12 September 2023: Articles 
Acute Presentation of Tuberculosis Empyema in a Healthy Adolescent
Unusual clinical course, Challenging differential diagnosis
Edzelle Hankins1BDEF, Dmitri Khvolis1BDEF, John T. Spigos1BDEF, Oksana Tatarina-Nulman1ABCDEF*, Brande Brown1ABCDEF, Minnie John1ABCDEFDOI: 10.12659/AJCR.939419
Am J Case Rep 2023; 24:e939419
Abstract
BACKGROUND: Tuberculosis (TB) was the leading cause of infectious death worldwide until the COVID-19 pandemic, which reduced case reporting and disrupted TB diagnosis and services. While Mycobacterium tuberculosis remains a leading cause of morbidity and mortality globally, the disease burden within developed nations remains relatively rare. Although the many complications of TB are well known, no current data exists on those infected with TB who subsequently developed recurrent TB empyema, as it is such a rare complication, especially in pediatric and adolescent populations.
CASE REPORT: A previously healthy 15-year-old male patient presented with 5-day duration of cough, congestion, intermittent fever, and post-tussive emesis. Although born in the United States, 3 months before presentation, he returned from Senegal, where he had lived for 4 years. Imaging demonstrated consolidation with loculated effusion. Patient underwent video-assisted thoracoscopy and chest tube placement, draining 750 mL of purulent fluid testing positive for rare acid-fast bacilli. Rifampin, isoniazid, pyrazinamide, and ethambutol were administered, with discharge medication compliance ensured by daily videos surveillance through the Department of Health. Although compliant with medications, patient presented to the Emergency Department 2 months later with a multi-loculated fluid recollection and fistula formation requiring chest tube placement. After this discharge, patient experienced resolution of disease following completion of therapy.
CONCLUSIONS: TB complication should be considered as a differential diagnosis for pleural effusion in the appropriate clinical setting. Providers should not only consider the diagnosis but pursue appropriate testing and management early, particularly in those with risk factors, including travel to an endemic location.
Keywords: Adolescent Health, Empyema, Pleural, Empyema, Tuberculous, Pediatrics, Male, Adolescent, Humans, Child, Pandemics, COVID-19, Mycobacterium tuberculosis, Cough, Empyema
Background
In 2020, the World Health Organization (WHO) reported 1.1 million incident tuberculosis (TB) cases occurring among children, of which only 317 were reported in the United States [1,2]. The incidence rate of TB cases in the United States in 2021 was 157 per 100 000 among children aged 5 to 14 years, while in the 15 to 24 age group, the incidence rate was 675 per 100 000. According to the Center for Disease Control, pediatric TB is defined as disease in children under 15 years of age. As such, the patient discussed here is considered an adolescent or intermediate child-adult.
In 2019, the WHO estimated that there were about 205 000 deaths due to TB in children less than 15 years old [1]. Although there was a large drop in the number of people newly diagnosed with TB from 2019 to 2020, this is most likely a false decrease because of the COVID-19 pandemic. This reduction in case reporting reflect disruptions in TB diagnosis and services, such as reduced health system capacity, less willingness and ability to seek care due to lockdowns, concerns about risks of going to health care centers during a pandemic, and stigma associated with similarities in the symptoms related to TB and COVID-19 [3]. The most immediate consequence of this decrease in diagnosis was an increase in the number of people who died from TB in 2020, at all levels: global, regional, and country [3].
There are no current data published on those infected with TB who subsequently developed TB empyema, as it is such a rare complication, especially in the pediatric population. In addition, this complication burden may also be underrepresented due to missed diagnosis. These pulmonary complications typically occur 6 to 12 weeks after a primary TB infection or can result due to reactivation of TB [4]. In developed countries, TB pleurisy usually occurs in older individuals, with the median age of 35.9±15.8 years [5]. Here, we present the rare case of a previously healthy 15-year-old male patient with an acute presentation of TB complicated by right-sided empyema, with subsequent fistula formation and fluid drainage.
It has been shown that TB rates are highest among US persons from sub-Saharan Africa, Asia, and the Pacific Islands, and the median incidence rate ratio is 0.5 for persons who received a TB diagnosis <1 year after US entry [6]. Children born in the United States who had traveled to a country with a high prevalence of TB in the past 12 months before the skin test were 3.9 times more likely to have a positive skin test than were children who had not traveled [7].
