21 July 2022: Articles 
A 77-Year-Old Man with Heparin-Induced Aldosterone Suppression Causing Hyperkalemia
Unusual or unexpected effect of treatment, Adverse events of drug therapy
Jonathan Kovacs1EF*, Samer Talib1E, Abdallah Khashan1E, Bhaveshkumar Garsondiya1E, Michael P. CarsonDOI: 10.12659/AJCR.937017
Am J Case Rep 2022; 23:e937017
Abstract
BACKGROUND: Anticoagulation with heparin infrequently causes elevated serum potassium via a reduction in the number and affinity of adrenal angiotensin II receptors, causing reversible aldosterone suppression, thereby leading to enhanced sodium excretion and hyperkalemia.
CASE REPORT: A 77 year-old man presented with productive cough and shortness of breath and was subsequently found to have non-ST-elevation myocardial infarction and concomitant symptomatic COVID-19 infection, for which he was started on a high-dose unfractionated heparin infusion. A gradual increase in serum potassium followed, with a subsequent return to a normal potassium level after stopping treatment with heparin. An evaluation for hemolysis was unrevealing, and the patient was not on any other medications known to cause hyperkalemia. On day 6, heparin was restarted owing to a high suspicion of pulmonary embolism. There was a subsequent increase in serum potassium level, which was followed by a return to baseline after discontinuation of heparin, thereby confirming the suspected diagnosis.
CONCLUSIONS: Acute increases in serum potassium levels in hospitalized patients can result in weakness, paralysis, conduction abnormalities, and cardiac arrhythmias that, if left untreated, can result in serious morbidity and potentially death in a short period of time. As this clinical entity is infrequently encountered in clinical practice, it can easily be overlooked by clinicians. The prompt exclusion of alternative causes of acutely elevated serum potassium levels and the identification of heparin administration as an easily reversible trigger is imperative and can potentially be life-saving.
Keywords: acute coronary syndrome, Aldosterone, Heparin, Hyperkalemia, Aged, Anticoagulants, COVID-19, Humans, Male, Potassium
Background
Heparin-induced hyperkalemia is a well-established but infrequently observed event and a diagnosis of exclusion. First recognized in the clinical literature as early as 1964, new cases continue to challenge clinicians to this day [1,2]. The insidious elevation of serum potassium observed in this clinical entity is thought to be the consequence of the inhibitory effects of heparin at the level of the zona glomerulosa, possibly via a reduction in the number and affinity of adrenal angiotensin II receptors, causing reversible aldosterone suppression, thereby leading to enhanced sodium excretion and hyperkalemia. Evidence suggests a slightly lower risk with low-molecular-weight heparin [3].
Case Report
A 77-year-old man with a past medical history significant for type 2 diabetes, benign prostatic enlargement, chronic renal disease stage 3B, and nephrectomy for renal cancer presented with a productive cough and shortness of breath, but no chest pain. Three days prior, he tested positive for SARS-CoV-2. He was a nonsmoker and denied use of alcohol or any illicit drugs.
On initial presentation, his vital signs were as follows: temperature of 36.6°C, blood pressure of 128/69 mmHg, pulse rate of 92 beats per min, respiratory rate of 22 breaths per min, and a peripheral oxygen saturation of 92% on non-rebreather mask. He was determined not to be a candidate for treatment with remdesevir for SARS-CoV-2 infection owing to acute kidney injury on presentation, but received tocilizumab on hospital day 1. On physical examination, he was awake, alert, and oriented, ill in appearance, and in visible respiratory distress, exhibiting difficulty speaking in complete sentences. On lung examination, diffuse rhonchi and rales were auscultated bilaterally. No murmurs or added heart sounds were appreciated, and +1 pitting edema was noted in the bilateral lower extremities.
Pertinent studies from the time of admission included a serum troponin level of 1.97 ng/mL (reference range, <0.3 ng/mL) and an electrocardiogram showing no acute ischemic abnormalities. Creatinine and blood urea nitrogen levels were 2.4 mg/dL (reference range, 0.7–1.2 mg/dL) and 67 mg/dL (reference range, 6–20 mg/dL), respectively, and estimated glomerular filtration rate of 28 mL/min/1.73 m2 (reference range, >60 mL/min/1.73 m2), although no prior values were available. The serum potassium level was 5.1 mmol/L (reference range, 3.6–5.1 mmol/L).
