19 June 2023: Articles 
Bilateral Locked Posterior Fracture-Dislocation of the Shoulder After Epileptic Seizures Secondary to Cavernous Hemangioma: A Case Report and Literature Review
Challenging differential diagnosis, Diagnostic / therapeutic accidents, Management of emergency care, Rare disease
Andreas PangopoulosDOI: 10.12659/AJCR.940141
Am J Case Rep 2023; 24:e940141
Abstract
BACKGROUND: Posterior shoulder dislocation is an uncommon injury, accounting for less than 5% of all glenohumeral dislocations. Bilateral locked posterior shoulder fracture-dislocation is an extremely rare entity with an incidence of 0.6 cases/100 000 people/year. A few reports have been published in the literature, predominantly associated with epileptic seizures.
CASE REPORT: We present a rare case of a 55-year-old male patient with a history of epileptic seizures, who presented with bilateral, locked, posterior fracture-dislocation of the shoulder following an epileptic seizure. The patient was diagnosed with a cavernous hemangioma, which caused his epileptic episode. He was treated operatively, with a modified McLaughlin procedure performed on both sides, at 1 stage, by 2 surgical teams. The cavernous hemangioma was also resected 2 months later. After a follow-up period of 18 months, no recurrent episodes of instability or dislocation were identified. Full range of motion was present on both sides, with good clinical and radiological outcomes. We also conducted a literature review to elucidate the causes of this rare incidence, along with diagnostic workup and treatment options. We were able to identify 36 cases, involving 72 shoulders of bilateral posterior fracture-dislocations in 30 case reports and 2 case series.
CONCLUSIONS: Bilateral posterior fracture-dislocation of the shoulder is uncommon. Treatment strategy depends on the chronicity, involvement of the humeral head, and the patient’s age and functional level. The target is to restore shoulder anatomy and maintain a functional range of motion.
Keywords: Hemangioma, Cavernous, Central Nervous System, Seizures, Shoulder Dislocation, Male, Humans, Middle Aged, Shoulder Fractures, Radiography, fracture dislocation, Hemangioma, Cavernous
Background
Posterior shoulder dislocation is an uncommon injury, accounting for less than 5% of all glenohumeral dislocations [1]. However, acute bilateral locked posterior fracture-dislocation is extremely rare, with an incidence of 0.6 cases per 100 000 people per year [2]. Diagnosis can be challenging in chronic cases; a thorough history-taking and clinical examination are essential. Misdiagnosis occurs in almost 50% of all cases [3]. Patients with a fixed internal rotation deformity, a palpable prominence of the coracoid, an enlarged palpable prominence of the humeral head in the posterior portion of the shoulder, or a noticeable total lack of external rotation should be suspected of chronic posterior shoulder dislocation [4]. Specific radiographic views such as the lateral scapular view or axillary view are mandatory due to a lack of sensitivity from the classic anteroposterior (AP) view, which is often misinterpreted. However, computed tomography (CT) is the modality of choice, as it provides a clear visualization of the lesions, confirms the diagnosis, and assists in the determination of treatment strategy [5]. Treatment options vary, from conservative to surgical methods [1,2,5]. The decision is made based on several factors such as chronicity, humeral defect percentage, and the patient’s profile. Cavernous hemangioma, also known as cavernoma or cerebral cavernous angioma, is a hemorrhagic vascular lesion associated with a developmental venous anomaly. Epileptic seizure is the most common clinical symptom, although about 50% of all cases are completely asymptomatic [6].
This article presents a rare case of bilateral locked posterior shoulder fracture-dislocation after epileptic seizures due to cavernous hemangioma, which was successfully treated with a modified McLaughlin procedure performed at 1 stage.
