05 December 2020: Articles 
Duodenal Laceration Due to Blunt Trauma Caused by Horse Kick: A Case Report and Literature Review
Unusual clinical course, Challenging differential diagnosis, Rare disease
Jan-Peter Correia Sousa Périssé1ACDEF*, Ana Luiza de Carvalho Miranda Rosati Rocha2AF, Raphael Lessa Coelho3ABCDEFG, Bruno Guerra Campanario3BF, Luis Fernando Rosati Rocha3ABCFDOI: 10.12659/AJCR.927461
Am J Case Rep 2020; 21:e927461
Abstract
BACKGROUND: Duodenal trauma usually consists of retroperitoneal lesions. Its management can be complicated by the location of the injury and difficulty in making an early diagnosis. Duodenal injuries are divided into blunt and penetrating trauma, and the possible results are hematoma, laceration, and devascularization. Duodenal lesions due to blunt trauma are usually accompanied by lesions of nearby organs. We present a rare case of a single duodenal laceration due to blunt abdominal trauma caused by a horse kick, along with a literature review.
CASE REPORT: A 13-year-old boy presented to our emergency department after being kicked by a horse in his abdomen. He was stable and complained of abdominal pain without any other specifications. Computed tomography imaging revealed a retropneumoperitoneum and free fluid in the abdominal cavity. The patient was taken for an emergency laparotomy, which showed a single duodenal laceration of the second and third portions of the duodenum. The laceration was repaired with a double-layer closure using monofilament 3-0 polypropylene suture. The patient recovered from his injuries and was well at his last follow-up.
CONCLUSIONS: This case highlights the possible outcomes of an innocent blunt trauma and the importance of early diagnosis for the best outcome of a duodenal laceration. It also identifies the dissociation between the patient’s clinical presentation and his significant intra-abdominal injury.
Keywords: Abdominal Injuries, Lacerations, Retropneumoperitoneum, Wounds and Injuries, Wounds, Nonpenetrating, Duodenum, Horses, Laparotomy
Background
Duodenal trauma can present a challenging clinical situation because the retroperitoneal location of the larger part of the duodenum hinders early diagnosis, resulting in a higher rate of morbidity and mortality [1–3]. Duodenal trauma usually consists of retroperitoneal lesions, which represent a small percentage of abdominal injuries. These injuries can be divided into blunt or penetrating lesions, with blunt injuries being rarer (ratio of 1: 5) [1–3]. The kinetic mechanism in blunt duodenal trauma is mainly caused by crushing or compression, involving a direct force applied to the abdominal wall, which is then transmitted to the duodenum as it is compressed against the spinal column [1–4].
The American Association for Surgery of Trauma Organ Injury Scale (AAST-OIS) committee classifies duodenal injuries as grades I to V. The primary purpose of the duodenal injury grading system is to help a surgeon identify the procedure with the greatest chance of success, depending on the specific grade of injury [1,2,5,6].
Postoperative complications of duodenal surgery include an intra-abdominal abscess, duodenal obstruction, recurrent pancreatitis, and fistula related to surgical repair failure caused by suture line dehiscence [1–3]. The mortality rate of duodenal injury ranges from 5.3% to 30%, and the most relevant causative factor for a higher rate is late diagnosis [1–3].
We report a case of blunt abdominal trauma with a single lacerative lesion of the second and third portions of the duodenum due to a horse kick, without any associated lesions. Also, we briefly discuss the lesion’s diagnostic modalities and primary treatments.
Case Report
A 13-year-old boy was kicked by a horse in the right upper quadrant of his abdomen. He presented to the emergency department in stable condition, reporting that the accident had occurred 5 h earlier and that he was feeling only diffuse abdominal pain, without specifying the location. During the physical examination, the patient was stable, normotensive, normocardic, and did not show signs of confusion or altered consciousness. His abdomen was flaccid, diffusely painful, with no signs of peritoneal irritation. A computed tomography (CT) scan of the abdomen showed a retropneumoperitoneum near the duodenum (Figure 1) and free fluid around the duodenum arch and hepatic hilum and in the rectovesical pouch (Figure 2). To avoid a delay in surgery, contrast material was not used in the CT scan. Therefore, the trauma team directed the patient for an emergency xiphopubic laparotomy.
