01 November 2021: Articles 
Rickets Due to Severe Vitamin D and Calcium Deficiency During the COVID-19 Pandemic in Malaysia
Challenging differential diagnosis
Nurul Izzah Sodri1ABCDEF, Mohamed-Syarif Mohamed-YassinDOI: 10.12659/AJCR.934216
Am J Case Rep 2021; 22:e934216
Abstract
BACKGROUND: Rickets is the deficiency in mineralization of the bone associated with lack of sunlight exposure and inadequate dietary calcium and/or vitamin D in children. Important efforts to eradicate rickets include appropriate sunlight exposure advice and fortification of food and milk with vitamin D. However, there is a growing concern that the current Coronavirus Disease 2019 (COVID-19) pandemic will increase the incidence of rickets due to inadequate sunlight exposure resulting from movement restriction measures imposed by governments across the world.
CASE REPORT: A 22-month-old girl presented to our primary care clinic in Selangor, Malaysia with abnormal gait and bowing of the legs during the COVID-19 pandemic. She had a history of inadequate sun exposure as she lived in an apartment and there was a Movement Control Order in place because of the pandemic. Calcium intake was also poor as she could not tolerate formula milk and did not consume any other dairy products. Investigations revealed severe hypocalcemia and low vitamin D level. She was diagnosed with nutritional rickets and was referred for admission to correct the hypocalcemia. She was subsequently discharged with oral calcium and vitamin D supplementation. Her calcium and vitamin D levels improved and at her 6-month review, her bilateral bowed legs had improved significantly.
CONCLUSIONS: This case highlights the importance of having a high degree of suspicion for vitamin D deficiency and rickets in young children growing up during the COVID-19 pandemic. Public health messages on preventing the spread of COVID-19 should also be interlaced with messages addressing the possible effects of our new norms such as inadequate sunlight exposure.
Keywords: COVID-19, Hypocalcemia, Rickets, Vitamin D Deficiency, COVID-19, Child, Child, Preschool, Female, Humans, Infant, Malaysia, Pandemics, SARS-CoV-2, Vitamin D
Background
Rickets is a disease characterized by failure of the mineralization of the growth plate and osteoid matrix causing skeletal disorder in growing children [1,2]. Nutritional rickets is associated with inadequate sunlight exposure or insufficient dietary intake of either calcium, vitamin D, or both [1–4]. Vitamin D plays a vital role in the absorption and utilization of dietary calcium. It also maintains the normal serum level of calcium by stimulating the release of parathyroid hormone for bone resorption when there is a low calcium level [4]. The main source of vitamin D is exposure to natural sunlight, as vitamin D3 is produced in the human skin following exposure to ultraviolet B (UVB) light [5]. Vitamin D can also be found in specific food such as mackerel, salmon, and fortified formula milk or cereals [5]. Malaysian guidelines recommend a daily vitamin D in-take of 400 IU (10 µg) for infants and 600 IU (15 µg) for children and adults [6].
Prior to the start of the COVID-19 pandemic in 2020, there were varying reports of the prevalence of nutritional rickets in many countries worldwide. These ranged from 1% to more than 50%, possibly due to the different methods of diagnosis used in the studies, either only clinical diagnosis or involving radiography and laboratory data, and possibly also due to the geographical area analyzed [4]. The COVID-19 pandemic has prompted governments across the world, including Malaysia, to implement non-pharmaceutical interventions, such as national lockdowns, travel restrictions, and school closure, to curb the spread of the virus [7]. Although effective in decreasing COVID-19 cases, lockdowns and school closure have been reported to adversely affect children’s health and well-being [8]. This case report presents an example of this, in which nutritional rickets was diagnosed in a child who had limited dietary calcium intake and sunlight exposure. It highlights the importance of having a high degree of suspicion for rickets in a patient who presents with bowed legs during the pandemic.
