10 June 2021: Articles 
Surgical and Radiological Management of Complicated Uterine Leiomyoma Aided by 3D Models in a Patient with Fibrodysplasia Ossificans Progressiva
Unusual setting of medical care, Rare disease
Michelle Ho12ABDEF*, Beau Y. Park3ABEF, Norman G. Rosenblum3DEF, Mona Al Mukaddam4DEF, Frederick S. Kaplan4ADEF, Victor Kucherov5EF, Scott G. Hubosky5EF, Gregory Kane6AD, Vishal Desai7DE, Michael R. Kramer7DE, Bon S. Ku28AD, Eric S. SchwenkDOI: 10.12659/AJCR.931614
Am J Case Rep 2021; 22:e931614
Abstract
BACKGROUND: Fibrodysplasia ossificans progressiva (FOP) is a rare autosomal dominant disorder of the connective tissue. Over time, patients with FOP experience decreased range of motion in the joints and the formation of a second skeleton, limiting mobility. Patients with FOP are advised to avoid any unwarranted surgery owing to the risk of a heterotopic ossification flare-up. For patients who do require a surgical procedure, a multidisciplinary team is recommended for comprehensive management of the patient’s needs.
CASE REPORT: A 27-year-old woman with FOP underwent a hysterectomy for removal of a suspected necrotic uterine fibroid. To aid in presurgical planning and management, patient-specific 3-dimensional (3D) models of the patient’s tracheobronchial tree, thorax, and lumbosacral spine were printed from the patient’s preoperative computed tomography (CT) imaging. The patient required awake nasal fiberoptic intubation for general anesthesia and transversus abdominus plane block for regional anesthesia. Other anesthesia modalities, including spinal epidural, were ruled out after visualizing the patient’s anatomy using the 3D model. Postoperatively, the patient was started on a multi-modal analgesic regimen and a course of steroids, and early ambulation was encouraged.
CONCLUSIONS: Patients with FOP are high-risk surgical patients requiring the care of multiple specialties. Advanced visualization methods, including 3D printing, can be used to better understand their anatomy and locations of heterotopic bone ossification that can affect patient positioning. Our patient successfully underwent supracervical hysterectomy and bilateral salpingectomy with no signs of fever or sepsis at follow-up.
Keywords: airway management, Hysterectomy, Imaging, Three-Dimensional, Myositis Ossificans, Intubation, Intratracheal, Leiomyoma, Ossification, Heterotopic, Radiography
Background
Fibrodysplasia ossificans progressiva (FOP; #MIM135100) is a very rare genetic disorder of progressive heterotopic bone formation caused by an activating mutation in activin receptor A, type I (ACVR1) [1]. Individuals with classic FOP have congenital malformations of the great toes, an invariant clinical feature of the disease [2]. Painful swellings or “flare-ups” develop in childhood and herald the formation of heterotopic bone in the skeletal muscles and connective tissue, which is most disabling in the shoulders and hips [3]. Eventually, individuals with FOP form a second skeleton of heterotopic bone, which leads to progressive and catastrophic disability. Trauma, including surgery, falls, or intramuscular injections, can trigger flare-ups.
Individuals with FOP are instructed to avoid surgery unless absolutely necessary owing to concern of exacerbating a flare-up. Intramuscular injections are contraindicated as they can cause flare-ups, while subcutaneous injections are considered safe [4]. Because surgery in patients with FOP is rare, there are few published case reports describing surgery for patients with FOP under general anesthesia. Previously described surgeries include dental, spinal, and thoracic procedures [5–9]. Flare-ups following procedures such as cesarean sections and heterotopic ossification removal have been reported [7,10,11].
The assembly of a multidisciplinary team is paramount to maximize the chance of a successful and safe outcome of surgery [4,12]. Airway management in patients with FOP is challenging because of the presence of cervical spine fusion, ankylosed jaw, thoracic insufficiency syndrome, and restrictive chest wall disease, which can pose life-threatening complications [13]. Moreover, for longer procedures requiring an indwelling uri-nary catheter, insertion of a catheter can be challenging if the patient has limited mobility of the lower extremities. We report on a severely disabled 27-year-old woman with FOP who successfully underwent supracervical hysterectomy for a necrotic uterine fibroid, highlighting the importance of a multi-disciplinary team and advanced technology.