Given the patient’s presentation of acute respiratory distress (an anginal equivalent) with elevation of serum troponin and in the context of a possible underlying hypercoagulable state due to concomitant COVID-19 infection, the decision was made to start the patient on a high-dose unfractionated heparin drip. As the cause of troponin elevation was thought to be ischemia due to increased demand in the setting of acute kidney injury/chronic kidney disease, the patient was never taken for cardiac catheterization. No computed tomography scan or test requiring the administration of intravenous contrast was performed over the course of hospital admission. On hospital day 4, the serum potassium level rose to 5.6 mmol/L (reference range, 3.6–5.1 mmol/L). An evaluation for hemolysis was negative (LDH and haptoglobin was not low). The patient had not received any beta blockers, angiotensin converting enzyme (ACE) inhibitors/angiotensin receptor blockers, calcineurin inhibitors, or any other medication known to cause elevation of serum potassium; therefore, heparin was stopped and sodium polystyrene (kayexalate), insulin, and dextrose were administered after the potassium reached a high of 6.2 mmol/L on hospital day 5, resulting in only a slight drop of potassium to 5.5 mmol/L on the following day (Table 1, Figure 1). Owing to a high clinical suspicion for pulmonary embolism on hospital day 6, supported by worsening tachycardia, respiratory distress, and a nonspecific elevation of D-dimer of 15.71 mg/ dL (reference range, <0.50), high-dose heparin was restarted; however, the serum potassium level promptly rose again on the same evening, reaching a level of 6.0 mmol/L. Computed tomography angiography was not obtained owing to the patient’s renal function, and in the absence of hemodynamic instability, a ventilation/perfusion lung scan was not obtained because the patient was already being treated with systemic anticoagulation, and findings would have not altered the choice of management. At this time, the diagnosis of heparin-induced aldosterone suppression was strongly suspected, heparin was again discontinued, and the potassium level quickly normalized to 4.8 mmol/L on the fifth evening of admission and remained within normal limits with the heparin withheld (Table 1, Figure 1).
Discussion
Hospitalized patients often require chemical venous thromboembolism prophylaxis. Unfractionated and low-molecular-weight heparins are preferred because of their favorable safety profile. The exact mechanism for heparin-induced hyperkalemia is not fully understood but appears to be related to a heparin-induced reduction in the number and affinity of angiotensin II receptors in the zona glomerulosa. Angiotensin II activates calcium influx into the zona glomerulosa [4,5], which is the key to aldosterone production; frequent and long-term interruption in this process can result in some degree of loss in cellular function and volume. This inhibition of aldosterone synthesis can occur within a few days after giving the medication, as observed in our patient, who began to show an increase in potassium level by the fourth day of admission. This phenomenon can be observed with a low dosage and with subcutaneous or intravenous routes, leading to increased excretion of sodium and increased retention of potassium. This effect is reversible after stopping heparin.
This process is generally compensated in healthy individuals but is more pronounced in older adults with diabetes and patients with renal insufficiency or failure, as was the case in our patient, with a diagnosis of chronic kidney disease stage 3B [6]. The risk increases with higher doses, prolonged dosages, and unfractionated heparin therapy, and in hospitalized patients on a prophylactic dose of heparin with ACE inhibitors or those who have a baseline potassium level >4.6 mmol/L between days 4 and 8 of hospital admission [7]. Therefore, potassium levels should be checked at least every 4 days for patients on heparin for 3 days or more, patients on a high dose of heparin, patients on ACE inhibitors, patients with diabetes, and patients with renal insufficiency [8]. In the present clinical scenario, the chronology, clinical exclusion of other causes, recurrence of hyperkalemia with heparin administration, and prompt return to a sustained, normal serum potassium level after cessation of heparin supported heparin as the cause of the hyperkalemia.
