14 November 2021: Articles 
A 2-Month-Old with Kawasaki Disease with Coronary Artery Dilation in the Pre-COVID-19 Era
Challenging differential diagnosis, Rare disease
Frank A. Osei12EF*, Sue Hill2B, Lisa-Gaye Thomas-Messado12EDOI: 10.12659/AJCR.933356
Am J Case Rep 2021; 22:e933356
Abstract
BACKGROUND: Kawasaki disease (KD) is an acute inflammatory vasculitis, which occurs mostly in childhood, predominantly between the ages of 6 months and 5 years. The incidence of coronary artery abnormalities associated with KD has decreased from 25% to 4% as a result of timely diagnosis and treatment with intravenous immunoglobulin (IVIG). Infants ≤6 months of age are the most likely to develop prolonged fever without the other clinical criteria for KD, and diagnosis can sometimes be challenging or delayed. They are therefore at particularly high risk of developing coronary artery abnormalities.
CASE REPORT: A 2-month-old male infant with no significant medical history initially presented with a history of nasal congestion, right conjunctivitis, red lips, and 1 loose stool in the pre-COVID-19 era. He was diagnosed with otitis media and was started on oral amoxicillin. By day 7 of fever, he had developed symptoms and signs and laboratory findings consistent with Kawasaki disease, which is rare in this age group. His echocardiogram showed dilated proximal left anterior descending and right coronary arteries. He was successfully treated, and his most recent echocardiogram, performed 17 months after his treatment, showed remarkable improvement in the coronary arteries.
CONCLUSIONS: Kawasaki disease in children less than 6 months of age is still rare, and the presentation can sometimes make the diagnosis somewhat challenging. Increased clinical suspicion is required for recognition in the youngest patients, as they are more likely to present with few features of KD. Early diagnosis and treatment are needed to prevent or minimize the risk of significant coronary artery abnormalities.
Keywords: Acute Disease, Conjunctivitis, Fever, Infant, Inflammation, COVID-19, Child, Coronary Artery Disease, Coronary Vessels, Dilatation, Humans, Male, Mucocutaneous Lymph Node Syndrome, SARS-CoV-2
Background
Kawasaki disease (KD) is an acute, self-limited febrile illness of unknown cause, which predominantly affects children <5 years of age. The acute febrile phase of KD is characterized by inflammation in the medium-sized arteries and in multiple organs and tissues. It classically presents with fever, conjunctivitis, mucocutaneous lesions, and cervical adenopathy. However, vasculitis of coronary arteries with aneurysm formation can occur. KD is one of the leading causes of acquired cardiovascular diseases in the young. Coronary aneurysms are the most important complication of KD, and young infants have the highest rate of coronary artery aneurysm formation and often present with incomplete clinical criteria [1,2]. The incidence of coronary artery abnormalities associated with KD has decreased from 25% to 4% as a result of timely diagnosis and treatment with intravenous immunoglobulin (IVIG) [3]. The multisystem involvement in KD and the fact that the clinical features may not all be present at a single time, while some clinical features may have resolved in some of the patients who present after 1 to 2 weeks of fever, can delay the timing of the diagnosis or make the diagnosis very challenging. Also, infants ≤6 months of age are the most likely to have prolonged fever without showing the other clinical symptoms of KD and are at a higher risk of developing the typical coronary artery abnormalities associated with KD. Patients with incomplete clinical criteria of KD, especially infants <6 months of age, can experience significant delays in diagnosis [4], which can lead to significant morbidity and mortality.
Timely diagnosis and initiation of IVIG are critical for the prevention of coronary artery aneurysms. We report a case of a 2-month-old who was diagnosed with KD with coronary artery dilation in the pre-COVID-19 era.
