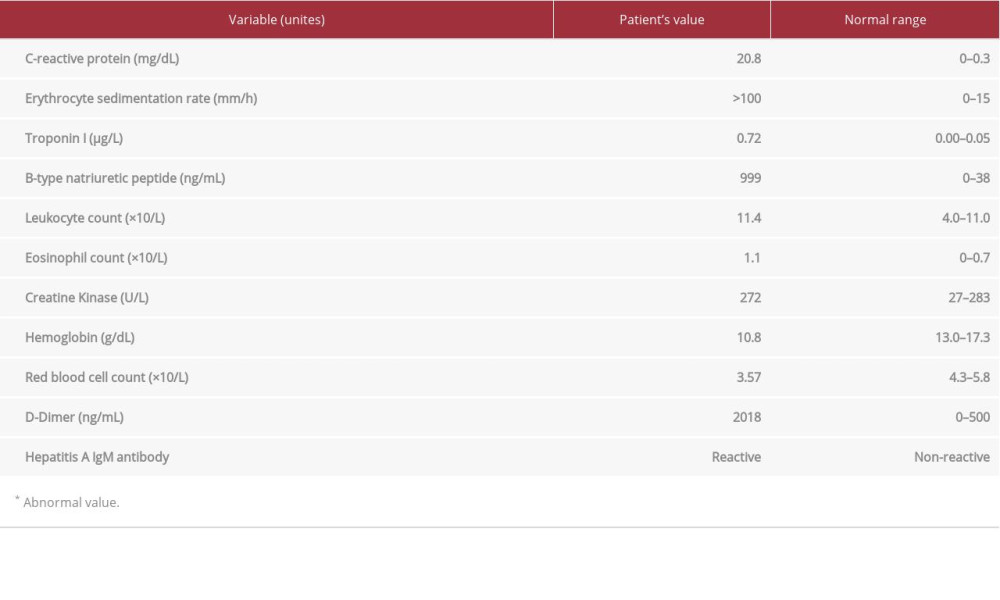
While on the medicine floor, an extensive workup was completed, and the patient was found to have transaminitis secondary to positive hepatitis A serology. We also assessed levels of elevated B-type natriuretic peptide (BNP) (999 ng/ml), C-reactive protein (CRP) (20.8 mg/dL), erythrocyte sedimentation rate (ESR) (>100 mm/h), troponin (0.72 µg/L), D-dimer, and eosinophil count (Table 1). Transesophageal echocardiography (TEE) showed dilated right-sided heart chambers, heart failure with reduced ejection fraction (HFrEF) of 25%, and a pulmonary artery pressure of 36 mmHg. Chest CT angiography was negative for pulmonary embolism. Metoprolol succinate and lisinopril were also started, and the patient was supportively treated and placed on contact isolation precautions secondary to hepatitis A. Over the next 3 weeks, his clinical symptoms resolved, and repeat blood test results were normalized. Repeated lab tests showed the resolution of transaminitis, and repeat echocardiography demonstrated improvement of the ejection fraction (EF) from 25% to 45–50%. Cardiac function impairment was less likely secondary to methamphetamine use due to rapid improvement in the EF; therefore, it was hypothesized that the most likely cause was clozapine. However, the patient endorsed the return of hallucinations and had worsening psychosis despite treatment with increasing doses of quetiapine. The timeline and dosage of administered antipsychotic medications during admission can be seen in Figure 2.
Risks and benefits of clozapine therapy were considered and extensively discussed with the patient and his conservator, and the decision was made to re-challenge with clozapine slowly while under close supervision. Slower titration was initiated with the initial dose of 12.5 mg, followed by increases of 25 mg per 48 h (Figure 2) while closely monitoring the patient on the telemetry unit with daily vital signs, weekly CRP and troponin, and assessments by the hospitalist. Approximately 3 weeks later, a repeat ECG showed a normal QTc of 442, sinus tachycardia of 102 beats/min, and borderline ST elevation. The patient continued to be closely monitored while clozapine was titrated back up to 100 mg in the morning and 200 mg in the evening, and his psychosis and agitation were resolved. He was stabilized and asymptomatic and educated on the adverse effects of clozapine and symptoms of recurrent myocarditis.