When hyponatremia and hyperkalemia due to hypoaldosteronism are accompanied by a state of metabolic acidosis and a normal anion gap, this condition has been referred to as type 4 renal tubular acidosis and can be stratified by etiology, based on those associated with reduced aldosterone production and those associated with increased aldosterone resistance. Etiologies related to reduced aldosterone production include those precipitated by a number of medications, including non-steroidal anti-inflammatory drugs, beta blockers, ACE inhibitors, angiotensin receptor blockers, calcineurin inhibitors, and heparins, while aldosterone resistance can be precipitated by potassium-sparing diuretics as well as by select antibiotics (namely, trimethoprim and pentamidine) [9]. Due to the absence of laboratory evidence of metabolic acidosis, the patient discussed herein was not thought to fulfill the diagnostic criteria for type 4 renal tubular acidosis.
The calculation of a transtubular potassium gradient may be a helpful tool to consider in select cases, as it has demonstrated utility in distinguishing between patients with suspected mineralocorticoid deficiency or resistance. A transtubular potassium gradient was not calculated for the present case, as neither urine osmolality nor serum osmolality were obtained over the course of hospital admission, which would have both been necessary to perform the calculation. Additionally, treatment with fludrocortisone was not considered owing to the rapid return of the potassium level to normal limits following the discontinuation of heparin [10].
Unfractionated and low-molecular-weight heparins are most frequently the anticoagulants of choice for non-ST elevation acute coronary syndromes owing to their demonstrated ability to reduce the incidence of thrombus-related ischemic events. When heparin must be discontinued due to complications of treatment, such as the development of heparin-induced thrombocytopenia, or suspected aldosterone suppression, as in our patient, many patients can require ongoing anticoagulation with the selection of an alternative agent. Fondaparinux has been found to offer a similar reduction in the risk of ischemic events and lower bleeding risk and can be considered as a safe alternative in this population [11].
Conclusions
Acute increases in serum potassium levels in hospitalized patients can result in weakness, paralysis, conduction abnormalities, and cardiac arrhythmias that, if left untreated, can result in serious morbidity and potentially death in a short period of time. The differential diagnosis for causes of hyperkalemia in patients like the one discussed herein remains broad. As this clinical entity is infrequently encountered in clinical practice, it can be easily overlooked by clinicians. As such, the prompt exclusion of alternative causes of acutely elevated serum potassium levels can be facilitated by taking a detailed history to rule out the use of other medications known to elevate serum potassium, such as non-steroidal anti-inflammatories, beta blockers, ACE inhibitors/angiotensin receptor blockers, and calcineurin inhibitors. The identification of heparin administration as an easily reversible trigger is imperative and can potentially be life-saving. In the case discussed, the diagnosis of heparin-induced aldosterone suppression was reached by exclusion; however, obtaining standard assays to evaluate serum aldosterone, cortisol, and renin levels may aid in circumstances of diagnostic uncertainty and help identify similarly presenting conditions, such as primary adrenal insufficiency.
