13 July 2022: Articles 
Whistling Scrotum: An Unusual Presentation of Pneumomediastinum in the Setting of an Open Scrotal Wound
Unusual clinical course
Brant Bickford12AEF*, Andrew J. Berglund23EF, Ronald J. Markert2AEF, Hari PolenakovikDOI: 10.12659/AJCR.936441
Am J Case Rep 2022; 23:e936441
Abstract
BACKGROUND: Pneumoscrotum is a rare clinical occurrence in which air accumulates in the scrotum. The origin of air is primarily from trauma, but spontaneous pneumoscrotum can develop from gastrointestinal or pulmonary sources. Physical examination of pneumoscrotum typically includes crepitus of the perineal region and scrotal swelling and associated findings depending on the origin of the free air. However, pneumoscrotum in the setting of a scrotal wound, which allows air to pass freely outside the body, has not been previously documented in the literature.
CASE REPORT: A 72-year-old man who recently underwent a scrotal incision and drainage for recurrent epididymitis presented to a local emergency room with chief concerns of “whistling scrotum” and dyspnea. The chest CT revealed bilateral pneumothoraces, pneumomediastinum, and excessive subcutaneous emphysema throughout his abdomen, perineum, and scrotum. His scrotum had a dehiscent wound without any gross edema or air trapping contained within the scrotum. He received bilateral chest tubes and subcutaneous air drains with complete resolution of his pneumothoraces. The pneumoscrotum and associated subcutaneous emphysema of the perineum and thighs resolved after a prolonged period, and necessitated additional scrotal surgery.
CONCLUSIONS: Prompt evaluation for source control is necessary with pneumoscrotum, as the source likely requires immediate stabilization or surgical intervention. This case report describes a unique presentation of a common entity (pneumothorax) within pulmonology/critical care in a patient with an open scrotal wound from a recent scrotal procedure, which allowed the air to escape from his abdominal compartment, and resulted in his “scrotal whistling.” It is unclear how the air passing through the scrotum affected the patient’s presentation, such as allowing more air to build up in the subcutaneous tissues versus developing critical illness.
Keywords: Pneumothorax, Scrotum, Subcutaneous Emphysema, Aged, Edema, Genital Diseases, Male, Humans, Male, Mediastinal Emphysema, Singing
Background
Pneumoscrotum, or air within the scrotum, is an abnormal finding that requires further evaluation. Pneumoscrotum includes both pneumatocele and scrotal emphysema. Pneumatocele is air within the tunica vaginalis of the testicle and is often not palpable, while scrotal emphysema has the typical features of scrotal edema and crepitus. Scrotal emphysema can have 3 sources: (1) direct production or introduction of air, such as in Fournier’s gangrene or auto-injection of air into the scrotum, (2) extraperitoneal (lungs, mediastinum, or retroperito-neal space), or (3) intraperitoneal (hollow viscera) [1]. Many anatomical pathways into the scrotum exist that can allow passage of air from pneumothorax or pneumomediastinum into the scrotum, such as embryologic defects in the processus vaginalis (present in 15–30% of male adults), communication via Scarpa’s and Camper’s fascia via connective tissue across abdominal compartments, or diffusion through the inguinal canal [2,3]. The presence of a pneumoscrotum requires prompt identification for source control, stabilizing the patient, supportive care, and an invasive procedure or surgery if clinically indicated.
Subcutaneous emphysema (SE) can be localized or spread throughout the body. Typically, SE resolves spontaneously over days. However, case reports have described massive air buildup causing cardiac or pulmonary decompensation [4]. The mediastinum extends beyond the dimensions of the thoracic outlet to the diaphragm. Vessels, connective tissue, and anatomic structures connect the mediastinum to the retroperitoneal space, submandibular/retropharyngeal spaces, and flanks into the pelvis. Hence, air can hypothetically move from the mediastinum to nearly all body parts, including the scrotum [5]. The presence of a scrotal wound during pneumothorax allowing air to flow outside the body has not been previously reported. A grading system of 1 to 5 has been developed to quantify sub-cutaneous emphysema after pneumothorax, but no literature is available on how air loss via the scrotum affects presentation, management, or outcome [6]. We present a case of bilateral spontaneous pneumothoraces in a patient who had a non-healing scrotal wound from a recent incision and drainage (I&D) of the left hemiscrotum, which allowed the release of air from inside the scrotum to the atmosphere.
Case Report
A 72-year-old man with a past medical history of diabetes, coronary artery disease status-post coronary artery bypass graft, thyroidectomy, and recurrent epididymitis presented to a small local emergency department with chief concerns of dyspnea, facial edema, and “whistling scrotum.” He had no pulmonary disease history and had never smoked. His social history was negative for any illicit drug use. His coronary bypass surgery was performed 2 years prior to his current presentation, without any ongoing coronary complaints. He struggled with recurrent epididymitis for over a year and received several courses of antibiotics, without improvement. Five months before the current presentation, he underwent I&D of the left hemiscrotum but developed a non-healing scrotal wound.
