06 June 2021: Articles 
Ileal Neuroendocrine Tumor in a Patient with Sclerosing Mesenteritis: Which Came First?
Unusual clinical course, Challenging differential diagnosis, Patient complains / malpractice, Rare disease
Cristine Pathirannehalage Don1ABCDEFG*, Daniele Sforza2ACDEG, Leandro Siragusa1ABCDEFG, Bruno Sensi1ABCDEFG, Matteo Ciancio Manuelli2DG, Rossana Telesca3BDG, Luca Savino3BDG, Valentina FerrazzoliDOI: 10.12659/AJCR.931372
Am J Case Rep 2021; 22:e931372
Abstract
BACKGROUND: Jejunoileal neuroendocrine tumors (JI-NETs) are rare tumors that can be associated with mesenteric fibrosis. This case report is of an incidental finding of a JI-NET in a patient who was previously misdiagnosed with sclerosing mesenteritis.
CASE REPORT: A 42-year-old man was admitted to our institution with diffuse abdominal pain and clinical and radiographic signs of bowel obstruction. He had a previous diagnosis of sclerosing mesenteritis, which had been histologically diagnosed after an exploratory laparoscopy performed in 2009 for recurrent acute abdominal pain. He was also annually monitored through computed tomography scans for an incidentally discovered, gradually enlarging mesenteric mass for which a “wait and watch” management approach was adopted. After a period of fasting and observation, the patient underwent an urgent exploratory laparotomy because of his worsening condition. Intraoperatively, an ileocecal resection was performed, along with excision of the known mesenteric mass. The pathology report revealed an ileal NET with nodal metastases within the mesentery and mesenteric tumor deposits (pT3N1).
CONCLUSIONS: JI-NETs are rare entities, which are usually encountered as incidental findings or in patients with unspecific abdominal pain. Our case represents a probable delayed diagnosis of JI-NET in the context of sclerosing mesenteritis; therefore, a possible association between these 2 conditions should be investigated.
Keywords: Fibrosis, Gastrointestinal Neoplasms, neuroendocrine tumors, Panniculitis, Peritoneal, Intestinal Neoplasms, Mesentery, Pancreatic Neoplasms
Background
A neuroendocrine tumor (NET) is a rare entity that occurs mostly in the gastrointestinal tract, especially in the small bowel. Jejunoileal neuroendocrine tumors (JI-NETs) comprise the second largest subgroup of NETs of the gastrointestinal system [1]. JI-NETs have an incidence of 0.67 to 0.81 per 100 000 persons per year and are usually diagnosed in patients between the ages of 60 and 65 years, with no difference in occurrence between men and women [2]. Diagnosis is often challenging because JI-NETs are typically found as an incidental finding in asymptomatic patients or in the clinical setting of unspecific abdominal symptoms. Advanced cases can present as large tumors that cause intestinal obstruction or as carcinoid syndrome in the case of metastatic disease.
Here, we report an incidental ly discovered JI-NET with nodal metastasis in a patient with a history of sclerosing mesenteritis.
Case Report
A 42-year-old man was referred to our Emergency Department in July 2020 with diffuse abdominal pain, emesis, and 3 days since last passing feces or flatus.
The patient had a medical history of hypertension, untreated type 2 diabetes, and chronic
The latter was performed for acute abdominal pain when a mass was found at the root of the mesentery and biopsied. The mass was classified as a sclerotic and fibromatous tissue, with chronic inflammation consisting of giant cells, macrophages, and necrosis, consistent with a diagnosis of sclerosing mesenteritis. Oncological markers CA19.9, CEA, and AFP were negative and thus a radiological follow-up with annual computed tomography (CT) was indicated as well as therapy with prednisone and tamoxifen.
A persistent finding was the mesenteric mass in the mesogastrium, measuring 5×7 cm and consisting of parenchymatous-like tissue, without remarkable contrast enhancement (last CT was on April 8, 2020). The patient was also routinely evaluated for nutritional difficulties and persistence of nausea and vomiting. He had a positron emission tomography (PET) scan on January 1, 2020, which showed hyperfixation of the mesogastric lesion and of a previously unrecognized lesion of the left colon. Because of these findings, colonoscopy was planned but not completed due to a lack of adequate intestinal preparation.
