29 March 2023: Articles 
Management of Labor in Pregnancy Complicated with Previous Tuberculosis with Giant Lung Bullae and Intrauterine Growth Restriction: A Case Report
Challenging differential diagnosis, Unusual setting of medical care, Rare coexistence of disease or pathology
Muhammad Alamsyah Aziz1ACEF, Alfonsus Zeus Suryawan1BDEF*DOI: 10.12659/AJCR.939006
Am J Case Rep 2023; 24:e939006
Abstract
BACKGROUND: Tuberculosis (TB) is the leading infectious cause of mortality in developing countries. In pregnancy, TB may cause complications including intrauterine growth restriction (IUGR) and vertical transmission of TB. Recurrent TB infection can cause permanent damage to lung tissue, and formation lung bullae can occur. Giant lung bullae may be harmless in normal conditions, but cause concern if the patient is pregnant.
CASE REPORT: A 22-year-old G1P0A0 woman at 9 months of pregnancy came to our institution due to labor pain. She also presented with active TB from 1 month before admission. Chest X-ray findings suggestive of tuberculosis and giant bullae were found. She was diagnosed with active 1st phase of labor with active TB and giant lung bullae. The Cardiothoracic Surgery Department was on standby during labor to take countermeasures if bullae rupture occurred. The 2nd stage of labor was shortened with vacuum extraction. After delivery, the patient was shifted to an isolation room and started on antitubercular drugs.
CONCLUSIONS: Tuberculosis in pregnancy leads to many adverse outcomes, both in maternal and fetal. Prolong TB infection also causes lung scaring, which leads to formation of bullae. Possible causes of rupture of bullae during pregnancy are Valsalva maneuver during labor, increased alveolar ventilation, and positive‑pressure ventilation during general anesthesia. Normal vaginal delivery would increase the need for Valsalva maneuver, and vacuum extraction is advised to shorten the 2nd stage of labor to minimize the need of Valsalva maneuver and avoid increased intrapulmonal pressure.
Keywords: latent tuberculosis, Pulmonary Bullae Causing Pneumothorax, Vacuum Extraction, Obstetrical, Pregnancy, Female, Humans, young adult, Adult, Fetal Growth Retardation, Blister, Tuberculosis, Antitubercular Agents
Background
Tuberculosis (TB) is one of the infectious diseases leading to mortality in developing countries. Indonesia is the second country after India with the most deaths due to TB [1]. Due to its chronic course, TB may interfere with pregnancy. In 2011, approximately 216 500 (CI 95% 192 000–247 000) people were diagnosed with active TB [2]. Chronic inflammation in a mother with TB may lead to several fetal complications, including intrauterine growth restriction (IUGR) and vertical transmission of TB. Furthermore, long-term administration of anti-TB drugs can also contribute to the development of adverse fetal outcomes, as the evidence of their safety in pregnancy remains controversial [3]. Recurrent TB infection can cause permanent damage to lung tissue, and formation of lung bullae can occur. Giant lung bullae are usually harmless in normal conditions but can cause concern if the patient is pregnant. Spontaneous rupture of bullae rarely occurs in woman and poses a significant danger to fetus and mother. The most common cause is apical bleb rupture in the absence of a known significant pulmonary disease or trauma [4]. There have been few reports of bullae in pregnancy and labor, which leads to controversies in method of delivery. We present a case of vacuum-accelerated labor in a woman with tuberculosis and giant lung bullae.
Case Report
A 22-year-old G1P0A0 woman at 9 months of pregnancy came to our institution due to labor pain. She also presented with active TB starting 1 month before admission. She had a history of confirmed pulmonary active TB in 2018 and completed a 6-month anti-TB regimen. During the present pregnancy, she was diagnosed with TB at 8 months of gestation. She was prescribed an intensive phase of anti-TB regimen consisting of Rifampicin 300 mg/day, Isoniazid 150 mg/day, Pyrazinamide 800 mg/day, and Ethambutol HCl 550 mg/day according to Indonesia guidelines. The patient had already been on an anti-TB regimen for 1 month upon arrival at our facility. On physical examination, her vital signs were within normal limits, respiration rate was 20 ×/minutes, and oxygen saturation was 96% on room air. On vaginal examination, she presented with 3-cm dilation, with head presentation. Breath sounds were normal, and there were no additional sounds. However, anthropometric evaluation revealed underweight body mass index (BMI=12.98 kg/m2). A chest X-ray was performed and revealed relapsed TB with giant bullae, thickened pleura, and pleural effusion on the left lung (Figure 1). She was then suspected to have drug-resistant TB, and we consulted the Internal Medicine Department, but a rapid molecular diagnostic test was negative. A complete blood count along with liver and kidney function evaluation was conducted and no abnormalities were found.
