07 May 2022: Articles 
Successful Resuscitation of Cardiac Arrest After Refeeding Syndrome Associated with Hiatal Hernia: A Case Report
Diagnostic / therapeutic accidents, Management of emergency care, Rare coexistence of disease or pathology
Kazumasa Kotake1ABCDEF*, Takashi Hongo2ABCDE, Hiroki Sugiyama3B, Narusato Iizuka4B, Noriya Momoki3B, Yasuhiro Kawakami1DDOI: 10.12659/AJCR.935605
Am J Case Rep 2022; 23:e935605
Abstract
BACKGROUND: Refeeding syndrome (RFS) is a life-threatening syndrome, which can cause sudden death. RFS has been reported frequently in young patients with anorexia without organic disease; however, there are few reports in elderly patients with organic disease. Herein, we report a case of cardiac arrest after refeeding syndrome associated with hiatal hernia.
CASE REPORT: We report the case of a 59-year-old woman who had a diagnosis of RFS during treatment for anorexia secondary to hiatal hernia. She was hospitalized with hypothermia, anemia, and hypovolemic shock and treated with electrolytes, hydration, and transfusion at the Emergency Department. Upper gastrointestinal endoscopy revealed hiatal hernia with severe reflux esophagitis. We initiated parenteral nutrition (8.7 kcal/kg/day). However, QTc prolongation caused pulseless ventricular tachycardia. Temporary cardiac pacing was performed to prevent recurrence. Her nutritional status steadily improved, and she was transferred to another hospital without complications.
CONCLUSIONS: Patients with gastrointestinal comorbidities are more likely to have inadequate food intake and to be undernourished on admission and therefore should be carefully started on nutritional therapy, considering their risk of RFS.
Keywords: Hernia, Hiatal, refeeding syndrome, Resuscitation, Anorexia, anorexia nervosa, Female, Heart Arrest, Humans
Background
Refeeding syndrome (RFS) is a group of metabolic changes caused by rapid nutrient administration in cases of hypovolemia, which may be induced by extreme and prolonged starvation [1]. Although there are no clear diagnostic criteria for RFS, it is a life-threatening syndrome that may cause sudden death. The 2006 guidelines of the National Institute for Health and Care Excellence (NICE) described RFS [2], yet many clinicians are not aware of problem and RFS still occurs [3]. Although there have been many reports of RFS in young patients with anorexia nervosa without organic disease [4], there are few reports of RFS in elderly patients with organic disease, and the pathogenesis varies [5]. Herein, we report the case of a patient who suffered cardiac arrest after RFS secondary to hiatal hernia.
