07 June 2022: Articles 
Thrombotic Microangiopathy Secondary to Systemic Sclerosis with Severe Complement Activation Not Responsive to Eculizumab: A Case Report
Unusual clinical course, Challenging differential diagnosis, Unusual or unexpected effect of treatment, Diagnostic / therapeutic accidents, Unexpected drug reaction
Masahiko Nakamura1ABCDEF*, Tomohiro AbeDOI: 10.12659/AJCR.936116
Am J Case Rep 2022; 23:e936116
Abstract
BACKGROUND: Secondary thrombotic microangiopathies (TMAs) are induced by several underlying conditions and most are resolved by treating the underlying disease. Eculizumab, a human monoclonal antibody, blocks the final stages of the complement system. Several studies have shown that complement C5 monoclonal antibodies are effective in treating secondary TMA. Systemic sclerosis (SSc) is one of the most common causes of secondary TMA, and early diagnosis is important because TMA secondary to SSc has a poor prognosis. We report a case of TMA secondary to SSc that did not respond to eculizumab, despite the presence of severe complement activation.
CASE REPORT: A 61-year-old previously healthy man was admitted for acute renal failure and thrombocytopenia. TMA was suspected because hemolytic anemia, thrombocytopenia, and organ damage were detected. Based on the physical findings, we suspected SSc as the underlying cause. All tests for specific antibodies, including Scl-70, were negative, and C5b-9 levels were markedly elevated (11 041 ng/mL). We initiated plasma exchange on day 3, followed by eculizumab therapy, but with limited improvement. SSc with secondary TMA was identified upon further testing. After completion of the plasma exchange, the platelet count was maintained above 30 000/μL. Creatinine levels gradually decreased, and the patient was weaned off dialysis. Steroid treatment for SSc was continued, and the patient was eventually discharged.
CONCLUSIONS: A case of SSc-TMA was ineffectively treated with eculizumab, despite abnormal activation of the complement system. Continuous monitoring and investigation are required, and discontinuation of eculizumab should be determined according to the final diagnosis.
Keywords: Complement Activation, eculizumab, Plasma Exchange, Scleroderma, Systemic, Thrombotic Microangiopathies, Antibodies, Monoclonal, Humanized, Complement Inactivating Agents, Humans, Male, Middle Aged, Renal Dialysis
Background
Thrombotic microangiopathy (TMA) is characterized by thrombocytopenia, microangiopathic hemolytic anemia, and organ damage. The acute mortality rate of TMA due to delayed treatment is extremely high, and early treatment with plasma exchange and complement inhibitors is required. TMA is mainly classified into 4 types: thrombotic thrombocytopenic purpura (TTP), which is caused by a marked decrease in a disintegrin-like and metalloproteinase with thrombospondin type 1 motifs 13 (ADAMTS13) activity; Shiga toxin-producing
Several diseases and conditions can cause secondary TMA, including collagen diseases, hematopoietic stem cell transplantation [2], medications [2,3], pregnancy [2,4], and infections [5]. Secondary TMAs are caused by vascular endothelial damage via various inflammatory reactions, including complement activation. Rapidly differentiating secondary TMAs is difficult because emergently introducing treatments such as plasma exchange is needed once TMA is diagnosed, regardless of identification of the causative disease. According to some experts, complement activation is important regardless of the type of TMA [6], and several reports state that treatment with a complement C5 monoclonal antibody is effective in secondary TMAs [7].
Systemic sclerosis (SSc) is a cause of secondary TMA [8]. Secondary TMA caused by SSc has a poor prognosis; therefore, early diagnosis is important [9]. Another complication of SSc is scleroderma renal crisis (SRC). The main pathogenesis of SRC is increased blood pressure and systemic vasoconstriction due to decreased renal blood flow and renin released by thickened and proliferated arcuate and interlobular arteries [10]. The main treatments for SRC are angiotensin-converting enzyme inhibitors. SRC occasionally presents with normal blood pressure (normotensive SRC) [11]. In addition to acute kidney injury, patients with SRC show thrombocytopenia and microangiopathic hemolytic anemia [12]. These SRC findings, similar to those of TMA, make the differential diagnosis difficult. Furthermore, there have been reports of SRC complicated by TMA [8].