Case Report
The patient, a 55-year-old man, came to the Accident and Emergency Department of our hospital reporting bilateral shoulder pain. He had a history of epileptic seizures from the age of 17 years and he was receiving antiepileptic medication with carbamazepine until 2 years ago, when he spontaneously quit his treatment. His last epileptic episode before the most recent one was 5 years ago. The patient described an epileptic episode 24 hours ago that lasted several minutes. Since then, he had acute pain, swelling, and restricted range of motion on both shoulders. The patient was hemodynamically stable with normal vital signs and no alternation of consciousness. Both shoulders were locked in internal rotation, with almost complete loss of external rotation (the right shoulder had a −35° external deficit and the left −30°). The absence of normal glenohumeral joint contour was observed bilaterally, and an increased anterior coracoid process prominence was present.
Neurovascular examination of the upper extremities was normal. A high clinical suspicion for bilateral posterior shoulder dislocations was confirmed by routine anteroposterior radiographs (Figure 1A, 1B). CT scans revealed bilateral reverse Hill-Sachs lesions (Figure 1C, 1D). Using the gamma-angle method between the posterior defect edge and the bicipital groove after a best-fit circle placing over the remainder of the humeral articular surface, the bone loss was estimated to be 32% for the right shoulder and 34% for the left. Surgical treatment was proposed, and the patient was admitted to the Orthopedics Department. In addition, a neurological consultation was performed to investigate the potential cause of the epileptic episode. An MRI scan showed a round malformation, approximately 1.3 cm in diameter, located at the right temporal lobe, and at the superior temporal gyrus (Figure 2). The contrast of the gadolinium signal was distributed unevenly, while a hemosiderin ring was also noticed in T2 sequences. The radiologists suggested the presence of a cavernous hemangioma; this was confirmed by neurosurgeons who planned the surgical excision at a later stage, at least 4–6 weeks after shoulder surgery. The reason for that delay was the location, size, and symptoms of the lesion, which was considered mostly as a chronic case than an urgent one; positioning of the patient and unexpected intra- and postoperative complications after cavernous hemangioma resection could possibly alter or delay the optimal approach or timing for the operative treatment of the shoulders.
The surgery was performed on both shoulders 2 days after admission. The patient was placed in a beach chair position under general anesthesia. Both shoulders were prepared and draped in a standard manner. A second-generation cephalosporin (Ceforanide, 2 g, intravenous) was administered for infection prophylaxis. The surgical technique (modified McLaughlin procedure [7]) was identical for both shoulders and was performed by 2 teams (Figure 3A–3D). A deltopectoral approach was utilized to expose the glenohumeral joint. The subscapularis tendon was identified and tagged with Ethibond No. 2 sutures. The lesser tuberosity was osteotomized with the subscapularis elevated to allow visualization of the humeral head. Thorough irrigation of the joint was performed. Two radiolucent, 5.5-mm peek anchors (HEALIX, Depuy-Mitek) were inserted at the base of the defect. Next, the lesser tuberosity was mobilized and fixed into the defect with 2 transosseous horizontal mattress sutures. To enhance stability, the tag suture of the subscapularis was passed transosseously via the humeral head and tied lateral to the bicipital groove. The biceps tendon was inflamed in both shoulders and a soft-tissue biceps tenodesis was performed bilaterally. Full range of motion was obtained intraoperatively. Postoperative radiographs showed well-contoured glenohumeral joints bilaterally (Figure 3E–3J). Postoperatively, wrist and hand exercises were suggested, while both shoulders were immobilized for 6 weeks in a simple sling. External rotation of the shoulder was prohibited during this time. Then, rotator cuff strengthening, and passive, active-assisted, and gradually active ROM exercises were prescribed. No postoperative complications were identified. Two months later, the patient was admitted to the Neurosurgery Department, and he underwent surgical resection of the cavernous hemangioma. After an uncomplicated hospitalization, he was discharged on new antiepileptic medication. After a follow-up period of 18 months, he had a painless almost full range of motion (Right shoulder: 170° forward elevation, 45° internal rotation, and 40° external rotation; Left shoulder: 180° forward elevation, 45° internal rotation, and 45° external rotation). The radiological examination revealed well-contoured shoulder joints (Figure 4). The patient was able to completely return to his preinjury level of activity, with a Constant score of 92 on the right side and 89 on the left side. No epileptic seizure episodes were documented by that time.
