02 March 2023: Articles 
Intra-Tendinous Ganglion Cyst of the Peroneus Tertius: A Case Report and Literature Review
Challenging differential diagnosis, Rare disease
Raymond C. Walls1ABCDEF, Hugo A. UbillusDOI: 10.12659/AJCR.938498
Am J Case Rep 2023; 24:e938498
Abstract
BACKGROUND: This article presents a rare case of an intra-tendinous ganglion cyst of the peroneus tertius. Ganglion cysts are benign lesions frequently seen in hand pathologies, but they are rarely seen in the foot and ankle. This article discusses the present case and similar previously reported cases in the English literature.
CASE REPORT: We present a case of a 58-year-old man with a 3-year history of right foot pain caused by a mass located at the dorso-lateral aspect of the midfoot. Preoperative MRI demonstrated a ganglion cyst arising from the peroneus tertius tendon sheath. The lesion was successfully decompressed in the office; however, it recurred 7 months later. As it was symptomatic, we elected to proceed with surgical resection. During dissection, it became apparent that the cyst was arising from an intrasubstance tear of the peroneus tertius tendon, and a branch of the superficial peroneal nerve was noted to be adherent to the pseudo-capsule. Following excision of the lesion and its expansile pseudo-capsule, the tear was repaired with tubularization of the tendon and external neurolysis of the nerve was performed. At 6 months after surgery, there was no recurrence of the lesion, and the patient was pain free and had regained normal physical function.
CONCLUSIONS: Intra-tendinous ganglion cysts are rare, especially in the foot and ankle. This makes it challenging for an accurate preoperative diagnosis. When a tendon is arising from a tendon sheath, we recommend exploration of the underlying tendon for an associated tear.
Keywords: Foot, Ganglion Cysts, Tendon Injuries, Male, Humans, Middle Aged, Tendons, Leg, Lower Extremity, Hand
Background
Ganglion cysts are common benign lesions most commonly occurring in the hand and wrist [1]. While the exact etiology is unclear, it is believed they arise from myxoid degeneration of connective tissue forming gelatinous material within a cystic pseudo-capsule [2,3].
While the foot and ankle are considered the second most common location for ganglia, this region only accounts for 3–5% of all lesions [4,5]. An MRI study that evaluated lower-extremity ganglia noted a prevalence of 5.6% in the ankle and 0.4% in the foot [6]. Most of these lesions were occult, and none were reported as occurring within a tendon. Of those that were symptomatic, the most common location was the Lisfranc joint.
Intra-tendinous ganglion cysts are rare, both in the upper and lower extremities [7–10]. We present a case of an intra-tendinous ganglion cyst arising in the peroneus tertius tendon and review previous reports of similar lesions occurring in the foot and ankle.
Case Report
A 58-year-old man presented to our orthopedic outpatient department reporting a 3-year history of right foot pain secondary to a mass located at the dorso-lateral aspect of the midfoot. As it increased in size, the patient reported increasing difficulty and discomfort with shoe wear. He did not recall any specific traumatic injury preceding the onset of symptoms. Plain radiology demonstrated no osseus involvement (Figure 1). The patient documented his pain as 6/10 on the Visual Analogue Scale (VAS). Conservative treatment had been unsuccessful, including compression bandages, reducing physical activities, shoe wear modification, and over-the-counter anti-inflammatories.
Physical examination demonstrated a rubbery-firm, subcutaneous, mobile, lobulated, lesion that was 3 cm in diameter and non-tethered to the skin. It was located at the dorso-lateral aspect of the midfoot in the region of the base of the fourth metatarsal. Ankle and foot motion was normal, with intact per-fusion and sensation as well as normal power for all motions.
Aspiration was first attempted in the office using an 18-gauge needle, but only yielded a very small volume of gelatinous fluid. We converted to decompression as the patient declined formal excision at this stage. Under sterile technique, local anesthesia (1% lidocaine) was infiltrated to the skin overlying the lesion and a stab incision was made with an 11-blade scalpel. The lesion was fully decompressed and approximately 8cc of straw-colored gelatinous contents were obtained. The sample was sent for pathologic analysis, which reported the contents to be compatible with a mucin-filled synovial benign cyst. There was clinical improvement after decompression without immediate complications.
The patient presented again 7 months later with recurrence of the mass at the dorso-lateral midfoot. At this stage, it had increased in size, with a diameter of 4 cm. An MRI was performed, which demonstrated a T2 hyperintense, T1 hypointense soft-tissue mass measuring 3.7×3.0×1.7 cm overlying the extensor digitorum tendons. It was suspected to arise from the extensor digitorum longus tendon sheath (Figure 2). There was no presence of tenosynovitis on MRI. The patient was unable to wear enclosed shoe wear due to the increased size and discomfort. He now consented to formal resection of the lesion in the operating room.