Case Report
HISTORY AND EXAMINATION:
A 27-year-old woman with classic FOP and the canonical ACVR1R206H mutation presented with recurrent bacteremia due to a necrotic uterine fibroid. The patient’s past medical history included hearing loss, seizure disorder, anxiety/depression, gastroesophageal reflux disease, and an overactive bladder. The patient was diagnosed with classic FOP at the age of 4 years based on malformed great toes and progressive hetero-topic ossification in characteristic anatomic patterns [2]. Over time, she developed complete ankylosis of the neck, thoracolumbar spine, both shoulders, the left elbow, and both hips, as well as partial ankylosis of the right elbow and both knees. While the patient required a motorized wheelchair for transportation, she was able to ambulate by shuffling. The patient had limited movement of her wrists, hands, and ankles. The great toes were malformed and both hips were fused in an adducted position.
The patient was admitted with fever, chills, right lower-quadrant abdominal pain, and right hip pain and was diagnosed with Escherichia coli bacteremia of an unclear source. On admission, laboratory values were significant for a white blood cell (WBC) count within the reference range, aspartate aminotransferase (AST) of 112, alanine aminotransferase (ALT) of 143, total bilirubin of 1.6 mg/dL, and direct bilirubin of 1.0 mg/dL. Urine culture and magnetic resonance imaging (MRI) of the right hip were negative. A computed tomography (CT) scan of the chest was negative for pneumonia (Figure 1). A transthoracic echocardiogram was negative for cardiac vegetation, with an ejection fraction of 65%. A CT scan and ultra-sound of the abdomen demonstrated an enlarged endometrium. She was discharged after a 2-week course of intravenous (i.v.) antibiotics.
After 3 months, the patient was readmitted with fever, chills, severe abdominal pain and cramps, and vaginal bleeding. Admission laboratory tests were significant for a WBC count of 18 200/μl, and hepatic enzymes were within the reference range. Blood cultures were positive for
An MRI of the pelvis revealed a hypointense irregular solid mass measuring 6×4×6 cm with diffusion restriction within the endometrial cavity, scattered small cystic/necrotic portions within the mass, and adenomyosis along the posterior uterine wall (Figure 2). She responded to antibiotic treatment, and was scheduled for hysterectomy.
CONSULTATIONS – DESIGN MEDICINE:
To aid in general anesthesia surgical planning and patient education, the team designed and printed patient-specific 3-dimensional (3D) models of the thorax and the tracheobronchial tree (Figure 3). Advances in technology and affordability have expanded the use of 3D models for surgical planning, simulation training, and patient education. Previous studies have reported greater patient understanding of anatomy, disease, and surgical procedure and reduced operating room costs with the use of 3D models [14,16]. In a previous case, a 3D model of the thorax and tracheobronchial tree of a patient with FOP and recurrent left lower-lobe pneumonia demonstrated severe obliteration of the left bronchial tree secondary to severe kyphoscoliosis. This finding precluded bronchial stent insertion and selective lobectomy (personal communication, ZG).
To create the 3D models, the patient’s CT data were imported into processing software, where a 3D reconstruction was created (Mimics® Innovation Suite, Materialise NV, Leuven, Belgium). Segmentation of the normotopic bone, heterotopic bone, and tracheobronchial tree was performed and validated by a board-certified radiologist. The model was then exported as a Surface Tessellation Language file and uploaded to Ultimaker Cura® (Ultimaker, Cambridge, MA, USA), an open-source 3D printer slicing application, for preprinting processing. A spine model and tracheobronchial tree model were printed at 100% scale and a thorax model was printed at 50% scale. All models were printed with polylactic acid filament and polyvinyl acetate filament for support. Heterotopic bone on the thorax model was identified by sanding and coloring the model using an indelible marker after printing.
ANESTHESIA CONCERNS:
General and regional anesthesia were required for adequate perioperative sedation and pain management.
