15 October 2022: Articles 
Case of Secondary Syphilis with Mucocutaneous, Articular, and Pulmonary Involvement in a 74-Year-Old Moroccan Man
Challenging differential diagnosis
Ahmed Mougui1ABCDEF*, Zineb Baba1EF, Imane El Bouchti1ABCDEFDOI: 10.12659/AJCR.937513
Am J Case Rep 2022; 23:e937513
Abstract
BACKGROUND: Syphilis is a sexually transmitted infection (STI) caused by Treponema pallidum. If untreated, primary syphilis can progress to secondary syphilis, which has a characteristic rash and diverse systemic features. This report is of a case of secondary syphilis with mucocutaneous, articular, and pulmonary involvement.
CASE REPORT: A 74-year-old Moroccan man presented with an 8-week history of bilateral knee pain and swelling. On examination, he had bilateral knee effusions. Articular puncture brought an inflammatory fluid with a significant presence of white blood cells. Inflammatory markers were elevated. X-rays of both knees showed bilateral osteoarthritis with intra-articular calcification in the left knee. Nonsteroidal anti-inflammatory drugs and colchicine were prescribed, but were ineffective. A closer clinical examination of the patient revealed pigmented papules on the palms, soles, oral mucosa, trunk, and genitals. Treponema pallidum hemagglutination assay and Venereal Disease Research Laboratory results were positive in the blood (titers 1: 32) and joint fluid. A computed tomography scan of the chest revealed a focal opacity in the lateral basal segment of the right lung. The diagnosis of secondary syphilis with mucocutaneous, articular, and pulmonary involvement was made. The evolution was favorable after a single intramuscular injection of benzathine-penicillin.