During the procedure, the surgeon noticed a bilious secretion in the retroperitoneal area around the duodenum, in the same topography indicated in the CT scan. Therefore, the Kocher and Cattell-Braasch maneuvers were performed to increase duodenal exposure, revealing a single laceration on the anterior wall of the second and third portions of the duodenum, which compromised 40% of the duodenal circumference (Figure 3) and was associated with increased bilious secretion in the area. No hematomas were noticed.
The surgical procedure for this injury was a primary double-layer closure with monofilament 3-0 polypropylene suture (Figure 4) and nasoenteric tube placement until the Treitz ligament. Also, a thorax tube jacket with a Penrose drain was inserted in the retroperitoneum close to the injury location, draining to the right flank.
The patient showed satisfactory improvement, with flatus elimination in the second postoperative day. Parenteral nutrition was given until the ninth postoperative day, as episodes of vomiting hindered the initiation of an oral diet and implicated the use of a nasogastric tube. The patient was transferred to another ward on the ninth day. Antibiotic therapy of ciprofloxacin plus metronidazole was administered for 6 days, which was then changed to amoxicillin plus clavulanic acid for 10 days. Also, octreotide and prophylactic enoxaparin were given for 7 days.
Discussion
Duodenal lesions represent 4.3% of all abdominal injuries and occur in a male: female ratio of 5: 1. Individuals between 16 and 30 years old have 70% of all duodenal injuries. Only 20% of duodenal injuries are due to blunt trauma, while 80% are due to penetrating trauma. Therefore, the present case report represents the group of less common lesions. However, blunt duodenal lesions are most common in pediatric patients (70– 78%); although, they represent less than 1% of all pediatric traumas [1–3,7].
The mechanism of injury of blunt duodenal trauma is crucial in determining the surgical course. Blunt duodenal trauma involves the application of a direct force toward the abdominal wall, mainly the right upper quadrant, which projects the duodenum posteriorly against the rigid and firm vertebral column. Examples of a duodenal crush injury include the impact of a steering wheel against the epigastrium and a bicycle handle-bar against the midepigastrium, which is especially common in children. Also, the lesion can happen when acceleration and deceleration forces act in the duodenum during a fall from a great height [1–4,8]. In the present case, the horse kick represents the same mechanism as the steering wheel contusion, as it applied a strong deceleration force against the abdominal right upper quadrant.
Duodenal injuries are reported as lesions with significant morbidity and mortality rates. There is a scarcity of cases in the literature, which results in less information regarding its management, especially when the mechanism of injury involves blunt trauma. Furthermore, these injuries can be significantly challenging for a surgeon owing to their retroperitoneal location [1,3].
The patient may present clinical signs and symptoms such as vomiting (especially hematemesis) and epigastralgia. The pain becomes more specific for this category of injury when it intensifies with peritoneal stimulation and radiates to the lower back. Other less common presentations are back pain, peritonitis, and upper-quadrant abdominal distension associated with infrequent or muted borborygmus. Moreover, a patient may present with fever and tachycardia. Physical examination may identify retropneumoperitoneum as anterior sacral crepitus during the rectal digital examination. Butler et al. (1993) described testicular pain and priapism in association with duodenal injury, which was possibly due to the stimulation of sympathetic fibers running along the gonadal vessels [1,4,9–12]. Our patient did not show any of the specific symptoms described above, presenting with only diffuse abdominal pain and tachycardia.
Because of its retroperitoneal location and proximity to several organs and structures, such as the right kidney, liver, common biliary duct, and colon, the duodenum is rarely injured alone. Therefore, an isolated duodenal laceration is a significant exception, especially when caused by blunt trauma. The most commonly injured organs associated with duodenal injury are the liver (17%) and colon (13%). Anatomically, the most affected region of the duodenum is the second portion (36%), followed by the third (18%), fourth (15%), and first (13%). Although rare, isolated laceration of the duodenum is possible [1,3], as shown in the present case report.
The diagnosis of duodenal injury in hemodynamically unstable patients is often performed by exploratory laparotomy. In such severe cases, damage control management should always be considered, especially if the patient presents with acidosis, coagulopathy, or hypothermia [2,3,5].