Between February and June 2020, the patient reported weight loss of 20 to 25 kg and recurrent episodes of acute abdominal pain, which he managed with antiemetics and pain medication.
On July 8, 2020, he underwent an urgent abdominal CT scan. A solid mass measuring 5×7 cm and strictly attached to the ileal loop was confirmed at the root of the mesentery, causing its compression and upstream distension (Figure 1A, 1B). Fasting and close observation were initially chosen as the therapeutic approach. The next day, an urgent exploratory laparotomy was indicated because of the patient’s worsening condition.
Intraoperative findings included a largely distended small bowel, which was adhered to the mesenteric root mass. The surgeon performed a thorough evaluation of the small intestine from the ligament of Treitz to the ileocecal valve, without identifying other pathological findings. A complete resection of the mesenteric mass was performed, along with resection of the cecum, appendix, and the last ileal loop, as these structures were firmly adhered to the mass. No other findings were reported, and an intraoperative colonoscopy excluded endoluminal masses and any signs of macroscopic lesions. A laterolateral mechanical ileocolonic anastomosis was fashioned without fecal diversion.
The histological examination highlighted a nodular retracting mesenteric mass measuring 8.5×6.5×7 cm that twisted the bowel loops because of fibrotic adhesion. The mass was irregularly shaped and light colored, had a hard consistency, and was composed of a mixture of vascular structures, myxoid areas, and calcified spots.
Another irregularly shaped, yellowish, hard area measuring 1.6 cm was described in the intestinal loops in connection with the sclerosing mesentery. Pathological examination revealed an NET of the ileum (NET-G1) with Ki67 <3% invading throughout the intestinal wall. The nearby mesentery was intensely sclerotic, with a microscopic examination confirming a strong chronic fibrotic and inflammatory reaction with few plasma cells and lymphocytes and occasionally IgG4+ plasma cells. NET deposits were found in the sclerosing mesentery (Figure 2).
Amid the fibrotic reaction, 12 lymph nodes were encountered, 2 of which had a positive result for tumoral cells. This NET was thus classified as pT3N1, stage III, according to the American Joint Committee on Cancer (AJCC) staging system (Figure 3).
The postoperative course was characterized by the absence of surgical complications, yet it was complicated by neurological distress, which was diagnosed as Wernicke-Korsakoff syndrome. The patient was treated with intravenous vitamin supplements and, on postoperative day 25, he was transferred to a neurological clinic for rehabilitation for about 30 days.
After a multidisciplinary discussion of the case, no adjuvant therapy was indicated, and, at the time of this report, the patient was in good condition. He continues to recover from the neurological dysfunction and is undergoing oncological follow-up.
Discussion
There is diagnostic difficulty in clearly distinguishing primary cases of sclerosing mesenteritis from secondary cases that are associated with an underlying malignancy. Some authors affirm that the fibrosis can be an actual sclerosing mesenteritis underneath a concomitant neoplasm and can therefore be a pure coincidence [3]; other authors suggest that the mesenteric fibrosis is a response of the microenvironment surrounding the NET to fibrotic proliferation [4].
Sclerosing mesenteritis is a rare condition that is characterized by chronic fat necrosis, associated with inflammation and/or fibrosis of the mesentery [5]. Its range of incidence in the population is 0.16% to 3.4%, peaking between the fifth and seventh decade of life [3,6].
Sclerosing mesenteritis was first described in 1924 by Jura et al with the name of “retractile mesenteritis”. Over time, this condition was further studied and defined under the single name of “sclerosing mesenteritis”; however, it comprises 3 different conditions that differ only in the histopathological aspects: mesenteric panniculitis, retractile mesenteritis, and mesenteric lipodystrophy [7].