Discussion
There are multiple reports of clozapine-induced myocarditis in the published literature. Although clozapine-induced myocarditis is rare, it is probably under-reported due to: (a) the non-specific nature of clinical presentation; (b) lack of mandatory regulatory requirements to monitor clozapine-induced cardiac complications; and (c) the similarity between the features associated with the initiation of clozapine and the symptoms of myocarditis such as low-grade fever, tachycardia, fatigue, and eosinophilia [13].
CIM is a hypersensitivity reaction and some studies suggest it to be dependent on the rate of dose titration [14]. Rapid titration of over 25 to 50 mg per day may increase the risk [15]. Most cases of myocarditis have been reported to occur within the first month of clozapine treatment [16–18], although a few cases have been reported after several months of treatment [3]. Ronaldson et al. conducted a systematic review of 75 cases and 94 controls in Australia and found that the time to onset of myocarditis was 10 to 33 days, with 83% of cases occurring between days 14 to 21 after clozapine initiation [17]. Laboratory features of CIM may include elevated peripheral eosinophil counts and rise in serum concentrations of inflammatory biomarkers, especially ESR, CRP, BNP, cardiac troponins I and T, creatinine kinase-MB (CK-MB), interleukin-6 (IL4), and tumor necrosis factor-α (TNF-α) [6]. Due to the range of symptoms associated with CIM, it is important to monitor laboratory biomarkers for signs of possible myocardial inflammation [17,19]. To date, there is not a standard monitoring protocol for CIM. In a study conducted by Ronaldson and colleagues, a combination of troponins greater than twice the upper limit of normal and CRP over 100 mg/dl showed an estimated 100% sensitivity for symptomatic CIM, thus proposing a new monitoring protocol consisting of weekly monitoring of troponins and CRP for the first 4 weeks of clozapine initiation [17]. If the clinical presentation is consistent with CIM, a further workup with ECG and echo is warranted. CIM can be definitively diagnosed with eosinophilic inclusions on EMB, although it cannot be practically implemented routinely because of its clinical risks and limitations [3].
Our patient presented with acute chest pain, flu-like symptoms, weakness, fever, eosinophilia, reduced EF, and elevation in BNP, troponin, CRP, ESR, and D-dimer, approximately 16 days after the first trial of clozapine. Although clozapine-induced cardiomyopathy can present with similar manifestations, it is often a delayed reaction occurring after about 8 months of treatment [20]. Our patient also had a history of chronic methamphetamine and alcohol use, which can also cause cardiac function impairment. Most of the evidence for meth-amphetamine-associated cardiomyopathy suggest that cardiac dysfunction can be reversed after discontinuance of meth-amphetamine, but the recovery time window is unclear [21]. Given the rapid improvement in our patient’s LVEF, myocarditis was more likely secondary to clozapine treatment rather than chronic methamphetamine use. Also, alcoholic cardiomyopathy is often associated with a history of excessive alcohol consumption (>90 g/day) for at least 5 years [22], which is inconsistent with our patient’s history. Moreover, although our patient experienced acute hepatitis A concurrent with possible myocarditis, hepatitis A appears to be an extremely rare cause of myocarditis, as we have identified only 5 other such cases in the literature [23–26]. Finally, the temporal association of cardiac function impairment, clinical symptoms, and laboratory abnormalities with clozapine administration suggests a high likelihood of clozapine etiology.