Discussion
Bilateral posterior fracture-dislocation is an extremely rare occurrence, first described by Mynter in 1902 [8]. The main causes can be summarized in a so-called ‘triple E syndrome’, described by Brackstone et al: epilepsy (or any convulsive seizure, including ethanol or drug withdrawal seizures), electrocution (including electroconvulsive therapy), and extreme trauma [9]. Epileptic seizures account for over 50% of bilateral posterior dislocations, and this number increases to about 90% when a fracture is present [10]. In 1971, Shaw [11] was the first to address the mechanism of a posterior shoulder dislocation. Adduction, flexion, and internal rotation of the shoulder is the typical position during a seizure episode. Massive, involuntary muscular contractions push the humeral head medially and superiorly on the glenoid fossa, as well as posteriorly and superiorly against the acromion. Infraspinatus and teres minor are the main muscles involved in dislocation, along with the deltoid, latissimus dorsi, and teres major. The humeral head is trapped beneath the glenoid rim at the end of a seizure, frequently with a reversed Hill-Sachs lesion [11]. If the convulsion persists, continued pressure on the humeral head can lead to a complex proximal humerus fracture [12]. More than half of all shoulder lesions in patients with seizures are caused by uncontrolled muscular activity, particularly in younger patients. This frequently results in bilateral lesions, anterior and posterior dislocations, or fracture-dislocations, as in our case. Shoulder injury treatment in epilepsy patients is associated with higher complication rates: recurrent instability was identified in almost two-thirds of patients treated operatively [13]. Rouleau et al reported that humeral head impression fractures – also known as reverse Hill-Sachs lesions – were the most frequently observed fracture type (29%), followed by humeral neck fractures (18.5%) and fractures of the lesser (14.3%) and greater (7.8%) tuberosities, with other fractures (humeral diaphysis, scapula, and clavicle) present in 6% of cases [14].
Diagnosis of bilateral posterior fracture-dislocation is often delayed. A thorough history-taking will raise suspicion for this complication and add the probability of a bilateral fracture-dislocation in the differential diagnosis of ‘painful shoulders’ prior to imaging. A complete trauma series should be performed, including classic anteroposterior, axillary, and scapular lateral views, when tolerated by the patient [15]. Several abnormal radiological signs have been described, such as the ‘light bulb sign’, the ‘rim sign’, and the ‘vacant glenoid sign’ [16]. However, they are challenging to distinguish and are not always present. To properly comprehend the anatomy of the injury and develop the most appropriate treatment plan, CT imaging should be used, as in our case, to determine the size of the humeral defect, the amount of intact articular surface, and any additional fracture lines or fragments [17].
Regarding posterior bilateral fracture-dislocations, there are no established therapeutic guidelines. As a result, management is based on current therapeutic protocols for unilateral injuries. It is commonly acknowledged that the duration of the dislocation, the patient’s age and activity level, the extent of the humeral head defect, the vascularity of the humeral head, and the degree of glenoid erosion all play significant roles in decision-making for posterior fracture-dislocations [18]. The humeral head defect – known as reverse Hill-Sachs lesion – is thought to be the single most relevant factor for posttraumatic recurrent posterior instability. It is generally accepted that defects over 25% require operative intervention to restore stability [19]. In our case, the reverse Hill-Sachs lesion was 32% for the right shoulder and 34% for the left, using the gamma-angle method in the CT images as proposed by Moroder et al [20].
Treatment options include closed reduction, open reduction combined with defect-filling procedures (such as McLaughlin’s), hemiarthroplasty, and total shoulder arthroplasty [1,2,10]. Closed reduction should be considered in acute cases (less than 3 weeks old) with humeral head defects less than 25%. Acute cases involving severe fracture-dislocations and defects larger than 25% of the humeral head require open reduction and further procedures (modified McLaughlin) to achieve stability [7,18,21]. Osteochondral allograft [22] and shoulder replacement are the recommended treatment options for lesions accounting for more than 50% of the humeral head; depending on patient’s age and level of activity, hemi- or total shoulder arthroplasty can be used.