There are 4 hypotheses for the etiopathogenesis of sclerosing mesenteritis: (1) iatrogenic etiology provoked by abdominal surgery or trauma; (2) autoimmune disease (multiple studies have reported an association with autoimmune diseases, such as Riedel thyroiditis and primary sclerosing cholangitis); (3) paraneoplastic syndrome; and (4) infections such as tuberculosis, histoplasmosis, and Whipple’s disease [3,5].
The clinical presentation of sclerosing mesenteritis can be challenging, as patients can be either asymptomatic or present with unspecific symptoms such as abdominal pain (78.1%), fever (26%), weight loss (22.9%), diarrhea (19.3%), vomiting (18.2%), and occasionally an abdominal mass [3,5,8]. Therefore, a final diagnosis is complex, also because there are no specific laboratory findings for sclerosing mesenteritis.
Imaging tests are helpful in diagnosing sclerosing mesenteritis because the condition has several specific radiological signs.
In 2011, Coulier et al defined 5 signs on CT that are specific for this disease: (1) mesenteric mass causing mass effect on nearby structures without any sign of invasion; (2) high attenuation; (3) mesenteric fat containing small nodes; (4) “fat halo sign” or “fat ring sign” as a hypoattenuating sign that surrounds the lymph nodes or the mesenteric vessels without their encasement; and (5) a hyperattenuating sign of a pseudo-capsule that encircles the mesenteric mass [4,6]. However, once a diagnosis is made, choosing the proper treatment course is controversial, with several case reports and small series having established medical treatment with corticosteroids, tamoxifen, thalidomide, and azathioprine [8]. Nonetheless, there are cases of involvement of the mesenteric vasculature and intestinal loops by the mass which indicate surgery, especially if there is bowel ischemia or obstruction, as in our present case [5].
NETs consist of a heterogeneous group of tumors with different morphologies and functions. They represent 0.5% of all malignant conditions and 2% of all gastrointestinal malignant tumors [1]. NETs originate from neuroendocrine cells, which are ubiquitous throughout the whole human body. Most of these tumors occur in the gastrointestinal tract (55%) and in the bronchopulmonary system (25%); gastrointestinal NETs are often detected in the small bowel (45%) but can also be detected in the rectum (20%), appendix (16%), colon (11%), and stomach (7%).
JI-NETs are the most common type of small bowel NETs and occur at a mean patient age of 60 to 70 years, without sex predilection [1]. Most JI-NETs are nonfunctioning, and therefore their clinical presentation can be unspecific. JI-NETs are usually detected incidentally in asymptomatic patients or in patients with generic abdominal pain, weight loss, and fatigue [1,2,9]. A rare presentation is with obstructive symptoms (nausea and vomiting), bleeding, or perforation [10]. Rare cases of specific clinical presentation usually occur with metastatic disease or functioning JI-NETs, where there is an excess of hormonal secretion by neuroendocrine tumoral cells [2,11].
JI-NETs are usually small and slow-growing tumors and are therefore classified as indolent [12]. However, at the time of diagnosis, 70% of JI-NETs have invaded the muscularis propria and include nodal metastasis, and another 50% can have hepatic metastasis regardless of tumor dimension [13].
Laboratory markers, such as serum chromogranin A (CgA), serum neuron-specific enolase (NSE), and urinary 5-hydroxy indole acetic acid (5-HIAA), are used to help in the diagnosis of JI-NETs. CgA and NSE are specific for neuroendocrine cells, while 5-HIAA is specific for serotonin metabolism; therefore, its use is limited to carcinoid syndrome or metastatic disease [2,12]. CgA is produced by all types of NETs, including those that are nonfunctioning. CgA is a specific and sensitive marker of NET because its production is correlated with tumor dimension and prognosis. It has been reported that higher CgA levels indicate a worse prognosis, perhaps because it is correlated with a higher tumor volume [1,2,13].
Imaging techniques are useful to assess the location of the tumor and to allow for its staging. CT and MRI are useful tools even if there is an unknown primary tumor with evidence of nodal involvement and/or distant metastasis [12]. Other imaging techniques include the functional studies such as somatostatin receptor imaging, namely gallium-68-PET and indium-111-SPECT. It is reported that the combination of gallium-68-PET with CT scanning improves sensibility in an additional 20% to 30% of cases [2].