Case Report
A 2-month-old male infant with an unremarkable previous medical history initially presented to his primary care provider’s office after 2 days of fever (maximum temperature of 39.1°C) and a 1-week history of nasal congestion and right conjunctival injection. He also had a 1-day history of red lips and 1 loose stool. After evaluation, he was diagnosed with otitis media and was started on oral amoxicillin. He was taken back to the office the following day, which was day 3 of fever, with poor oral intake, more diarrhea, and a maculopapular rash on the trunk, arms, and legs, with more grouped at the back and a few fading papules on the palms and soles. He had a very dry mouth and bleeding and peeling lips. The diagnosis at the office at that time included dehydration, acute right otitis media, and viral conjunctivitis. The patient was therefore admitted for inpatient care on that day.
The main findings on his physical examination on admission included ill-appearing, febrile, soft anterior fontanelle, bilateral conjunctival injection, and cracked, red, bleeding, and peeling lips. He also reportedly had what looked like an ulcer on the anterior portion of his tongue and macular rash, which was more significant in the diaper area and on the back.
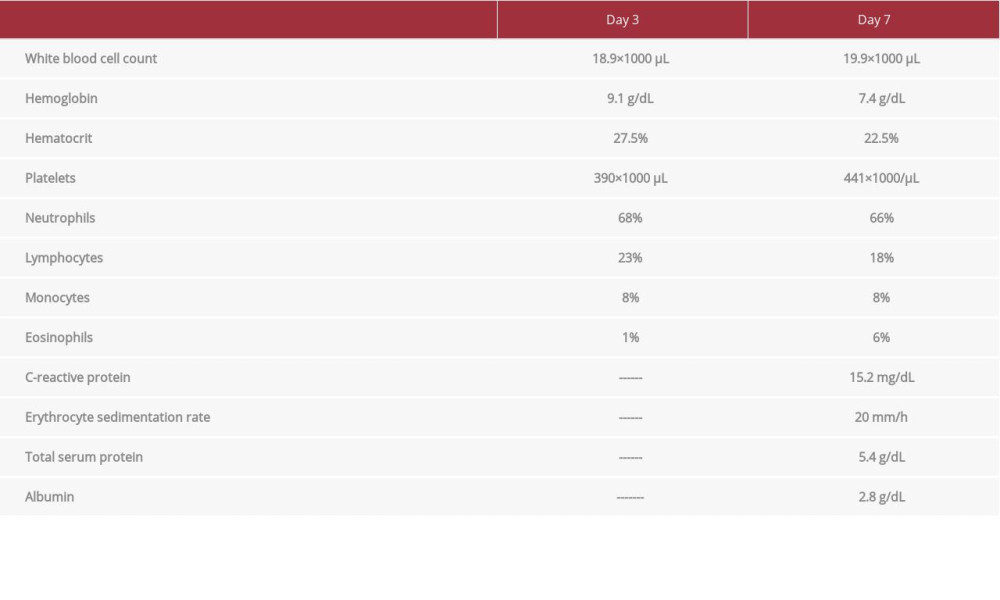
The main findings on his laboratory tests are shown in Table 1. His chest X-ray showed very mild peribronchial cuffing and inter-stitial prominence, without focal infiltrate or pleural pathology. A blood culture was performed, and ceftriaxone was empirically started pending the blood culture results. Cultures were also taken from the eyes and mouth for suspected herpes simplex virus 1, and he was started on acyclovir. The symptoms reportedly appeared to improve by days 4 and 5 of fever, and nothing was isolated from the cultures. Another differential diagnosis that was considered was hand-foot-and-mouth disease, owing to the oral stomatitis and viral exanthem, along with possible contact.
The fever persisted on day 7, and the patient continued to be fussy, even though the parents had the impression that he had improved at that point. Because of the 7-day history of fever, erythematous (polymorphous) maculopapular rash, desquamation in the groin (resolved), erythema of the mouth with red, cracked, and peeling lips, although the tongue looked normal, erythematous conjunctivae, and erythema of the palms and soles, Kawasaki disease was included in the differential diagnosis. The laboratory tests at that point are shown in Table 1, and the rest of his liver and renal function tests were within the reference range. No coagulation studies were performed.
