26 July 2021: Articles 
A Rare Case of Invasive Mucormycosis in a Diabetic Patient Treated with a Short Course of Dexamethasone
Unusual clinical course, Rare disease
Gurchetan Randhawa1EF*, Sean Hagaman1EF, Mahsa Pourabdollah Tootkaboni1EF, Sanchit V. Kundal1EF, Sharad OliDOI: 10.12659/AJCR.932129
Am J Case Rep 2021; 22:e932129
Abstract
BACKGROUND: Invasive mucormycosis is a rare, life-threatening infection that requires urgent medical management. Here we describe a patient who developed invasive mucormycosis after receiving only a short course of dexamethasone. The purpose is to highlight this atypical presentation of a rare disease.
CASE REPORT: A 74-year-old woman with a medical history of diabetes mellitus (DM), hypertension, hyperlipidemia, and small cell lung cancer with metastasis to the brain presented to the Emergency Department with altered mental status and a hyperosmolar hyperglycemic state. Three weeks before, she had been diagnosed with DM (hemoglobin A1c [HbA1c] 6.5%) and was started on dexamethasone to treat cerebral edema. On admission, her HbA1c was 10.8%, although she had received only a short course of dexamethasone. Her physical exam was concerning for left eyelid swelling and ophthalmoplegia. Computed tomography of the head and neck revealed signs of left ocular proptosis and invasive rhinomaxillary fungal disease. The patient underwent urgent surgical debridement; subsequent magnetic resonance imaging revealed extensive fungal disease extending into her left inferior frontal lobe. A surgical pathology report was positive for Rhizopus oryzae and Stenotrophomonas maltophilia. Her blood cultures were positive for methicillin-susceptible Staphylococcus aureus. She was treated with antibiotics and amphotericin B. Her clinical course was complicated by hypokalemia. She eventually recovered and was discharged from the hospital.
CONCLUSIONS: This case highlights an atypical presentation of mucormycosis. Clinicians should remain vigilant for this rare complication of dexamethasone use even when the therapy is given for a short time.
Keywords: amphotericin B, Dexamethasone, Diabetes Mellitus, mucormycosis, Magnetic Resonance Imaging
Background
Mucormycosis is an infection caused by fungi of the order Mucorales. Fungi of the family
Case Report
A 74-year-old woman with newly diagnosed DM and a history of hypertension, hyperlipidemia, and small cell lung cancer (SCLC) metastatic to the brain presented to the Emergency Department (ED) with lethargy and weakness that had significantly worsened over the past 2 days. Her cancer had been diagnosed 3 weeks before admission and was treated with gamma knife radiation therapy 1 week after that. She was taking 4 mg of dexamethasone twice a day to treat cerebral edema. Three weeks before admission, she had been diagnosed with DM and her hemoglobin A1c (HbA1C) was 6.5%. When she was admitted, however, her initial blood glucose level was >799 mg/dL and her HbA1c was 10.8% – a significant change in a matter of weeks (Table 1). During a follow-up appointment with her oncologist several days before presenting to the ED, the patient’s blood glucose level was noted to be elevated. She had no symptoms at that time and was advised to follow up with her primary care provider for optimization of her DM regimen. Before she could do that, however, she started to feel ill and went to the ED instead. She was admitted with an initial diagnosis of a hyperosmolar hyperglycemic state.
The patient’s physical exam was significant for left eyelid swelling and erythema, which was concerning for preseptal cellulitis. She developed ophthalmoplegia and visual impairment in her left eye. Her mental status worsened and she had difficulty following commands. She received aggressive hydration with i.v. fluids and insulin to control her blood glucose levels. Then, she went into septic shock and was started on broad-spectrum antibiotics and vasopressors through a central venous catheter (Table 1).
The patient next was evaluated in the Medical Intensive Care Unit (ICU); however, because of her poor prognosis, she was not a candidate for ICU-level care. She was medically managed on the Inpatient Medicine Service for the duration of her admission.
A computed tomography scan of the patient’s head and neck revealed signs of left ocular proptosis and invasive rhinomaxillary fungal disease (Figures 1, 2). She was started on amphotericin B and underwent urgent surgical debridement to remove the necrotic tissue. Magnetic resonance imaging of the head and neck subsequently was performed (Table 1) and revealed invasive fungal disease extending into the left inferior frontal lobe (Figure 3). After a multidisciplinary meeting with the patient’s family, her healthcare agent declined further surgery, given the patient’s current illness. Orbital exenteration and skull base surgery were offered, but the healthcare agent preferred conservative medical management instead because of the patient’s poor long-term prognosis.