Case Report
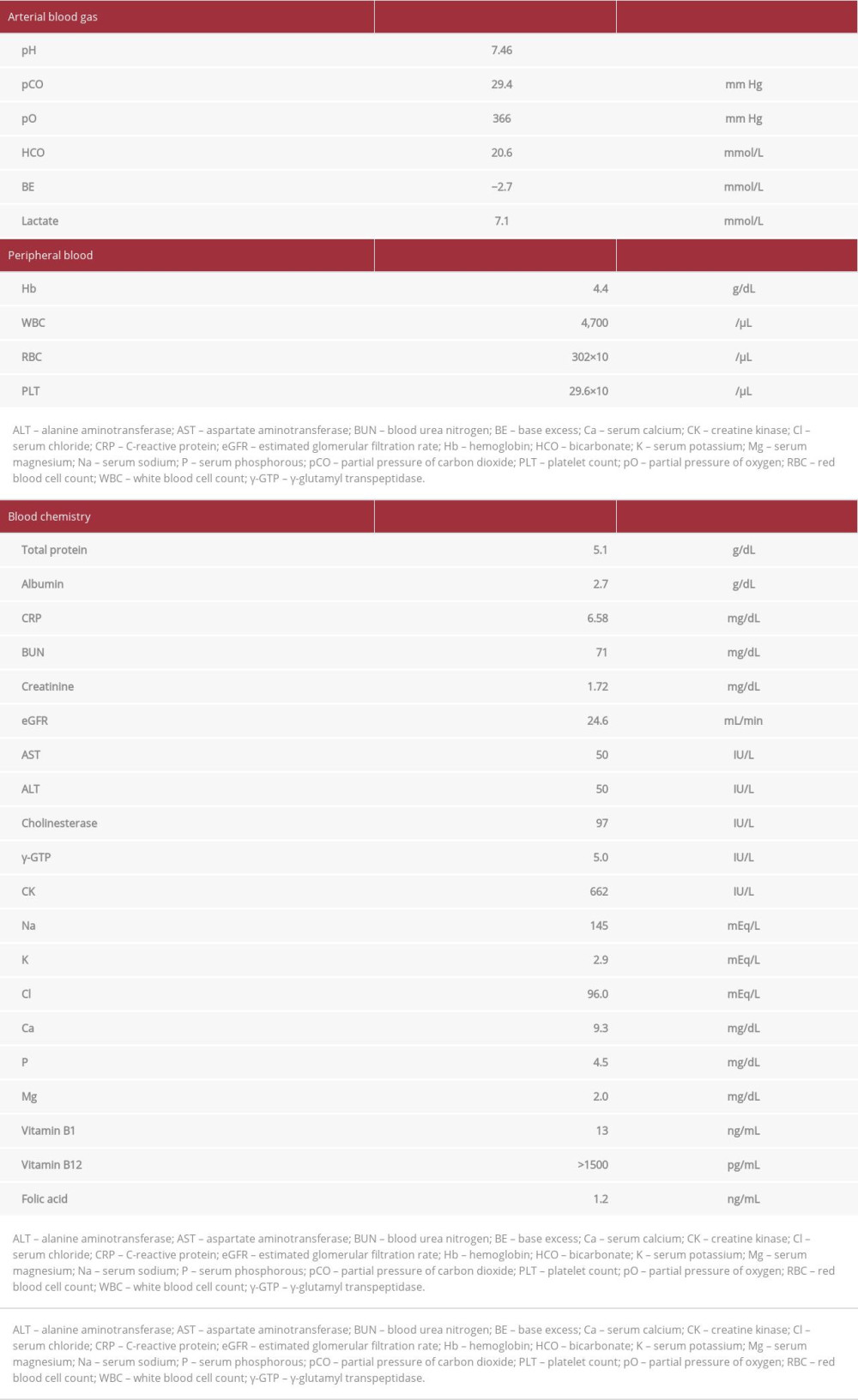
The patient, a 59-year-old woman, had been feeling ill for nearly 1 year, although she never visited a hospital. For approximately 1 month prior to hospital admission, she was bedridden and had a low intake of food. Her husband found her lying in vomit and presented her to our Emergency Department. The patient’s body weight and body mass index (BMI) were 32.3 kg and 16.5 kg/m2, respectively. Her vital signs upon admission were as follows: respiratory rate, 20 breaths/min; blood pressure and peripheral capillary oxygen saturation, undetectable; heart rate, 40 beats/min; body temperature, 27.5°C; and Glasgow Coma Scale score, 7 (E1V1M5). The laboratory test results are shown in Table 1.
We treated the patient with a rapid infusion of Ringer’s acetate solution (500 mL/h) as the extracellular fluid and a blood trans-fusion (2 units) for anemia (initial hemoglobin level of 44 g/dL). We treated the hypothermia by rewarming her with a warm-air blanket, after which her body temperature increased from 27.5°C to 36.0°C in 8.5 h (mean rewarming rate: 1.0°C/h). As shown in Table 1, the serum potassium level was low, but the patient was followed up without potassium correction, considering the risk of hyperkalemia due to renal dysfunction and re-release of intracellular potassium by rewarming.
As the patient was unconscious and had prolonged low-calorie intake at the time of admission, we considered the possibility of Wernicke’s encephalopathy and administered fursultiamine 1500 mg/day for 2 days, followed by 5 days of 1000 mg intravenous (IV) bolus injections (Figure 1). Because of the low serum vitamin B1 concentration of 13 ng/mL (reference value: 24–66 ng/mL), fursultiamine 100 mg/day was orally administered for 5 days after completion of the IV administration. Upper endoscopy was performed to investigate the cause of severe anemia and revealed the presence of a hiatal hernia with severe reflux esophagitis (Figure 2A); therefore, we administered omeprazole twice daily as a proton pump inhibitor.