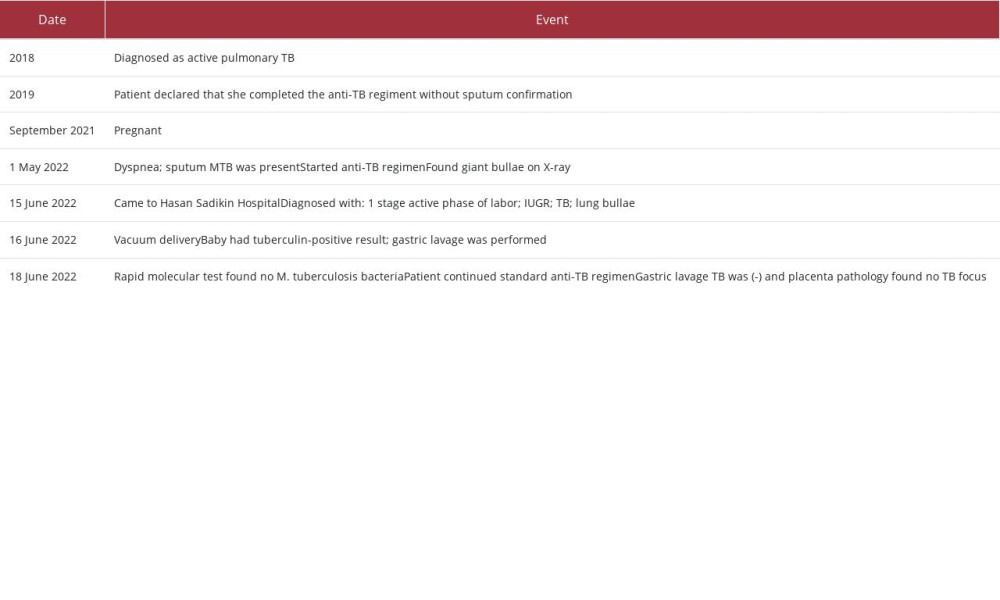
The patient was then diagnosed as having parturient first-stage active phase with TB and giant lung bullae. After 6 hours of observation, she was fully dilated, and then had vacuum extraction to shorten the 2nd phase of the labor due to her giant bullae. The risk of this condition is the increase of intrapulmo-nary pressure due pushing effort in labor. The Cardiothoracic Department was consulted for management of a giant bullae in labor, and they recommended observation during labor and no absolute contraindication in labor. The Cardiothoracic Department was present during labor. A baby boy was born with birth weight of 2054 grams, body length 45 cm, with Apgar score 7–9. The patient was discharged 2 days later after labor. The treatment timeline is presented in Table 1.
Discussion
Pregnancy is one of the conditions in which the immune system is relatively suppressed. However, a study found that pregnancy does not appear to increase susceptibility to TB infection or progression from latent TB infection to active TB disease [2]. On the first antenatal care visit, every pregnant woman should be evaluated for TB by assessing symptoms, performing a physical examination, and accessing risk factors (contact with people who have TB or working in a setting where TB exposure may be possible, contact with IV drug users, people with HIV, or immunocompromised people). The Mantoux tuberculin skin test or a TB blood test (eg, interferon-gamma release assay) could be used to test for TB in pregnancy [3]. However, tuber-culin skin tests have high false-positive rates, especially in countries where BCG vaccination is obligatory for infants [5]. Furthermore, the history of active TB in this patient may have obscured the result of the tuberculin test; therefore, a tuber-culin test was not conducted in this case. To the best of our knowledge, there is no guideline recommending routine sputum examination or chest X-ray evaluation for TB screening in pregnancy. This may contribute to the high number of TB cases in pregnancy, especially in countries where TB is endemic [5]. In this patient, we performed the MTB test, sputum test, and thorax X-ray, as recommended in Indonesian TB guidelines.