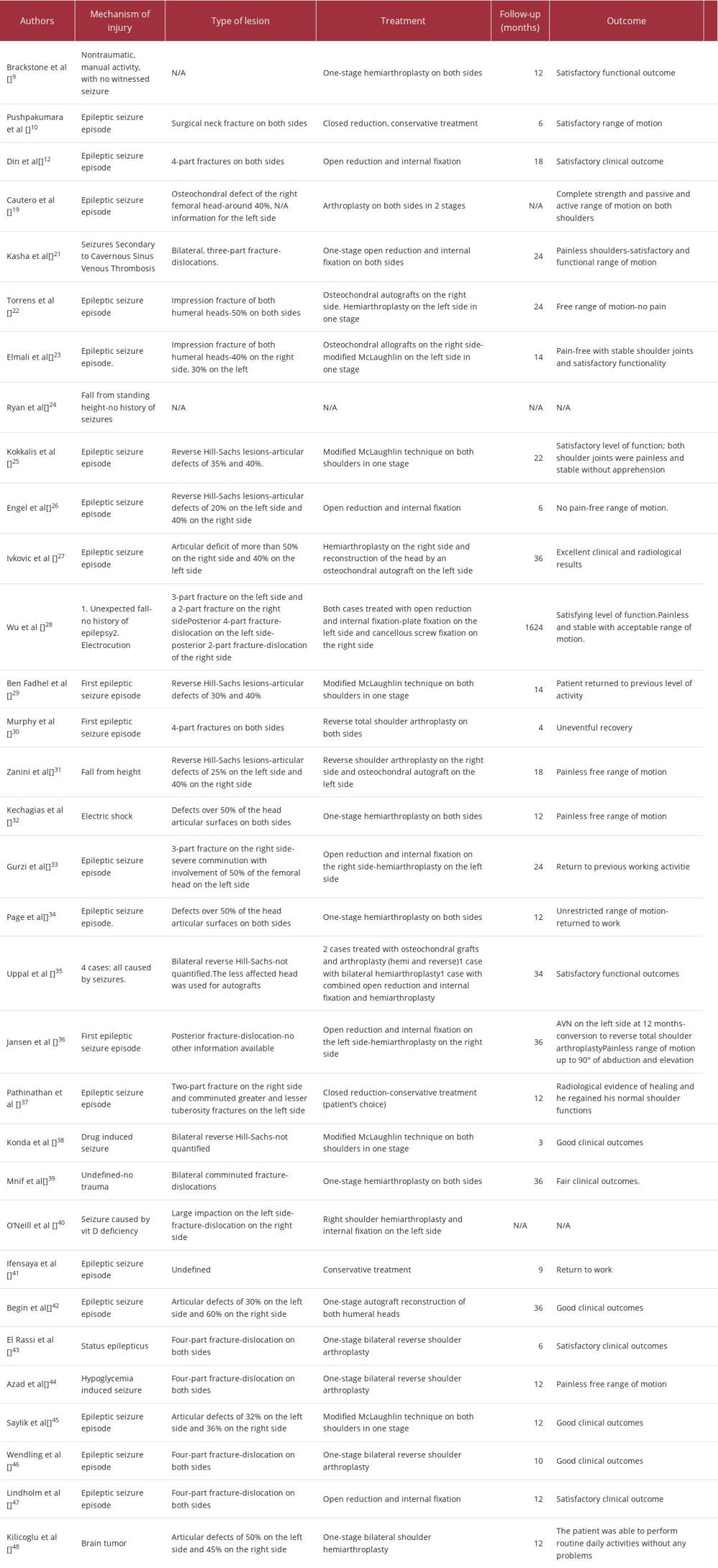
To the best of our knowledge, few case reports regarding posterior bilateral fracture-dislocations have been published in the literature [9,10,12,19,21–48]. Thirty-six cases involving 72 shoulders of bilateral posterior fracture-dislocations have been described so far in 30 case reports and 2 case series (Table 1); 28/36 cases were caused by seizures, 3 by falls from standing height, 2 by electrocution, 1 case by nontraumatic, manual activity, 1 case by brain tumor, and 1 case was undefined. One-stage operation was selected in all cases, except for 1. Three patients were treated conservatively, 1 patient was treated with bilateral autograft reconstruction, 6 patients were treated with open reduction and internal fixation, 11 patients were treated with bilateral shoulder arthroplasty, and 4 patients were treated with bilateral McLaughlin procedure. The other cases were managed with a combination of auto/allograft reconstruction and shoulder arthroplasty in 5 patients, autograft reconstruction and McLaughlin procedure in 1 patient, and open reduction and hemiarthroplasty in 4 patients. Treatment was not reported in 1 case. Uppal et al recommended the use of autograft osteochondral reconstruction combined with various techniques on the contralateral side. They noted that one of the bilateral injured shoulders is often more severely damaged and thus is the preferred donor for a large reverse Hill-Sachs lesion [35]. All cases had satisfactory clinical outcomes and painless free range of motion, with a mean follow-up of 16.1 months (range, 3–36 months), regardless of the treatment selected. Jansen et al described the development on avascular necrosis of the humeral head after open reduction and internal fixation [36]. Their patient underwent conversion to reverse total shoulder arthroplasty with acceptable outcomes. Surprisingly, there is disagreement among authors regarding the surgical intervention selected based on the amount of the humeral head defect. More studies need to be conducted to better understand this rare entity and establish a standardized treatment protocol.
Conclusions
Bilateral posterior fracture-dislocation of the shoulder is rare. Thirty-six cases involving 72 shoulders have been described so far in the literature, of which 78% were caused by seizures. Treatment strategy depends on the chronicity, the extent of the humeral head depression, and the patient’s age and functional level. For acute cases, a 1-stage modified McLaughlin procedure can restore shoulder anatomy and maintain a functional range of motion for both shoulders.
Figures
References:
1.. Robinson CM, Aderinto J, Posterior shoulder dislocations and fracture-dislocations: J Bone Joint Surg Am, 2005; 87(3); 639-50