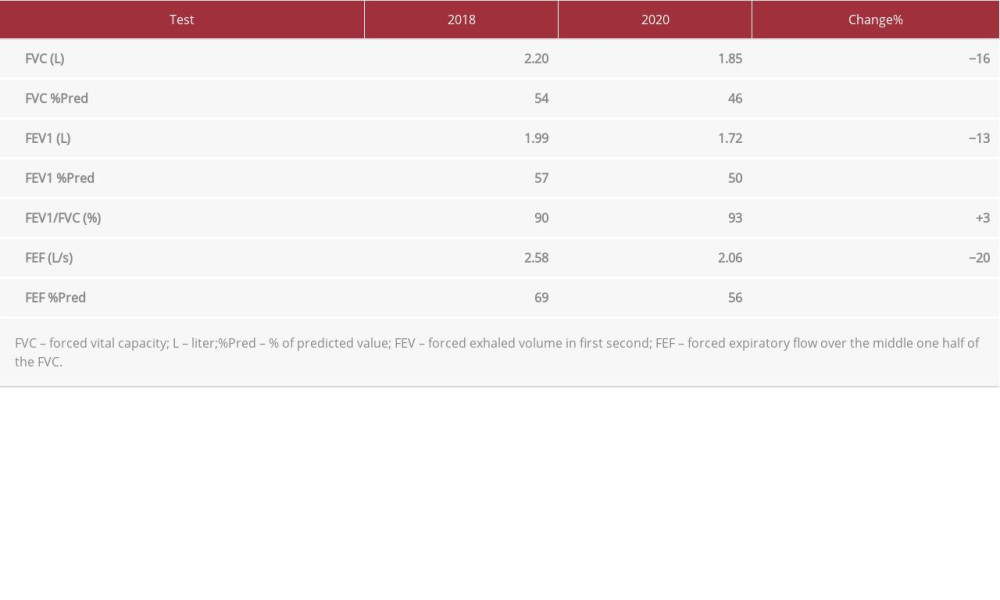
Cervical spine fusion, inability to open the mouth due to ankylosis of the temporomandibular joint, thoracic insufficiency syndrome, restrictive chest wall disease, and sensitivity to oral trauma complicate airway management and anesthesia and pose life-threatening risks for patients with FOP [13]. Thoracic insufficiency syndrome and restricted lung volume, secondary to ossification of the chest wall, can lead to cardiorespiratory failure [17]. Pulmonary function tests of the patient demonstrated a worsening restrictive pattern over the last 2 years (Table 1). However, the 3D models of the thorax and the tracheobronchial tree demonstrated that all branches of the bronchial tree were intact, with no signs of bronchomalacia. As the patient could ambulate and lead an active life using her motorized chair, she committed to an early postoperative ambulation schedule. We concluded that the ability of the patient to safely tolerate the surgical procedure and maintain adequate spontaneous ventilation after surgery were the major determinants for approving the surgical procedure, which was the only solution to prevent future life-threatening infections from the necrotic uterine content.
Awake nasal fiberoptic intubation is considered the first choice for airway management of patients with FOP [13]. To minimize the use of opioids and the risk of respiratory depression after surgery, regional anesthesia using epidural analgesia or transversus abdominus plane block (TAP) was considered. The TAP block was first described by Rafi in 2001 as an effective technique that utilized anatomical landmarks to deliver regional anesthesia to the anterior abdominal wall [18]. In a study of patients undergoing elective total abdominal hysterectomy, use of the TAP block was found to be associated with reduced postoperative visual analog scale pain scores, compared with a placebo block [19]. As was indicated by the 3D spine model, epidural placement with the patient’s anatomy was risky, if not impossible. Although a TAP block would be technically less challenging to perform, there was concern that minor soft-tissue trauma to the abdominal wall as well as possible direct injury to the skeletal muscle from the local anesthetic could lead to inflammation and heterotopic ossification. After discussing the risks and benefits with the patient, an ultrasound-guided TAP block was selected for postoperative analgesia.
UROLOGIC CONCERNS:
The standard position for preoperative Foley catheter insertion in a female patient for a supine surgery is the “frog-leg” position [20]. For our patient, such positioning was rendered impossible owing to her ankylosed hips that were in an adducted position. Alternatively, the team planned to carefully position the patient in right lateral decubitus, a position that did not require mobility at any lower-extremity joint. In the event that a transurethral Foley catheter could not be placed, the patient had also provided consent for a suprapubic catheter placement.