Case Report
A 15-year-old male patient presented to the Emergency Department (ED) with a 5-day duration of cough, congestion, intermittent fever and chills, and post-tussive emesis. Although born in the United States, 3 months prior to presentation, the patient returned from Senegal, where he had been residing for 4 years. While in Senegal, he had a self-resolving illness associated with cough, intermittent fever, and weight loss, which he recalled as occurring almost 1 year before his return to the United States. At that time, he was seen by a primary provider; however, a chest X-ray was not performed, nor was any additional laboratory testing done. The patient was not given any medication for his illness and did not recall any specific diagnosis. The patient had never received the bacillus Calmette-Guérin vaccine and had tested negative for purified protein derivative (PPD) prior to his travel to Senegal. On return to the United States, he had full resolution of his previous symptoms and had regained the lost weight. He further reported being in his normal state of health, until this acute presentation to the ED.
In the ED, the chest X-ray demonstrated a large right-sided loculated effusion and associated consolidation, (Figure 1A) with subsequent contrast-enhanced computed tomography showing a large loculated peripherally enhancing pleural effusion, consistent with an empyema (Figure 2). Initial laboratory results were largely unremarkable, except for a slightly elevated C-reactive protein level (15.1 mg/L, ref: ≤3.0). HIV testing also resulted negative. The patient was started on ceftriaxone 2 g daily, clindamycin 600 mg every 6 h, and azithromycin (first dose of 500 mg, followed by 250 mg daily) for presumed community acquired pneumonia. On day of admission 1, the patient was placed on airborne precautions, and a was PPD test placed, which was later positive, with a 22-mm diameter induration.
On the same day, a video-assisted thoracoscopic surgery was performed and showed approximately 750 mL of frank pus in the right chest, which was completely evacuated. A fair amount of fibrinous rind was also debrided as part of a decortication, and a chest tube (10 French) was placed.
Due to the thickness of the pleural fluid, the fluid could not be analyzed for cells and chemistry. However, there was rare acid-fast bacilli on staining, and it was positive for
Acid-fast bacteria sputum cultures were sent on 3 separate days, all resulting negative. First-line therapy for TB was also started (rifampin, isoniazid, pyrazinamide, ethambutol [RIPE], and supplemental pyridoxine). The patient had blurry vision 2 days after initiation of the RIPE therapy, and ethambutol was replaced with levofloxacin. Pleural fluid and lung tissue cultures both grew antibiotic-sensitive mTB. A chest tube drained an additional 260 cc of fluid and was removed after 5 days (Figure 1B). The patient was discharged home the following day with instructions to complete a 6-month treatment course for TB.
At home, the patient’s medication compliance was monitored by uploading daily videos via a phone application through the United States Department of Health, with good patient compliance reported. The patient’s family were evaluated for latent TB infection. His biological father and 3 siblings tested negative; however, his biological mother tested positive and was advised to start isoniazid therapy. Two months after discharge, the patient had a 1-week duration of skin irritation and pruritis at the location of the previous right-sided chest-tube, which also had a scab-like exterior surface with some mild swelling. A minor abrasion to the scab caused a “handful-sized” amount of yellow fluid drainage at the site, along with small amounts of occasional flow with torso position changes. The patient returned to the ED, at which time imaging confirmed a multi-loculated recollection of fluid on the right side (Figure 3).