2.. Robinson CM, Akhtar A, Mitchell M, Beavis C, Complex posterior fracture-dislocation of the shoulder. Epidemiology, injury patterns, and results of operative treatment.: J Bone Joint Surg Am, 2007; 89(7); 1454-66
3.. Jones TP, Beckenbaugh JP, Sperling JW, Your diagnosis? Posterior shoulder dislocation: Orthopedics, 2003; 26(7); 682-746
4.. Wallace WA, Hellier M, Improving radiographs of the injured shoulder: Radiography, 1983; 49; 229-33
5.. Aparicio G, Calvo E, Bonilla L, Neglected traumatic posterior dislocations of the shoulder: Controversies on indications for treatment and new CT scan findings: J Orthop Sci, 2000; 5(1); 37-42
6.. Awad IA, Polster SP, Cavernous angiomas: Deconstructing a neurosurgical disease: J Neurosurg, 2019; 131(1); 1-13
7.. Kokkalis ZT, Mavrogenis AF, Ballas EG, Modified McLaughlin technique for neglected locked posterior dislocation of the shoulder: Orthopedics, 2013; 36(7); e912-e16
8.. Mynter H, XIV. Subacromial dislocation from muscular spasm.: Ann Surg, 1902; 36(1); 117-19
9.. Brackstone M, Patterson SD, Kertesz A, Triple “E” syndrome: Bilateral locked posterior fracture dislocation of the shoulders: Neurology, 2001; 56(10); 1403-4
10.. Pushpakumara J, Sivathiran S, Roshan L, Gunatilake S, Bilateral posterior fracture-dislocation of the shoulders following epileptic seizures: A case report and review of the literature: BMC Res Notes, 2015; 8; 704
11.. Shaw JL, Bilateral posterior fracture-dislocation of the shoulder and other trauma caused by convulsive seizures: J Bone Joint Surg Am, 1971; 53(7); 1437-40
12.. Din KM, Meggitt BF, Bilateral four-part fractures with posterior dislocation of the shoulder. A case report.: J Bone Joint Surg Br, 1983; 65(2); 176-78
13.. Cucchi D, Baumgartner T, Walter SG, Epidemiology and specific features of shoulder injuries in patients affected by epileptic seizures: Arch Orthop Trauma Surg, 2022; 143(4); 1999-2009
14.. Rouleau DM, Hebert-Davies J, Incidence of associated injury in posterior shoulder dislocation: Systematic review of the literature: J Orthop Trauma, 2012; 26(4); 246-51
15.. Neer CS, Displaced proximal humeral fractures. I. Classification and evaluation.: J Bone Joint Surg Am, 1970; 52(6); 1077-89
16.. Arndt Jh, Sears Ad, Posterior dislocation of the shoulder.: Am J Roentgenol Radium Ther Nucl Med, 1965; 94; 639-45
17.. Wadlington VR, Hendrix RW, Rogers LF, Computed tomography of posterior fracture-dislocations of the shoulder: Case reports: J Trauma, 1992; 32(1); 113-15
18.. Kokkalis ZT, Iliopoulos ID, Antoniou G, Posterior shoulder fracture-dislocation: An update with treatment algorithm: Eur J Orthop Surg Traumatol, 2017; 27(3); 285-94
19.. Cautero E, Gervasi E, Locked bilateral posterior fracture-dislocation of the shoulder in an epileptic patient: Case report: Joints, 2014; 2(3); 146-48