GYNECOLOGIC CONCERNS:
The physical examination for mobility and awareness of patient comfort are paramount in determining the surgical approach. Our patient’s lower extremities were ankylosed in a neutral position, excluding vaginal surgery and hysteroscopy. Limitations for laparoscopic surgery included the inability to place a uterine manipulator through the vagina or trocars on the left abdomen owing to the ankylosed position of the patient’s left arm. Pneumoinsufflation with the Trendelenburg position posed concerns for interference with ventilation. Operative exposure via a low abdominal vertical incision was selected as safe and feasible.
OPERATIVE CONCERNS:
Following the multidisciplinary consultation with the patient and family, the decision was made to perform a supracervical hysterectomy, bilateral salpingectomy, and appendectomy via a low midline supraumbilical incision.
PREOPERATIVE MEDICATIONS:
The patient received 1000 mg acetaminophen, 200 mg celecoxib, and 75 mg pregabalin prior to surgery for preemptive analgesia. Additionally, 80 mg i.v. methylprednisolone sodium succinate and 5000 units of subcutaneous heparin were administered for flare-up prophylaxis and deep vein thrombosis (DVT) prophylaxis, respectively.
PATIENT POSITIONING:
Positioning of the surgical bed and adequate padding were imperative to accommodate the patient’s fixed posture and avoid unintended pressure points which could cause micro-trauma and promote heterotopic ossification. The head of the bed was raised to match the patient’s flexion of the torso and eliminate pressure in her lower back. She was placed in the right lateral recumbent position for the Foley catheter placement, her preferred side for comfort. The patient’s left arm was well secured with foam padding, and the left hand was gently taped to the lateral abdomen to keep it away from the surgical incision (Figure 4). The operating room staff had been educated before the surgery to avoid any passive movement of limbs and joints at all times. Rolled 4-×4-cm surgical dressings were placed between any lines and the patient’s body to avoid microtrauma.
NASAL FIBEROPTIC INTUBATION:
Flexible fiberoptic nasopharyngolaryngoscopy by an otolaryngologist showed a widely patent upper airway with normal landmarks. The otolaryngologist remained available throughout the duration of the procedure to assist with intubation or emergency tracheostomy if needed.
Noninvasive monitoring included electrocardiography, pulse oximetry, blood pressure, and temperature. Supplemental oxygen was administered via a nasal cannula held at the mouth, with carbon dioxide end-tidal monitoring. Midazolam, ketamine, and remifentanil were administered i.v. and titrated for conscious sedation. Oxymetazoline (0.05%) nasal spray was applied for topical vasoconstriction. The nasal passages were progressively dilated with lubricated flexible nasal airways (26-French to 34-French). With the patient sedated, a nasal fiberoptic intubation was accomplished with a silicone-lubricated fiberoptic bronchoscope. Lidocaine 4% was applied as topical analgesia as the bronchoscope was advanced toward the epiglottis with a final position above the tracheal carina. The endotracheal tube positioning was confirmed visually, by auscultation, and by end-tidal carbon dioxide monitoring. Finally, i.v. propofol and rocuronium bromide were used for induction of general anesthesia and muscle relaxation.
TAP BLOCK:
The patient was positioned supine and her right anterolateral abdominal wall was prepped with chlorhexidine (ChloraPrep™, BD, Franklin Lakes, NJ, USA) for a TAP block. A 12-MHz linear ultrasound probe was placed in a transverse orientation on the lateral abdominal wall, across the midaxillary line, between the inferior costal margin and the anterior superior iliac spine. The TAP, located between the internal oblique muscle and transversus abdominis muscle, was visualized. Guided by continuous ultrasound, a 22-gauge, short-bevel needle was introduced and advanced into the TAP under continuous ultra-sound guidance. Following confirmation of position with 2 to 3 mL of saline, 15 mL of 0.2% ropivacaine was injected into the plane. The same procedure was repeated on the contralateral side. While the right TAP block was straightforward, the left TAP block was more challenging because of the patient’s fixed arm positions and a very small area of the abdomen that was able to be visualized with ultrasound (Figure 3). A successful bilateral loss of sensation was achieved. The 16-French Foley catheter was then inserted under sterile conditions with the patient in the right lateral decubitus position.