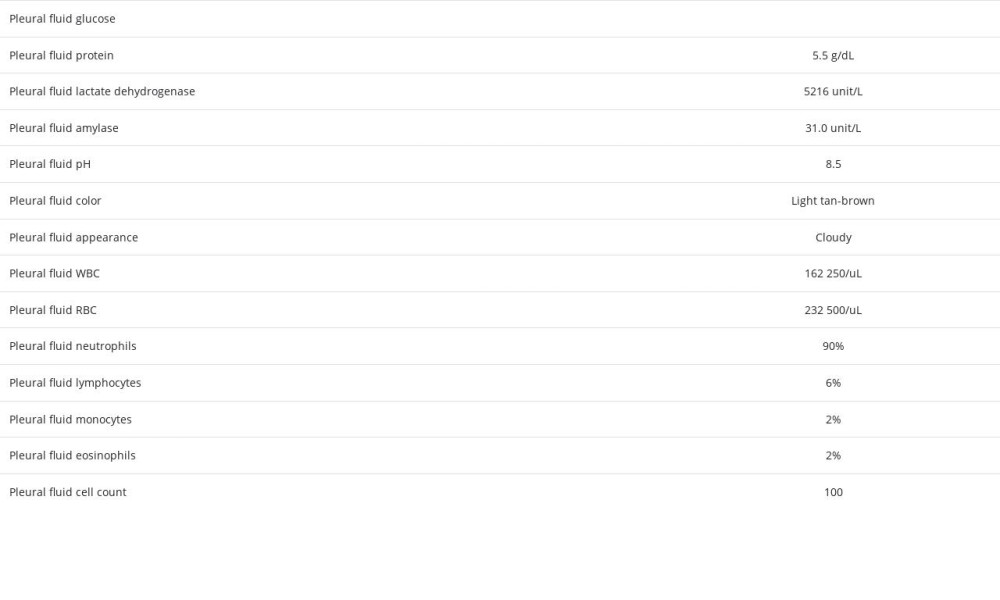
A second right posterior chest tube (10 French) resulted in 290 cc of initial fluid. Frank pus was noted during initial drainage, transitioning to drain a total of 400 mL of serosanguineous fluid, which was sent for analysis (Table 1). Alteplase 4 mg was required daily over the next 3 days to assist with drainage, and the chest tube was removed on day 4 of admission. Throughout admission, he was maintained on his initial therapy course (rifampin, isoniazid, pyrazinamide, levofloxacin), with a subsequent increase in the dose of levofloxacin (750 mg). The patient was asymptomatic on discharge home (Figure 4) and completed the remaining medication course for TB. He remained compliant, completing the 6-month antibiotic course, and experienced resolution of symptoms. Resulting cultures grew mTB susceptible to the prescribed drugs. After completion of therapy, imaging performed by the Department of Health showed resolution of pulmonary pathology.
Discussion
Owing to the rarity of occurrence, the diagnosis of TB in adolescents is often delayed in countries where TB burden is low [8]. In this case presentation, the patient’s initial symptoms of cough for 5 days with intermittent fever led to an initial suspicion for community-acquired pneumonia, given the acute nature of illness in a previously healthy adolescent. In one study, patients with active TB in Amsterdam were identified, and their tuberculin skin test-positive contacts who did not take isoniazid prophylaxis for 10 years (2002–2011) were monitored; 75% of active TB cases in the contacts occurred within 1 year of diagnosis of TB in the index case, and 97% within 2 years [9]. Children and adolescents were at the greatest risk of developing active TB, but the timeline of developing TB was similar in all age groups.
Endorsement of travel to Senegal expanded the differential diagnosis to include TB, as approximately one-quarter of all global TB cases in 2020 confirmed travel history to Africa [3]. The present case stresses that, in the evaluation of a patient with classic symptoms of pneumonia or pleural infection, it is of the utmost importance to gather a thorough history of recent travel, antibiotic use, and vaccination status.
Although pediatric empyema is relatively uncommon, its incidence has become more prevalent in the United States [10]; however, in a previously healthy child, pleural complications are usually secondary to acute bacterial pneumonia, in comparison to chronic infections, such as pulmonary TB [11]. TB pleural effusion is the second most common form of extrapulmonary TB, and the most common cause of pleural effusion in endemic areas [12]. In the pediatric population, effusions occur most often in the setting of primary TB, in contrast to in the adult population, in which effusions are primarily secondary to reactivation of the disease [12].
There are 2 “prototypical” types of TB effusion: a reactive effusion, and the much less common TB empyema, as seen in this case. Reactive TB pleural effusions occur due to a delayed hypersensitivity reaction to mycobacteria and mycobacterial antigens in the pleural space. The inflammation that is produced results in lymphocytic pleuritis, which decreases the amount of fluid that can be absorbed from the pleural space [4], which is typically characterized as serous straw-colored fluid [13]. TB empyema is rare, is characterized as purulent fluid filled with TB organisms on acid-fast bacteria stains, and usually develops in fibrous scar tissue [4]. Unlike typical TB pleural effusion, the macroscopic appearance of pleural fluid in empyema is pus or turbid fluid with predominantly neutrophilic cells [13].
Lymphocyte predominant pleural fluid has long been considered part of the diagnostic criteria for pleural TB; however, a retrospective analysis of 200 patients aged over 18 years demonstrated 9.5% of patients with pleural TB had neutrophil-predominant pleural fluid [14]. In the same population, TB was more frequently detected in the pleural fluid from patients in the neutrophil-predominant group. Those with neutrophil-predominant pleural TB demonstrated a more intense inflammatory response than did the lymphocyte-predominant population [14]. The pleural effusion in the present patient was exudative in character, with high protein, neutrophilic predominance, and high lactate dehydrogenase. This further supports that TB should always be considered among the differential diagnoses in those with neutrophil predominant pleural analysis.