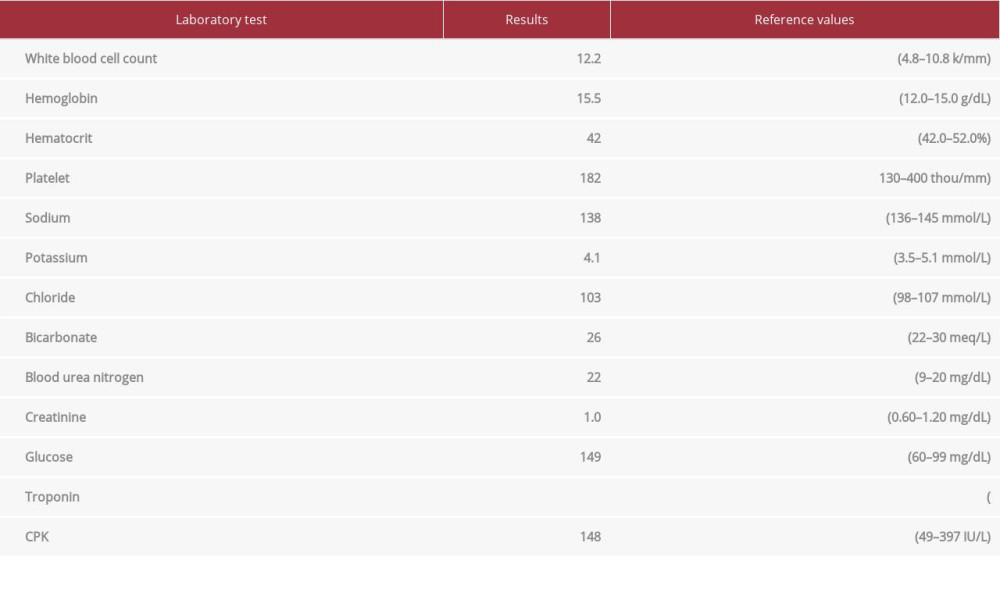
In the emergency department, he was afebrile (37°C), with a heart rate of 80 beats per minute, blood pressure 104/70 mmHg, respiratory rate of 36 breaths per minute with SpO2 of 100% while breathing 2 L/min of oxygen via nasal cannula. He was alert and oriented in mild distress. A physical exam revealed a marked crepitus from head to thigh with bilateral orbital emphysema making it difficult to visualize his left pupil. He had a regular rate and rhythm on cardiac auscultation. Palpable crepitus was appreciated throughout the anterior chest, but without Hamman’s sign or an accessory crunching sound. Respirations were non-labored with decreased breath sounds bilaterally. His scrotum was tender to palpation with a dehis-cent left scrotal wound. The scrotum was not grossly swollen and had no signs of free air or rapid expansion. Routine laboratory results were unremarkable except for mild leukocytosis of 12.2 k/mm3 (Table 1). A chest X-ray disclosed bilateral pneumothoraces, pneumomediastinum, and excessive sub-cutaneous air. Two chest tubes were placed before obtaining computed tomography (CT) of the chest, abdomen, and pelvis. Being in a small local emergency department, he was transferred to a larger regional hospital for further treatment. Upon arrival, concern for worsening of the right-sided pneumothorax prompted a repeat CT chest, abdomen, and pelvis (Figures 1–3). This study revealed that the chest tube was not communicating with the pneumothorax, which had increased in size from the previous report. He had placement of an additional chest tube. On hospital day 3, with resolution of the pneumotho-races, his chest tubes were removed and he was discharged in stable condition.
The pneumoscrotum and associated subcutaneous emphysema of the perineum and thighs took an abnormally long time to resolve. The patient required additional scrotal procedures and eventually needed bilateral orchiectomy. After nearly 2 years, all the subcutaneous emphysema of the perineum and thighs resolved, as noted in the most recent CT scan.
Discussion
Pneumoscrotum is rarely encountered, with the most recent review article by Cochetti et al describing 59 cases in 2015. Cochetti classified pneumoscrotum into 2 categories: spontaneous (1/3 of cases) versus traumatic (eg, after blunt chest trauma, thoracic or abdominal surgery, or gastrointestinal endoscopy). Among the reports of spontaneous pneumoscrotum in the literature, most cases are of gastroenteric origin (46%; eg, perforation of hollow abdominal organs and gas-producing bacterial infections) or due to a pneumothorax (18%) [3]. Originally, our case of pneumoscrotum was thought to be caused by pneumothorax, although the exact mechanism will likely remain unknown. Given the diffuse subcutaneous emphysema, primary spontaneous pneumomediastinum could have been the original cause. However, our patient did not have the traditional risk of being young and did not have chest pain [7]. Air travels along pressure gradients between intra-alveolar and perivascular interstitia, spreading to the neck, abdomen, and, in our case, the scrotum by connecting fascial and anatomic planes [8]. Our patient had previous thyroid removal and CABG that may have altered the traditional pressure gradients between fascial planes allowing for significant facial edema. Furthermore, none of the previously documented pneumoscrotum cases included a route for air to escape from the chest cavity outside the body, which was the case with our patient with an open wound in the scrotum. It is unclear whether this escape route allowed for additional buildup of air within his subcutaneous tissues without causing worsening of the patient’s tension pneumothorax and hemodynamic compromise. Additionally, we cannot claim that there was no influx of air from the scrotum wound prior to the patient’s chief concern of scrotal whistling.