HYSTERECTOMY, PARTIAL OMENTECTOMY, AND APPENDECTOMY:
A midline incision was performed from above the umbilicus to the pubic bone. Access to the pelvis proved to be a challenge owing to the patient’s ankylosed hips, left arm position, and body habitus. To maximize exposure of the enlarged uterus, a Bookwalter retractor was used with double posts to secure the ring safely above the left arm. The supracervical hysterectomy with ablation of the endocervical canal and bilateral salpingectomy were completed without complications and with minimal blood loss. A portion of the greater omentum was found to have a transomental defect and was removed to prevent future small-bowel obstruction or hernia. A general surgeon performed an appendectomy using a transverse anastomosis stapler. The appendectomy stump was cauterized. The wound was closed using 3-0 Monocryl deep dermal sutures and 3-0 V-Loc running subcuticular suture, and sterile dressings were applied. A drain was placed superficially to the superficial fascia in the subcutaneous space because of the presence of a large amount of subcutaneous adipose tissue. The patient was awakened, extubated uneventfully, and transferred to the surgical intensive care unit (SICU).
POSTOPERATIVE COURSE:
The patient was admitted to the SICU for recovery and close monitoring of the airway and respiratory system. The head of the bed remained at 30° flexion to eliminate lower-back pressure, and she remained stable on room air. Because peripheral i.v. lines were placed in the feet bilaterally, no sequential compression devices were used, and subcutaneous heparin was given for DVT prophylaxis. A few hours after surgery, the patient was out of bed ambulating and using incentive spirometry. Antibiotic coverage was continued for 24 h after the procedure (2 doses each of 500 mg i.v. metronidazole and 2000 mg i.v. cefazolin). She remained afebrile without signs of infection.
The patient was started on a multi-modal postoperative analgesic regimen of 1000 mg oral acetaminophen, 15 mg i.v. ketorolac, and 75 mg oral pregabalin. On postoperative day (POD) 1, she was transitioned from hydromorphone patient-controlled analgesia to 5 mg oral oxycodone.
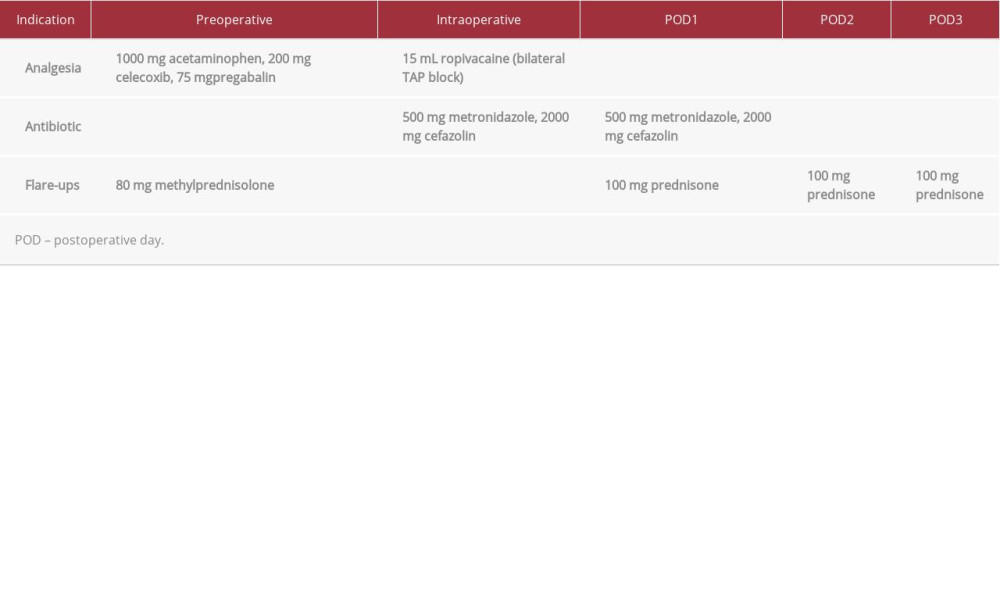
To reduce risk of flare-ups and heterotopic ossification, 100 mg oral prednisone was given daily for 3 days (Table 2) [4]. The Foley catheter was removed on POD 2 to ensure return of bladder function and avoid the need for recatheterization. The sub-cutaneous drain was removed on POD 3. The patient was discharged from the hospital on POD 3.