Anesthesia was achieved using monitored sedation and a local nerve block. A 5-cm longitudinal incision over the cystic mass was performed (Figure 3), lateral to the intermediate dorsal cutaneous branch of the superficial peroneal nerve (SPN), which was identified with the fourth toe flexion sign [11]. This nerve was noted to be adherent to the pseudo-capsule, so careful neurolysis was performed and the nerve retracted medially.
During initial dissection, we did not identify a stalk arising from the underlying tendon sheath. Instead, the lesion appeared to have a broad base adherent to the underlying tendinous structures. We ultimately determined the lesion was arising from the tendon of the peroneus tertius. The cyst was decompressed to identify the pseudo-capsule and the origin of the lesion, which was from a longitudinal split tear within the peroneus tertius tendon. The pseudo-capsule was incised at the distal extent of the tear and carefully traced proximally to intact tendon structure. The lesion measured more than 4 cm in length once fully excised (Figure 4A, 4B). Additional dissection of 2 cm in each direction along the tendon was performed in search of satellite masses that may precipitate recurrence, with none identified. The peroneus tertius had a 5-cm partial thickness longitudinal split tear, which was repaired by tubularization using a running 3-0 Vicryl suture (Figure 5). The specimen was sent for pathology, which was confirmed to be a ganglion cyst with presence of fibrous connective tissue.
Postoperatively, a soft dressing was applied, and the patient was permitted to bear weight as tolerated in a short controlled ankle movement (CAM) boot. The wound healed uneventfully, and the patient was permitted to return to work in the boot after 2 weeks. The boot was discontinued at 6 weeks postoperatively. At the 3-month follow-up assessment, the patient was pain free and had minimal postoperative swelling. He was wearing normal shoes without difficulty and had returned to all prior activities.
Discussion
Ganglion cysts are mucin-filled synovial cysts most often identified in the wrist and are often associated with trauma, mucoid degeneration, or synovial herniation [12]. They usually occur in the upper extremities and infrequently in the feet and ankles [13]. Lecene first reported an intra-tendinous ganglion cyst within the common extensor tendon of the middle finger over the dorsum of the hand [14]. Since then, there have been sporadic case reports documenting intra-tendinous ganglion cysts, mostly occurring within the extensor tendons of the wrists and hands [15,16]. Lower-limb lesions that present as intra-tendinous cysts are very rare, with only a handful of cases reported to date arising in the peroneus tertius, peroneus longus below the knee, the extensor digitorum longus close to the ankle, and the quadriceps femoris tendons [13,17–19].
The clinical presentation of ganglion cysts arising from a joint and those arising from tendon sheaths or even intra-tendinous lesions are similar. Higher-level imaging, such as MRI and ultrasound, are often recommended [2]. This provides valuable diagnostic information about the location and anatomical relationship between the lesion and adjacent musculoskeletal structure [20]. They typically demonstrate fluid within the cyst and often determine the origin of the lesion, typically a joint or, less commonly, tendon sheath. In our case, we obtained a preoperative MRI where the lesion was felt to arise from the tendon sheath of the extensor digitorum longus. It did not clearly demonstrate that we were treating an intra-tendinous ganglion cyst arising from a tear of the peroneus tertius tendon and reflects the difficulty in getting an accurate diagnosis of these lesions preoperatively.
First-line treatment of ganglion cysts is conservative, involving compression (acute and gradual), warm compress, observation, and in recalcitrant cases, aspiration with possible cortisone injection. Oftentimes, the cyst will resolve on its own, with reportedly 58% resolving without any type of intervention [13]. The recurrence rate after aspiration is approximately 59% [21]. It is important to determine if the lesion is arising from a joint or tendon prior to performing an injection as there is a risk of precipitating rupture in the setting of a pathologic tendon. In addition, it is important to attempt to distinguish between a synovial cyst (SC) versus a ganglion cyst (GC), as in our case. Contrary to SCs, GCs lack a synovial cell lining and are constituted by a dense collagenous capsule surrounding a mucopolysaccharide-rich gelatinous fluid [22–25] at a higher concentration compared to SCs [22]. A distinction between a SC and a GC could also help target therapy by means of surgical excision, as there is a higher chance of recurrence when performing an aspiration, such as in our case.