On the first day after admission, we initiated total parenteral nutrition at 280 kcal/day (8.7 kcal/kg/day). Immediately following the initiation of parenteral nutrition, electrocardiographic monitoring showed a sinus rhythm. However, a few hours later, there was an episode of marked QT interval prolongation (QT 0.64 s), resulting in pulseless ventricular tachycardia (VT) (Figure 3A). Chest compressions were started immediately; however, the QT prolongation continued. Therefore, we administered continuous IV potassium chloride and a bolus of 1 g magnesium sulfate IV, followed by a continuous infusion of a total of 0.5 g magnesium sulfate over the next 6 h. The potassium chloride dosage was adjusted according to the results of the blood gas analysis (Figure 1). Consequently, the electrocardiographic monitoring changed from a pulseless VT to sinus rhythm. However, because the QT prolongation continued (QTc 0.68 s), a temporary pacemaker was inserted through the left internal jugular vein to prevent the recurrence of arrhythmia, and overdrive pacing was started at a heart rate of 70 beats/min.
On day 2 of hospitalization, the QT prolongation improved (QTc 0.520 s). However, blood tests revealed low serum phosphorus levels; therefore, dibasic potassium phosphate solution was administered IV.
On day 3 of hospitalization, the corrected QT (QTc) prolongation had improved (QTc 0.473 s) on the 12-lead electrocardiogram (Figure 3B), and temporary cardiac pacing was discontinued. To prevent the recurrence of RFS, we increased the patient’s nutrition in increments of 200 kcal/day (6.2 kcal/kg/day).
On day 19 of hospitalization, upper endoscopy revealed that the reflux esophagitis had improved (Figure 2B). Therefore, the feeding route was changed from a central venous catheter to a transduodenal tube. The patient’s nutritional status gradually improved; her weight increased to 36.9 kg and her BMI to 18.8 kg/m2. On day 30 of hospitalization, she was transferred to another hospital without any complications.
Discussion
To the best of our knowledge, this is the first report of RFS in a patient with hiatal hernia. In addition, this is a valuable case of severe QTc prolongation with subsequent cardiac arrest following nutrient administration, which was improved by temporary cardiac pacing.
RFS is associated with water and electrolyte imbalances after the administration of nutrition to starving patients. In the hypotrophic state, the supply of sugar is reduced, lipid metabolism is altered, and insulin secretion is decreased [1]. However, when dietary sugar is supplied, excessive insulin is secreted, resulting in rapid glucose metabolism in the cells. Hypophosphatemia develops because phosphorus is consumed for energy synthesis. As insulin secretion is stimulated, the cellular uptake of potassium and magnesium also increases rapidly. Consequently, hypokalemia and hypomagnesemia may worsen, leading to potentially fatal arrhythmias.
With the onset of RFS, the cardiovascular, respiratory, neurological, and hematological systems may be affected which can lead to multiple organ failure and death in the most severe cases [1]. In particular, cardiac disease has been reported to cause Torsades de pointes, with marked QT prolongation and ventricular tachyarrhythmias in several cases [6,7]. The patient involved in our report also experienced QT prolongation, suggesting a similar mechanism leading to pulseless VT.
In cases of refractory arrhythmias that are difficult to control with pharmacological therapy, as in the present case, ventricular overdrive pacing can be considered as a non-pharmacological treatment [8]. It has been reported that continuous pacing at heart rates above self-regulation reduces the heterogeneity of the refractory period and suppresses abnormal automatic capacity and extrasystoles that trigger ventricular tachycardia and ventricular fibrillation [8]. Our patient was treated with electrolyte correction, but since QT prolongation did not improve and her circulation was stable, ventricular overdrive pacing was performed based on poor control on pharmacologic therapy. In this case, pacing at 70 beats/min completely suppressed the arrhythmia, and QT prolongation improved approximately 1 day after pacing was initiated.