At her 6-week postoperative visit, the patient reported doing very well and had no concerns. She remained afebrile without signs of fevers or sepsis. On physical examination, the patient’s abdomen was nontender with a well-healed incision site and no clinical signs of flare-ups or heterotopic ossification.
The final pathology report confirmed a uterus of 400 g with extensive adenomyosis and adenomyoma and a grade 1 neuroendocrine tumor of the appendix with negative margins.
Discussion
FOP is a rare disease characterized by progressive heterotopic bone formation that occurs spontaneously or following minor trauma. For this reason, patients with FOP are advised to avoid any unnecessary surgery. Due to progressive ossification of soft tissue, patients with FOP lose flexibility and mobility. To the best of our knowledge, this is the first case of a hysterectomy in a patient with FOP.
Prior to the hysterectomy, our patient had 2 hospital admissions for sepsis of unknown origin. Following an extensive evaluation, including chest X-ray, CT scan of the chest and abdomen, transabdominal ultrasound, and pelvic MRI, it was suspected that her recurrent episodes of bacteremia were due to a necrotic fibroid. MRI of the pelvis demonstrated a 6-cm mass with scattered cystic and necrotic portions and adenomyosis along the posterior uterine wall (Figure 2). While infection of fibroids is rare and typically encountered during the peripartum period or with uterine instrumentation, the patient’s fevers coincided with the onset of her menstrual cycle for both admissions, suggesting the leiomyoma as the source of sepsis [21,22].
In preparation for surgery, a multidisciplinary team consisting of clinicians from the gynecology, anesthesiology, otolaryngology, pulmonology, urology, endocrinology, genetics, general surgery, critical care, pain management, and nursing departments, and clinicians with FOP expertise, was assembled for perioperative and surgical planning. Goals of this meeting included team education about FOP, discussion of surgical approaches, and review of the patient’s preoperative, intraoperative, and postoperative care. To aid in these discussions, 3D models of the patient’s thorax, tracheobronchial tree, and spine were designed and printed. With these models, clinicians were able to visualize and appreciate the patient’s heterotopic ossification.
Many precautions were taken to minimize any microtrauma to tissue. The surgical bed was positioned to match the patient’s ankylosed position, and pillows, blankets, and foam were used to ensure adequate padding. In locations where i.v. lines came into contact with the patient’s body, 4×4 cm sterile dressings were placed as a buffer.
Because FOP’s characteristic heterotopic ossification does not occur in smooth muscle, there is no direct effect on bladder or pelvic floor mechanics. The progressive immobility of FOP, however, can lead to urinary complications. For our patient, Foley catheter insertion was accomplished through alternative patient positioning and adequate exposure of the urethra. In the event that neither of these conditions could be achieved, the team was prepared to perform a suprapubic catheter placement.
While the patient’s hysterectomy was indicated to remove the source of infection, additional procedures were completed to minimize the number of potential future surgeries. The cervix was left in situ to minimize risk of vaginal cuff complications and introduction of vaginal flora into the pelvis. The vaginal cuff would have been inaccessible for a postoperative examination. Risk of cervical dysplasia in the remaining cervix was low because the patient had never been sexually active. The salpingectomy was planned to reduce the risk of high-grade serous carcinoma and the need for future procedures, as was the indication for an appendectomy. Partial omentectomy and appendectomy were performed to reduce the risk of small-bowel obstruction and infection, respectively.
Conclusions
The experience from this multidisciplinary approach to hysterectomy in a patient with FOP provides a broad perspective on the preoperative, intraoperative, and postoperative considerations for care. To aid in decision making and patient education, the team designed and printed patient-specific 3D models to better understand the extent of the patient’s condition. Given the high intraoperative risks that patients with FOP face during any surgery, the experience from this patient’s care can be used for planning and execution of future surgeries for patients with FOP.