20.. Moroder P, Tauber M, Scheibel M, Defect characteristics of reverse Hill-Sachs lesions: Am J Sports Med, 2016; 44(3); 708-14
21.. Kasha S, Bandari G, Bilateral posterior fracture-dislocation of shoulder following seizures secondary to cavernous sinus venous thrombosis – a rare association: J Orthop Case Rep, 2018; 8(4); 49-52
22.. Torrens C, Santana F, Melendo E, Osteochondral autograft and hemiarthroplasty for bilateral locked posterior dislocation of the shoulder: Am J Orthop (Belle Mead NJ), 2012; 41(8); 362-64
23.. Elmalı N, Taşdemir Z, Sağlam F, One-stage surgical treatment of neglected simultaneous bilateral locked posterior dislocation of shoulder: A case report and literature review: Eklem Hastalik Cerrahisi, 2015; 26(3); 175-80
24.. Ryan J, Whitten M, Bilateral locked posterior shoulder dislocation in a footballer: Br J Sports Med, 1997; 31(1); 74-75
25.. Kokkalis ZT, Mavrogenis AF, Ballas EG, Bilateral neglected posterior fracture-dislocation of the shoulders: Orthopedics, 2012; 35(10); e1537-e41
26.. Engel T, Lill H, Korner J, Josten C, Bilateral posterior fracture-dislocation of the shoulder caused by an epileptic seizure – diagnostic, treatment and result: Unfallchirurg, 1999; 102(11); 897-901
27.. Ivkovic A, Boric I, Cicak N, One-stage operation for locked bilateral posterior dislocation of the shoulder: J Bone Joint Surg Br, 2007; 89(6); 825-28
28.. Wu J, Li L, Wang F, Bilateral posterior fracture-dislocation of the shoulders: Two rare case reports and literature review: Medicine (Baltimore), 2020; 99(36); e22088
29.. Ben Fadhel W, Ghrairi R, Sabathe S, Bégué T, Surgical management of bilateral concomitant posterior fracture-dislocation of the shoulder: Trauma Case Rep, 2022; 41; 100691
30.. Murphy JD, Braunlich PR, Bansal M, Bilateral posterior four-part fracture-dislocation of the proximal humerus after first-time seizure: Cureus, 2021; 13(9); e17688
31.. Zanini B, Rusconi M, Fornara P, Grassi FA, Bilateral neglected posterior dislocation of the shoulder treated by reverse arthroplasty and contralateral osteochondral autograft: A case report. Trauma Case Rep, 2021; 33; 100455
32.. Kechagias VA, Katounis CA, Badras SL, Bilateral posterior fracture-dislocation of the shoulder after electrical shock treated with bilateral hemiarthroplasty: A case report: Malays Orthop J, 2022; 16(1); 146-49
33.. Gurzì MD, De Meo D, Pugliese M, Bilateral posterior fracture-dislocation of the shoulder after epileptic seizure: Trauma Case Rep, 2017; 13; 35-41
34.. Page AE, Meinhard BP, Schulz E, Toledano B, Bilateral posterior fracture-dislocation of the shoulders: Management by bilateral shoulder hemiarthroplasties: J Orthop Trauma, 1995; 9(6); 526-29