The NICE guidelines state that energy input should be started at a maximum of 5 kcal/kg/day and increased slowly to reach the maximum level by 4 to 7 days to avoid RFS in patients with a BMI <14 kg/m2 or those who have had little or no nutrition for more than 15 days [2]. However, there is no definitive recommendation for daily caloric intake in RFS. As our patient had a low BMI (16.5 kg/m2) and had not eaten well for 3 weeks due to vomiting, parenteral nutrition was started at <10 kcal/kg/day. However, the patient developed RFS at this energy level. After stabilization of the patient’s cardiac condition, we increased her nutrition gradually by 200 kcal/day. Based on the NICE guidelines and our report, nutritional supplementation should be started at 5 kcal/kg/day for patients at a high risk of RFS.
Because our patient was unconscious at the time of hospital admission, we administered fursultiamine at an early stage in consideration of the potential onset of Wernicke’s encephalopathy. Fursultiamine is a vitamin B1 derivative used as a co-enzyme in glucose metabolism. In situations in which rapid glucose metabolism occurs, such as in RFS, a large amount of fursultiamine is used [9]. The patient’s serum vitamin B1 level upon admission was low, at 13 ng/mL (reference values: 24–66 ng/mL), indicating that fursultiamine supplementation was necessary. However, there is currently no clear recommendation for the dose and duration of fursultiamine administration, rendering this a topic for further study.
Young patients with anorexia nervosa without organic disease are at high risk for refeeding syndrome and are often given attention, but it is not recognized in elderly patients with underlying disease, such as the present case, and may be missed [3].
It has been reported that malnourished patients with inflammatory bowel disease, liver cirrhosis, and chronic intestinal insufficiency and patients who have undergone endoscopic gastrostomy due to long-term dysphagia are at higher risk of RFS in gastroenterology practice [10]. Nutritional therapy for patients with gastrointestinal complications, not only in this case, should be started at a low dose in accordance with NICE guidelines to prevent the development of RFS.
Conclusions
We report a case of successful resuscitation of cardiac arrest after RFS associated with hiatal hernia. Patients with gastrointestinal complications are more likely to have inadequate food intake and be undernourished on admission, so nutritional therapy should be started at a low dose according to NICE guidelines. Treatment with a temporary pacemaker may be implemented in cases of RFS with arrhythmia including QTc prolongation. Additionally, over-pacing may be an alternative option to prevent lethal arrhythmia.
Figures
References:
1.. Crook MA, Hally V, Panteli JV, The importance of the refeeding syndrome: Nutrition, 2001; 17; 632-37
2.. , Nutrition support for adults: oral nutrition support, enteral tube feeding and parenteral nutrition: National Institute for Health and Care Excellence Clinical Guideline, 2006 . Accessed 1 May 2021https://www.nice.org.uk/guidance/cg32
3.. Wirth R, Diekmann R, Fleiter O, [Refeeding syndrome in geriatric patients : A frequently overlooked complication.]: Z Gerontol Geriatr, 2018; 51; 34-40 [in German]
4.. Usdan LS, Khaodhiar L, Apovian CM, The endocrinopathies of anorexia nervosa: Endocr Pract, 2008; 14; 1055-63
5.. Aubry E, Friedli N, Schuetz P, Stanga Z, Refeeding syndrome in the frail elderly population: Prevention, diagnosis and management: Clin Exp Gastroenterol, 2018; 11; 255-64
6.. Inoue T, Doi T, Beppu K, Warning to “Refeeding syndrome”. Torsades de pointes and ventricular tachyarrhythmia with marked QT prolongation induced by acute glucose injection: report of two cases: Int J Cardiol, 2012; 156; 222-24
7.. Nakashima T, Kubota T, Takasugi N, Hyperglycemia and subsequent torsades de pointes with marked QT prolongation during refeeding: Nutrition, 2017; 33; 145-48
8.. Kurisu S, Inoue I, Kawagoe T, Temporary overdriving pacing as an adjunct to antiarrhythmic drug therapy for electrical storm in acute myocardial infarction: Circ J, 2005; 69; 613-16
9.. Pacei F, Iaccarino L, Bugiardini E, Wernicke’s encephalopathy, refeeding syndrome and wet beriberi after laparoscopic sleeve gastrectomy: The importance of thiamine evaluation: Eur J Clin Nutr, 2020; 74; 659-62
10.. Nunes G, Brito M, Santos CA, Fonseca J, Refeeding syndrome in the gastroenterology practice: how concerned should we be?: Eur J Gastroenterol Hepatol, 2018; 30; 1270-76
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133