03 August 2021: Articles 
Role of Emergent Nephrectomy for Grade V Blunt Renal Injuries
Unusual clinical course, Challenging differential diagnosis, Management of emergency care
John D. Ehrhardt Jr.1ABCDEF, Adel Elkbuli1ABCDEF*, Mark McKenney12ACDE, Dessy Boneva12ABCDEFDOI: 10.12659/AJCR.932357
Am J Case Rep 2021; 22:e932357
Abstract
BACKGROUND: Blunt renal injuries constitute a small proportion of solid organ trauma cases. Many American Association for the Surgery of Trauma grade IV and V lacerations are manageable with volume resuscitation and angioembolization. In select cases, emergent nephrectomy can be beneficial to patients, with little associated morbidity.
CASE REPORT: In 2 separate cases, an 18-year-old man and a 21-year-old woman were brought to our center after sustaining blunt trauma to the left flank. They were both found to have isolated grade V renal lacerations with vascular compromise. Both initially had normal vital signs but became unstable. Active extravasation was visible on contrast-enhanced computed tomography scans, and the patients ultimately underwent exploratory laparotomy and nephrectomy on hospital day 1. Both of them recovered quickly, had no acute complications, and were discharged in <1 week. Follow-up over the course of 1 year showed no untoward sequelae.
CONCLUSIONS: These cases highlight the role of nephrectomy to mitigate life-threatening hemorrhage in unstable patients. While observation or angioembolization is the preferred approach for many renal injuries, emergent nephrectomy remains important for patients who do not respond to blood products and have rapidly deteriorating shock. In these patients, results of an initial trauma evaluation can be unclear because of concomitant splenic injury, as well as renal injuries with hemoperitoneum that are visible on focused abdominal ultrasonography for trauma. When forgoing immediate laparotomy, surgeons can use continuous noninvasive hemoglobin monitoring along with serial hemoglobin measurements and abdominal examinations. Laparotomy with nephrectomy results in limited morbidity when it is done expeditiously with ongoing volume resuscitation.
Keywords: Abdominal Injuries, Lacerations, Nephrectomy, Adolescent, Kidney, Spleen, Wounds, Nonpenetrating, young adult
Background
Eight percent to 10% of injuries to abdominal organs are caused by renal trauma [1]. Contemporary management of most renal lacerations is medical. Patients who are hemodynamically stable or respond to volume resuscitation can be candidates for observation or endovascular therapy even if they have American Association for the Surgery of Trauma (AAST) grade IV and V lesions (Table 1) [2], which include renovascular compromise and shattered kidneys [3]. Observation involves serial abdominal examinations, short-interval hemoglobin measurements (every 4-6 h), and volume resuscitation. Endovascular therapy most often involves selective catheterization and angioembolization of active renal vessel extravasation [4]. Given these trends, scenarios in which patients undergo acute nephrectomy have become uncommon and noteworthy. The present series highlights 2 patients who underwent nephrectomy after experiencing blunt renal trauma. In these cases, the departure from what is considered standard nonsurgical management informs a discussion about the clinical scenarios in which nephrectomy may be beneficial when performed urgently or emergently. In highly select cases, acute nephrectomy after severe blunt trauma can be lifesaving and actually attenuate a patient’s risk of morbidity and mortality.
Case Reports
CASE 1:
A healthy 18-year-old man presented to our Trauma Center after a blow to his left flank during an American football game. On arrival, he had a Glasgow Coma Scale (GCS) score of 15, was normotensive, saturating well on room air, and in normal sinus rhythm on cardiac monitoring. His primary symptom was isolated left flank pain and he had only minimal abdominal tenderness with no peritoneal signs. Initial computed tomography (CT) of the abdomen and pelvis revealed a lacerated, anterolaterally displaced left kidney with an associated perinephric hematoma that measured 10.5 cm in maximal diameter (Figure 1). There was no evidence of active extravasation. Although the patient was hemodynamically stable, his imaging findings warranted admission to the Trauma Intensive Care Unit (ICU) for serial hemoglobin measurements and abdominal examinations. His hemoglobin values declined from 14 g/dL to 8.5 g/dL overnight and his base deficit worsened to −8. A repeat CT of the abdomen and pelvis with 5-min delays showed a fractured left kidney. The perinephric hematoma had grown to a maximum diameter of 15 cm and there was segmental artery dissection, contrast extravasation from the left renal pedicle, and hemoperitoneum. Overnight, the patient also had developed tachycardia and progressively worsening, diffuse, peritoneal abdominal pain. Given his newly acute abdomen, increasing tachycardia despite administration of crystalloid and blood products, and the interval radiographic evolution of his left renal injury with vascular compromise, the patient was taken to the Operating Room (OR). An exploratory laparotomy revealed hemoperitoneum and a zone II retroperitoneal hematoma atop the left kidney. Vascular control of the renal vessels was obtained medial to the left inferior mesenteric vein. Further retroperitoneal exposure was accomplished through left medial visceral rotation (Mattox maneuver) for left nephrectomy with sparing of the left adrenal gland. The remainder of the exploration was negative and the patient’s abdomen was irrigated and primary closure of the fascia was performed. He received a transfusion of 5 units of packed red blood cells.