The surgical pathology report confirmed the presence of invasive mucormycosis (
Discussion
Invasive mucormycosis is a life-threatening condition that is associated with significant morbidity and mortality. Risk factors for acquiring it include uncontrolled DM (especially leading to diabetic ketoacidosis), use of corticosteroids, immunosuppressive therapy (such as for bone marrow and organ transplantation), neutropenia, cancer (especially hematological), and trauma and burns [2]. Mucormycosis is difficult to diagnose, but early diagnosis and treatment are critical to patient outcome [8]. One study demonstrated that delaying treatment for 6 days from symptom onset is associated with an increase in 30-day mortality from 35% to 66% [8].
The mortality rate with localized cutaneous mucormycosis is 10% to 30%, whereas disseminated mucormycosis carries a much higher rate (50% to 90%), depending upon organ involvement [9–11]. One study comparing treatment modalities indicated that the lowest mortality rate was associated with amphotericin B plus surgery (18.8% to 43.7%) [12]. This was in comparison to surgery alone (38.5% to 60.9%) and amphotericin B alone (50% to 61.3%) [12]. As a result, early, aggressive surgical excision combined with systemic antifungal therapy is the mainstay of treatment [9,11,13,14]. Ideally, surgery should be performed before fungus dissemination, although it is beneficial even after fungus spread [9,11,13,14]. Recently, endoscopic sinus surgery for radical resection has been found to result in better local control of the disease (with reduced operative morbidity) compared to the classical transantral approach [15,16].
Our patient received dexamethasone therapy for cerebral edema caused by metastatic SCLC, but it was given for only 3 weeks before her HbA1c level rapidly increased (6.5% to 10.8%). That presentation is rare, as most cases of invasive mucormycosis are in patients who have received steroids for a longer time [5,6]. Steroid use in conjunction with the hyperglycemic and acidic state found in uncontrolled DM causes phagocytic impairment – the primary defense mechanism against mucormycosis [2]. Mucormycosis causes angioinvasion, which leads to tissue necrosis, thrombosis, and a disseminated infection (Figures 6, 7) [2]. Thrombosis and tissue necrosis subsequently prevent leukocytes and other immune-regulating cells from arriving via the bloodstream to control the infection [2]. Heme supplied by red blood cells is thought to be a substrate leading to increased pathogenicity [2]. The rich blood supply to the head and neck allows the fungus to cause rhinocerebral mucormycosis – the most common site of infection [17].
Treatment of invasive mucormycosis involves the use of antifungals, with liposomal amphotericin B being the drug of choice [18]. It is well-known to cause renal impairment and electrolyte abnormalities such as the hypokalemia, which developed in our patient [19]. Early potassium supplementation (within 2 days of the initiation of liposomal amphotericin B) reduces the risk of liposomal amphotericin B-induced hypokalemia [19].
Conclusions
In summary, invasive mucormycosis is a rare, life-threatening infection most commonly seen in patients with depressed immunity. Our patient’s history of DM, cancer, and dexamethasone use put her at risk for it because of immunosuppression; however, her presentation is rare, as she only received dexamethasone for a brief time. Liposomal amphotericin B is the mainstay of therapy for invasive mucormycosis, along with surgical intervention, and clinicians should remain vigilant for complications associated with it. A multidisciplinary approach is suggested for successful treatment of this devastating disease.