CONCLUSIONS: Arthritis, mucocutaneous involvement, and lung lesions can be manifestations of secondary syphilis. A detailed anamnesis, clinical examination, serology, and imaging techniques are the pillars of diagnosing this condition.
Keywords: Diagnosis, Arthritis, Skin, syphilis, Aged, Anti-Inflammatory Agents, Colchicine, Humans, Male, Penicillin G Benzathine, Treponema pallidum
Background
Syphilis is an infection caused by contact, usually sexual, with mucosal lesions infected with
Case Report
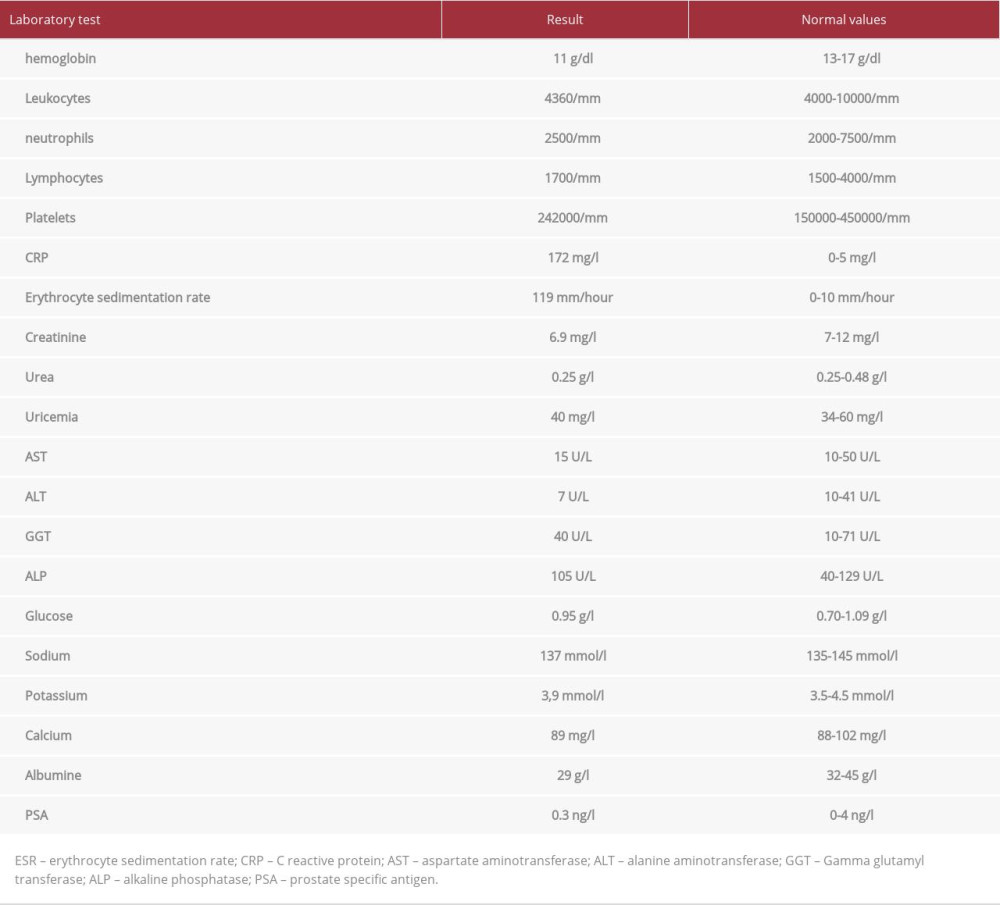
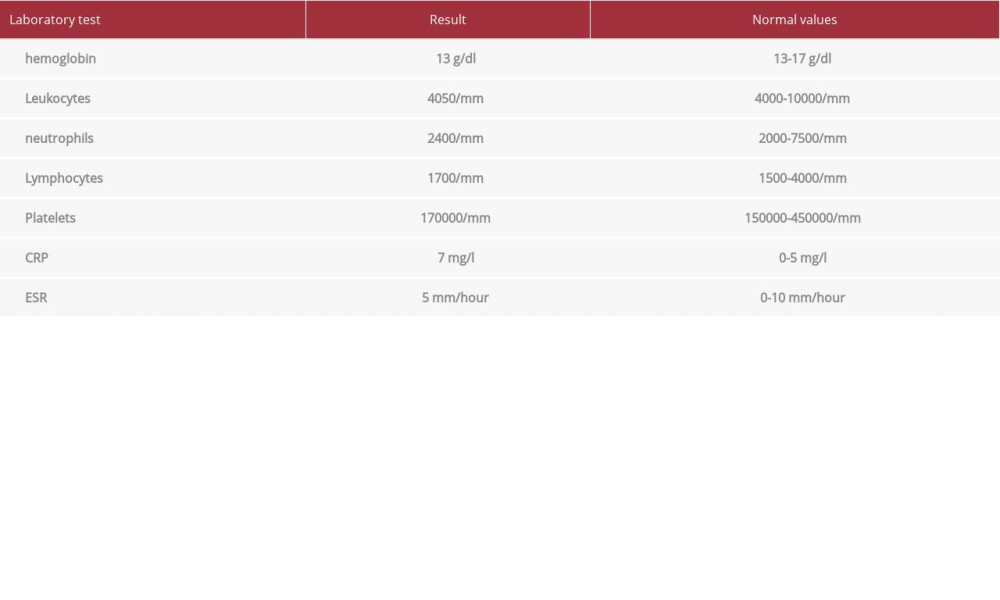
A 74-year-old Moroccan man with no significant medical history was admitted to our hospital for an etiological assessment of bilateral knee pain and swelling that started 8 weeks prior. There were no symptoms of an infection. The patient was afebrile and hemodynamically stable. The osteoarticular examination showed bilateral palpable knee effusion (Figure 1). The articular puncture (Figure 2) brought an inflammatory fluid with a significant presence of white blood cells. A Gram stain, bacterial culture, and search for microcrystals were negative. Blood culture results remained negative. Initial laboratory tests collected at hospital admission showed hypochromic and microcytic anemia, high C-reactive protein level, and high erythrocyte sedimentation rate. The results of the immunological workup, including anti-nuclear antibodies, anti-cyclic citrullinated peptide, rheumatoid factor, and anti-neutrophil cytoplasmic antibody, were negative. All additional laboratory values are shown in Table 1. X-rays of both knees showed bilateral osteoarthritis with intra-articular calcification in the left knee (Figure 3). The diagnosis of pseudo gout was made.