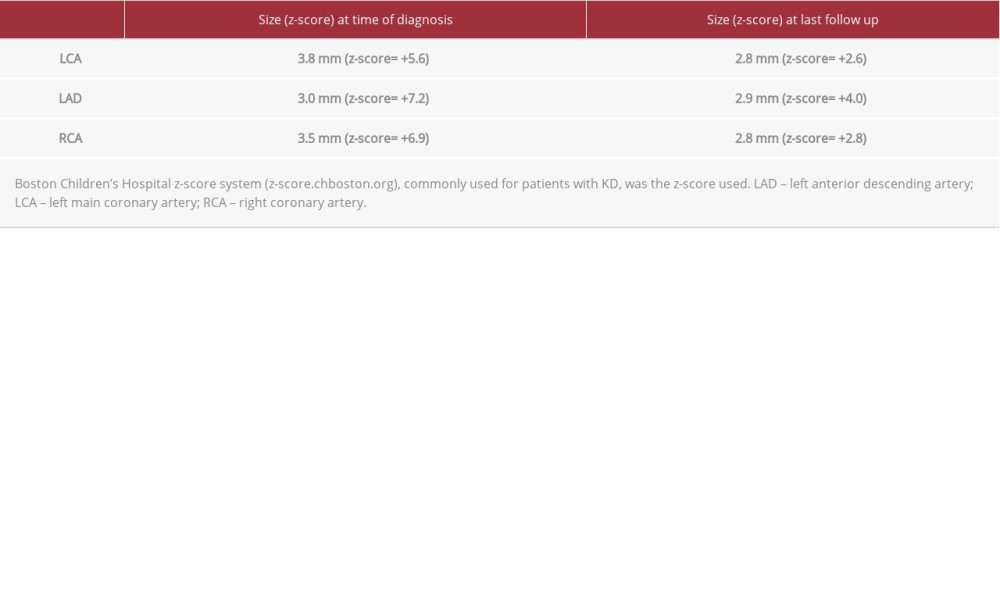
His electrocardiogram was normal, and his echocardiogram showed normal intracardiac anatomy and function but coronary artery abnormalities (Figures 1, 2) and ectasia of the proximal left main coronary artery, left anterior descending artery, and right coronary artery (Table 2). The coronary artery measurements in this case could be classified as medium (z-score ≥5 to <10 and absolute dimension <8 mm), based on the guidelines of the American Heart Association [3]. An abdominal ultrasound for evaluation of the liver and gall bladder were not performed in this case.
The patient received IVIG 2 g/kg as a single infusion over 16 h, with no adverse reaction, and high-dose aspirin 80 mg/kg/day divided every 6 h. He became afebrile, more alert and active the next day and had an improved appetite. His white blood cell count increased to 22.5×1000 µL and his platelet count increased to 532×1000 µL and maximized at 702×1000 µL in the next couple of days. All of the various laboratory parameters improved during the following few days. There was no significant change in his follow-up echocardiograms prior to discharge. He was discharged on low-dose aspirin (ASA) prophylaxis (5 mg/kg/day).
The patient continues to be followed up on an outpatient basis and is still on the ASA prophylaxis. He has been asymptomatic from the cardiac standpoint, and his most recent echocardiogram, which was performed 17 months after his treatment for KD, showed remarkable improvement in the proximal sections of the main coronary arteries (Figures 3, 4; Table 2). There have been no significant changes on his electrocardiogram from the time of initial diagnosis of KD to this report.
Discussion
Coronary artery abnormalities from inflammation are the most important clinical outcomes in KD. During the acute febrile phase of KD, coronary artery abnormalities can occur in addition to inflammation in all the medium-sized arteries and multiple organs and tissues. The acute systemic inflammation associated with KD can lead to findings that include myocarditis, pericarditis, hepatitis, interstitial pneumonitis, aseptic meningitis, irritability, gastrointestinal tract issues, such as abdominal pain, vomiting, and diarrhea, gallbladder hydrops, pyuria lymphadenopathy, and pancreatitis [3,5].