Figures
Tables
Table 1.. Clinical course.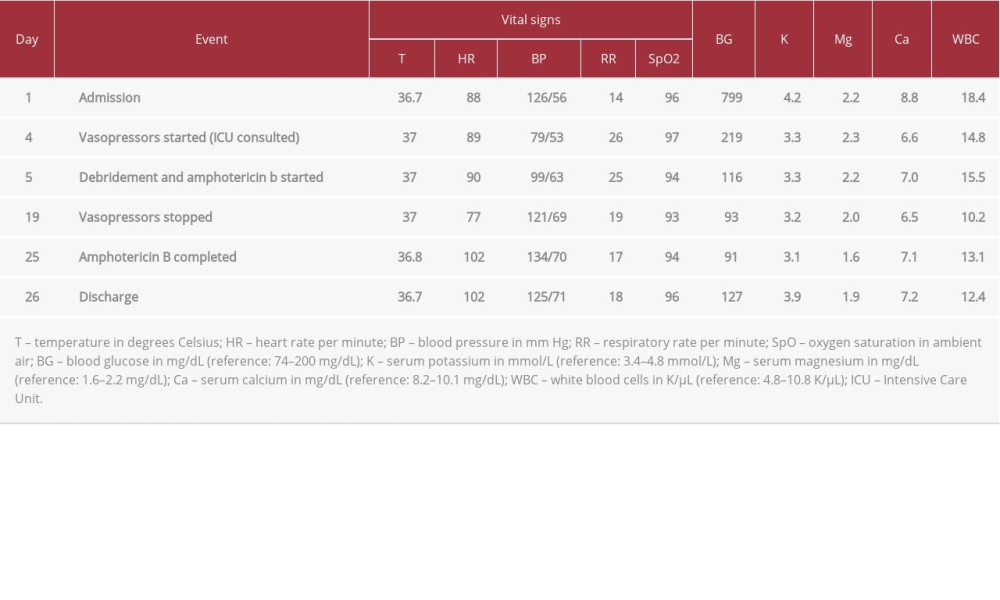
References:
1.. Roden MM, Zaoutis TE, Buchanan WL, Epidemiology and outcome of zygomycosis: A review of 929 reported cases: Clin Infect Dis, 2005; 41; 634-53
2.. Ibrahim AS, Spellberg B, Walsh TJ, Kontoyiannis DP, Pathogenesis of mucormycosis: Clin Infect Dis, 2012; 54(Suppl.1); S16-22
3.. Spellberg B, Edwards J, Ibrahim A, Novel perspectives on mucormycosis: Pathophysiology, presentation, and management: Clin Microbiol Rev, 2005; 18; 556-69
4.. Prakash H, Chakrabarti A, Global epidemiology of mucormycosis: J Fungi, 2019; 5; 26
5.. Hoang K, Abdo T, Reinersman JM, Lu R, Higuita N, A case of invasive pulmonary mucormycosis resulting from short courses of corticosteroids in a well-controlled diabetic patient: Med Mycol Case Rep, 2020; 29; 22-24
6.. Tran D, Schmit B, An aggressive case of mucormycosis: Cureus, 2020; 12; e9610
7.. Guarner J, Brandt ME, Histopathologic diagnosis of fungal infections in the 21st century: Clin Microbiol Rev, 2011; 24; 247-80
8.. Werthman-Ehrenreich A, Mucormycosis with orbital compartment syndrome in a patient with COVID-19: Am J Emerg Med, 2021; 42; 264
9.. Reid G, Lynch JP, Fishbein MC, Clark NM, Mucormycosis: Semin Respir Crit Care Med, 2020; 41; 99-114
10.. Danion F, Aguilar C, Catherinot E, Mucormycosis: New developments into a persistently devastating infection: Semin Respir Crit Care Med, 2015; 36; 692-705
11.. Brunet K, Rammaert B, Mucormycosis treatment: Recommendations, latest advances, and perspectives: J Mycol Med, 2020; 30; 101007
12.. Prakash H, Chakrabarti A, Epidemiology of mucormycosis in India: Microorganisms, 2021; 9; 523
13.. Di Carlo P, Pirrello R, Guadagnino G, Multimodal surgical and medical treatment for extensive rhinocerebral mucormycosis in an elderly diabetic patient: A case report and literature review: Case Rep Med, 2014; 2014; 527062
14.. Kim ST, Kim WS, Lee HH, Kim JY, Successful treatment of invasive rhinopulmonary mucormycosis with an indolent presentation by combined medical and surgical therapy: J Craniofac Surg, 2013; 24; e182-84
15.. Jiang RS, Hsu CY, Endoscopic sinus surgery for rhinocerebral mucormycosis: Am J Rhinol, 1999; 13; 105-9
16.. Vironneau P, Verillaud B, Tran H, [Rhino-orbito-cerebral mucormycosis, surgical treatment, state of the art]: Med Sci (Paris), 2013; 29; 31-35 [in French]
17.. Kolekar JS, Rhinocerebral mucormycosis: A retrospective study: Indian J Otolaryngol Head Neck Surg, 2015; 67; 93-96
18.. Cornely OA, Alastruey-Izquierdo A, Arenz D, Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium: Lancet Infec Dis, 2019; 19; e405-21
19.. Okada N, Azuma M, Imanishi M, Potential usefulness of early potassium supplementation for preventing severe hypokalemia induced by liposomal amphotericin B in hematologic patients: A retrospective study: Clin Ther, 2018; 40; 252-60
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








