31 January 2021: Articles 
Acute Lower-Extremity Ischemia in a Patient with COVID-19
Unusual clinical course
Hadia Ahmad1BDEF*, Swhaeb M. Shubair1BDEF, James Kruer1EF, Chehada Anthony Hatoum1ACDEFDOI: 10.12659/AJCR.928471
Am J Case Rep 2021; 22:e928471
Abstract
BACKGROUND: Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) causes coronavirus disease 2019 (COVID-19), which has become a global pandemic. The typical symptoms are fever, cough, and shortness of breath, but the disease can present with atypical signs, including those associated with a hypercoagulable state. These signs include deep venous thrombosis, pulmonary embolism, ischemic stroke, and acute coronary syndrome. Herein, we present the case of acute bilateral lower-extremity ischemia as a thromboembolic complication in a patient with COVID-19.
CASE REPORT: A 76-year-old woman presented with acute bilateral lower-extremity ulcerations covered with eschar formation of several weeks’ duration. During her hospital course, she underwent a test for COVID-19 and the result was positive. An angiogram of the patient’s lower extremities showed occlusions of the right distal posterior tibial artery, right mid-distal anterior tibial artery, right dorsalis pedis artery, left mid-distal anterior tibial artery, left dorsalis pedis artery, and left popliteal vein. Tissue plasminogen activator was administered to treat the occlusions. On the following day, the patient had an acute decline in her neurologic state and was emergently intubated. A computed tomography scan of the brain confirmed a subarachnoid hemorrhage requiring reversal of tissue plasminogen activator. The patient was transitioned to comfort care and ultimately died.
CONCLUSIONS: In conclusion, acute limb ischemia should be acknowledged as a rare complication associated with COVID-19. It is important to raise awareness of arterial thrombosis as a possible complication of the hypercoagulable state caused by SARS-CoV-2 because prompt recognition is essential for early diagnosis and treatment. These actions could have a significant impact on patients’ overall outcome.
Keywords: COVID-19, Embolism and Thrombosis, Lower Extremity, COVID-19, Fatal Outcome, Ischemia, Subarachnoid Hemorrhage, thromboembolism
Background
A novel coronavirus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is responsible for a global pandemic that has caused over 1,000,000 deaths worldwide as of November 2020 [1]. SARS-CoV-2 causes coronavirus disease 2019 (COVID-19), which can present with a wide range of manifestations including acute respiratory distress syndrome/respiratory failure, acute liver or kidney injury, and heart failure [2]. Another manifestation that has recently garnered attention is abnormalities in coagulation leading to a hyper-coagulable state that can in turn lead to both arterial and venous thrombosis. We present a case of a 76-year-old woman with COVID-19 who presented with acute limb ischemia of her bilateral lower extremities requiring administration of tissue plasminogen activator (tPA).
Case Report
A 76-year-old woman with a history of primary biliary cirrhosis and autoimmune hepatitis (treated with azathioprine), hyper-tension, and hyperlipidemia presented to our hospital with ulcers on her lower extremities and intermittent fever of several weeks’ duration. The patient noted increased swelling and discoloration of her feet but denied shortness of breath, cough, calf tenderness, or any additional symptoms. Her body mass index was 20.6 kg/m2, and she had no prior history of diabetes mellitus, obesity, cerebral vascular accident, myocardial infarction, or peripheral artery disease. The patient initially noticed ulcers on her feet while on vacation in Florida 4 weeks prior and believed they were possibly due to bug bites. She initially sought treatment at an urgent care center and was prescribed clindamycin and ciprofloxacin after receiving a diagnosis of cellulitis.
Upon returning home to Georgia, the patient visited an Emergency Department because her symptoms had not resolved and she was experiencing intermittent fever. During that visit, the patient was treated with an additional course of antibiotics and was underwent testing for SARS-CoV-2, with a positive result. The patient completed this second course of antibiotics, but worsening of the ulcers prompted her to seek care at our hospital.