Case Report
A 22-month-old Malay girl was brought by her mother to an urban academic primary care clinic in Selangor, Malaysia, in November 2020 with concerns regarding the shape of her child’s legs and her abnormal gait. These were noticed by family members for a few months prior to the clinic visit. She began to walk at 13 months old, but her parents could not recall any obvious abnormality of her legs at that time. The child was otherwise well and active at home. There was no fever, history of seizures, diarrhea, or other systemic problems. She was born via spontaneous vertex delivery at term, with a normal birth weight of 3.56 kg. Her perinatal period was uncomplicated, and she was up to date with her immunizations. She had no significant past medical history except for a one-week hospital admission for pneumonia when she was 1 year old. There was no history of rickets or other genetic diseases in the family. Her development was consistent with her age in the gross motor, fine motor, speech, and social domains.
According to her mother, she had been eating the same diet that her family ate, with supplementary expressed and directly-fed breast milk as she developed rashes from drinking formula milk. However, a detailed dietary history revealed low calcium and vitamin D intake. She only drank 120 ml of expressed breast milk during the day and did not consume any dairy products. She lived with her parents and a 7-year-old sister in an apartment. During the day, when both parents worked, she was sent to her babysitter’s apartment. Further questioning revealed that she had minimal exposure to sunlight, and her mother stated the girl had less than 2 h of sun exposure per week. There were no outdoor activities or visits to the park due to the Movement Control Order enforced by the Malaysian government in view of the COVID-19 pandemic.
On examination, she was active, but walked with a waddling gait. Her height was 75 cm, weight was 9.5 kg, and both were between the 3rd to 10th centile for her age. Her head circumference was 47 cm, which was in the 25th centile for her age. Her vital signs were within normal ranges. There was noticeable bilateral symmetrical bowing of her legs (Figure 1). There was also a small, non-tender swelling noted over both wrists. The rest of her examination results were unremarkable.
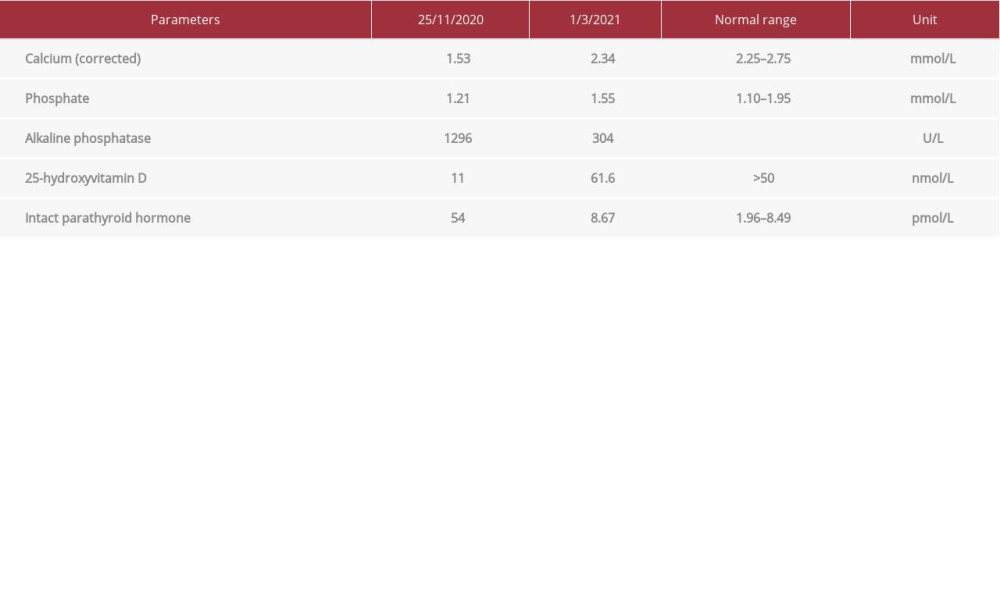
Blood investigations sent urgently revealed severe hypocalcemia with a corrected calcium level of 1.53 mmol/L (normal: 2.25–2.75 mmol/L), but a normal phosphate level of 1.21 mmol/L (normal: 1.10–1.95 mmol/L) (Table 1). Alkaline phosphatase was very high at 1296 U/L (normal: <281 U/L). Her hemoglobin level was 11.0 g/dL, which was within normal range (normal: 11.0–14.1 g/dL), renal profile was normal, and creatinine was 24 µmol/L (normal: 21–36 µmol/L). An X-ray of the left hand and forearm showed fraying and splaying of the radial and ulnar metaphyses, which is a feature of rickets. There was also concavity or “cupping” of both metaphyses (Figure 2). There was no acute fracture or joint dislocation. An X-ray of the lower limbs showed bowing of bilateral legs and widened metaphyses on bilateral knee joints (Figure 3). An ECG was not performed as she was already at home when her investigation results were available. Only her father came to collect the referral letter from our clinic and brought her urgently to the nearby emergency department.