Patients who have symptomatic lesions and who fail to respond to non-operative treatment may consider surgical intervention. Recurrence rates after open surgery are reported as up to 21% [21]. However, this is for lesions arising from wrist joints and data on lesions from foot and ankle tendon sheaths are scarce. In a study by Ahn et al, 53 cases of ganglion cysts in the foot and ankle treated by open resection were retrospectively analyzed and had a recurrence rate of only 5.7% (3 cases), all of which originated from the tendon sheath. In all 3 of these cases, satellite masses were located [26].
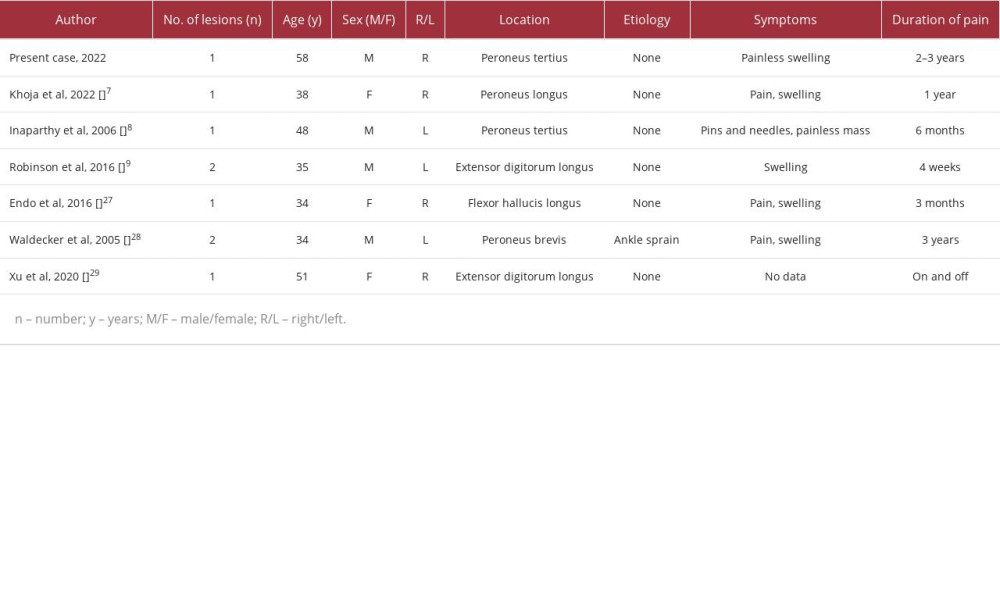
We are only aware of 6 previous case reports of intra-tendinous ganglions reported as arising in the foot and ankle, which we have summarized in Table 1. In all cases, the tendon was preserved, and no recurrence was reported. As in our case, they all occurred spontaneously, without a history of trauma or underlying arthritis/exostosis. No postoperative complications were documented. While 1 case did report preoperative neuropathy [7], the symptoms fully resolved after resection of the lesion. We found that the mean age from the 7 studies (including this study) was 42.6±9 years, which may suggest a relation between tendon degeneration or tears and the pathogenesis of intra-tendinous ganglion cysts.
Conclusions
Intra-tendinous ganglion cysts are rare, especially when arising in the foot and ankle. We are only aware of a handful of other case reports of these lesions. This can pose a challenge in determining an accurate definitive diagnosis. While aspiration may alleviate the size of the mass and the severity of the symptoms, the recurrence rate is so high that surgical intervention is often necessary. We recommend formal excision for intratendinous ganglion cysts as there may be associated tendon degeneration or tears that need to be addressed at the same.