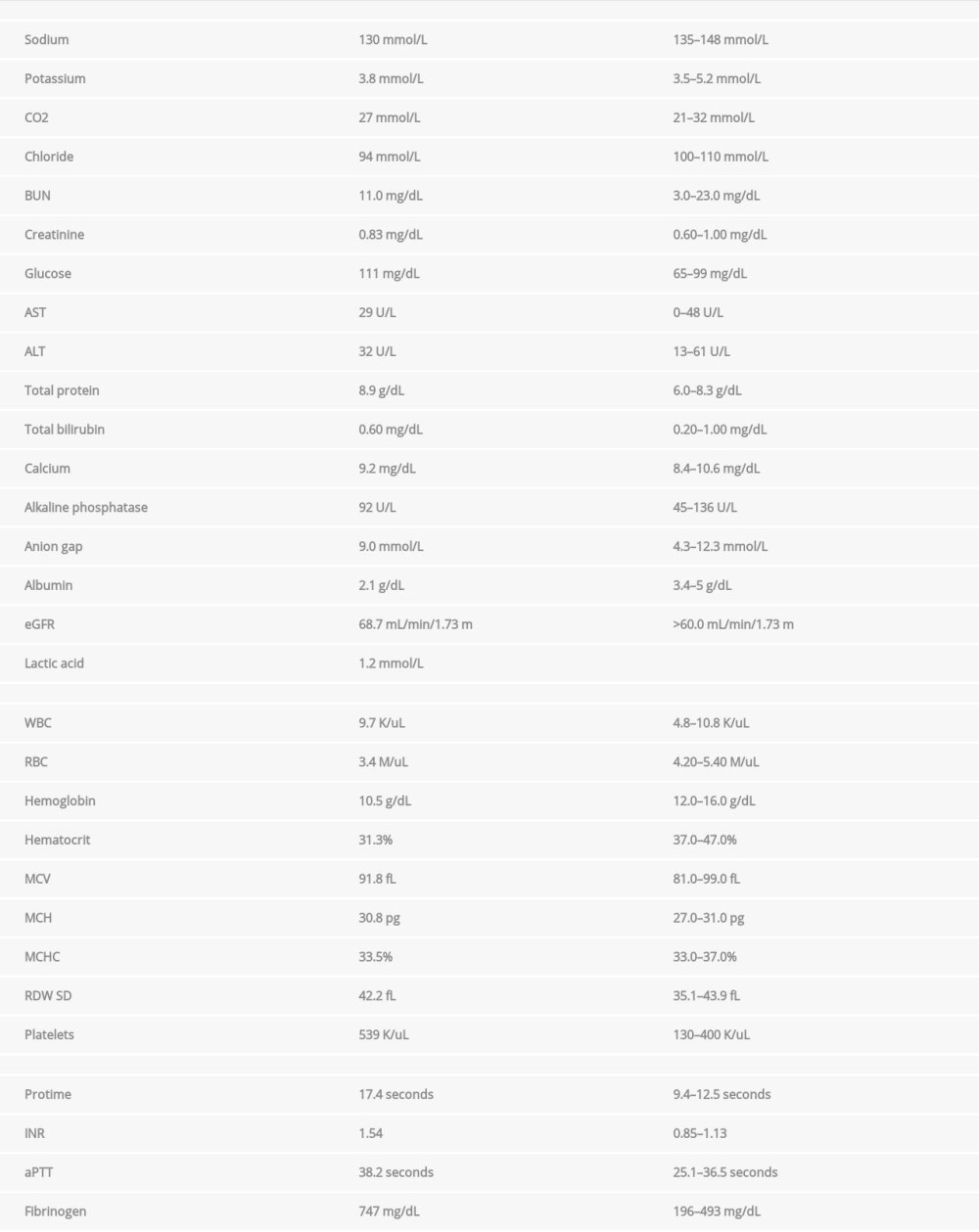
On presentation, the patient was afebrile but tachycardic (104 beats/min). Her examination showed a 4.0×5.0-cm ulcer over the lateral aspect of the left ankle and a 2.0×4.0-cm ulcer over the dorsal aspect of the right foot at the metatarsal region. Both ulcers had overlying eschars as shown in Figures 1 and 2. Her laboratory test results were significant for a sodium level of 130 mmol/L and hemoglobin of 10.5 g/dL. Her test results also showed a white blood cell count of 5500/μL, erythrocyte sedimentation rate of 40 mm, and C-reactive protein of 26.00 mg/dL. The D-dimer level was elevated at 1.898 μg/mL (≤0.400 μg/mL FEU). The remainder of the patient’s laboratory results on admission are presented in the Table 1. Radiographs of bilateral feet were indeterminate for osteomyelitis. The patient was started on empiric vancomycin and piperacillin-tazobactam and admitted to the hospital to rule out osteomyelitis.
The following day, magnetic resonance imaging was performed. It showed soft tissue inflammation of the right foot, a possible wound overlying the right lateral malleolus, and reactive periostitis in the left foot. There was no evidence of osteomyelitis. Upon further assessment of the patient’s ulcers, dry gangrene was diagnosed. Bilateral dorsalis pedis and posterior tibialis pulses were not palpable on examination. Dorsalis pedis signal was not appreciated on bedside Doppler; however, the patient was found to have monophasic posterior tibialis signals bilaterally. The patient was started on a heparin drip. Vascular Doppler of the bilateral lower extremities showed occlusion of the right distal posterior tibial artery, right mid-distal anterior tibial artery, right dorsalis pedis artery, left mid-distal anterior tibial artery, left dorsalis pedis artery, and left popliteal vein. A vascular surgeon performed an angiogram of the patient’s bilateral lower extremities, with placement of lytic catheters for transcatheter tPA. The patient remained on heparin infusion while receiving tPA at 2.0 mg/h through Cragg-McNamara catheters, which were placed in the bilateral anterior tibial and popliteal arteries. The following day, the patient had an acute decline in her neurological status and was found to have a subarachnoid hemorrhage with herniation requiring tPA reversal and craniotomy for clot evacuation. After a goals-of-care discussion with the patient’s family, the decision was made to de-escalate care and pursue comfort measures. The patient ultimately died.