The patient in this case developed shortness of breath in the 8th month of gestation and a chest X-ray suggested TB relapse. She presented to our facility with no dyspnea in the 9th month of pregnancy due to her medication with TB drugs. Based on guidelines from the Indonesian Health Ministry (Figure 2), an anti-TB regimen can be started even without sputum confirmation if clinical characteristics suggest TB.
She was prescribed an intensive phase of anti-TB regimen consisting of Rifampicin 300 mg/day, Isoniazid 150 mg/day, Pyrazinamide 800 mg/day, and Ethambutol HCl 550 mg/day according to the Indonesian guidelines [6]. All of the drugs are category C according to the US Food and Drug Administration (FDA). However, pyrazinamide was not recommended in pregnancy according to CDC guidelines due to limited evidence of its safety and efficacy. Although not recommend by the CDC, a guideline by Queensland Health, Australia recommends the use of pyrazinamide as it does not cause significant fetal morbidity and mortality [7]. Inclusion of pyrazinamide in the treatment of tuberculosis in pregnancy therefore reduces the risk of ineffective treatment and must be balanced against the lack of animal studies [8]. In our patient, pyrazinamide did not affect the pregnancy because the TB started at the 8th month/3rd trimester of pregnancy and did not interfere with organogenesis.
A meta-analysis by Sobhy (2017) which evaluated 13 studies, including 3384 pregnancies in women with active TB, found that maternal and perinatal outcomes were consistently poorer with active TB disease than without [9], and there were higher odds of maternal death in pregnant women with active TB disease (odds ratio 4.1, 95% CI 0.65–25.2). Antenatal admission was also 9 times more frequent in pregnant women with active TB disease than in those without. Maternal anemia was 4 times more likely with active TB disease than without, and cesarean delivery was twice as likely. Active TB disease was associated with a 9 times greater rate of miscarriage. In pregnancies in women with active TB disease, perinatal death increased 4.2-fold, preterm birth increased 1.6-fold, acute fetal distress increased 2.3-fold, and low birth weight increased 1.7-fold [9].
TB is a chronic disease that induces a pro-inflammatory state. Patients with TB have higher levels of interleukin (IL)-1, IL-6, and tumor necrosis factor (TNF)-α. Ongoing inflammatory and immune responses are associated with dramatic shifts in tissue metabolism. These changes include local depletion of nutrients, increased oxygen consumption, and the generation of large quantities of reactive nitrogen and oxygen intermediates. These result in lower caloric intake and increased nutrition requirements. Furthermore, chronic inflammation produces reactive oxygen species and other inflammatory mediators that can impair placentation and increase the production of hypoxia inducible factors (HIF). HIF is associated with decreased fetal perfusion and subsequent intrauterine growth restriction (IUGR) [10]. In this patient, we found the fetus had IUGR due to underweight nutritional status and current active TB, which were correlated.
Prolonged or recurrent TB infection can alter lung histology where scarring occurs. Changes in integrity of lung structure can lead to formation of bullae in TB patients, although such cases are rare. Bullae are defined as air spaces in the lungs, measuring more than 1 cm in diameter when distended, while giant bullae occupy at least 30% of the hemithorax. Bullae rupture is the most common cause of spontaneous pneumothorax [7]. Possible causes of bleb rupture during pregnancy are Valsalva maneuver during labor, increased alveolar ventilation, and positive-pressure ventilation during general anesthesia. Cesarean delivery can prevent the need for Valsalva maneuver, but general anesthesia is best avoided as positive-pressure ventilation can cause rupture of bullae and blebs; thus, if indicated, spinal or epidural anesthesia should be preferred. To the best of our knowledge, there has been no study evaluating the safety and benefit of vaginal versus abdominal delivery in pregnant women with giant bullae. However, Jain et al stated that in mothers with spontaneous pneumothorax there is no evidence that cesarean section is necessary, and it should be performed for obstetric indications only [11]. There have been few reported cases of bullae in pregnancy and labor, which leads to controversies in method of delivery. We performed vacuum extraction to minimize the need for the Valsalva maneuver and to accelerate the 2nd phase of labor.
