27 June 2022: Articles 
Bilateral Emphysematous Pyelonephritis Associated with COVID Pneumonia: A Case Report
Unusual clinical course, Challenging differential diagnosis, Diagnostic / therapeutic accidents, Unusual setting of medical care, Unexpected drug reaction, Educational Purpose (only if useful for a systematic review or synthesis), Rare coexistence of disease or pathology
Slaviša Savić1ADE*, Tadija Pejović1BC, Nataša Savić2DFDOI: 10.12659/AJCR.936370
Am J Case Rep 2022; 23:e936370
Abstract
BACKGROUND: 0ptviral pneumonia and bilateral emphysematous pyelonephritis create a rapid acute respiratory distress syndrome.
CASE REPORT: A 59-year-old diabetic man with altered awareness was admitted as an emergency due to fever, shivering, and pain in the lap. Based on the accurate diagnosis, we concluded that the patient had bilateral emphysematous pyelonephritis, as well as inflammatory changes in the lung parenchyma caused by coronavirus infection (SARS-CoV-2). Active therapy – nephrectomy – was ruled out due to the late detection of the gas collection in the kidneys, as well as the general condition caused by respiratory symptoms. With symptomatic, supportive, and antimicrobial therapy, such as percutaneous renal drainage, renal abnormalities improved. Unfortunately, the virus-induced parenchymal inflammation progressed and proved fatal. The inflammatory process in the urothelial cell is most likely where the linkage and potentiation of COVID-19 infection and emphysematous pyelonephritis begins. Local inflammation that obstructs the movement of the generated gas is one of the hypothesized processes of emphysematous pyelonephritis. The renal and urothelial tubular cells contain the angiotensin-converting enzyme II (ACE2) receptor, which is used by the SARS-CoV-2 virus to enter human cells and may be a risk factor for simultaneous and direct viral injury to urinary tract cells. Sepsis was most likely caused by viral pneumonia, based on the resolution of changes in the kidneys.
CONCLUSIONS: The combination of EPN and COVID-19 is difficult to treat. Despite multidisciplinary treatment, it has been linked to a worse prognosis and fatal outcome.
Keywords: case reports, Pyelonephritis, Diabetes Mellitus, COVID-19, Diabetes Complications, emphysema, Humans, Male, Middle Aged, SARS-CoV-2, Sepsis, Treatment Outcome
Background
Emphysematous pyelonephritis (EPN) requires immediate, aggressive, general surgical treatment. Gas buildup in the kidney and perirenal region characterizes this necrotic parenchymal kidney infection [1].
EPN was first reported in the ninth century, and the term also describes the core pathogenic process [2]. Women, diabetics, and individuals with urinary tract blockage, as well as the immunocompromised, are at risk. Diabetes patients have a 6-fold increased risk [3], which can be explained in part by the presence of glucose in the tissues, alterations in tissue perfusion, and an insufficient immunological response [4].
Hyperglycemia, a proclivity for necrosis of urinary tract cells due to stress or infection, and a weakened immune system due to chronic kidney disease are all thought to be factors that promote bilateral emphysematous pyelonephritis (BEPN) in diabetics. One explanation of gas formation mechanisms in emphysematous infections involves the production of carbon dioxide (CO2) by enzyme-producing microorganisms, which further convert acids to CO2 when the pH reaches 6 or lower, and fermentation conditions of high glucose concentration in urine and tissues, which actually lowers pH in tissues due to acid accumulation. It should be noted, however, that urinary lactose or tissue proteins can also act as substrates for gas formation. Rapid catabolism, which increases gas production, is part of the pathogenesis of gas bubble formation. Gas accumulation raises local pressure and can cause infarction of neighboring tissues, which can serve as a good culture medium for gas-producing pathogens, increasing the gas transport barrier and creating a vicious circle [5,6]. As a result, patients with urinary tract structural abnormalities and urolithiasis are more likely to develop this type of infection [6].
This condition is only mentioned in the context of adults.
Simultaneous inflammatory processes in both kidneys are uncommon (10% of all EPNs), but it is evident that bilateral gas inflammation raises the risk of consequences in terms of acute renal function impairment and septic state, which causes and consequently increases risk of mortality. According to statistics, up to 33% of all people are overweight [8,9].
Early diagnosis and initiation of effective and optimal medical treatment, as well as an adequately scheduled surgical intervention, leads to a better prognosis and may potentially prevent progression, even leading to cure of the patient with this type of kidney infection.