She was referred to the nearest hospital for further management of her severe hypocalcemia on the background of possible nutritional rickets with vitamin D deficiency. She was admitted and received intravenous calcium gluconate 4.8 ml every 6 h for 1 day (0.5 ml/kg/dose) under close observation.
Subsequently, her calcium level improved to 2.02 mmol/L on day 3 of admission. She was discharged with oral calcium carbonate 500 mg 3 times daily (elemental calcium 60 mg/kg/day), oral calcitriol 0.5 mcg once daily for 2 weeks (50 ng/kg/day), and oral cholecalciferol 2000 IU once daily. Subsequently, her results returned with a very low level of 25-hydroxyvitamin D at 11 nmol/L (normal: >50 nmol/L), while the intact parathyroid hormone level was very high at 54 pmol/L (normal: 1.96–8.49 pmol/L). She was also referred for regular follow-up at the pediatric endocrinology clinic. Her mother’s 25-hydroxyvitamin D level was also checked and was found to be 32 nmol/L (normal: >50 nmol/L). She remained asymptomatic and was counseled for further treatment and follow-up.
Six months after the child’s first presentation to this primary care clinic, the bowing of her legs had improved (Figure 4). Her calcium and vitamin D levels also showed marked improvement (Table 1). In June 2021, she was still having regular pediatric endocrinology follow-up every 3 months. She continued taking oral calcium (elemental calcium 35 mg/kg/day) and vitamin D supplements 800 IU once daily. To ensure adequate sun exposure, her parents had started bringing her outdoors to play for about 30 min a day most days of the week. Her parents were also advised to increase her dietary calcium intake by including other dairy products in her diet, such as cheese and yogurt.
Discussion
Nutritional rickets is defined as the disorder of defective chondrocyte differentiation and defective osteoid mineralization, due to low calcium intake and/or vitamin D deficiency in children [2]. Other types of rickets include genetically inherited rickets due to defects in vitamin D metabolism, renal rickets, familial hypophosphatemic rickets, and rickets caused by malignancy [9]. The most common cause of rickets is vitamin D deficiency [10,11]. A recent study in China, which reviewed the effect of pandemic-related confinement on vitamin D levels in children aged 6 years and below, found that decreased sunlight exposure during confinement was associated with lower vitamin D levels in children aged 3 to 6 years [12]. A Polish study found a significant reduction in serum vitamin D levels in a total of 1472 children studied due to COVID-19 pandemic restrictions [13]. However, further studies are needed to determine whether there is increased prevalence of rickets during the COVID-19 pandemic.
The reported prevalence of nutritional rickets varies among countries. A study on a tea farm population in India in 2016 involving 16 274 children aged 1 to 18 years old reported 2.7 cases of nutritional rickets per 1000 children [14]. There are limited data on the prevalence of rickets in Malaysia. Interestingly, there was a case report published in 2016 about a 2.5-year-old Malay boy with vitamin D-deficiency rickets who, like our patient, lived in an apartment and spent most of his time indoors [15]. His 25-hydroxyvitamin D level was low (26 nmol/L) but calcium level was normal.