Suggestive surgical findings of duodenal injury include duodenal subcutaneous emphysema, bile in the duodenal wall, free biliary fluid, a retroperitoneal hematoma around the duodenum, and a right perirenal hematoma. The duodenum must be thoroughly inspected to avoid missing any injury. Therefore, the Kocher and Catell-Braasch maneuvers are recommended to mobilize and fully inspect the duodenum [2,3,5,10,12].
In stable patients, the best examination to investigate duodenal injury is the CT scan, which has higher accuracy when an intravenous or oral contrast material is used. CT scanning shows 86% sensitivity and 88% specificity in diagnosing blunt hollow viscus injury when performed with intravenous contrast, compared with 53% sensitivity and 69% specificity in a diagnosis by physical examination. The main CT scan findings associated with duodenal injury are mesenteric hematoma (37%) and free fluid (30%). Duodenal perforation can be observed on the CT scan, as the air (or fluid) leakage gathers in the lesser sac. Occasionally, a pneumoperitoneum may also be visualized, as this pouch communicates with the greater sac through the Winslow foramen. The presence of extraluminal air has high specificity for bowel perforation. Furthermore, there may be lesions communicating directly to the greater sac because of the location of the inferior portion of the duodenum. Kunin et al. described the presence of gas or fluid in the right anterior pararenal space and focal thickening of the duodenal wall, although these are not commonly found [1–3,13–15]. To avoid surgical treatment delay in the present case, contrast was not used, as a retropneumoperitoneum and free abdominal fluid were already identified in the non-contrasted CT scan.
Laboratory findings provide little help in diagnosing duodenal injury in an early scenario. Although the serum amylase level can indicate duodenal injury, it has low sensibility and specificity; therefore, it must not be used as an indicator for exploratory laparotomy [1].
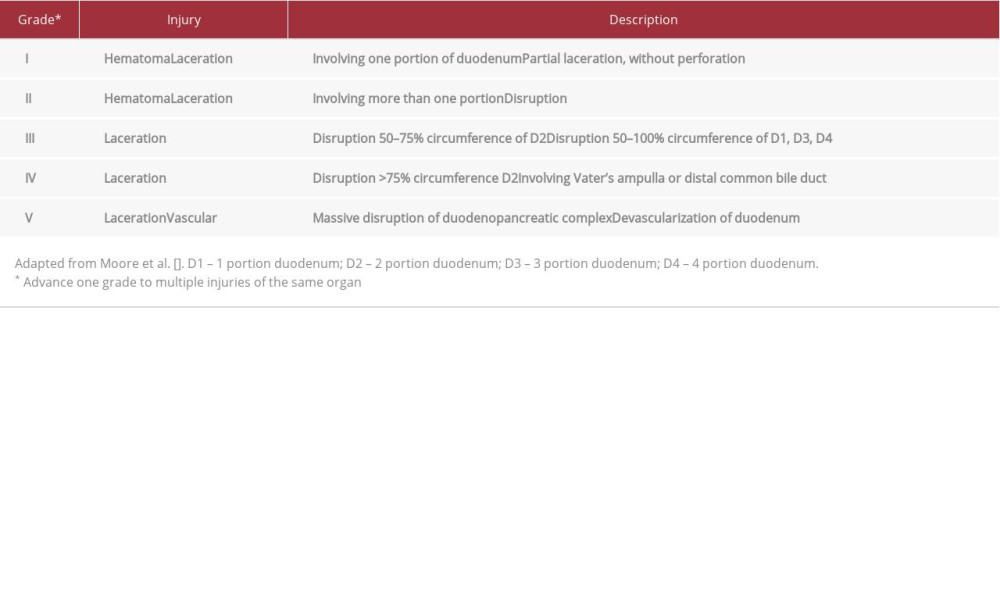
The AAST-OIS divides duodenal injuries into grades I to V, according to the lesion’s type (laceration or hematoma), length, and enterovascular repercussions (Table 1). These categories help surgeons choose the best approach for each presentation [1,2,5,6].
The AAST-OIS classification of duodenal injury has a significant benefit for surgical management, making it possible to design a full management algorithm, as described by Malhotra et al. The use of a drain adjacent to duodenal repairs is indicated in all duodenorrhaphies [2–5].