Many people with urological disorders, both malignant and benign in nature, are now infected with SARS-CoV-2. Because of the nature of this pandemic disease and the medical system’s load of caring for a huge number of COVID-19 patients, we have seen patients who are aware of the basic urological condition and seek medical care in the later stages of the disease. Treatments must be modified and adapted to the current situation.
Case Report
In this paper, we present a patient with bilateral EPN and SARSCoV-2 pneumonia. He was transferred from another hospital where he had been receiving care for 3 days before being admitted to our hospital.
The anamnestic data acquired were insufficient, given his severe general state, changed mental status, and requirement for aggressive oxygen replacement therapy. He had a tooth surgically removed 5 days before admittance to the hospital, according to previous documents. He had been diabetic for many years, and his blood sugar was kept under control with oral hypoglycemics. The patient was febrile, adynamic, anxious, and confused during his previous hospitalization. Increased white blood cell counts, high CRP levels, hyperglycemia, and nitrogenous compounds in the blood were discovered during a laboratory examination.
Rehydration, supportive and symptomatic medication, and empirical antibiotic therapy were all administered. During the 3-day hospitalization at the regional health center, the patient received Longacef/ceftriaxone at a dose of 2 g/24 h in combination with marocen/ciprofloxacin/500 mg/12 h. Antibiotic therapy was changed immediately after admission to our hospital, taking into account the risk of potential dysglycemia and neuropathy in diabetic patients, as well as subsequent complications.
Due to a positive PCR test for SARS-CoV-2 infection, the patient was admitted to our emergency department with a high fever (40°C), hypotension (88/57 mmHg), tachycardia (pulse 130–140 beats per minute), normal sinus rhythm, altered state of consciousness (somnolent and confused), oligoanuria (diuresis of approximately 200 ml of concentrated urine), dyspnea, tachypnea, and peripheral saturation less than 70% with the use of non-invasive ventilation and oxygen therapy.
A neurologist was called because of the changed state of consciousness, and he recommended a CT scan of the endocranium. There were no pathomorphological alterations, active ischemia lesions, evidence of bleeding, or expanding processes found during this examination.
Lumbar discomfort was discovered during an abdominal examination. Leukocytosis, anemia, thrombocytopenia, metabolic acidosis, dyselectrolytemia, hyperglycemia, and acute renal failure with the uremic syndrome were discovered in the blood tests (Table 1). Before intubation, the gases were: pH 7.5; pCO2 28 mmHg; pO2 60 mmHg; Glyc 19.1mmol/L; K4.8 mmol/l; Lac 4 mmol/L; sO2 82%. Respiratory rate was 35 breaths per minute (tachydyspnoeic, with poor respiratory mechanics). Due to peripheral saturation (70%), a respiratory rate of 35/min, a poor state of consciousness, and respiratory rhythm disorders, the patient was placed on the most aggressive form of non-invasive ventilation (NIV) upon admission.
An ultrasound examination of the abdomen and pelvis revealed enlarged kidneys with edematous parenchyma and a large number of hyperechoic areas in the parenchyma, indicating the presence of intraparenchymal gas.
An urgent computed tomography scan of the chest, abdomen, and pelvis was conducted after further evaluation. The CT scan of the lungs revealed bilateral basal zone lung parenchyma consolidation, compressive atelectasis, and bilateral pleural effusions with a diameter of 31 mm and a density of clear liquid (Figure 1).
Abdominal CT revealed bilaterally enlarged kidneys with vo-luminous, inhomogeneous parenchyma, some signs of necrosis with pronounced vascular structures, larger irregular gas particles in the parenchyma next to the perirenal capsule, and extrarenal extension subfascial, more pronounced on the left kidney (Figures 2, 3). It does not emit a contrast agent. Acute renal failure symptoms can also be seen.
Because the patient’s general condition was extremely poor due to poor hemodynamic status secondary to associated sepsis, it was decided to postpone active treatment in consultation with anesthesiologists and internists. We began with intensive supportive therapy and resuscitation techniques. It was decided to intubate and link to mechanical ventilation because the patient was in a state of acute sepsis and multiorgan failure. Active treatment in septic circumstances and hemodynamic instability was not a current treatment choice after consultation with anesthesiologists and internists.
He was medicated, hemodynamically unstable, and on vasopressor support all of the time. Treatment included fluid resuscitation, electrolyte management, and ionotropic support, as well as empirical triple broad-spectrum antibiotic therapy (carbapenems with aminoglycosides and metronidazole, in doses tailored to renal insufficiency). An insulin infusion was used to help him manage his diabetes. Upon admission, blood and urine cultures were obtained for bacteriological investigation.