In this article, we report a case of TMA secondary to SSc that was unresponsive to eculizumab, despite the presence of severe complement activation.
Case Report
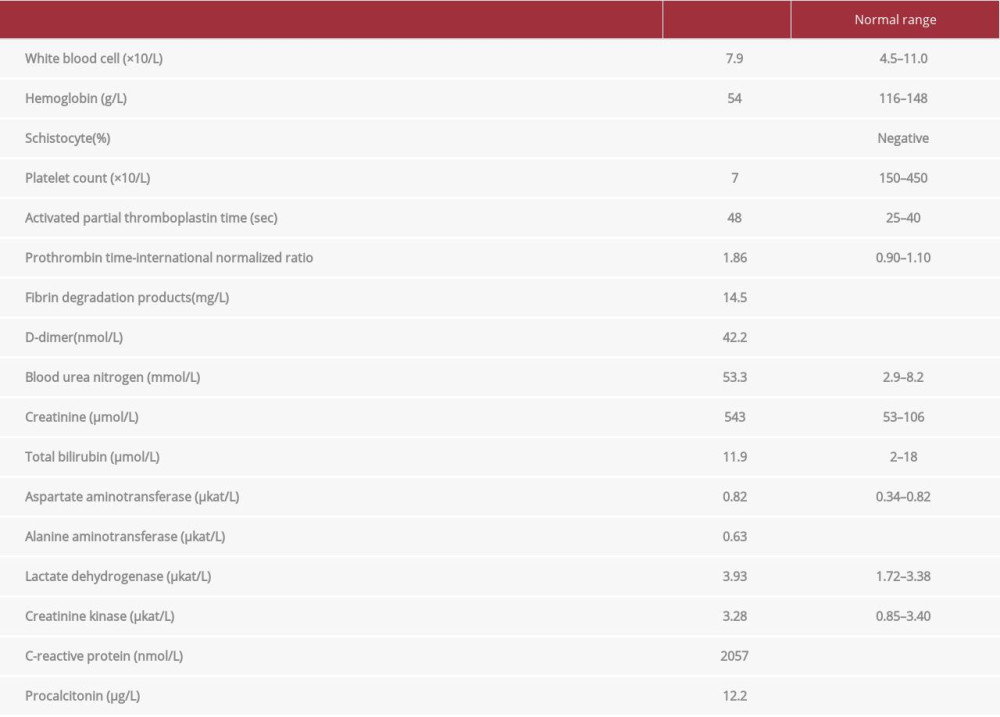
A 61-year-old man with no previous underlying medical condition visited a local clinic because of common cold-like symptoms. The patient had petechiae of unknown onset on his trunk, and returned 11 days later because of constipation and abdominal distension. After being subsequently diagnosed with acute kidney injury and thrombocytopenia, the patient was transferred to our hospital. Upon further examination, the patient’s temperature was 37.2°C, blood pressure was 110/62 mmHg, heart rate was 104 beats/min, respiratory rate was 12 breaths/min, and oxygen saturation was 97% (ambient air). The eyelids and conjunctiva were pale, the tips of the fingers and toes were poorly pigmented (Figure 1), the nails had epithelial hemorrhages, and purpura were present on the trunk and extremities. He had acute kidney injury with a blood urea nitrogen level of 149.4 mg/dL and creatinine level of 6.15 mg/dL, and a platelet count markedly decreased to 7000/μL (Table 1).