The management of a grade I initial hematoma diagnosed by CT scanning includes nasogastric tube decompression and withholding of oral intake. The hematoma can cause duodenal obstruction and, if it persists for 14 days, surgical intervention with drainage of the hematoma and simple repair should be performed. This intervention is also recommended for an intraoperative finding of duodenal hematoma when the lumen is compromised by 50% or more; otherwise, nothing needs to be done. If the hematoma occupies more than 75% of the intestinal lumen, a gastrojejunostomy should be performed to avoid delayed duodenal obstruction. When a grade I laceration is found, it should be repaired [2–5].
Grade II hematomas require the same management as grade I. However, grade II lacerations may be repaired early after injury with a simple primary tension-free closure in the longitudinal orientation, providing that the edges are viable and clean. Closure in the transverse orientation is recommended, as several authors suggest it prevents the intestinal lumen from narrowing. However, in situations when tension-free repair is not possible or when there is contamination or delay in surgery, the injury should be managed as a grade III injury [2–5]. Our patient was treated successfully with this technique, with a second layer added to ensure security of the closure and prevent further leakage.
The treatment of grade III injuries can vary. When possible, tension-free repair is recommended. In the case of more extensive lacerations, a segment of the organ can be resected, and an endto-end duodenostomy should be performed. If duodenal mobilization is not possible because of lesions in the second portion, a Roux-en-Y duodenostomy can be performed. If the injury is in the first portion of the duodenum or proximal to the second portion, the surgeon can perform an antrectomy along with gastrojejunostomy with the distal duodenal closed (Billroth II procedure) [2–5].
For grade IV injuries, if the bile duct and ampulla are intact, the surgery can be performed similarly to grade III injuries; otherwise, grade IV can be treated in the manner of grade V [2–5].
Grade V injuries have the worst prognosis and can be devastating, often requiring the patient to undergo damage control surgery. If the patient survives after posttraumatic management, the reconstructive surgery may involve replantation of the common bile duct to the duodenum or an anastomosis to the Roux-en-Y jejunal loop. If the duodenum cannot be repaired or the pancreatic head is destroyed, a pancreaticoduodenectomy (Whipple procedure) can be performed [2–5].
Mortality secondary to duodenal trauma can be divided into early (in the first 48 h after injury) and late mortality (after 48 h). Of all deaths associated with duodenal trauma, 75% are early deaths and are usually associated with hemorrhage and injuries to the central nervous system. Late deaths are mainly due to sepsis, duodenal fistula, and multiple organ failure. Postoperative complications include the development of an abscess (15%), fistula related to surgical repair failure due to suture line dehiscence (6%), duodenal obstruction (0.9%), and recurrent pancreatitis (0.5%) [1–3].
According to a review by Santos et al., the mortality rate associated with duodenal trauma ranges from 5.3% to 30%. Factors that increase the mortality rate include pancreatic injuries and common bile duct injuries. However, the most important factor related to mortality is a delay in diagnosis and repair. Regarding mortality by lesion classification, grade IV injuries have a 58.8% mortality rare, while grade I, II, and III injury rates are 8.3%, 18.7%, and 27.6%, respectively [1–3,16].
Octreotide administration for duodenal trauma has 2 main effects. First, as a somatostatin analogue, octreotide reduces gastrointestinal secretions, including exocrine pancreatic secretions. In that case, the postoperative administration of octreotide can prevent fistula formation, in addition to reducing the secretion of fluid into the retroperitoneal cavity. Second, octreotide can also potentially act as a splanchnic vasoconstrictor, assisting in the control of possible bleeding in the area. Thus, octreotide may be an important factor in postoperative recoveries after duodenal and pancreatic trauma [17–21].
Conclusions
Although rare, duodenal injuries are a serious concern in patients with abdominal trauma owing to a high mortality rate and potentially difficult early diagnosis, even with the aid of imaging examinations.
This case report describes a grade II blunt duodenal injury with an unusual etiology. It consisted of a single lacerative lesion of the second and third portions of the duodenum with a length less than 50% of the organ’s circumference. Surgical management consisted of a primary double-layer closure. Single-layer closure is also possible, and has more reports in the literature than double-layer closure. The present case is a rare report because of the mechanism of injury, a kick by a horse, that caused the isolated duodenal injury.