The diagnosis of classic KD requires the presence of fever for at least 5 days (with the day of onset of the fever counting as the first day) in addition to at least 4 of 5 of the following principal clinical findings [3]: (1) bilateral bulbar non-exudative conjunctival injection; (2) oral mucous membrane changes, including erythema or fissured lips, injected pharynx, or strawberry tongue; (3) polymorphous rash; (4) peripheral extremity changes, including erythema of palms or soles, edema of hands or feet (acute phase), or periungual desquamation (convalescent phase); and (5) cervical lymphadenopathy (at least 1 lymph node ≥1.5 cm in diameter), which is usually unilateral.
In the presence of ≥4 principal clinical features, especially when there is redness and swelling of the hands and feet, the diagnosis of KD can be made in the presence of 4 days of fever. Also, in rare cases, experienced clinicians who have treated many patients with KD can make a diagnosis of KD in the presence of 3 days of fever [3].
Prolonged fever and irritability can be the only clinical findings of KD in infants < 6 months of age; therefore, these patients tend to be at a high risk of developing coronary artery abnormalities. Review of the literature on cases of KD published so far showed that the clinical presentation can vary greatly, from cases having the typical symptoms of KD to cases with incomplete clinical criteria with rare presentation and ages of presentation. A literature review by Genizi et al [6] published in 2003 revealed 31 infants in addition to their own 2 cases who were younger than 6 months old, and those 31 cases had been described in 12 articles up to that point. The most common findings were fever >5 days, which occurred in 97% of the cases, and rash, which occurred in 82%. Unfortunately, these symptoms can be found in other conditions as well. Genizi et al found coronary abnormalities in 85% of patients. In the case of a 44-day-old infant with incomplete criteria for KD reported by Nor Aziah et al [7], the presence of unexplained fever for ≥5 days with erythema of a BCG vaccine scar and thrombocytosis on day 2 were key findings before the development of other symptoms over subsequent days. Prior to that publication, Nigrovic et al [8] reported that the presence of unexplained, prolonged fever and extreme thrombocytosis in infants should increase the suspicion for possible KD. There is also a report of a 6-month-old infant with KD that manifested as bilateral facial nerve palsy and meningitis [9]. Other reported neurological complications that tend to be manifest in KD include irritability, cerebral infarction, aseptic meningitis, and sometimes cranial nerve palsy [10]. KD cases presenting with neurologic symptoms are not common, and these symptoms are nonspecific, making timely diagnosis difficult.
Even though fever is a key clinical symptom in KD, there is a report of a 3-month-old male patient who developed the typical presentation of KD and coronary aneurysms in the absence of fever [11]. This also emphasizes the challenges in making the diagnosis of KD in younger infants. The age of the patient should not prevent clinicians from considering KD when patients present with nonspecific symptoms. There are also reported cases in patients as young as 2 weeks old [12]. Therefore, a higher index of suspicion is needed to make the diagnosis of diagnosis of KD in the newborn period. There is a reported case of a 3-month-old infant with severe KD who had a timely diagnosis and was treated with IVIG, but that treatment could not prevent the development of coronary artery aneurysms [13]. Fatamar et al [14] reviewed data on 105 755 patients with KD from the first 12 Japanese nationwide surveys of KD, covering the period from 1970 to 1992. They identified 1768 patients (1.67%) with KD who were 90 days old or younger, and only 6 of those patients were reportedly 30 days old or younger, and the youngest was 26 days old [15]. When the Japanese nationwide surveys of KD from 2001 to 2012 were reviewed, 23 neonates were identified, which represented 0.02% of the overall patients with KD. According to the cases reviewed by Fatamar et al, KD can present as early as the first week of life [14]. The aforementioned varied presentations in KD and incomplete KD cases emphasize the need for clinicians to strongly consider KD in these young infants and not only in the typical age range for KD.