After surgery, the patient’s condition improved significantly and he was discharged on hospital day 5. His creatinine level on arrival was 1.3, peaked at 1.8 on the day after surgery, and resolved to 1.2 on discharge. He did not require hemodialysis during his hospitalization or follow-up. His further recovery and follow-up visits in the Trauma Clinic were uncomplicated.
CASE 2:
A healthy 21-year-old woman presented to our Trauma Center as a transfer from an outside hospital. There was concern for a splenic injury because she had been involved in an all-terrain vehicle accident and was ejected from the passenger seat. On arrival, her GCS score was 15 and she was tachycardic to 115 bpm. She was normotensive, saturating well on room air, and had severe abdominal pain and left-sided upper- and lower-extremity pain from her orthopedic injuries. Her abdominal examination was notable for left-sided abdominal tenderness with voluntary guarding. A focused assessment with sonography in trauma (FAST) examination of the left upper quadrant demonstrated modest free fluid in the splenorenal window. Laboratory analysis was significant for a hemoglobin of 8.9 g/dL and base deficit of −8. Prior to the patient’s transfer, her hemoglobin was 11 g/dL, which supported the decision to begin blood product transfusion. Fortunately, the patient’s well-compensated hemodynamic status allowed for further evaluation. Contrast-enhanced CT of the abdomen and pelvis with 5-min delays revealed a shattered left kidney with active renal arterial extravasation, complete renal devascularization, and a large perinephric hematoma (Figure 2). Interventional Radiology (IR) became involved, but before their intervention could begin, the patient became tachycardic to 130 bpm with hypotension that did not respond to blood product transfusion, which informed the decision for emergent laparotomy. Intraoperatively, there was some breakthrough hemoperitoneum, but the patient’s spleen and other abdominal viscera were uninjured. The tense retroperitoneal hematoma was entered medial to the inferior mesenteric vein, clots were evacuated, and the renal vessels were ligated with sutures. The patient’s fractured left kidney was removed, her abdomen was systematically explored for additional injuries, and her abdominal fascia was ultimately closed primarily. After surgery, the patient was resuscitated in the Trauma ICU and her acidosis (which reached a nadir of base deficit −12) and anemia from acute blood loss were corrected. She received a total of 5 units of blood product components. She was extubated the day after surgery and discharged 4 days later. Outpatient follow-up in our Trauma Clinic showed that she had made a full recovery. She did not need hemodialysis during her hospitalization or follow-up. She continued to receive outpatient orthopedic care at our center for more than 1 year and was otherwise functional, healthy, and had no untoward renal dysfunction on routine laboratory analysis.
Discussion
The present series highlights 2 cases of isolated, high-grade, blunt renal trauma (Table 2). The patients in this series arrived with normal vital signs but deteriorated, with shock and worsening abdominal examinations. They both became unresponsive to fluids and required transfusion of multiple blood products. The decision to operate was based on the rate at which these patients became clinically unstable despite ongoing volume resuscitation.
Modern evidence-based therapy for renal injuries is largely focused on the power of either nonsurgical treatment or IR. The latest literature is replete with descriptions of advances in endovascular therapy for renal trauma [5,6]. Overall, only about 8% of all patients with renal trauma are managed with nephrectomy [7]. As the frontier broadens for endovascular techniques, it remains important to further clarify and discuss which cases should be managed surgically. For these reasons, surgical decision-making for severe renal trauma is dynamic, nuanced, and complex. In both cases presented here, IR was available for possible angioembolization and involved in discussing these cases. However, given the rate at which these patients deteriorated, with signs of hemorrhagic shock and acute abdomen, the IR team agreed with surgical management over an endovascular approach for angioembolization.