Since clozapine is the only medication with regulatory approval for TRS, it presents a real therapeutic challenge if myocarditis occurs. At present, there is no guideline in place for clozapine re-challenge after CIM and reports are very limited and quite heterogeneous. Manu et al. reviewed published case reports of clozapine re-challenge after major adverse effects and suggested that clozapine re-challenge is reasonable after neutropenia and neuroleptic malignant syndrome, but not after myocarditis and agranulocytosis [10,27]. To date and to the best of our knowledge, there are reports that described 22 cases of clozapine retrial after CIM, including 12 successful and 10 unsuccessful, suggesting at least limited support for re-challenge. In a 2018 systematic review involving 359 cases of possible CIM, clozapine re-challenge was reported for 19 patients; of these, 12 had a successful re-challenge while the remaining 7 had unsuccessful re-challenges [16]. Also, a 2019 case series reported 3 cases that all had unsuccessful retrial after CIM [28]. However, clozapine re-challenge may be critical for the recovery of patients who continue to be resistant to other first- and second-generation antipsychotics by displaying psychotic symptoms and suicidality [29]. Factors that may affect decision-making and outcome include the severity of psychotic illness for which clozapine was initially started, resistance to other treatments, the degree of the initial response to clozapine trial, concurrent use of valproic acid [14,28], the severity of myocarditis, rate of clozapine titration, and time of re-challenge [30].
Our patient’s young age, rapid deterioration of psychiatric illness after a positive response to clozapine, and nonresponse to a broad range of other antipsychotics appeared to justify the risks associated with clozapine re-challenge. Our study is limited by lack of resources to perform endomyocardial biopsy for definitive diagnosis of myocarditis in our institution, as well as lack of a longstanding follow-up of our patient to determine the outcome, as that access to the patient/caregiver was not possible. Based on this case report and literature review, we are unable to outline distinct clinical factors that can predict which patients are better candidates for clozapine re-challenge following an episode of CIM. First and foremost, all physicians should be aware of this potentially fatal cardiac adverse effect of clozapine. Monitoring protocols may help in the early detection and treatment of CIM. We also suggest that physicians should consider clozapine re-challenge on a case-by-case basis by conducting a risk-benefit analysis of untreated schizophrenia versus CIM, and the patient should be included in this discussion to obtain consent. If a clozapine re-challenge is deemed appropriate, clozapine should be slowly titrated while the patient is hospitalized and monitored for recurrent symptoms.
Conclusions
Clozapine plays a unique role in the management of treatment-resistant schizophrenia, and it may be critical for the improvement of certain patients. This uniqueness becomes even more prominent during decision-making for clozapine re-challenge after an episode of myocarditis. The current literature on this subject is very limited, and only 10 (45%) of 22 studied cases have been reported to have had a successful retrial. The present case adds to the previous cases and suggests that clinicians may consider clozapine re-challenge after an episode of myocarditis based on clinical judgment, on a case-by-case basis, and under close observation and monitoring. We emphasize the need for development of clinical guidelines for clozapine re-challenge and more research to establish the risks, benefits, and strategies.
Figures
References:
1.. Curto M, Comparelli A, Ciavarella GM, Impairment of left ventricular function early in treatment with clozapine: A preliminary study: Int Clin Psychopharmacol, 2015; 30(5); 282-89
2.. Yuen JWY, Kim DD, Procyshyn RM, Clozapine-induced cardiovascular side effects and autonomic dysfunction: A systematic review: Front Neurosci, 2018; 12; 203
3.. Curto M, Girardi N, Lionetto L, Systematic review of clozapine cardiotoxicity: Curr Psychiatry Rep, 2016; 18(7); 68
4.. Rose NR, Viral myocarditis: Curr Opin Rheumatol, 2016; 28(4); 383-89