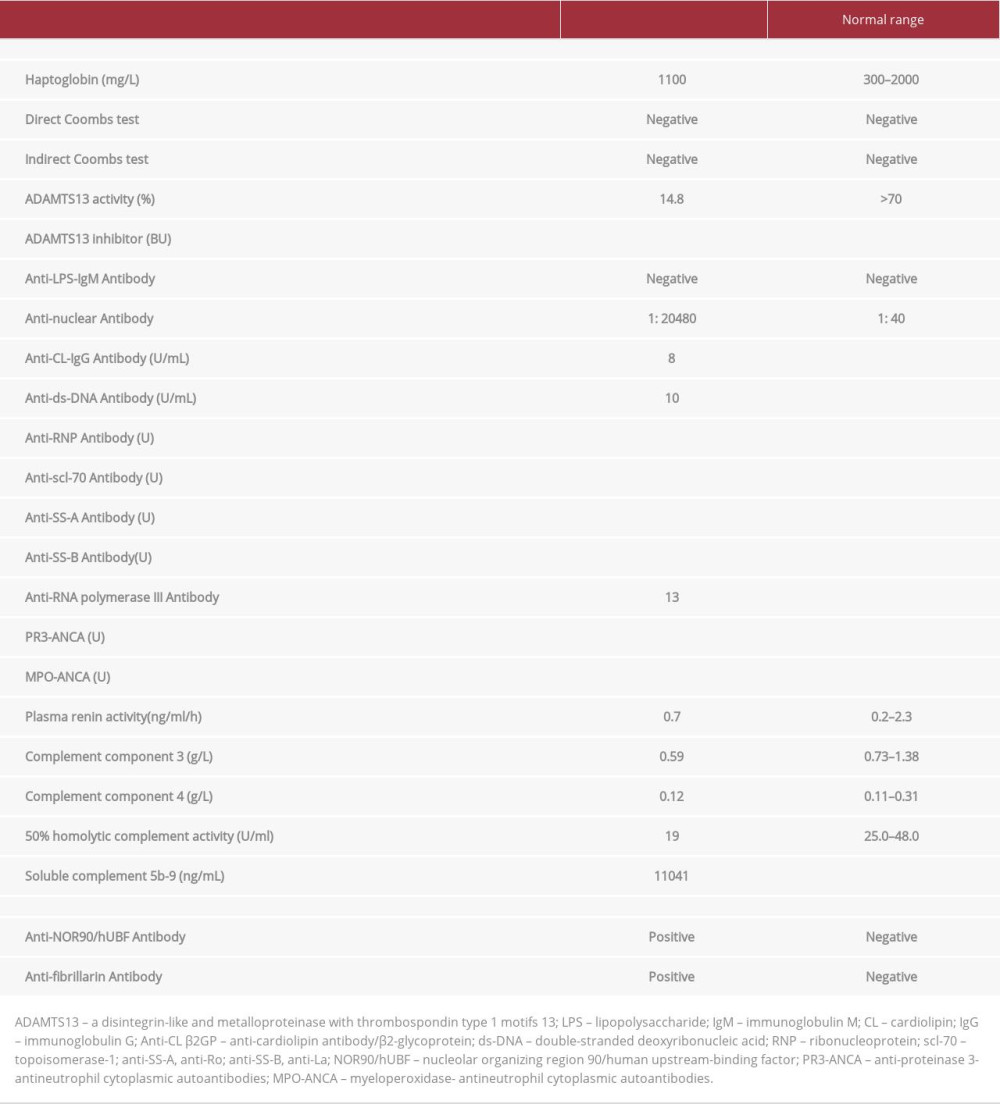
On the basis of the findings of hemolytic anemia, thrombocytopenia, and organ dysfunction, we considered the pathogenesis of TMA. Various tests, including those for ADAMTS13 activity, ADAMTS13 inhibitor, and other diseases causing secondary TMAs, were performed to identify the cause of TMA. We suspected aHUS rather than TTP because the renal impairment was obvious. We initiated continuous hemodiafiltration for acute kidney injury on the day of admission. SSc was suspected because of swelling of the fingers, poorly colored fingertips, and bleeding under the nail fold. No specific antibodies, including the Scl-70 antibody, were detected at the initial screening. On the other hand, the levels of C3 were reduced to 59 mg/dL (reference range 86–160 mg/dL), the levels of C4 were reduced to 12 mg/dL (reference range 17–45 mg/mL), 50% homolytic complement activity was reduced to 19 U/mL (reference range 25–48 U/mL), and soluble C5b-9 was markedly elevated to 11 041 ng/mL (reference range <303 ng/mL), suggesting complement activation. A positive result for occult blood on urinalysis and the presence of schistocytes in the blood smear indicated intravascular hemolysis, although haptoglobin type 2-2 did not decrease (Table 2).