Leakage of pus from the lymphatic system with hematological distribution of the disease is believed to contribute to the pathological process of pulmonary empyema. Although current data is not available, a cohort of patients infected with TB in the United States from 1993 to 2003 demonstrated that 3.6% of patients developed TB empyema [4]; however, this presentation typically occurred in older individuals. Prognosis of TB empyema is variable, ranging from slow disease progression and even death, to that of slow resolution with pleural calcification and fibrosis [4]. At present, there are no available data on the recurrence rate of TB empyema, as seen in the present patient.
In the present patient, it is difficult to discern whether the associated complications in the reported infection were from primary and reactivated TB. He was a healthy adolescent with no evidence of healed TB on imaging and had only rare acid-fast bacilli in plural fluid, which is typically seen in primary TB. However, the presentation of primary TB usually occurs within 4 to 12 weeks after exposure. This patient had a symptom-free interval of at least 1 year, along with a pleural fluid analysis and thick rind, as typically seen in reactivated TB.
Conclusions
Although TB empyema cases are rare in the pediatric population, TB should remain a differential of potential causes of pleural effusion and empyema, especially in patients with a history of immigration or travel to endemic areas. Furthermore, providers must maintain a high level of suspicion to diagnose TB in cases of thoracic infections and routinely assess for TB in collected samples, such as pleural fluid. This remains more important than ever as the COVID-19 pandemic has reversed years of progress in reducing disease burden and deaths due to TB.
Additional research regarding diagnosis and management options for pleural complications, such as TB effusions or empyema, in the pediatric and adolescent population are needed.
Figures
References:
1.. : Global tuberculosis report 2019, 2019, Geneva, World Health Organization License: CC BY-NC-SA 3.0 IGO. Available from: https://www.who.int/publications/i/item/9789241565714
2.. : Division of Tuberculosis Elimination, National Center for HIV, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention Available from: https://www.cdc.gov/tb/topic/populations/tbinchildren/default.htm
3.. : Global tuberculosis report 2021, 2021, Geneva, World Health Organization License: CC BY-NC-SA 3.0 IGO. Available from: https://www.who.int/publications/i/item/9789240037021
4.. Cohen LA, Light RW, Tuberculous pleural effusion.: Turk Thorac J, 2015; 16(1); 1-9
5.. Zhao T, Xu Y, Song Q, Medical thoracoscopy for tuberculous pleurisy: A retrospective analysis of 575 cases.: Ann Thorac Med, 2019; 14(2); 134-40
6.. Tsang CA, Langer AJ, Kammerer JS, Navin TR, US tuberculosis rates among persons born outside the United States compared with rates in their countries of birth, 2012–20161.: Emerg Infect Dis, 2020; 26(3); 533-40
7.. Lobato MN, Hopewell PC, Mycobacterium tuberculosis infection after travel to or contact with visitors from countries with a high prevalence of tuberculosis.: Am J Respir Crit Care Med, 1998; 158(6); 1871-75
8.. Al Dubisi F, Harvey G, Ostrow O, Distinguishing features of adolescents with undiagnosed infectious tuberculosis attending a Pediatric Emergency Department.: Open Forum Infect Dis., 2021; 8(9) ofab435
9.. Sloot R, Schim van der Loeff MF, Kouw PM, Borgdorff MW, Risk of tuberculosis after recent exposure. A 10-year follow-up study of contacts in Amsterdam.: Am J Respir Crit Care Med, 2014; 190(9); 1044-52
10.. Byington CL, Spencer LY, Johnson TA, An epidemiological investigation of a sustained high rate of pediatric parapneumonic empyema: Risk factors and microbiological associations.: Clin Infect Dis, 2002; 34(4); 434-40
11.. Balfour-Lynn IM, Abrahamson E, Cohen G, BTS guidelines for the management of pleural infection in children: Thorax, 2005; 60; i1-i21
12.. Chopra A, Huggins JT, Tuberculous pleural effusion. April 5, 2022 . Available from: Uptodate.com
13.. Ayuk AC, Gray D, Vanker A, Zampoli M, Tuberculosis in children presenting with chylothorax - Report of two cases and review of the literature.: Respir Med Case Rep, 2019; 27; 100848
14.. Choi H, Chon HR, Kim K, Clinical and laboratory differences between lymphocyte- and neutrophil-predominant pleural tuberculosis.: PLoS One, 2016; 11(10); e0165428
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133