In certain circumstances, exploratory laparotomy can be the safest maneuver for patients with AAST grades IV and V renal injuries who are unresponsive or have only a transient response to volume resuscitation. The 2019 kidney and urologic trauma practice guidelines from the World Society of Emergency Surgery (WSES) and AAST outlined evidence about when surgery is advisable (Table 3) [8]. This subcategory includes patients who are hemodynamically unstable or do not respond to transfusion of blood products, as well as those with severe, uncontrolled renovascular bleeding. Transient responders also may be candidates for surgery during the acute period. This subgroup of patients may respond to volume resuscitation for a given, as-yet-undefined interval, but by definition in the WSES-AAST literature, they are not considered clinically stable enough for observation or for IR procedures.
A delayed surgical repair should be considered for patients with renal pelvis leaks that are not amenable to endoscopic therapy. In some cases, renal devascularization can cause dysregulated renin-angiotensin-aldosterone feedback, leading to unremitting hypertensive emergencies. At times, these cases can be tenuous to manage without nephrectomy, especially when they occur in adults who have other cardiovascular comorbidities.
Defining an indication for trauma nephrectomy assumes that the injury pattern is clearly delineated or that there is isolated renal trauma. When patients have hemoperitoneum, and with severe left kidney injuries in general, there is a natural concern for associated splenic injury. Even in patients who do not have concomitant abdominal visceral injuries, severe blunt renal trauma can create clinical and radiographic signs that lead surgeons to the OR. A large perinephric hematoma can be perceived as positive with a FAST examination in the splenorenal view. Traumatic disruption or preexisting discontinuity in Gerota’s anterior renal fascia can decompress a retroperitoneal tamponade with an expanding perinephric hematoma [9]. The resultant retroperitoneal hematoma leak creates hemoperitoneum, which represents ongoing hemorrhage into a larger space. This can contribute to worsening shock and peritonitis, which would be viewed as a valid reason to operate.
Intraoperative discovery of a devastating renal injury merits special consideration. Some patients are taken to the OR with an acute abdomen and hemodynamic instability before CT imaging is obtained. Cases also arise in austere clinical settings in which advanced imaging is not available. The classic dictum is to explore all penetrating zone II retroperitoneal hematomas, but to only do so in cases of blunt trauma when the lesions are pulsatile or expanding [10]. Left medial visceral rotation with the Mattox maneuver provides exposure for the left kidney; right renal exposure is accomplished through a right medial visceral rotation, known as the Cattell-Braasch maneuver [11,12]. The 2019 WSES-AAST kidney and urologic trauma guidelines state that with renal devascularization, having a non-viable kidney is not an indication to operate in the acute setting. However, a nephrectomy is justifiable when a shattered kidney is discovered intraoperatively. In some cases, the presence of concomitant visceral injuries can be a source of contamination, and leaving a retained devascularized kidney could be a nidus for a retroperitoneal abscess.
From a critical care standpoint, managing a trauma patient who has a retained, devascularized kidney is not without risk. For grade IV and V injuries managed without surgery, the potential for continued hemorrhage or rebleeding is a valid concern. These patients can be closely monitored with serial short-interval hemoglobin and hematocrit measurements. There may be a role for modern, minimally invasive, continuous hemoglobin monitoring technology, like the Masimo system [13]. Again, the stress of unchecked hypovolemia during the resuscitative phase can be detrimental to renal function in a patient’s remaining solitary kidney.
Retention of a shattered kidney also can predispose a patient to urinary leaks or urinoma, increasing the risk for sepsis. In general, urinary leaks should be repaired with stents or diverted appropriately with drains provided by IR and Urology [14]. Delayed recognition and control of these complications can worsen sepsis. Acute respiratory distress syndrome and multiorgan dysfunction can ensue. Treatment of sepsis requires use of broad-spectrum antibiotics, some of which are nephrotoxic, and should be used judiciously in patients who have only a solitary functional kidney. This is even more important in patients who have multiple medical comorbidities, such as geriatric individuals, who are the fastest-growing subset of trauma patients in the United States [15].
The potential complications associated with nonsurgical management of severe renal trauma should be contrasted with the morbidity of nephrectomy. In general, laparotomy poses an inherent risk of surgical site infection and future hernia formation. Short- and long-term outpatient urological care should be a priority for patients who are discharged after undergoing a nephrectomy.