Plasma exchange was initiated on day 3 because of progressive necrosis of the hand. However, the effects of plasma exchange were limited. No abnormalities were found in ADAMTS13 activity or ADAMTS13 inhibitor in the plasma submitted prior to plasma exchange, and no Shiga toxin-producing
On day 48, we obtained the results of additional tests that were positive for antinuclear antibody quantification 20 480 times, anti-centromere antibody 14.4 (+/−), anti-NOR-90 antibody (anti-hUBF antibody), and anti-fibrillarin antibody (anti-U3-RNP antibody). Plasma renin activity levels were normal. Thus, the patient was diagnosed with SSc with secondary TMA. Because the necrosis on the patient’s fingers and toes worsened with interruption of plasma exchange, we performed plasma exchange 24 times until day 64. After the completion of plasma exchange, the platelet count was maintained at >30 000/μL (Figure 2).
The patient developed complete atrioventricular block and repeated sinus arrest on day 60, and an external pacemaker was inserted. Myocardial conduction tract defect due to SSc was diagnosed, and additional steroid pulse therapy was administered for 3 days starting on day 112. Regarding renal function, the patient’s creatinine levels gradually decreased, and the patient was weaned off dialysis on day 151. Steroid treatment for SSc was continued, and the patient was discharged on day 279.
Discussion
Here, we present a case of SSc concomitant with secondary TMA. At presentation, the clinical scenario suggested TMAs, such as severe thrombocytopenia, microangiopathic hemolytic anemia, and renal dysfunction. Through continuous exploration for the underlying disease, we finally diagnosed the patient with SSc. Although the soluble C5b-9 levels were markedly elevated, the patient did not respond to the terminal complement inhibitor eculizumab. The patient underwent repeated plasma exchange therapy.
This case was a TMA secondary to SSc, which lacked the clinical symptoms of SSc and had not been previously diagnosed as SSc. Since there was no history of steroid administration, which is a risk factor for SSc-TMA, and the anti-Scl-70 antibody test was negative at the initial screening, diagnosing SSc as a cause of TMA was challenging. Finally, the patient was diagnosed with SSc based on the positive results for anti-fibrillarin (anti-U3-RNP) and anti-NOR-90 (anti-hUBF) antibodies. Anti-fibrillarin antibodies are detected in 4% to 10% of patients with SSc and are associated with pulmonary hypertension and fibrosis [13,14]. Anti-NOR-90 antibodies are observed in patients with relatively mild SSc and have been associated with other autoimmune disorders [15]. However, these antibodies have not been reported as risk factors for renal damage. As in this case, the diagnosis of SSC as the causative disease of TMA is challenging in patients with severe renal dysfunction and negative results for the anti-Scl-70 antibody. Anti-fibrillarin and anti-NOR-90 antibodies are key to the diagnosis.
In SSc, different pathologies are known to cause renal dysfunction, such as SRC, TMA (SSC-TMA), and anti-neutrophil cytoplasmic antibody-associated vasculitis [16]; they also overlap with other collagen diseases (systemic lupus erythematosus and Sjogren syndrome) [17]. In particular, SRC is difficult to differentiate from TMA because of their similar clinical findings, such as low platelet count and renal dysfunction, and they can occur concomitantly. In the present case, normal plasma renin activity and the absence of severe hypertension suggested that the primary pathogenesis was SSc-TMA.