Discussion
COVID-19 has a wide spectrum of manifestations including hypercoagulability. Although the pathogenesis underlying this hypercoagulable state is not completely understood, some researchers have proposed that it could be related to changes in prothrombic factors, such as elevated levels of factor VIII and fibrinogen [3]. Others have attributed the hypercoagulable state to the inflammatory response and cytokine storm associated with the disease. These factors ultimately lead to local dysfunction in the coagulation cascade, which can in turn cause a widespread hypercoagulable state involving the macro- and microvasculature [4]. Patients with certain risk factors have been noted to have poorer outcomes from SARS-CoV-2 infection [5]. Some of these risk factors, including elevated levels of D-dimer and C-reactive protein as well as hypertension, which were present in our patient, can increase the risk of thrombosis [5]. Multiple studies have reported thrombotic complications associated with COVID-19; these complications have mainly included venous thromboembolic events such as pulmonary emboli and deep vein thromboses [4]. Arterial thrombosis reported thus far includes ischemic strokes, but there have also been reports of mesenteric ischemia, limb ischemia, and acute coronary syndrome [4].
Although uncommon, a few studies and case reports have discussed acute limb ischemia in patients with COVID-19. Kaur et al. [6] reported a case of a 71-year-old man who was admitted with acute respiratory failure due to COVID-19. On day 5 of hospitalization, he reported severe pain in his right arm and was found to have extensive occlusive disease requiring embolectomy of the right brachiocephalic, subclavian, axillary, brachial, radial, and ulnar arteries; endarterectomy of the right brachial artery; and anticoagulation with low molecular weight heparin. After this multipronged treatment, the patient had palpable pulses in his upper extremity, in addition to normal sensation and function [6]. An observational study performed in Italy focused on the incidence and outcomes of 20 patients with acute limb ischemia [7]. The researchers found the incidence of acute limb ischemia to be greater in the previous few months of 2020 compared with 2019, and they attributed the higher incidence to the increase in cases caused by thromboembolic disease associated with COVID-19. With regard to treatment, the study reported the success of revascularization was low, but the use of systemic heparin was thought to possibly improve “surgical treatment efficacy, limb salvage, and overall survival” [7]. We were able to identify at least 22 additional case reports that discussed arterial thrombosis involving the lower extremities, carotid artery, superior mesenteric artery, and descending aorta that were managed medically with anticoagulation and thrombectomy, although some cases also required amputation.
Conclusions
In conclusion, thromboembolic events should be recognized as a complication of the hypercoagulable state associated with SARS-CoV-2 infection. It is important to acknowledge these findings because the number of COVID-19 cases worldwide continues to increase. Acute limb ischemia is a rare manifestation of the disease. Early identification and treatment of acute limb ischemia are critical because they can have a significant impact on a patient’s outcome.
References:
1.. : WHO coronavirus disease (COVID-19) dashboard, Geneva, WHO https://covid19.who.int/
2.. Baj J, Karakuła-Juchnowicz H, Teresiński G, COVID-19: Specific and non-specific clinical manifestations and symptoms: the current state of knowledge: J Clin Med, 2020; 9(6); 1753
3.. Cuker A, Peyvandi F, Coronavirus disease 2019 (COVID-19): Hypercoagulability UpToDate 2020 July. https://www.uptodate.com/contents/coronavirus-disease-2019-covid-19-hypercoagulability
4.. Abou-Ismail MY, Diamond A, Kapoor S, The hypercoagulable state in COVID-19: incidence, pathophysiology, and management: Thromb Research, 2020; 194; 101-15
5.. Cooper ID, Crofts CA, DiNicolantonio JJ, Relationships between hyper-insulinaemia, magnesium, vitamin D, thrombosis and COVID-19: Rationale for clinical management: Open Heart, 2020; 7(2); e001356
6.. Kaur P, Qaqa F, Ramahi A, Acute upper limb ischemia in a patient with COVID-19: Hematol Oncol Stem Cell Ther, 2020 [Online ahead of print]
7.. Bellosta R, Luzzani L, Natalini G, Acute limb ischemia in patients with COVID-19 pneumonia: J Vasc Surg, 2020; 20; 31080-86
Figures
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133