The apparent delay in diagnosis of our patient was due to how he initially presented. It remains unclear whether young infants like this patient have a greater propensity to develop coronary artery aneurysms or if this complication results from delayed diagnosis in incomplete KD. Sometimes the presence of coronary artery aneurysms can be the only definite means of diagnosing incomplete KD.
Fever with upper respiratory symptoms, unilateral conjunctivitis, diagnosis of right otitis media, and age of the patient might have contributed to the delay. The sore on the tongue might also have been misleading when the herpes simplex virus 1 was considered as a differential diagnosis on day 3 of fever. It was also learned that the patient had been exposed to hand-foot-and-mouth disease, which might have compounded the problem of diagnosis, although 2 months of age is not a common age for that disease. When the patient was seen on day 3 of fever with rash, conjunctivitis, and lesions in the mouth, on the lips, and the extremities, a diagnosis of incomplete KD could have been considered, although the criteria were not all met [3]. The patient reportedly improved clinically from days 4 to 6 of fever on the antibiotic and antiviral except for the persistence of the low-grade fever, which might have also been misleading. In a 2-month-old infant, KD would not be one of the top differential diagnoses at that point. In cases like this, a high index of suspicion is required to make a timely diagnosis so that immediate treatment can be started.
In this era of the severe acute respiratory syndrome coronavirus 2 pandemic, with associated COVID-19, there has been a rise in multisystem inflammatory syndrome in children (MIS-C), a condition in which different body parts can become inflamed, including the heart, lungs, kidneys, brain, skin, eyes, and gastrointestinal organs. Some children with MIS-C meet the criteria for complete or incomplete KD, which can also make the diagnosis of KD in older children difficult. Fortunately, the epidemiology of MIS-C differs from that of classic KD. Most MIS-C cases have occurred in older children and adolescents, with a median age of 8 to 11 years (range 1 to 20 years), who were previously healthy [16–18]. By contrast, classic KD typically affects infants and young children.
The following are findings in our patient on day 7 of fever prior to the echocardiogram which were suggestive of KD: erythematous (polymorphous) maculopapular rash and desquamation in the groin (resolved); erythema of the mouth with red, cracked and peeling lips; bilateral conjunctivitis; erythema of palms and soles; and laboratory findings that were indicative of KD, including protein of 15.2 mg/dL; WBC of 19.9×1000 µL; Hgb of 7.4 g/dL; and albumin of 2.8 g/dL.
Most coronary artery abnormalities in children with KD are often identified in the initial echocardiogram and during the first week of illness, and earlier diagnosis and treatment are needed to impact the incidence of the coronary artery abnormalities [19]. The development of coronary artery aneurysms or dilations are thought to decrease when IVIG is administered in the first 10 days of fever in KD [20], but there was already coronary artery dilation on day 7 prior to the IVIG in this patient.
Fortunately, there was no further increase in the coronary artery z-scores, which may or may not have been due to the IVIG treatment. Low-dose ASA was used for antithrombotic prophylaxis after the initial high-dose treatment. According to the guidelines for the diagnosis and treatment of KD [3], ASA prophylaxis can be combined with a thienopyridine, such as clopidogrel, to antagonize the adenosine diphosphate-mediated activation of platelets. Because the coronary artery dilation appeared to be stable and continued to show some improvement in our patient, the low-dose ASA was continued without needing to add another agent.
Conclusions
Kawasaki disease in children younger than 6 months of age is still rare, and the presentation can make the diagnosis somewhat challenging. Increased clinical suspicion is required to recognize KD in the youngest patients, as they are more likely to present with fewer features of KD. Early diagnosis and treatment are needed to prevent or minimize the risk of significant coronary artery abnormalities in that population. This case reinforces the need to remain vigilant and consider KD in the differential diagnosis for any febrile infant who has no clear source of infection.