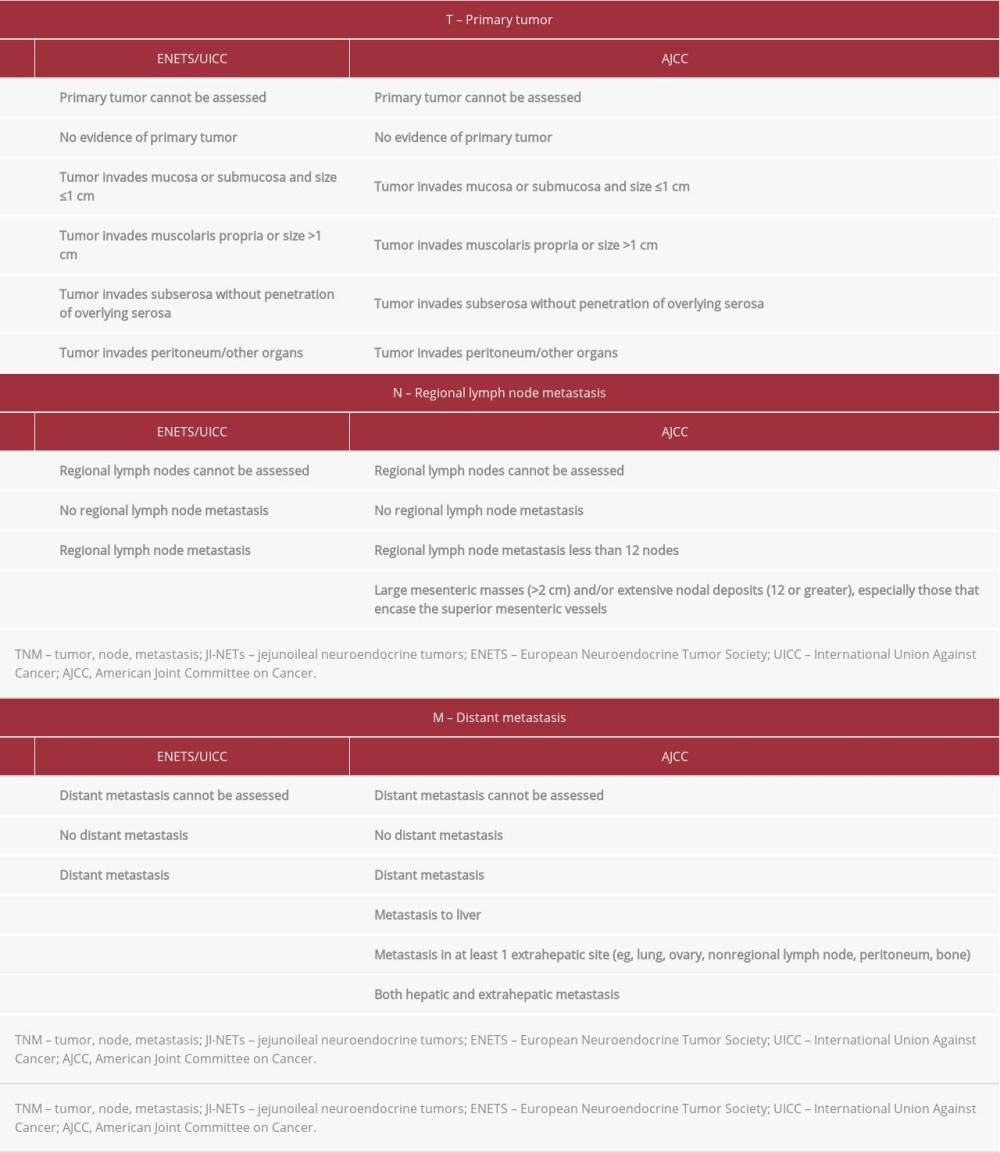
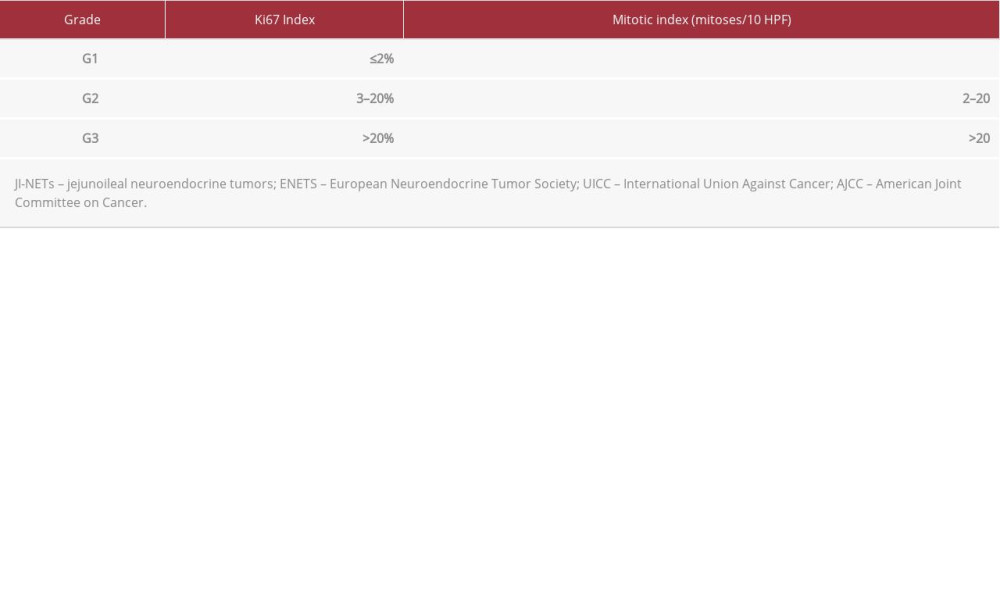
Definitive diagnosis of JI-NET is histological. The mitotic index and calculation of the Ki67 index are prognostically important in JI-NETs, since they are classified according to the European Neuroendocrine Tumor Society (ENETS), International Union Against Cancer (UICC), and AJCC systems through tumor, node, metastasis (TNM) staging and Ki67 grading [2] (Tables 1, 2).
JI-NETs are inclined to produce a desmoplastic reaction that leads to strong fibrosis in the mesentery; simultaneously, a mesenteric mass that is also in enlarged regional lymph nodes can be detected [1,14].
The desmoplastic reaction can cause mesenteric fibrosis, as was shown for the first time in 1961 by Moertel et al, who also determined its association with increased morbidity and mortality [15]. This process can expand to the retroperitoneal space, causing retroperitoneal fibrosis, obstructive uropathy, and hydronephrosis [12]. Mesenteric fibrosis can also cause mesenteric retraction, resulting in the kinking of the intestinal loops, followed by intestinal obstruction. The fibrotic process can also entail the mesenteric blood vessels, causing intestinal ischemia in 10% of cases [16,17]. Mesenteric fibrosis associated with JI-NETs is regarded as an independent negative prognostic factor, as it is associated with distant metastasis [1].
Standard treatment of JI-NETs is oncologic resection of the tumor with locoregional lymphadenectomy proximal to the branches departing from the superior mesenteric vessel and resection of the eventual mesenteric fibrosis [16]. It is important to fully explore the abdominal cavity to check for peritoneal carcinomatosis, which is present in 20% cases with no symptoms, and to perform a complete manual palpation of the small bowel from the ligament of Treitz to the ileocecal valve [16]. The criterion standard technique is a diagnostic laparotomy. Laparoscopy can be considered as an alternative, even though the guidelines from Europe and North America do not recommend it, considering the small size of NETs and the possibility of a multifocal nature [18,19].