Rickets can be diagnosed based on detailed clinical history, physical examination, and biochemical tests, and can be confirmed by radiographs [2,4,9]. A comprehensive history is important to assess for nutritional rickets. This includes a child’s gestational age, amount of sunlight exposure, and a detailed dietary history specifically regarding vitamin D and calcium intake [1,9]. Genetically inherited rickets should be suspected if there is a family history of short stature, poor dentition, orthopedic abnormalities, alopecia, or parental consanguinity [1]. Another differential diagnosis that needs to be considered is renal rickets secondary to chronic kidney disease, which was unlikely in our case as the patient had a normal renal profile and was not anemic.
Patients with nutritional rickets can present with varying clinical features, which can be severe, including softening of the skull bones in infants, swelling of the wrists, lower limb deformities, and inability to walk in older children [2,4]. Nonosseous manifestations include convulsions, muscular hypotonia, dilated cardiomyopathy, and failure to thrive [2,4]. In the present case, the patient did not have any other symptoms of severe hypocalcemia such as muscle cramps or seizures but presented with bowing of the legs and abnormal gait. Bow legs, also referred to as genu varum, may be physiological in the first 2 years of life provided there is absence of other findings [1]. However, rickets should be suspected in cases associated with asymmetry, pain, or progression in bowing severity, especially in older children [1].
The laboratory investigation findings that are seen in nutritional rickets include decreases in vitamin D level and serum calcium, and elevations in parathyroid hormone and alkaline phosphatase levels, all of which were present in this patient [1]. Radiographic changes in nutritional rickets include osteopenia, cortical thinning of long bones, widening of growth plates, and an irregular metaphyseal outline such as widening, cupping, or fraying, especially over the wrists in infants and young children [4].
Nutritional rickets is most commonly associated with lack of sunlight exposure and also dietary calcium and vitamin D deficiency. Thus, it can be prevented with appropriate sunlight exposure and adequate dietary intake [2,4]. Studies have suggested that an adequate amount of sunlight exposure for infants is about 2 h a week if fully-clothed, but the exact minimum amount required for a specific child is not known [1]. Unfortunately, due to her living conditions and the movement restrictions put in place by the Malaysian government, this patient did not receive adequate sunlight exposure. Starting from March 18, 2020, a Movement Control Order (MCO) was implemented in Malaysia by the government to limit the spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which included restriction of movement of people into or out of an area. Public parks and schools were closed during this time and people were advised to stay at home to reduce the risk of spreading the infection [16]. In addition, she had inadequate dietary intake of calcium and vitamin D, which led her to develop rickets. A similar case was recently reported in Sri Lanka, which also highlighted vitamin D deficiency rickets during the COVID-19 pandemic [17], but that patient had a normal calcium level.
To prevent rickets, the Global Consensus Recommendations on Prevention and Management of Nutritional Rickets suggested that supplementation of 400 IU per day (10 µg) of vitamin D is sufficient and is suggested for all infants from birth to 12 months old, regardless of their mode of feeding [2]. They also suggested that everyone above 12 months old needs to meet their vitamin D requirement of at least 600 IU per day (15 µg) either through diet or supplementation. This is similar to the recommended level of vitamin D and calcium intake for Malaysians [18]. In the absence of food fortification, candidates for preventative vitamin D supplementation after age 12 months include children with a history of symptomatic vitamin D deficiency requiring treatment, children and adults at elevated risk of vitamin D deficiency, or with factors that decrease consumption or production of vitamin D, and pregnant women [2]. However, these recommendations are not yet widely implemented in Malaysia. Moving forward, physicians can help prevent rickets by identifying high-risk children, especially infants who are exclusively breastfed, and providing them with vitamin D supplementation [1]. Asking specifically about sunlight exposure during this pandemic is also important to identify those at risk of vitamin D deficiency, who may need supplementation [12].