35.. Uppal HS, Robinson PW, Packham I, Crowther M, The management of bilateral posterior fracture dislocations of the shoulder: A case series illustrating management options: Shoulder Elbow, 2016; 8(2); 111-17
36.. Jansen H, Frey SP, Doht S, Meffert RH, Simultaneous posterior fracture dis -location of the shoulder following epileptic convulsion.: J Surg Case Rep., 2012; 2012(11); rjs017
37.. Pathinathan K, Perera NN, Marasinghe MMGSN, Bilateral fracture-dislocation of the shoulder following a seizure – a case report & review of literature: Ann Med Surg (Lond), 2022; 77; 103646
38.. Konda SR, Fisher N, Gage M, Egol KA, Posterior fracture dislocation of the shoulder: A modified McLaughlin procedure: J Orthop Trauma, 2017; 31(Suppl.3); S36-S37
39.. Mnif H, Koubaa M, Zrig M, Bilateral posterior fracture dislocation of the shoulder: Chir Main, 2010; 29(2); 132-34
40.. O’Neill D, Nair JR, Binymin KA, Simultaneous bilateral posterior fracture dislocation of the shoulders in a young man with unexpected severe vitamin D deficiency: Int J Gen Med, 2012; 5; 399-402
41.. Ifesanya AO, Ogundele OJ, Anejukwo AA, Non-operative treatment of neglected bilateral posterior four-part fracture-dislocation of the shoulders – a case report: Afr J Med Med Sci, 2015; 44(3); 277-81
42.. Begin M, Gagey O, Soubeyrand M, Acute bilateral posterior dislocation of the shoulder: one-stage reconstruction of both humeral heads with cancellous autograft and cartilage preservation: Chir Main, 2012; 31(1); 34-37
43.. El Rassi G, Dib N, Maalouly J, Bilateral reverse total shoulder arthroplasty with soft tissue release for bilateral posterior fracture dislocation after status epilepticus: Case Rep Orthop, 2021; 2021; 5525316
44.. Azad A, Antonios JK, Kang HP, Omid R, Single-stage bilateral reverse total shoulder arthroplasty for bilateral posterior shoulder fracture-dislocation following seizure: A case report: Int J Surg Case Rep, 2020; 73; 298-302
45.. Saylık M, Gökkuş K, Bilateral locked posterior shoulder dislocation overlooked for 15 months treated with the modified McLaughlin procedure: A case report: Jt Dis Relat Surg, 2023; 34(1); 226-33
46.. Wendling A, Vopat ML, Yang SY, Saunders B, Near-simultaneous bilateral reverse total shoulder arthroplasty for the treatment of bilateral fracture dislocations of the shoulder: BMJ Case Rep, 2019; 12(10); e230212
47.. Lindholm TS, Elmstedt E, Bilateral posterior dislocation of the shoulder combined with fracture of the proximal humerus: A case report. Acta Orthop Scand, 1980; 51(3); 485-88
48.. Kilicoglu O, Demirhan M, Yavuzer Y, Alturfan A, Bilateral posterior fracture-dislocation of the shoulder revealing unsuspected brain tumor: Case presentation: J Shoulder Elbow Surg, 2001; 10(1); 95-96
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133