5.. Blauwet LA, Cooper LT, Myocarditis: Prog Cardiovasc Dis, 2010; 52(4); 274-88
6.. Cohen D, Bogers JPAM, van Dijk D, Beyond white blood cell monitoring: Screening in the initial phase of clozapine therapy: J Clin Psychiatry, 2012; 73(10); 1307-12
7.. Baptista T, Rojas N, Dávila DF, Heterogeneity of clozapine-associated myocarditis: An opportunity for novel preventing strategies: Aust NZJ Psychiatry, 2015; 49(11); 1068
8.. Hatton JL, Bhat PK, Gandhi S, Clozapine-induced myocarditis: Recognizing a potentially fatal adverse reaction: Tex Heart Inst J, 2015; 42(2); 155-57
9.. Kindermann I, Barth C, Mahfoud F, Update on myocarditis: J Am Coll Cardiol, 2012; 59(9); 779-92
10.. Manu P, Lapitskaya Y, Shaikh A, Nielsen J, Clozapine rechallenge after major adverse effects: Clinical guidelines based on 259 cases: Am J Ther, 2018; 25(2); e218-23
11.. Ittasakul P, Archer A, Kezman J, Rapid rechallenge with clozapine following pronounced myocarditis in a treatment-resistant schizophrenia patient: Clin Schizophr Relat Psychoses, 2016; 10(2); 120-22
12.. Hosseini A, Skrzypcak B, Yasaei R, Successful clozapine re-challenge after suspected clozapine-induced myocarditis
13.. Ronaldson KJ, Fitzgerald PB, McNeil JJ, Clozapine-induced myocarditis, a widely overlooked adverse reaction: Acta Psychiatr Scand, 2015; 132(4); 231-40
14.. Ronaldson KJ, Fitzgerald PB, Taylor AJ, Rapid clozapine dose titration and concomitant sodium valproate increase the risk of myocarditis with clozapine: A case-control study: Schizophr Res, 2012; 141(2–3); 173-78
15.. Chopra N, de Leon J, Clozapine-induced myocarditis may be associated with rapid titration: A case report verified with autopsy: Int J Psychiatry Med, 2016; 51(1); 104-15
16.. Bellissima BL, Tingle MD, Cicović A, A systematic review of clozapine-induced myocarditis: Int J Cardiol, 2018; 259; 122-29
17.. Ronaldson KJ, Fitzgerald PB, Taylor AJ, A new monitoring protocol for clozapine-induced myocarditis based on an analysis of 75 cases and 94 controls: Aust NZJ Psychiatry, 2011; 45(6); 458-65
18.. Haas SJ, Hill R, Krum H, Clozapine-associated myocarditis: A review of 116 cases of suspected myocarditis associated with the use of clozapine in Australia during 1993–2003: Drug Saf, 2007; 30(1); 47-57
19.. Freudenreich O, Clozapine-induced myocarditis: Prescribe safely but do prescribe: Acta Psychiatr Scand, 2015; 132(4); 240-41
20.. Grenade LL, Graham D, Trontell A, Myocarditis and cardiomyopathy associated with clozapine use in the United States: N Engl J Med, 2001; 345(3); 224-25
21.. Won S, Hong RA, Shohet RV, Methamphetamine-associated cardiomyopathy: Clin Cardiol, 2013; 36(12); 737-42
22.. George A, Figueredo VM, Alcoholic cardiomyopathy: A review: J Card Fail, 2011; 17(10); 844-49
23.. Allen O, Edhi A, Hafeez A, Halalau A, A very rare complication of hepatitis A infection: Acute myocarditis – a case report with literature review: Case Rep Med, 2018; 2018; 3625139
24.. Park YM, Kang WC, Shin K-C, Acute viral hepatitis A presented with myopericarditis: Int J Cardiol, 2011; 153(2); e34-36
25.. Özen M, Koçak G, Özgen Ü, Hepatitis-A virus induced acute myocarditis: İnönü Üniversitesi Tıp Fakültesi Dergisi, 2006; 13(1); 47-49
26.. Botero V, García VH, Aristizabal AM, Hepatitis A, cardiomyopathy, aplastic anemia, and acute liver failure: A devastating scenario: Transpl Infect Dis, 2018; 20(2); e12842
27.. Manu P, Sarpal D, Muir O, When can patients with potentially life-threatening adverse effects be rechallenged with clozapine? A systematic review of the published literature: Schizophr Res, 2012; 134(2–3); 180-86
28.. Noël M-C, Powell V, Burton L, Clozapine-related myocarditis and re-challenge: A case series and clinical review: J Clin Psychopharmacol, 2019; 39(4); 380-85
29.. Rosenfeld AJ, Gibbs T, Ivie R, Successful clozapine retrial after suspected myocarditis: Am J Psychiatry, 2010; 167(3); 350-51
30.. Ronaldson KJ, Fitzgerald PB, Taylor AJ, McNeil JJ, Observations from 8 cases of clozapine rechallenge after development of myocarditis: J Clin Psychiatry, 2012; 73(2); 252-54
Figures
In Press
26 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943893
27 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942126
27 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943098
27 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943725
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250