A successful recovery of duodenal injury is related to early diagnosis and repair. In our report, the patient was diagnosed and submitted to surgery in fewer than 12 h from injury and had a complete recovery.
Figures
References:
1.. Santos EG, Sanchez AS, Verde JM, Duodenal injuries due to trauma: Review of the literature: Cir Esp (English Edition), 2015; 93(2); 68-74
2.. Moore EE, Feliciano DV, Mattox KL: Trauma 8th ed New York (NY), 2017, Education, McGraw Hill
3.. Asensio JA, Feliciano DV, Britt LD, Kerstein MD, Management of duodenal injuries: Curr Probl Surg, 1993; 30(11); 1023-93
4.. Chen GQ, Yang H, Management of duodenal trauma: Chin J Traumatol, 2011; 14(1); 61-64
5.. Malhotra A, Biffl WL, Moore EE, Western Trauma Association Critical Decisions in Trauma: Diagnosis and management of duodenal injuries: J Trauma Acute Care Surg, 2015; 79(6); 1096-101
6.. Moore EE, Cogbill TH, Malangoni MA, Organ injury scaling, II: Pancreas, duodenum, small bowel, colon, and rectum: J Trauma, 1990; 30(11); 1427-29
7.. Coccolini F, Kobayashi L, Kluger Y, Duodeno-pancreatic and extrahepatic biliary tree trauma: WSES-AAST guidelines: World J Emerg Surg, 2019; 14; 56
8.. Rodríguez-García JA, Ponce-Escobedo AN, Pérez-Salazar DA, Duodenal injury in blunt abdominal trauma. Case report and literature review: Cir Cir, 2019; 87(S1); 53-57
9.. Pandey S, Niranjan A, Mishra S, Retrospective analysis of duodenal injuries: A comprehensive overview: Saudi J Gastroenterol, 2011; 17(2); 142-44
10.. Fraga GP, Biazotto G, Villaça MP, Trauma de duodeno: Análise de fatores relacionados à morbimortalidade: Revista do Colégio Brasileiro de Cirurgiões, 2008; 35(2); 94-102 [in Portuguese]
11.. Butler E, Carlson E, Pain in the testicles: A symptom of retroperitoneal traumatic rupture of the duodenum: Am J Surg, 1931; 11(1); 118
12.. Bhattacharjee HK, Misra MC, Kumar S, Bansal VK, Duodenal perforation following blunt abdominal trauma: J Emerg Trauma Shock, 2011; 4(4); 514-17
13.. Joseph DK, Kunac A, Kinler RL, Diagnosing blunt hollow viscus injury: Is computed tomography the answer?: Am J Surg, 2013; 205(4); 414-18
14.. Brofman N, Atri M, Hanson JM, Evaluation of bowel and mesenteric blunt trauma with multidetector CT: Radiographics, 2006; 26(4); 1119-31
15.. Kunin JR, Korobkin M, Ellis JH, Duodenal injuries caused by blunt abdominal trauma: Value of CT in differentiating perforation from hematoma: Am J Roentgenol, 1993; 160(6); 1221-23
16.. Asensio JA, Petrone P, Roldán G, El grado de lesión en la escala AAST-OIS establece el pronóstico para los traumatismos duodenales: Rev Argent Cir, 2002; 82(1/2); 6-10 [in Portuguese]
17.. Lamberts SW, van der Lely AJ, de Herder WW, Hofland LJ, Octreotide: N Engl J Med, 1996; 334(4); 246-54
18.. Ivanov PA, Grishin AV, [Surgical tactics in duodenal trauma.]: Khirurgiia (Mosk), 2004(12); 28-34 [in Russian]
19.. Ivanov PA, Grishin AV, Korneev DA, Ziniakov SA, [Injuries of pancreatoduodenal organs]: Khirurgiia (Mosk), 2003(12); 39-43 [in Russian]
20.. Mullins AP, Blumenthal SR, Hollenbeck JI, Messick WJ, Octreotide versus pyloric exclusion in reducing gastrointestinal secretions entering the duodenum in a canine model: Am J Surg, 1995; 61(2); 182-84
21.. Amirata E, Livingston DH, Elcavage J, Octreotide acetate decreases pancreatic complications after pancreatic trauma: Am J Surg, 1994; 168(4); 345-47
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133