Our patient’s pneumothorax was presumed to be spontaneous in origin, but he did not have the traditional risk factors. He is a never-smoker, of average stature (177 cm), and over 40 years old. One possible mechanism was unidentified subpleural bullae, found in 76–100% of patients during video-assisted thoracoscopic surgery and upwards of 81% on CT imaging in cases of primary pneumothorax [9,10]. Additional consideration for the air origin includes the Macklin effect, in which alveolar tree rupture causes free air to centripetally dissect along the bronchovascular sheaths, toward the pulmonary hila, into the mediastinum [11]. However, this source is typically found in patients younger than ours (ie, those less than 60 years of age). Also, our review of the patient’s history before hospitalization only revealed a single fall, for which he did not seek medical care.
Another intriguing aspect of the case was the time it took for the subcutaneous emphysema of the perineum and thighs to resolve. Our patient’s persistent scrotal wound necessitated repeated urology procedures, including bilateral orchiectomy and antibiotics. He adamantly denied injection of air or other self-instrumentation of the scrotum. Therefore, it is improbable that the air in the scrotum led to the evolution of bilateral pneumothorax. However, we longitudinally followed our patient for 3 years and did not notice any behaviors that aroused the suspicion of a factitious disorder. Furthermore, the subcutaneous air resolved entirely within 2 months from the final urologic procedure.
Conclusions
Pneumoscrotum is a rare clinical entity. When air is present within the scrotum, a prompt evaluation is required for source identification and stabilization of the patient. Taking a detailed history of events leading up to the pneumoscrotum is essential since a significant percentage are of iatrogenic or traumatic origin. Our case of pneumoscrotum from suspected spontaneous bilateral pneumothoraces was unusual. Our patient had an open scrotal wound from a recent scrotal procedure, which allowed the air to escape from his abdominal compartment, and resulted in his concern of “scrotal whistling.” Whether the air escape attenuated the patient’s presentation and led to a more favorable outcome will never be known. Nonetheless, he was successfully treated with multiple chest tubes, subcutaneous air drains, and supportive care.
Figures
References:
1.. Watson H, Klugo R, Coffield K, Pneumoscrotum: Report of two cases and review of mechanisms of its development: Urology, 1992; 40; 517-21
2.. Russo A, Del Vecchio C, Zaottini A, Giangregorio C, Role of emergency thoracic ultrasonography in spontaneous pneumomediastinum. Two case report: G Chir, 2012; 33(8–9); 285-96
3.. Cochetti G, Barillaro F, Cottini E, Pneumoscrotum: Report of two different cases and review of the literature: Ther Clin Risk Manag, 2015; 11; 581-87
4.. Robinson B, Rapid resolution of severe subcutaneous emphysema with simple percutaneous angiocatheter decompression: J Surg Case Rep, 2018; 2018(7); rjy173
5.. Zylak CM, Standen JR, Barnes GR, Zylak CJ, Pneumomediastinum revisited [published correction appears in Radiographics. 2001;21(6):1616]: Radiographics, 2000; 20(4); 1043-57
6.. Aghajanzadeh M, Dehnadi A, Ebrahimi H, Classification and management of subcutaneous emphysema: A 10-year experience: Indian J Surg, 2015; 77; 673-77
7.. Kouritas VK, Papagiannopoulos K, Lazaridis G, Pneumomediastinum: J Thorac Dis, 2015; 7(Suppl. 1); S44-49
8.. Sahn SA, Heffner JE, Spontaneous pneumothorax: N Engl J Med, 2000; 23; 868-74
9.. Bense L, Lewander R, Eklund G, Nonsmoking, non-alpha 1-antitrypsin deficiency-induced emphysema in nonsmokers with healed spontaneous pneumothorax, identified by computed tomography of the lungs: Chest, 1993; 103; 433-38
10.. Tonnesen A, Wagner W, Mackey-Hargadine J, Tension subcutaneous emphysema: Anesthesiology, 1985; 62; 90-92
11.. Wintermark M, Schnyder P, The Macklin effect: A frequent etiology for pneumomediastinum in severe blunt chest trauma: Chest, 2001; 120(2); 543-47
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133