The patient was first put on nonsteroidal anti-inflammatory drugs (NSAIDs) for 7 days (13 days before the later diagnosis) and then colchicine for 5 days (3 days before the later diagnosis), without any improvement. A closer clinical examination of the patient revealed pigmented papules on the palms (Figure 4), soles (Figure 5), oral mucosa, trunk, and genitals. There were no other extra-articular signs. A review of the patient’s history revealed he had unprotected extramarital sexual intercourse 4 months before. He had not noted the presence of genital ulceration. Syphilis serology was performed.
Discussion
Secondary syphilis is a contagious venereal infection responsible for variable and systemic manifestations that give it the characteristics of a “great imitator” [17]. The present case highlights that secondary syphilis can affect several systems, such as dermatological, musculoskeletal, and lung systems. Since 2001, there has been a worrying increase in the incidence of syphilis, aided by the underestimation of risks, increase in alcohol and drug use, development of social networks and dating applications that increase risky sexual activity, and number of sexual partners [18]. This resurgence of the disease underscores the clinician’s interest in knowing its clinical forms, including secondary syphilis [19].
Syphilitic arthritis is reported in congenital and tertiary syphilis [20], but joint involvement in secondary syphilis is rarely reported [5]. The joint disorders in secondary syphilis are polyarthralgia, monoarthritis, or migratory polyarthritis [20], and the most affected joints are the knees, hips, shoulders, and proximal interphalangeal joints [5,6,20,21]. Joint involvement usually occurs 3 to 12 weeks after the onset of the secondary stage [22]. The differential diagnosis of syphilitic arthritis is septic arthritis, rheumatoid arthritis, rheumatic fever, reactive arthritis, psoriatic arthritis, gout, and chondrocalcinosis [5,23]. Other musculoskeletal symptoms of secondary syphilis include bone involvement and tenosynovitis [7,24]. Our patient was admitted for bilateral knee pain and swelling. The presence of chondrocalcinosis led to the initiation of treatment, first with NSAIDs and then with colchicine, without improvement. The
Mucocutaneous involvement is characteristic of secondary syphilis [3,4]. It is symptomized by a copper-red maculo-papular rash of variable size involving the trunk, extremities, and, most frequently, the palms and soles [4,25,26]. As in the case of our patient and reported cases by Crouzy et al [7], the diagnosis of syphilis was made when 1 skin lesion was noticed in the palms and soles, thereby enhancing the importance of a systematic examination of the palms and soles [26]. Other mucocutaneous disorders can occur during secondary syphilis, including ulcerated plaques, painless and serpiginous lesions in the oral cavity, moth-eaten alopecia, which can be revealing, and condyloma lata [4,26,27]. These manifestations concern 25% of patients after 1 to 2 months of primary syphilis [26]. With the current epidemic of syphilis, practitioners will likely encounter these manifestations [5]. Cutaneous lesions resolved 2 to 3 weeks following treatment with benzathine penicillin [7].