Figures
References:
1.. Shore EM, Xu M, Feldman GJ, A recurrent mutation in the BMP type I receptor ACVR1 causes inherited and sporadic fibrodysplasia ossificans progressiva: Nat Genet, 2006; 38(5); 525-27
2.. Pignolo RJ, Shore EM, Kaplan FS, Fibrodysplasia ossificans progressiva: Diagnosis, management, and therapeutic horizons: Pediatr Endocrinol Rev, 2013; 10(2); 437-48
3.. Pignolo RJ, Bedford-Gay C, Lijesthrom M, A comprehensive global assessment: J Bone Miner Res, 2016; 31(3); 650-56
4.. Kaplan FS, Al Mukaddam M, Baujat , Current treatment considerations: Proc Intl Clin Council FOP, 2019; 1; 1-11
5.. Wadenya R, Fulcher M, Grunwald T, A description of two surgical and anesthetic management techniques used for a patient with fibrodysplasia ossificans progressiva: Spec Care Dent, 2010; 30(3); 106-9
6.. Liu JX, Hu R, Sun Y, Jiang H, General anesthesia in fibrodysplasia ossificans progressive: A case report and clinical review: Int J Clin Exp Med, 2014; 7(5); 1474-79
7.. Zaghloul KA, Heuer GG, Guttenberg MD, Lumbar puncture and surgical intervention in a child with undiagnosed fibrodysplasia ossificans progressiva: Case report: J Neurosurg Pediatr, 2008; 1(1); 91-94
8.. Gorji R, Li F, Nastasi R, Stuart S, Fibrodysplasia ossificans progressiva: Anesthetic management in complex orthopedic spine procedures: J Clin Anesth, 2011; 23(7); 558-61
9.. Seok Y, Cho S, Lee E, Surgical treatment combined with NSAIDs in fibrodysplasia ossificans progressiva: Ann Thorac Cardiovasc Surg, 2012; 18(1); 61-63
10.. Muglu JA, Garg A, Pandiarajan T, Pregnancy in fibrodysplasia ossifi-cans progressiva: Obstet Med, 2012; 5(1); 35-38
11.. Obamuyide H, Ogunlade S, A tumour for which surgery will do more harm than good: A case report of fibrodysplasia ossificans progressiva: Niger Postgrad Med J, 2015; 22(1); 83-88
12.. Botman E, Treurniet S, Lubbers WD, When limb surgery has become the only life-saving therapy in FOP: A case report and systematic review of the literature: Front Endocrinol (Lausanne), 2020; 11; 570
13.. Kilmartin E, Grunwald Z, Kaplan FS, Nussbaum BL, General anesthesia for dental procedures in patients with fibrodysplasia ossificans progressiva: A review of 42 cases in 30 patients: Anesth Analg, 2014; 118(2); 298-301
14.. Wake N, Rosenkrantz AB, Huang R, Patient-specific 3D printed and augmented reality kidney and prostate cancer models: Impact on patient education: 3D Print Med, 2019; 5(1); 3-4
15.. Kim PS, Choi CH, Han IH, Obtaining informed consent using patient specific 3D printing cerebral aneurysm model: J Korean Neurosurg Soc, 2019; 62(4); 398-404
16.. Ballard DH, Mills P, Duszak R, Medical 3D printing cost-savings in orthopedic and maxillofacial surgery: Cost analysis of operating room time saved with 3D printed anatomic models and surgical guides: Acad Radiol, 2020; 27(8); 1103-13
17.. Kaplan FS, Zasloff MA, Kitterman JA, Early mortality and cardiorespiratory failure in patients with fibrodysplasia ossificans progressiva: J Bone Jt Surg – Ser A, 2010; 92(3); 686-91
18.. Rafi AN, Abdominal field block: A new approach via the lumbar triangle: Anaesthesia, 2001; 56(10); 1024-26
19.. Carney J, McDonnell JG, Ochana A, The transversus abdominis plane block provides effective postoperative analgesia in patients undergoing total abdominal hysterectomy: Anesth Analg, 2008; 107(6); 2056-60
20.. Ortega R, Ng L, Sekhar P, Song M, Female urethral catheterization: N Engl J Med, 2008; 358(14); 3-6
21.. Obele CC, Dunham S, Bennett G, A Case of pyomyoma following uterine fibroid embolization and a review of the literature: Case Rep Obstet Gynecol, 2016; 2016; 9835412
22.. DeMaio A, Doyle M, Pyomyoma as a rare source of postpartum sepsis: Case Rep Obstet Gynecol, 2015; 2015; 263518
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133