Figures
References:
1.. Rosenfeld EA, Corydon KE, Shulman ST, Kawasaki disease in infants less than one year of age: J Pediatr, 1995; 126(4); 524-29
2.. Manlhiot C, Yeung RS, Clarizia NA, Kawasaki disease at the extremes of the age spectrum: Pediatrics, 2009; 124(3); e410-15
3.. McCrindle BW, Rowley HA, Newburger JW, Diagnosis, treatment, and long-term management of Kawasaki disease: A scientific statement for health professionals from the American Heart Association: Circulation, 2017; 135(17); e927-99
4.. Minich LL, Sleeper LA, Atz AM, Delayed diagnosis of Kawasaki disease: What are the risk factors?: Pediatrics, 2007; 120(6); e1434-40
5.. Amano S, Hazama F, Kubagawa H, General pathology of Kawasaki disease. On the morphological alterations corresponding to the clinical manifestations: Acta Pathol Jpn, 1980; 30(5); 681-94
6.. Genizi J, Miron D, Spiegel R, Kawasaki disease in very young infants: High prevalence of atypical presentation and coronary arteritis: Clin Pediatr (Phila), 2003; 42(3); 263-67
7.. Nor Azizah A, Thong SP, Hung LC, Incomplete Kawasaki disease in a 44-dayold baby: Med J Malaysia, 2018; 73(4); 257-59
8.. Nigrovic LE, Harper MB, Chiang VM, Extreme thrombocytosis predicts Kawasaki disease in infants: Clin Pediatr (Phila), 2006; 45(5); 446-52
9.. Zhang B, Hao Y, Yang N, Li H, Liang J, Kawasaki disease manifesting as bilateral facial nerve palsy and meningitis: A case report and literature review: J Int Med Res, 2019; 47(8); 4014-18
10.. Chou CP, Lin IC, Kuo KC, A male infant had subdural effusion and paroxysmal supraventricular tachycardia during the febrile episode of Kawasaki disease: A case report and literature review: BMC Pediatr, 2016; 16; 71
11.. Hinze CH, Graham TB, Sutherell JS, Kawasaki disease without fever: Pediatr Infect Dis J, 2009; 28(10); 927-28
12.. Stanley TV, Grimwood K, Classical Kawasaki disease in a neonate: Arch Dis Child Fetal Neonatal Ed, 2002; 86(2); F135-36
13.. Leonardi S, Barone P, Gravina G, Severe Kawasaki disease in a 3-month-old patient: A case report: BMC Res Notes, 2013; 6; 500
14.. Altammar F, Lang B, Kawasaki Disease in the neonate: Case report and literature review: Pediatr Rheumatol Online J, 2018; 16(1); 43
15.. Tsuchida S, Yamanaka T, Tsuchida R, Epidemiology of infant Kawasaki disease with a report of the youngest neonatal case ever reported in Japan: Acta Paediatr, 1996; 85(8); 995-97
16.. Feldstein LR, Rose EB, Horwitz SM, Multisystem inflammatory syndrome in U.S. children and adolescents: N Engl J Med, 2020; 383(4); 334-46
17.. Whittaker E, Bamford A, Kenny J, Clinical characteristics of 58 children with a pediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2: JAMA, 2020; 324(3); 259-69
18.. Davies P, Evans C, Kanthimathinathan HK, Intensive care admissions of children with paediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2 (PIMS-TS) in the UK: a multicentre observational study: Lancet Child Adolesc Health, 2020; 4(9); 669-77
19.. Dominguez SR, Anderson MS, El-Adawy M, Glode MD, Preventing coronary artery abnormalities: A need for earlier diagnosis and treatment of Kawasaki disease: Pediatr Infect Dis J, 2012; 31(12); 1217-20
20.. McCrindle BW, Li JS, Minich LL, Coronary artery involvement in children with Kawasaki disease: Risk factors from analysis of serial normalized measurements: Circulation, 2007; 116(2); 174-79
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133