A 2-volume central venous catheter for hemodialysis was inserted due to the bilateral presentation, oligoanuria, and azotemia. The patient was admitted to hemodialysis by the nephrologist. Cultures of blood and urine were also collected. Hemodialysis was used to treat acute renal failure and hyper-kalemia, with laboratory values being monitored daily. During his stay in the hospital, he had 8 hemodialysis treatments.
The day after hospitalization, a percutaneous kidney puncture was conducted. After 3 days, the patient’s infectious status and renal function improved, as evidenced by an increase in diuresis (about 35 ml per hour), afebrile state, improved laboratory test results (Table 2), and hemodynamic stability.
The presence of gas implies that there is an active infection and that antibiotic medication is ineffective. Daily repeated control echotomography of the abdomen in our patient revealed improvement in the local findings, as well as regression of the inflammatory process and gas inclusions.
Based on the results of bacteriological parameters (urine and blood culture results showed the presence of
Unfortunately, 6 days after admission, his overall state and laboratory test results deteriorated (Table 3), along with recurring fever, cardiac instability, and poor respiratory function.
Despite the disappearance of the local finding in the kidneys, daily bedside radiographic images of the lungs showed severe inflammatory changes bilaterally involving a large area of the lung parenchyma, indicating progression of bilateral pneumonia compared to previous findings, with no signs of pneumothorax or pneumomediastinum (Figures 4, 5).
As a result of refractory hypoxia, the disease’s clinical course was marked by deterioration of respiratory function and cardiorespiratory arrest. Unfortunately, the resuscitation efforts were ineffective, and the patient died.
Discussion
A potentially fatal, acute, progressive, necrotizing EPN, which is more frequently recognized now thanks to the use of computed tomography in diagnosis, is typically discovered after finding gas (carbon dioxide) in the kidney, which is attributable to bacterial activity (fermentation). The majority of patients are women (4: 1), diabetics, and those with metabolic syndrome. Pathogenesis is a great model for immune response and tissue perfusion capacity [10–12].
Two EPN classifications are currently available in the literature based on CT findings. According to Huang and colleagues’ classification, which proposed 4 classes of EPN, the finding in our patient belonged to Class 4. According to the classification of Wan et al, the finding in our patient were Type II EPN: the presence of renal or perirenal fluid with a bubbly gas pattern, or the presence of gas in the collecting system [13,14].
In diabetics, timely identification and prompt treatment of urinary tract infections are important aspects of disease management. Thrombocytopenia, hypoalbuminemia, acute renal failure, altered mental status, polymicrobial infection, and, of course, shock can all be assessed using radiological categorization to determine the severity and dynamics of the disease [3,15].
The treatment protocol for these patients shifts from a conservative approach using antibiotic therapy with renal drainage (percutaneously or stent), which is predicted to lower antibiotic concentrations in the tissue by reducing gas while still improving tissue perfusion, to nephrectomy. For nephrectomy, powerful antibiotic therapy is becoming a more viable alternative [16,17].
For these individuals, bilateral nephrectomy is unquestionably a life-saving procedure. With medical therapy alone, it is not possible to have excellent control of the disease’s fulminant course. On the other hand, renal drainage and conservative therapy are directly associated with survival rates, whereas emergency nephrectomy remains the final and most difficult option in situations when the septic state must be treated first [15,18–20].
So far, the most prevalent cause of EPN has been identified as
Our case study features an obese middle-aged patient with diabetes who, as a first step in the progression of the condition, had dental intervention in the form of a simple, conventional tooth extraction. The wound in the mouth, we believe, was the beginning the body’s inflammatory reaction cascade. Clinicains in the regional center of the small town in the early days of the pandemic misunderstood his condition as a neurological disease. He tested positive for SARS-CoV-19 after developing a fever, and was subsequently moved to our hospital, which was in the COVID-19 care system at the time. After evaluation by an internist, neurologist, anesthesiologist, and radiologist/diagnostician in our patients’ admission service, it was discovered that bilateral emphysematous pyelonephritis had developed. The occurrence of 2 major inflammatory disorders was coincidental, but it made urothelial cells more vulnerable to infection with SARSCoV-2, complicating the patient’s overall condition due to altered state of consciousness, and no kidney infection was recognized.
Infection spreads through the bloodstream. Septic shock with oliguria increases the chance of death by 54% [24]. Despite these challenges, our medical team understood that early diagnosis, comprehensive treatment, and proper and rigorous therapy play a critical role in the course and outcome of this disease. Concomitant COVID-19 pneumonia was undoubtedly the reason why nephrectomy was not performed, which could have saved the patient’s life.