Pneumothorax complicating pregnancy has to be treated urgently because oxygen needs are increase in pregnancy. It may cause harmful effects to the fetus due to hypoxia and leads to fetal distress and death. Pneumothorax may be treated by observation, needle aspiration, and chest tube insertion, but the definitive treatment of pneumothorax due to rupture of bullae and blebs is surgical pleurodesis with or without bullectomy. Surgical intervention is usually performed in patients with dyspnea or complications such as pneumothorax or prolonged air leakage after tube insertion [11]. In this case, the patient came into labor without dyspnea. We found no signs or symptoms of pneumothorax; hence, no further intervention was done regarding the bullae-related complication. There are no guidelines on the duration of anti-TB drug use for a TB-infected patient with giant bulla. In this case, we consulted the Thoracic Surgery Department and observation during labor was performed. After delivery, the patient was given a standard regimen for pulmonary TB for 6 months. As explained in Figure 2, this patient was given 6 months of TB drugs because she was in the category of clinical TB. She was screened with multidrug-resistance tests, which were negative, followed by microscopic examination of BTA (- -) and a suggestive relapse TB X-ray. The management of this case was appropriate according to the national guidelines [6].
The rate of mother-to-child transmission of TB is 0% to 16%. Transmission can occur through the placenta, during vaginal delivery, or via amniotic fluid or vaginal secretion aspiration [12]. In patients who are sputum-positive for
Conclusions
In this case, we managed a patient with giant bullae and tuberculosis by vaginal delivery with vacuum extraction to shorten the 2nd phase of labor to prevent increased intrapulmonal pressure, which could possibly cause pneumothorax.
References:
1.. Muharam M, Firina DW, Mizarti D, Literature review: Multiple drug resistant tuberculosis in pregnancy: Andalas Obstetrics and Gynecology Journal, 2022; 6(1); 33-37
2.. Mathad JS, Gupta A, Tuberculosis in pregnant and postpartum women: Epidemiology, management, and research gaps: Clin Infect Dis, 2012; 55(11); 1532-49
3.. Miele K, Bamrah Morris S, Tepper NK, Tuberculosis in pregnancy: Obstet Gynecol, 2020; 135(6); 1444-53
4.. Lateef N, Dawood M, Sharma K, Recurrent spontaneous pneumothorax in pregnancy – a case report and review of literature: J Community Hosp Intern Med Perspect, 2018; 8(3); 115-18
5.. Faujdar SS, Singh U, Kumar S, Mantoux test defaulters in rural population attending tertiary care hospital in a tuberculosis endemic area: J Family Med Prim Care, 2022; 11(2); 677-79
6.. : National Guidelines of Tuberculosis Management, 2020, Jakarta, Ministry of Health Indonesia [cited 2022 December]; Available from: https://tbindonesia.or.id/pustaka_tbc/pedoman-nasional-pelayanan-kedokteran-tatalaksana-tuberkulosis/
7.. : Management of tuberculosis in pregnant women and newborn infants – guideline, version 3.2, 2021, Australia, State of Queensland [cited 2022 10 November]; Available from: https://www.health.qld.gov.au/__data/assets/pdf_file/0030/444558/tb-guideline-pregnancy.pdf
8.. Bothamley G, Drug treatment for tuberculosis during pregnancy: Safety considerations: Drug Saf, 2001; 24(7); 553-65
9.. Sobhy S, Babiker Z, Zamora J, Maternal and perinatal mortality and morbidity associated with tuberculosis during pregnancy and the postpartum period: A systematic review and meta-analysis: BJOG, 2017; 124(5); 727-33
10.. Robb KP, Cotechini T, Allaire C, Inflammation-induced fetal growth restriction in rats is associated with increased placental HIF-1α accumulation: PLoS One, 2017; 12(4); e0175805
11.. Jain A, Sami-Zakhari IR, Pulmonary complications of obstetric and gynecologic conditions: Pulmonary Complications of Non-Pulmonary Pediatric Disorders, 2017; 139-61
12.. Saramba MI, Zhao D, A perspective of the diagnosis and management of congenital tuberculosis: J Pathog, 2016; 2016; 8623825
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133