Pulmonary involvement during secondary syphilis is rare and can go unnoticed in the absence of chest imaging, as seen in our case [11]. Most patients are asymptomatic or minimally symptomatic, with cough, dyspnea, and chest pain [28], and the clinical and radiological manifestations are not specific [11,28]. Severe acute pneumonia revealed the diagnosis in the case reported by Campos et al [8]. Florencio et al [9] reported syphilitic pulmonary involvement mimicking lymphoma with polyadenopathy and pulmonary nodules. Kassem Youssef et al [10] reported a case of syphilitic pulmonary involvement revealed by dyspnea, with thoracic imaging showing interstitial lung pattern, moderate pleural effusion, and hilar lymphadenopathy. A case of several bilateral, round, excavated opacities and 1 subtracheal adenopathy was reported by David et al [11]. These clinical and radiological manifestations pose a problem of differential diagnosis with several conditions, including cancer, lymphoma, tuberculosis, sarcoidosis, and connective tissue disease [8–11]. The diagnosis of pulmonary syphilis is based on Coleman’s criteria and includes a history or presence of clinical signs consistent with secondary syphilis, pulmonary abnormalities on imaging with or without pulmonary symptoms, positive serological tests for syphilis, exclusion of other pulmonary diseases, and good therapeutic response [28–30]. In our case, bronchoalveolar lavage was unremarkable, and the patient refused a follow-up chest CT scan. In previously reported cases for secondary syphilis involving the lung, a follow-up chest CT scan showed a progressive disappearance of pulmonary lesions after treatment with benzathine penicillin [7,11].
The management of syphilis is based on early diagnosis, prompt and effective treatment of the patient and partners, and patient education to avoid reinfection. The World Health Organization [31], European [32], and United States [33] guidelines for the management of secondary syphilis recommend a single intramuscular injection of benzathine penicillin 2.4 MIU as first-line therapy. Intramuscular procaine penicillin for 10 to 14 days is an alternative treatment. In case of contraindication, the first treatment option is doxycycline 100 mg twice daily for 10 to 14 days. Intramuscular or intravenous injection of 1 to 2 g of ceftriaxone daily for 10 to 14 days is a second option.
Conclusions
Secondary syphilis should be considered in all patients with articular, mucocutaneous, and lung manifestations. Pulmonary involvement is rare and can go unnoticed in the absence of chest imaging. A detailed anamnesis, clinical examination, serology, and imaging techniques are the pillars of the diagnosis.
Figures
References:
1.. O’Byrne P, MacPherson P, Syphilis: Br Med J, 2019; 365; l4159
2.. Patton ME, Su JR, Nelson R, Weinstock H, Primary and secondary syphilis – United States, 2005–2013: Morb Mortal Wkly Rep, 2014; 63(18); 402
3.. Hook EW, Syphilis: Lancet, 2017; 389(10078); 1550-57
4.. Sakthivel P, Kakkar A, Sharma SC, Panda S, Mucocutaneous secondary syphilis: ‘The great imitator’: Am J Med, 2018; 131(2); e57-e58
5.. Ruan XC, Lim JH, Tey HL, Acute inflammatory polyarthritis: A rare presentation of secondary Syphilis: Ann Acad Med Singap, 2017; 46(2); 72-73
6.. Aderinto J, Knight D, Keating JF, Early syphilis: A cause of mono-arthritis of the knee: Ann R Coll Surg Engl, 2008; 90(5); W1-W3
7.. Crouzy F, Alvarez V, Gex G, Troillet N, Unusual presentations and pitfalls of secondary syphilis: Osteitis, pneumonia and malignancy: Br Med J, 2015; 2015; bcr2015210618