Conclusions
Management of AAST grades IV and V renal injuries is dominated by medical care with observation, volume resuscitation, and sometimes angioembolization. For patients who are acutely unstable, respond transiently to transfusion of blood products, or who develop an acute abdomen, there is still a role for laparotomy with nephrectomy. Nephrectomy may be inevitable in situations in which unstable patients with bleeding are brought directly to the OR and renovascular disruption is identified intraoperatively. In the present series, we have described 2 cases of trauma nephrectomy in young adults who had signs of worsening shock. The satisfactory outcomes are attributable to intensive monitoring with little to no delay in definitive management after their clinical deterioration. Endovascular therapy will continue to play a significant role in these cases. Knowing when to convert from nonsurgical therapy to surgery is crucial for management of patients with renal injuries. In most trauma patients, morbidity associated with nephrectomy is related to inadequate volume resuscitation or delays in definitive control of the injury. In the present cases, prompt resuscitation and surgical intervention were followed by an uncomplicated recovery with no need for hemo-dialysis. Surgeons and interventionalists will continue to collaborate to provide the highest-quality care for patients with renal trauma, who have a diverse spectrum of injuries, all of which require deliberate and tailored care.
Figures
References:
1.. Erlich T, Kitrey ND, Renal trauma: The current best practice: Ther Adv Urol, 2018; 10(10); 295-303
2.. Keihani S, Rogers DM, Putbrese BE, The American Association for the Surgery of Trauma renal injury grading scale: Implications of the 2018 revisions for injury reclassification and predicting bleeding interventions: J Trauma Acute Care Surg, 2020; 88(3); 357-65
3.. Petrone P, Perez-Calvo J, Brathwaite CEM, Traumatic kidney injuries: A systematic review and meta-analysis: Int J Surg, 2020; 74; 13-21
4.. Johnsen NV, Betzold RD, Guillamondegui OD, Surgical management of solid organ injuries: Surg Clin North Am, 2017; 97(5); 1077-105
5.. Lanchon C, Fiard G, Arnoux V, High grade blunt renal trauma: Predictors of surgery and long-term outcomes of conservative management. A prospective single center study: J Urol, 2016; 195(1); 106-11