In general, TMA is diagnosed based on microangiopathic hemolytic anemia, thrombocytopenia, and organ damage due to platelet thrombi. Guidelines recommend plasma exchange as soon as possible after the diagnosis of TMA. Atypical HUS tends to involve renal function more commonly than TTP and should be treated with eculizumab as early as possible [18]. At the initial screening for the causative diseases of TMAs, we could not detect causative diseases, such as systemic lupus erythematosus, anti-phospholipid antibody syndrome, and SSc. Thus, we strongly suspected aHUS and administered eculizumab accordingly because of the presence of severe renal impairment and abnormal complement activation. Martis et al reported that aHUS is often associated with no previous dialysis history and higher creatinine and lactate dehydrogenase levels than those found in autoimmune disease-related TMAs [17]. Therefore, we concluded that the early administration of eculizumab was appropriate in this case of high aHUS suspicion. We discontinued eculizumab administration after 2 doses of ineffective therapy; there was no improvement in the platelet count or renal function, and we did not want to subject the patient to unwarranted adverse effects. For patients showing TMA findings, especially for those with severe renal dysfunction, eculizumab should be administered as soon as possible for the clinical likelihood of aHUS, and should be discontinued when further examinations indicate a diagnosis other than aHUS.
Interestingly, eculizumab has been reported to be effective in patients with secondary TMA who are not responsive to conventional treatment [19]. As in aHUS, the complement pathway is also activated in secondary TMA, and blocking C5 is reasonable [20]. There are a few case reports of SSc-TMA that responded to eculizumab [21,22]. Immunofluorescence studies in patients with SRC have shown marked deposition of C1q, C3b, C4d, and C5b-9 in the endothelium of renal arteries and glomeruli, pointing to the role of complement activation, mainly via the classical pathway [21]. In the present case, eculizumab was ineffective, while soluble C5b-9 was markedly elevated, suggesting abnormal activation of the complement terminal pathway. This paradox may indicate that the pathogenesis of SSc-TMA predominantly results from the antigen-antibody reaction, which leads to classical complement pathway activation followed by terminal pathway activation; thus, eculizumab may not be effective in SSc-TMA. It is necessary to accumulate more knowledge and study more cases to determine exactly which patients would benefit from eculizumab.
In general, plasma exchange is expected to remove harmful inflammatory substances and replace necessary protein components. The mechanism of the effect of plasma exchange on SRC is not fully understood, but it is thought to remove vasoconstrictors, autoantibodies, inflammatory cytokines, and pro-fibrotic cytokines. Plasma exchange for SSc-TMA has a limited effect on short-term hematologic normalization [17] but is expected to improve long-term prognosis [9]. In the absence of SSc diagnosis, early plasma exchange should be performed according to the TMA practice algorithm when the patient presents with TMA findings. Additionally, complement activation should be assessed, and eculizumab should be administered. Repeated plasma exchange might save patients’ lives in cases of progressive SSc.
Conclusions
We present a case of SSc-TMA that was treated with eculizumab. In this case, eculizumab was ineffective, despite abnormal activation of the complement system. However, in cases in which the renal dysfunction is severe and the causative disease of TMA is not apparent at initial screening, introducing eculizumab would be acceptable because of the possibility of aHUS. Continuous monitoring and investigation are required, and discontinuation of eculizumab should be determined according to the patient’s response and final diagnosis.