8.. Campos J, Ernst G, Simionato C, Ferraro M, [Secondary syphilis with pulmonary involvement]: Medicina (B Aires), 2019; 79(5); 415-18
9.. Florencio KBV, Costa ADD, Viana TCM, Secondary syphilis with pulmonary involvement mimicking lymphoma: A case report: Rev Soc Bras Med Trop, 2019; 52; e20190044
10.. Kassem Youssef H, Blind A, Chouta Ngaha F, Secondary pulmonary syphilis: Case report and review of literature: Ann Dermatol Venereol, 2018; 145(4); 278-87
11.. David G, Perpoint T, Boibieux A, Secondary pulmonary syphilis: Report of a likely case and literature review: Clin Infect Dis, 2006; 42(3); e11-15
12.. Satyaputra F, Hendry S, Braddick M, The laboratory diagnosis of syphilis: J Clin Microbiol, 2021; 59(10); e0010021
13.. Morshed MG, Current trend on syphilis diagnosis: Issues and challenges: Adv Exp Med Biol, 2014; 808; 51-64
14.. Ho EL, Lukehart SA, Syphilis: Using modern approaches to understand an old disease: J Clin Invest, 2011; 121(12); 4584-92
15.. Daskalakis D, Syphilis: Continuing public health and diagnostic challenges: Curr HIV/AIDS Rep, 2008; 5(2); 72-77
16.. Pastuszczak M, Wojas-Pelc A, Current standards for diagnosis and treatment of syphilis: Selection of some practical issues, based on the European (IUSTI) and U.S. (CDC) guidelines: Postepy Dermatol Alergol, 2013; 30(4); 203-10
17.. Afra TP, Handa S, Razmi TM, Vinay K, Secondary syphilis: Lest we forget it: Postgrad Med J, 2018; 94(1113); 415
18.. Bond SM, Blain MLM, Diagnosis and treatment of secondary syphilis in women: J Midwifery Womens Health, 2021; 66(3); 372-79
19.. Balagula Y, Mattei PL, Wisco OJ, The great imitator revisited: The spectrum of atypical cutaneous manifestations of secondary syphilis: Int J Dermatol, 2014; 53(12); 1434-41
20.. Ao X, Chen JH, Kata P, The great impostor did it again: Syphilitic arthritis: Cureus, 2021; 13(8); e17344-e44
21.. Kouassi Djaha JM, Maisonneuve L, de Bandt M, Syphilis, a curable cause of acute polyarthritis: Scand J Rheumatol, 2016; 45(4); 336-37
22.. Reginato AJ, Schumacher HR, Jimenez S, Maurer K, Synovitis in secondary syphilis. Clinical, light, and electron microscopic studies: Arthritis Rheum, 1979; 22(2); 170-76
23.. Zhu K, Zhou Q, Han R, Cheng H, Acute monoarthritis in a delayed diagnosis of syphilis patient with persistent rupioid psoriasis-like lesions: BMC Infect Dis, 2012; 12; 338
24.. Ratnaraj F, Brooks D, Walton M, Forgotten but not gone! Syphilis induced tenosynovitis: Case Rep Infect Dis, 2016; 2016; 7420938
25.. Ghanem KG, Ram S, Rice PA, The modern epidemic of syphilis: N Engl J Med, 2020; 382(9); 845-54
26.. Hughes Y, Do not miss secondary syphilis: Examine the palms and soles: Br Med J Case Rep, 2020; 13(11); e237725
27.. Mattei PL, Beachkofsky TM, Gilson RT, Wisco OJ, Syphilis: A reemerging infection: Am Fam Physician, 2012; 86(5); 433-40
28.. Ohta A, Furusyo N, Kishihara Y, Secondary syphilis with pulmonary involvement: Intern Med, 2018; 57(1); 121-26
29.. Ogawa Y, Imai Y, Yoshihara S, Pulmonary involvement of secondary syphilis: Int J STD AIDS, 2018; 29(1); 89-91
30.. Visuttichaikit S, Suwantarat N, Apisarnthanarak A, Damronglerd P, A case of secondary syphilis with pulmonary involvement and review of the literature: Int J STD AIDS, 2018; 29(10); 1027-32
31.. , WHO guidelines for the treatment of Treponema pallidum (syphilis), 2016
32.. Janier M, Hegyi V, Dupin N, 2014 European guideline on the management of syphilis: J Eur Acad Dermatol Venereol, 2014; 28(12); 1581-93
33.. Workowski KA, Bolan GA, Sexually transmitted diseases treatment guidelines, 2015: MMWR Recomm Rep, 2015; 64(Rr-03); 1-137
Figures
Tables
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133