Conclusions
In conclusion, having a high degree of suspicion for vitamin D deficiency and nutritional rickets in young children growing up during the COVID-19 pandemic is important, as movement restrictions may prevent adequate sunlight exposure. Public health messages on preventing the spread of SARSCoV-2 should also be interlaced with messages addressing the possible effects of our new norms such as inadequate sunlight exposure.
Figures
References:
1.. Nield LS, Mahajan P, Joshi A, Kamat D, Rickets: Not a disease of the past: Am Fam Physician, 2006; 74(4); 619-26
2.. Munns CF, Shaw N, Kiely M, Global consensus recommendations on prevention and management of nutritional rickets: J Clin Endocrinol Metab, 2016; 101(2); 394-415
3.. Pettifor JM, Calcium and vitamin D metabolism in children in developing countries: Ann Nutr Metab, 2014; 64(Suppl.2); 15-22
4.. : Nutritional rickets: A review of disease burden, causes, diagnosis, prevention and treatment, 2019, Geneva, World Health Organisation
5.. Nair R, Maseeh A, Vitamin D: The “sunshine” vitamin: J Pharmacol Pharmacother, 2012; 3(2); 118-26
6.. : A Report of the Technical Working Group on Nutritional Guidelines, 2017, Putrajaya, National Coordinating Committee on Food Nutrition, Ministry of Health Malaysia
7.. Haug N, Geyrhofer L, Londei A, Ranking the effectiveness of worldwide COVID-19 government interventions: Nat Hum Behav, 2020; 4(12); 1303-12
8.. Rajmil L, Hjern A, Boran P, Impact of lockdown and school closure on children’s health and well-being during the first wave of COVID-19: A narrative review: BMJ Paediatr Open, 2021; 5; e001043
9.. Chanchlani R, Nemer P, Sinha R, An overview of rickets in children: Kidney Int Rep, 2020; 5(7); 980-90
10.. Holick MF, Resurrection of vitamin D deficiency and rickets: J Clin Invest, 2006; 116(8); 2062-72
11.. Creo AL, Thacher TD, Pettifor JM, Nutritional rickets around the world: An update: Paediatr Int Child Health, 2017; 37(2); 84-98
12.. Yu L, Ke H-J, Che D, Effect of pandemic-related confinement on vita-min D status among children aged 0–6 years in Guangzhou, China: A cross-sectional study: Risk Manag Healthc Policy, 2020; 13; 2669-75
13.. Rustecka A, Maret J, Drab A, The impact of COVID-19 pandemic during 2020–2021 on the vitamin D serum levels in the paediatric population in Warsaw, Poland: Nutrients, 2021; 13(6); 1990
14.. Chabra T, Tahbildar P, Sharma A, Prevalence of skeletal deformity due to nutritional rickets in children between 1 and 18 years in tea garden community: J Clin Orthop Trauma, 2016; 7(2); 86-89
15.. Ting TH, Devnani AS, Vitamin-D-deficiency rickets even with abundant sunlight – a case to highlight emerging problem: Med J Malaysia, 2016; 71(6); 354-56
16.. Shah AUM, Safri SNA, Thevadas R, COVID-19 outbreak in Malaysia: Actions taken by the Malaysian government: Int J Infect Dis, 2020; 97; 108-16
17.. Liyanage G, de Silva Y, Vitamin D deficiency rickets and COVID-19 pandemic: Case Rep Pediatr, 2021; 2021; 5512668
18.. , Recommended nutrient intakes for Malaysia: A report of the technical working group on nutritional guidelines, 2017, Putrajaya, Ministry of Health Malaysia
Figures
In Press
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943214
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943010
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943687
17 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943070
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250