Pulmonary and thrombotic problems account for the increased rate of postoperative mortality and complications in SARS-CoV-2-positive patients who had to be operated on due to diverse diseases. There is currently a trend toward a cautious approach, non-operative treatment, or delaying surgical treatment. Of course, surgical intervention should only be considered for patients who will clearly benefit more from it in comparison to the danger of postoperative problems. Perhaps the underlying danger of exposure to healthcare personnel during the operative and particularly in the perioperative period should be considered to some extent when choosing surgical therapy in a COVID-19 patient. In the current COVID-19 pandemic, it may be critical to identify patients likely to have undeniable benefits from surgical treatment [25].
Conclusions
For both EPN and COVID-19, the course and prognosis are unknown and difficult to predict. As a result, each of these infections is quite dangerous on its own, and the combination of them is a major life-threatening condition.
A CT scan indicated bilateral emphysematous pyelonephritis and bilateral interstitial pneumonia in our patient. This case report shows that late diagnosis of EPN, especially when other morbidities are present, can result in rapid progression and development of septic shock, sudden acute respiratory distress syndrome, or multiple organ dysfunction syndromes. The combination of bilateral EPN with COVID-19 is a more severe illness, with a worse prognosis and potentially deadly results.
Figures
References:
1.. Michaeli J, Mogle P, Perlberg S, Emphysematous pyelonephritis: J Urol, 1984; 131(2); 203-8
2.. Sokhal AK, Kumar M, Purkait B, Emphysematous pyelonephritis: Changing trend of clinical spectrum, pathogenesis, management and outcome: Turk J Urol, 2017; 43(2); 202-9
3.. Huang JJ, Tseng CC, Emphysematous pyelonephritis: Clinicoradiological classification, management, prognosis, and pathogenesis: Arch Intern Med, 2000; 160(6); 797-805
4.. Shokeir AA, El-Azab M, Mohsen T, El-Diasty T, Emphysematous pyelonephritis: A 15-year experience with 20 cases: Urology, 1997; 49(3); 343-46
5.. Grupper M, Kravtsov A, Potasman I, Emphysematous cystitis: Illustrative case report and review of the literature: Medicine (Baltimore), 2007; 86(1); 47-53
6.. Pontin AR, Barnes RD, Current management of emphysematous pyelonephritis: Nat Rev Urol, 2009; 6(5); 272-79
7.. Misgar RA, Mubarik I, Wani AI, Emphysematous pyelonephritis: A 10-year experience with 26 cases: Indian J Endocrinol Metab, 2016; 20(4); 475-80
8.. Campbell I, Meredith F, Wein AJ, Kavoussi lR: Campbell-Walsh urology, 2007; 271-73, Philadelphia, W.B. Saunders
9.. Khaira A, Gupta A, Rana DS, Retrospective analysis of clinical profile prognostic factors and outcomes of 19 patients of emphysematous pyelonephritis: Int Urol Nephrol, 2009; 41(4); 959-66
10.. El-Nahas AR, Shokeir AA, Eziyi AK, Kidney preservation protocol for management of emphysematous pyelonephritis: Treatment modalities and follow-up: Arab J Urol, 2011; 9(3); 185-89
11.. Chen MT, Huang CN, Chou YH, Percutaneous drainage in the treatment of emphysematous pyelonephritis: 10-year experience: J Urol, 1997; 157(5); 1569-73