References:
1.. Knysak M, Smyk Ł, Stompór T, [Heparin-induced hyperkalaemia – a case report]: Pol Merkur Lekarski, 2018; 45(268); 158-60 [in Polish]
2.. Wilson ID, Goetz FC, Selective hypoaldosteronism after prolonged heparin administration. A case report, with postmortem findings: Am J Med, 1964; 36; 635-40
3.. Bengalorkar GM, Sarala N, Venkatrathnamma PN, Kumar TN, Effect of heparin and low-molecular weight heparin on serum potassium and sodium levels: J Pharmacol Pharmacother, 2011; 2(4); 266-69
4.. Oster JR, Singer I, Fishman LM, Heparin-induced aldosterone suppression and hyperkalemia: Am J Med, 1995; 98(6); 575-86
5.. Ezzatzadegan Jahromi S, Mahmoodi MS, Effect of switching unfractionated heparin to low-molecular-weight heparin on serum potassium in hemodialysis patients: Iran J Kidney Dis, 2014; 8(6); 475-80
6.. Hattangady NG, Olala LO, Bollag WB, Rainey WE, Acute and chronic regulation of aldosterone production: Mol Cell Endocrinol, 2012; 350(2); 151-62
7.. Liu AA, Bui T, Nguyen HV, O’Rourke F, Subcutaneous unfractionated heparin-induced hyperkalaemia in an elderly patient: Australas J Ageing, 2009; 28(2); 97
8.. Torres OH, Hernandez N, Francia E, Effect of prophylactic treatment with low-molecular-weight heparin bemiparin sodium on serum potassium levels: A prospective observational study: Drugs Aging, 2010; 27(5); 399-406
9.. Alappan R, Perazella MA, Buller GK, Hyperkalemia in hospitalized patients treated with trimethoprim-sulfamethoxazole: Ann Intern Med, 1996; 124(3); 316-20
10.. Choi MJ, Ziyadeh FN, The utility of the transtubular potassium gradient in the evaluation of hyperkalemia: J Am Soc Nephrol, 2008; 19(3); 424-26
11.. Yusuf S, Mehta SR, Comparison of fondaparinux and enoxaparin in acute coronary syndromes: N Engl J Med, 2006; 354(14); 1464-76
Tables
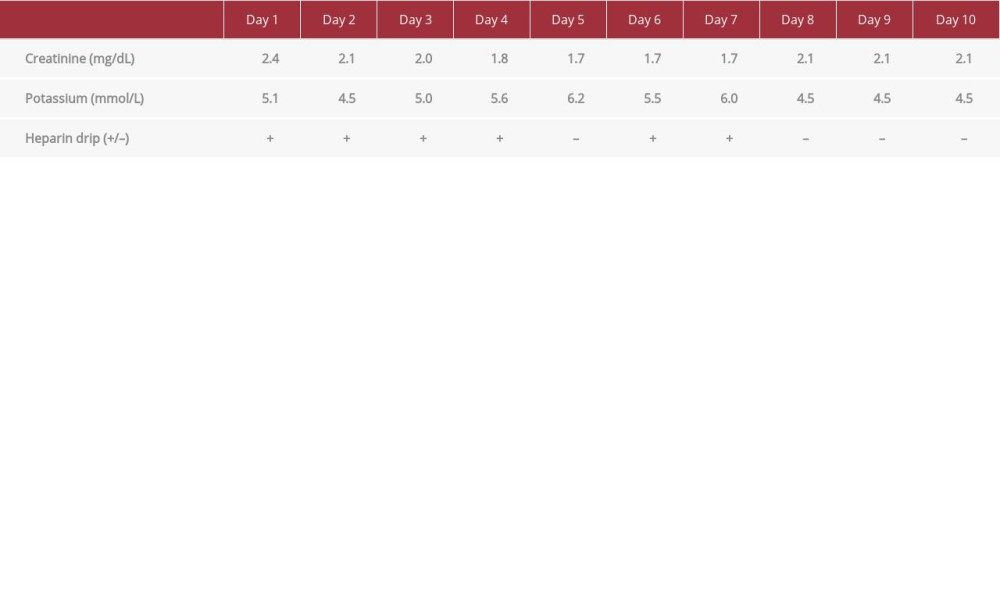 Table 1.. Serum creatinine and potassium level trend starting from day 1 of admission through day 10. Heparin was started in the evening of day 1, held on day 5 at 02: 55 AM, restarted on day 6, and held in the evening of day 7.
Table 1.. Serum creatinine and potassium level trend starting from day 1 of admission through day 10. Heparin was started in the evening of day 1, held on day 5 at 02: 55 AM, restarted on day 6, and held in the evening of day 7. Table 1.. Serum creatinine and potassium level trend starting from day 1 of admission through day 10. Heparin was started in the evening of day 1, held on day 5 at 02: 55 AM, restarted on day 6, and held in the evening of day 7.
Table 1.. Serum creatinine and potassium level trend starting from day 1 of admission through day 10. Heparin was started in the evening of day 1, held on day 5 at 02: 55 AM, restarted on day 6, and held in the evening of day 7. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