More than 80% of cases have regional nodal metastasis; therefore, regional lymphadenectomy is advisable in all patients. ENETs guidelines emphasize the importance of curative re-section of the JI-NETs, together with dissection of locoregional nodes along the superior mesenteric pedicle and within the mesentery, as this improves the 5-year and 10-year survival rates to 100%, 95%, and 80% for stages I, II, and III, respectively. R0 resection is an important prognostic factor in locoregional cancer (stages I-III), whereas other important independent prognostic factors in survival are patient age and disease stage [2,19,20].
In addition to being associated with standard nodal metastasis, up to 60% of JI-NETs are associated with mesenteric tumor deposits (MTDs), which are defined as irregular mesenteric tumoral nodules that are discontinuous from the primary NET [4,21]. MTDs can also be associated with an intense mesenteric reaction, which can cause obstruction or ischemia. MTDs are also considered as an adverse prognostic factor, since they are associated with liver metastasis and a poor general prognosis [22]. Follow-up typically consists of blood tests and clinical and radiological examination every 6 months for the first year, then annually for a decade.
In our present case, the patient was previously diagnosed with sclerosing mesenteritis elsewhere and was therefore treated medically. Symptoms of nausea and fatigue had been vague and episodic over the years, until the intestinal obstruction occurred. The abdominal CT scan was not sufficient to allow for a correct diagnosis, since it only confirmed the presence of the mesenteric mass in addition to the radiological signs of obstruction. Given that the patient came to our Emergency Department because of the abdominal clinical presentation, the priority was to treat the intestinal obstruction, and, because the first conservative treatment was ineffective, the surgical approach was the only remaining choice. During the procedure, the entire small bowel was evaluated to find the cause of the obstruction. Mesenteric fibrosis was encountered, and the mesenteric mass was found to be responsible; however, at that time, there was no suspicion of a malignancy since the intraoperative colonoscopy did not reveal any macroscopic lesions. In this patient, only the histological examination enabled us to make the diagnosis of the JI-NET with nodal metastasis and MTDs. The real challenge with this patient was understanding whether the preexisting mesenteric fibrosis was independent or if it was derived from the adjacent NET. We found afterward that the strong fibrotic reaction that is associated with NETs can mislead a correct diagnosis, since MTDs can radiologically mimic sclerosing mesenteritis, as stated above. Both MTDs and sclerosing mesenteritis can appear as a mesenteric mass with radiating fibrotic bands in a stellate or wheel pattern; the main difference is that MTDs tend to encase and infiltrate mesenteric vessels, while sclerosing mesenteritis creates the “fat ring sign” as described above because it surrounds vessels without invading them [4,23]. In our present case, the abdominal CT scan that was performed in an urgent setting revealed that the mesenteric mass was well-defined, spiculated, and hyperattenuating, compared with the adjacent mesenteric fat, and slightly inhomogeneous with some calcifications. It had caused compression on the nearby intestinal loops and mesenteric vessels, without infiltrating them. Of the 5 CT signs described by Coulier et al, the mass of this patient had 2 of them, hence the diagnostic difficulty in discriminating sclerosing mesenteritis from the fibrotic mesenteritis associated with JI-NETs.
Conclusions
JI-NETs are rare entities that are usually encountered as an incidental finding or in patients with unspecific abdominal pain. Here, we report a case of delayed diagnosis of JI-NET in a context of sclerosing mesenteritis. Since sclerosing mesenteritis is usually a diagnosis of exclusion, we want to focus on the importance of considering small bowel NETs in all cases of fibrotic mesenteritis. Furthermore, it is widely reported in the literature that mesenteritis is usually a sequela of the NET environment. Moreover, we think that the pathophysiologic correlation between mesenteritis and NETs needs to be better defined to support this complex diagnosis.