Figures
References:
1.. George JN, Nester CM, Syndromes of thrombotic microangiopathy: N Engl J Med, 2014; 371; 654-66
2.. George JN, The Oklahoma Thrombotic Thrombocytopenic Purpura-Hemolytic Uremic Syndrome Registry: A program for patient care, education and research: Transfusion, 2004; 44; 1384-92
3.. Kundra A, Wang JC, Interferon induced thrombotic microangiopathy (TMA): Analysis and concise review: Crit Rev Oncol Hematol, 2017; 112; 103-12
4.. Gupta M, Feinberg BB, Burwick RM, Thrombotic microangiopathies of pregnancy: Differential diagnosis: Pregnancy Hypertens, 2018; 12; 29-34
5.. Veesenmeyer AF, Edmonson MB: Pediatr Infect Dis J, 2013; 32; 731-35
6.. Palma LMP, Sridharan M, Sethi S, Complement in secondary thrombotic microangiopathy: Kidney Int Rep, 2021; 6; 11-23
7.. Gouin A, Ribes D, Colombat M, Role of C5 inhibition in idiopathic inflammatory myopathies and scleroderma renal crisis-induced thrombotic microangiopathies: Kidney Int Rep, 2021; 6; 1015-21
8.. Guillevin L, Bérezné A, Seror R, Scleroderma renal crisis: A retrospective multicentre study on 91 patients and 427 controls: Rheumatology (Oxford), 2012; 51; 460-67
9.. Cozzi F, Marson P, Cardarelli S, Prognosis of scleroderma renal crisis: A long-term observational study: Nephrol Dial Transplant, 2012; 27; 4398-403
10.. Bussone G, Bérezné A, Pestre V, The scleroderma kidney: Progress in risk factors, therapy, and prevention: Curr Rheumatol Rep, 2011; 13; 37-43
11.. Bussone G, Bérezné A, Pestre V, The scleroderma kidney: Progress in risk factors, therapy, and prevention: Curr Rheumatol Rep, 2011; 13; 37-43
12.. Bose N, Chiesa-Vottero A, Chatterjee S, Scleroderma renal crisis: Semin Arthritis Rheum, 2015; 44; 687-94
13.. Tall F, Dechomet M, Riviere S, The clinical relevance of antifibrillarin (anti-U3-RNP) autoantibodies in systemic sclerosis: Scand J Immunol, 2017; 85; 73-79
14.. Aggarwal R, Lucas M, Fertig N, Anti-U3 RNP autoantibodies in systemic sclerosis: Arthritis Rheum, 2009; 60; 1112-18
15.. Dagher JH, Scheer U, Voit R, Autoantibodies to NOR 90/hUBF: Longterm clinical and serological followup in a patient with limited systemic sclerosis suggests an antigen driven immune response: J Rheumatol, 2002; 29; 1543-47
16.. Chrabaszcz M, Małyszko J, Sikora M, Renal involvement in systemic sclerosis: An update: Kidney Blood Press Res, 2020; 45; 532-48
17.. Martis N, Jamme M, Bagnis-Isnard C, Systemic autoimmune disease-associated TMA: Eur J Intern Med., 2021; 93; 78-86
18.. Campistol JM, Arias M, Ariceta G, An update for atypical haemolytic uraemic syndrome: Diagnosis and treatment: A consensus document. Nefrologia, 2015; 35; 421-47
19.. Román E, Mendizábal S, Jarque I, Secondary thrombotic microangiopathy and eculizumab: A reasonable therapeutic option: Nefrologia, 2017; 37; 478-91
20.. Palma LMP, Sridharan M, Sethi S, Complement in secondary thrombotic microangiopathy: Kidney Int Rep, 2021; 6; 11-23
21.. Devresse A, Aydin S, Le Quintrec M, Complement activation and effect of eculizumab in scleroderma renal crisis: Medicine (Baltimore), 2016; 95; e4459
22.. Thomas CP, Nester CM, Phan AC, Eculizumab for rescue of thrombotic microangiopathy in PM-Scl antibody-positive autoimmune overlap syndrome: Clin Kidney J, 2015; 8; 698-701
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133