6.. McCombie SP, Thyer I, Corcoran NM, The conservative management of renal trauma: a literature review and practical clinical guideline from Australia and New Zealand: BJU Int, 2014; 114(Suppl.1); 13-21
7.. Keihani S, Xu Y, Presson AP, Contemporary management of high-grade renal trauma: Results from the American Association for the Surgery of Trauma Genitourinary Trauma study: J Trauma Acute Care Surg, 2018; 84(3); 418-25
8.. Coccolini F, Moore EE, Kluger Y, Kidney and uro-trauma: WSES-AAST guidelines: World J Emerg Surg, 2019; 14; 54
9.. Fu CY, Wu SC, Chen RJ, Evaluation of need for angioembolization in blunt renal injury: Discontinuity of Gerota’s fascia has an increased probability of requiring angioembolization: Am J Surg, 2010; 199(2); 154-59
10.. Kobayashi LM, Costantini TW, Hamel MG, Abdominal vascular trauma: Trauma Surg Acute Care Open, 2016; 1(1); e000015
11.. Mattox KL, McCollum WB, Beall AC, Management of penetrating injuries of the suprarenal aorta: J Trauma, 1975; 15(9); 808-15
12.. Cattell RB, Braasch JW, A technique for the exposure of the third and fourth portions of the duodenum: Surg Gynecol Obstet, 1960; 111; 378-79
13.. Galvagno SM, Hu P, Yang S, Accuracy of continuous noninvasive hemoglobin monitoring for the prediction of blood transfusions in trauma patients: J Clin Monit Comput, 2015; 29(6); 815-21
14.. Anselmo da Costa I, Amend B, Stenzl A, Bedke J, Contemporary management of acute kidney trauma: J Acute Dis, 2016; 5(1); 29-36
15.. Adams SD, Holcomb JB, Geriatric trauma: Curr Opin Crit Care, 2015; 21(6); 520-26
Figures
Tables
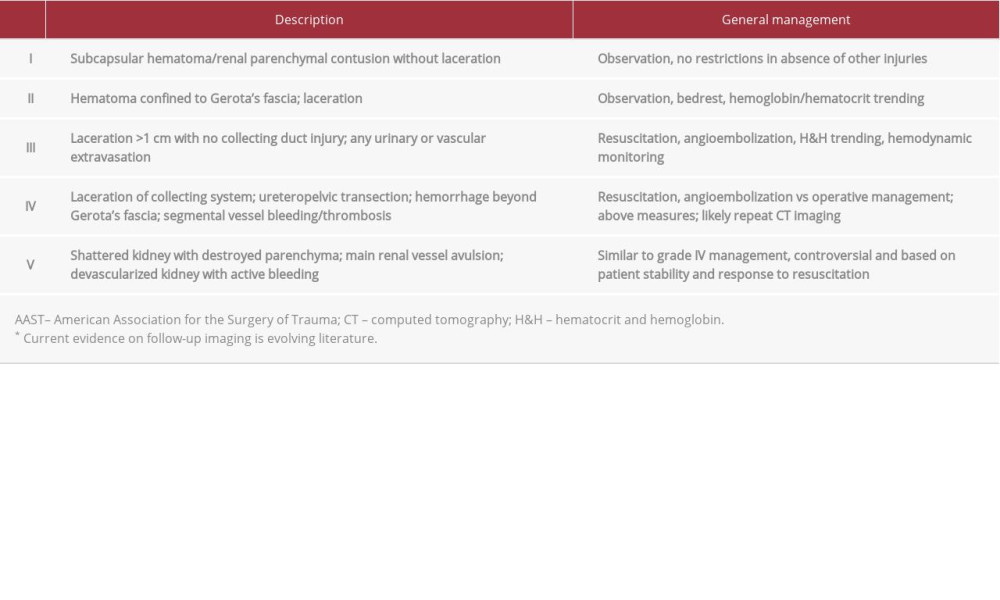 Table 1.. AAST Revised 2018 Renal Injury Grading Scale [2].
Table 1.. AAST Revised 2018 Renal Injury Grading Scale [2].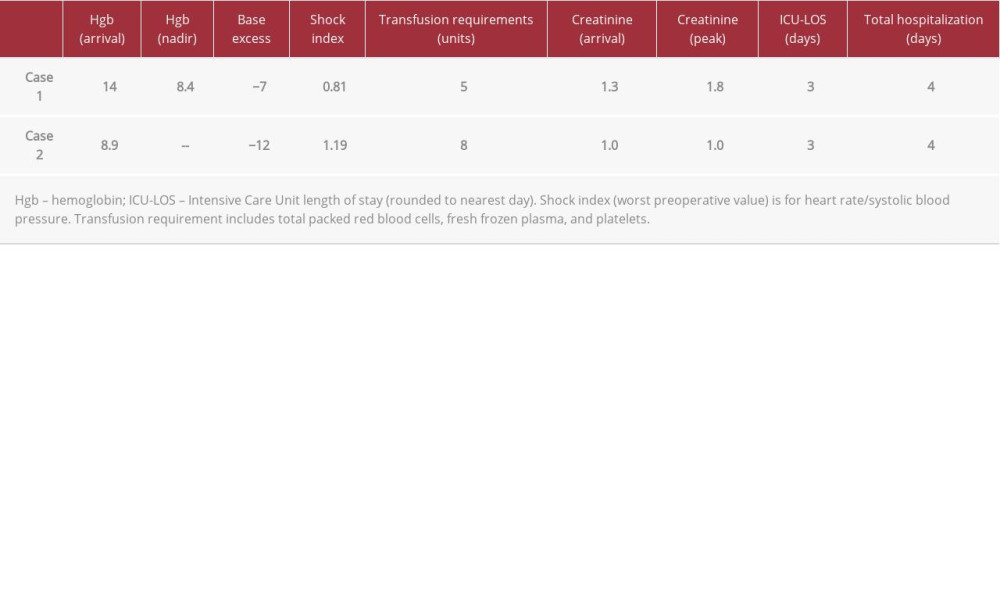 Table 2.. Comparison of nephrectomy cases.
Table 2.. Comparison of nephrectomy cases. Table 3.. WSES-AAST 2019 considerations for trauma nephrectomy [8].
Table 3.. WSES-AAST 2019 considerations for trauma nephrectomy [8]. Table 1.. AAST Revised 2018 Renal Injury Grading Scale [2].
Table 1.. AAST Revised 2018 Renal Injury Grading Scale [2]. Table 2.. Comparison of nephrectomy cases.
Table 2.. Comparison of nephrectomy cases. Table 3.. WSES-AAST 2019 considerations for trauma nephrectomy [8].
Table 3.. WSES-AAST 2019 considerations for trauma nephrectomy [8]. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