Figures
References:
1.. Ahmed M, Gastrointestinal neuroendocrine tumors in 2020: World J Gastrointest Oncol, 2020; 12(8); 791-807
2.. Niederle B, Pape UF, Costa F, ENETS consensus guidelines update for neuroendocrine neoplasms of the jejunum and ileum: Neuroendocrinology, 2016; 103(2); 125-38
3.. Danford CJ, Lin SC, Wolf JL, Sclerosing mesenteritis: Am J Gastroenterol, 2019; 114(6); 867-73
4.. Roberts J, Gonzalez RS, Revetta F, Shi C, Mesenteric tumor deposits arising from small-intestine neuroendocrine tumors are frequently associated with fibrosis and IgG4-expressing plasma cells: Histopathology, 2018; 73; 795-800
5.. Green MS, Chhabra R, Goyal H, Sclerosing mesenteritis: A comprehensive clinical review: Ann Transl Med, 2018; 6(17); 336
6.. Coulier B, Mesenteric panniculitis: Part 2: Prevalence and natural course: MDCT prospective study: JBR-BTR, 2011; 94(5); 241-46
7.. Kipfer RE, Moertel CG, Dahlin DC, Mesenteric lipodystrophy: Ann Intern Med, 1974; 80(5); 582-88
8.. Sharma P, Yadav S, Needham CM, Feuerstadt P, Sclerosing mesenteritis: A systematic review of 192 cases: Clin J Gastroenterol, 2017; 10(2); 103-11
9.. Niederle MB, Niederle B, Diagnosis and treatment of gastroenteropancreatic neuroendocrine tumors: Current data on a prospectively collected, retrospectively analyzed clinical multicenter investigation: Oncologist, 2011; 16; 602-13
10.. Landerholm K, Falkmer S, Järhult J, Epidemiology of small bowel carcinoids in a defined population: World J Surg, 2010; 34; 1500-5
11.. Bergestuen DS, Aabakken L, Holm K, Small intestinal neuroendocrine tumors: Prognostic factors and survival: Scand J Gastroenterol, 2009; 44; 1084-91
12.. Scott AT, Howe JR, Management of small bowel neuroendocrine tumors: Surg Oncol Clin N Am, 2020; 29; 223-41
13.. Pasieka JL, Carcinoid tumors: Surg Clin North Am, 2009; 89; 1123-37
14.. Druce MR, Bharwani N, Akker SA, Intra-abdominal fibrosis in a recent cohort of patients with neuroendocrine (‘carcinoid’) tumors of the small bowel: QJM, 2010; 103; 177-85
15.. Moertel CG, Sauer WG, Dockerty MB, Baggenstoss AH, Life history of the carcinoid tumor of the small intestine: Cancer, 1961; 14; 901-12
16.. Howe JR, Cardona K, Fraker DL, The surgical management of small bowel neuroendocrine tumors: Consensus guidelines of the North American Neuroendocrine Tumor Society: Pancreas, 2017; 46; 715-31
17.. Daskalakis K, Karakatsanis A, Stålberg P, Clinical signs of fibrosis in small intestinal neuroendocrine tumors: Br J Surg, 2017; 104; 69-75
18.. Norlén O, Stålberg P, Öberg K, Long-term results of surgery for small intestinal neuroendocrine tumors at a tertiary referral center: World J Surg, 2012; 36; 1419-31
19.. Sica GS, Iaculli E, Biancone L, Comparative study of laparoscopic vs open gastrectomy in gastric cancer management: World J Gastroenterol, 2011; 17(41); 4602-6
20.. Arezzo A, Farina V, Foppa C, EuroSurg: A new European student-driven research network in surgery: Colorectal Dis, 2016(2); 214-15
21.. Gonzalez RS, Liu EH, Alvarez JR, Should mesenteric tumor deposits be included in staging of well-differentiated small intestine neuroendocrine tumors?: Mod Pathol, 2014; 27; 1288-95
22.. Fata CR, Gonzalez RS, Liu E, Mesenteric tumor deposits in midgut small intestinal neuroendocrine tumors are a stronger indicator than lymph node metastasis for liver metastasis and poor prognosis: Am J Surg Pathol, 2017; 41; 128-33
23.. Winant AJ, Vora A, Ginter PS, More than just metastases: A practical approach to solid mesenteric masses: Abdom Imaging, 2014; 39; 605-21
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133