12.. Kuzgunbay B, Turunc T, Tokmak N, Tailored treatment approach for emphysematous pyelonephritis: Urol Int, 2011; 86(4); 444-47
13.. Huang JJ, Tseng CC, Emphysematous pyelonephritis: Clinicoradiological classification, management, prognosis, and pathogenesis: Arch Intern Med, 2000; 160(6); 797-805
14.. Wan YL, Lee TY, Bullard MJ, Tsai CC, Acute gas-producing bacterial renal infection: Correlation between imaging findings and clinical outcome: Radiology, 1996; 198(2); 433-38
15.. Tahir H, Thomas G, Sheerin N, Successful medical treatment of acute bilateral emphysematous pyelonephritis: Am J Kidney Dis, 2000; 36(6); 1267-70
16.. Chávez-Valencia V, Orizaga-de-La-Cruz C, Aguilar-Bixano O, Lagunas-Rangel FA, Coexistence of emphysematous cystitis and bilateral emphysematous pyelonephritis: A case report and review of the literature: CEN Case Rep, 2020; 9(4); 313-17
17.. Boakes E, Batura D, Deriving a management algorithm for emphysematous pyelonephritis: Can we rely on minimally invasive strategies or should we be opting for earlier nephrectomy?: Int Urol Nephrol, 2017; 49(12); 2127-36
18.. Karasavidou L, Nikolaou S, Archontakis S, Nonsurgical treatment of bilateral emphysematous pyelonephritis in a diabetic patient: J Nephrol, 2006; 19(5); 664-67
19.. Dutta D, Shivaprasad KS, Kumar M, Conservative management of severe bilateral emphysematous pyelonephritis: Case series and review of literature: Indian J Endocrinol Metab, 2013; 17(Suppl. 1); S329-32
20.. Aboumarzouk OM, Hughes O, Narahari K, Emphysematous pyelonephritis: Time for a management plan with an evidence-based approach: Arab J Urol, 2014; 12(2); 106-15
21.. Boyanova L, Marteva-Proevska Y, Markovska R, Urinary tract infections: Should we think about the anaerobic cocci?: Anaerobe, 2022 [Online ahead of print]
22.. Krol BC, Hemal AK, Fenu EM: CEN Case Rep, 2021; 10(1); 111-14
23.. Djafari AA, Hojjati SA, Rahnama H, First report of concurrent mixed germs induced destructive emphysematous pyelonephritis and emphysematous endophthalmitis in the patient with COVID-19: Urol Case Rep, 2022; 40; 101908
24.. Ubee SS, McGlynn L, Fordham M, Emphysematous pyelonephritis: BJU Int, 2011; 107(9); 1474
25.. Hegde AV, Kaul NK, Parab S, Hung up with a Huang class 4: Our experience with bilateral emphysematous pyelonephritis in a COVID 19 patient: Am J Clin Exp Urol, 2021; 9(5); 397-402
Figures
Tables
 Table 1.. Laboratory analyses at hospital admission.
Table 1.. Laboratory analyses at hospital admission. Table 2.. Laboratory analyses 4 days after admission to the hospital.
Table 2.. Laboratory analyses 4 days after admission to the hospital.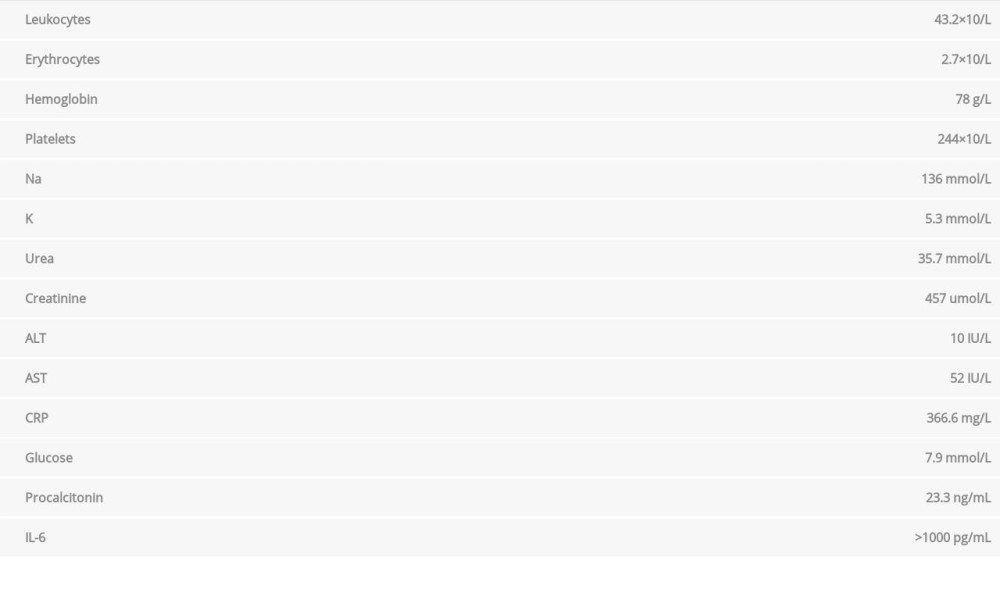 Table 3.. Laboratory analyses on the ninth day after hospital admission.
Table 3.. Laboratory analyses on the ninth day after hospital admission. Table 1.. Laboratory analyses at hospital admission.
Table 1.. Laboratory analyses at hospital admission. Table 2.. Laboratory analyses 4 days after admission to the hospital.
Table 2.. Laboratory analyses 4 days after admission to the hospital. Table 3.. Laboratory analyses on the ninth day after hospital admission.
Table 3.. Laboratory analyses on the ninth day after hospital admission. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