Figures
References:
1.. Nahra ME, Bucchieri JS, Ganglion cysts and other tumor related conditions of the hand and wrist: Hand Clin, 2004; 20(3); 249-60
2.. Gregush RE, Habusta SF, Ganglion Cyst. 2022 Jul 18: StatPearls [Internet], 2022, Treasure Island (FL), StatPearls Publishing
3.. Gude W, Morelli V, Ganglion cysts of the wrist: Pathophysiology, clinical picture, and management: Curr Rev Musculoskelet Med, 2008; 1(3–4); 205-11
4.. Sharma UK, Dhungel K, Pokhrel D, Magnetic resonance imaging evaluation of musculoskeletal diseases of ankle and foot: Kathmandu Univ Med J (KUMJ), 2018; 16(61); 28-34
5.. Lee JW, Joo MW, Sung JK, Origin of satellite ganglion cysts with ef-fusion in the flexor hallucis longus tendon sheath around the hallux: Clin Orthop Surg, 2018; 10(1); 94-98
6.. Weishaupt D, Schweitzer ME, Morrison WB, MRI of the foot and ankle: Prevalence and distribution of occult and palpable ganglia: J Magn Reson Imaging, 2001; 14(4); 464-71
7.. Khoja YT, Altammami AF, Alattas MH, Peroneus longus intra-tendinous ganglion cyst: J Surg Case Rep, 2022; 2022(6); rjac279
8.. Inaparthy PK, Ravikumar KJ, Intratendinous ganglion of peroneus tertius – a case report: Foot Ankle Surg, 2006; 12(4); 221-22
9.. Robinson C, Kocialkowski C, Bhosale A, Pillai A, Intratendinous ganglion cyst of the extensor digitorum longus tendon: A case report: Foot (Edinb), 2016; 27; 46-49
10.. Tomori Y, Motoda N, Nanno M, Majima T, Intratendinous ganglion of the extensor pollicis longus: Case report and literature review: J Nippon Med Sch, 2021; 88(5); 500-5
11.. Stephens MM, Kelly PM, Fourth toe flexion sign: A new clinical sign for identification of the superficial peroneal nerve [Erratum in: Foot Ankle Int. 2000;21(12): 995]: Foot Ankle Int, 2000; 21(10); 860-63
12.. Meyerson J, Pan YL, Spaeth M, Pearson G, Pediatric ganglion cysts: A retrospective review: Hand (N Y), 2019; 14(4); 445-48
13.. Suen M, Fung B, Lung CP, Treatment of ganglion cysts: ISRN Orthop, 2013; 2013; 940615
14.. Lecene MP, Three cases of pseudocystic gelatinous degeneration of juxta-articular connective tissue and tendon tissue: Bull Mem Soc Nat Chir, 1927; 53; 2
15.. Ikeda K, Tomita K, Matsumoto H, Intratendinous ganglion in the extensor tendon of a finger: A case report: J Orthop Surg (Hong Kong), 2001; 9(2); 63-65
16.. Balazs GC, Dworak TC, Tropf J, Incidence and risk factors for volar wrist ganglia in the U.S. military and civilian populations: J Hand Surg Am, 2016; 41(11); 1064-70
17.. Maheshwari P, Maheshwari P, Bapna P, Intratendinous ganglion cyst of the semitendinosus tendon: First reported case and literature review: J Orthop Case Rep, 2016; 6(5); 85-88
18.. Costa CR, Morrison WB, Carrino JA, Raiken SM, MRI of an intratendinous ganglion cyst of the peroneus brevis tendon: Am J Roentgenol, 2003; 181(3); 890-91
19.. Siebert CH, Kaufmann A, Niedhart C, Heller KD, The quadriceps tendon cyst: An uncommon cause of chronic anterior knee pain: Knee Surg Sports Traumatol Arthrosc, 1999; 7(6); 349-51
20.. McCarthy CL, McNally EG, The MRI appearance of cystic lesions around the knee: Skeletal Radiol, 2004; 33(4); 187-209
21.. Head L, Gencarelli JR, Allen M, Boyd KU, Wrist ganglion treatment: Systematic review and meta-analysis: J Hand Surg Am, 2015; 40(3); 546-53.e8
22.. Giard MC, Pineda C, Ganglion cyst versus synovial cyst? Ultrasound characteristics through a review of the literature: Rheumatol Int, 2015; 35(4); 597-605
23.. Beaman FD, Peterson JJ, MR imaging of cysts, ganglia, and bursae about the knee: Radiol Clin North Am, 2007; 45(6); 969-82 , vi
24.. Bermejo A, De Bustamante TD, Martinez A, MR imaging in the evaluation of cystic-appearing soft-tissue masses of the extremities: Radiographics, 2013; 33(3); 833-55
25.. Apostolaki E, Davies AM, Evans N, Cassar-Pullicino VN, MR imaging of lumbar facet joint synovial cysts: Eur Radiol, 2000; 10(4); 615-23
26.. Ahn JH, Choy WS, Kim HY, Operative treatment for ganglion cysts of the foot and ankle: J Foot Ankle Surg, 2010; 49(5); 442-45
27.. Endo J, Yamaguchi S, Sasho T, Tendoscopic excision of an intratendinous ganglion in the flexor hallucis longus tendon: A case report: J Foot Ankle Surg, 2016; 55(2); 345-47
28.. Waldecker U, Unusual location of a posttraumatic ganglion and rupture of the peroneus brevis tendon: a case report: J Foot Ankle Surg, 2005; 44(2); 163-65
29.. Xu H, Gazes MI, Jariwala T, Gambardella PT, Intratendinous ganglion cyst of the extensor digitorum longus: A case report: J Am Podiatr Med Assoc, 2020; 110(1) Article9
Figures
In Press
12 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943244
13 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943275
13 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943411
13 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942864
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250