05 May 2021: Articles 
A Case of Sheehan Syndrome 7 Years Postpartum with Transaminitis and Hyperlipidemia
Challenging differential diagnosis, Rare disease
Sanah Sadiq1ABCE*, Arnab Chowdhury1ABCEDOI: 10.12659/AJCR.930908
Am J Case Rep 2021; 22:e930908
Abstract
BACKGROUND: Sheehan syndrome (pituitary necrosis after postpartum hemorrhage) can present in various ways, depending on the hormones that are deficient. There may be a long delay to diagnosis of over a decade because symptoms are often vague and pituitary dysfunction progresses gradually. We describe a case of a patient with acute presentation of Sheehan syndrome 7 years after the obstetric event and with no clear precipitating event.
CASE REPORT: A 46-year-old woman with a history of hyperlipidemia and transaminitis came to the clinic for evaluation of hypotension and syncope. She had a history of longstanding anhedonia, fatigue, and postpartum hemorrhage 7 years previously and had undergone medical evaluations with her primary doctor with no cause found. Laboratory results showed anemia, central hypothyroidism, and adrenal insufficiency. A diagnosis of Sheehan syndrome was made.
CONCLUSIONS: Sheehan syndrome is a rare condition of progressive pituitary dysfunction, which can present with nonspecific symptoms and a myriad of laboratory abnormalities until an adrenal crisis is triggered years after the precipitating event. Screening patients for hypopituitarism by free thyroxine levels and adrenocorticotropic hormone (ACTH) stimulation testing is vital for determining whether hypopituitarism is the cause in the appropriate clinical scenario. Use of thyroid-stimulating hormone levels and morning cortisol testing alone will miss this diagnosis, and free thyroxine levels and ACTH stimulation testing are vital.
Keywords: Hormones, Hypopituitarism, Hypotension, Postpartum Hemorrhage, adrenal insufficiency, Hyperlipidemias, Postpartum Period, Pregnancy
Background
Hypopituitarism in general is a rare diagnosis, and Sheehan syndrome is diagnosed even less often. Sheehan syndrome (pituitary necrosis after postpartum hemorrhage) can be diagnosed immediately postpartum, but the diagnosis is often delayed for several years because patients have nonspecific symptoms (eg, fatigue, weight gain, headache) until an adrenal crisis occurs. Pituitary dysfunction progresses slowly, and contributing factors could include genetic predisposition, coagulation abnormalities, pituitary autoantibodies, and small sella turcica size, which increases the likelihood of compression of blood supply. Because of hypopituitarism, the mortality rate of patients with Sheehan syndrome is 1.2 to 2.17 times higher than that of the general population [1], and patients can present with adrenal crisis, myxedema coma, hypoglycemia, and hyponatremia, which could be precipitated by an infection or surgery. Herein, we describe a case of a patient with Sheehan syndrome to highlight the importance of considering and diagnosing hypopituitarism in patients with nonspecific symptoms to decrease potential morbidity and mortality from a potential Sheehan syndrome-related adrenal crisis [2,3].
Case Report
A 46-year-old woman with hyperlipidemia and chronically elevated liver enzyme levels of unclear origin sought care at her primary care practitioner’s office. She had awoken with severe abdominal pain, had a loose bowel movement, and lost consciousness when she stood up from the toilet. On examination, she was noted to be pale and hypotensive (blood pressure, 68/44 mmHg). She was transferred to the emergency department, where she received a 2-L normal saline fluid bolus, after which her hypotension resolved. The physical examination was normal, except for conjunctival pallor. Initial laboratory evaluations showed anemia, with a hemoglobin level of 9.8 g/dL, and elevated liver enzyme levels, with an alanine aminotransferase level of 102 U/L and an aspartate aminotransferase level of 115 U/L (at baseline for the patient). All of the following tests were within normal ranges or had negative results: basic metabolic panel, lipase level, hemoccult test, urinalysis, and pregnancy test. Because of mild hematochezia, the patient had been scheduled for outpatient colonoscopy before her current illness. She did not have any overt bleeding at her initial evaluation.
She was hospitalized for further evaluation and treatment. There was no evidence of infection or acute coronary syndrome. The following tests were within normal ranges or had negative results: thyroid-stimulating hormone (TSH) and random cortisol levels, stool infection panel, an abdominal computed tomography scan, and colonoscopy. She continued to have orthostatic symptoms after further fluid resuscitation. Given the absence of an alternative cause of her symptoms, additional endocrine testing was undertaken (Table 1). Her TSH was 2.9 mIU/L, and free triiodothyronine (T3) and free thyroxine (T4) levels were undetectable. A random cortisol level was 10 mcg/dL, and adrenocorticotropic hormone (ACTH) level was undetectable. With 1-mcg ACTH stimulation testing, her 30-min cortisol level was 12 mcg/dL, confirming a diagnosis of adrenal insufficiency. Her prolactin level was normal at 14.3 ng/mL. Her level of insulin-like growth factor binding-protein 3 was low at 0.9 mcg/mL, indicating growth hormone deficiency. Magnetic resonance imaging of the brain was consistent with empty sella (Figure 1).
During further examination of the patient’s history, she reported having postpartum hemorrhage 7 years earlier, with an estimated blood loss of 700 mL. She had delivered in the hospital, and bleeding subsided without intervention. She did not receive a blood transfusion. After childbirth, she had difficulty lactating and became menopausal 4 years later. She also reported having had symptoms of anhedonia and light-headedness for several years. Over the years, her primary care practitioners had evaluated her condition by TSH levels, which had remained in the normal range. She was noted to have elevated liver enzyme levels for several years, for which a cause could not be determined. She had also been diagnosed with hyper-lipidemia and was intolerant of statins because of myalgias.
The patient was diagnosed with Sheehan syndrome, which was associated with hypothyroidism, adrenal insufficiency, growth hormone deficiency, and gonadotropin deficiency. She was initially given hydrocortisone, 15 mg in the morning and 10 mg in the evening, which was followed by levothyroxine supplementation, 75 mcg daily started 5 days later, and her hypo-tension and orthostatic symptoms resolved. Furthermore, her hyperlipidemia also resolved with the above treatments, and her liver enzyme levels normalized (Table 2).
Discussion
The incidence of Sheehan syndrome has declined over the years, largely because of improved obstetric care, but under-diagnosis may also contribute to the lower incidence. Sheehan syndrome is far less common in developed countries than in places with limited access to obstetric care. During pregnancy, the pituitary gland enlarges 120% and is therefore highly vulnerable to ischemia in the setting of hypotension and hemorrhage during delivery. Patients can have deficiencies in some or all anterior pituitary hormones and even in posterior pituitary hormones, causing diabetes insipidus. Failure to lactate can result from decreased prolactin levels, and patients can develop amenorrhea from gonadotropin deficiency. Laboratory evaluations should include an ACTH stimulation test, a glucagon stimulation test, insulin-tolerance tests, and free T4 levels. Patients may have anemia, thrombocytopenia, and coagulation disorders, and pituitary imaging is likely to show partial or completely empty sella, as in the present case. Differential diagnoses include pituitary adenoma and lymphocytic hypophysitis [4–6].
A diagnosis may not be made for years because of vague symptoms, including fatigue and mild cognitive impairment. A study of 60 cases in Costa Rica estimated an average time to diagnosis of 13 years from delivery, while another study in France estimated an average of 9 years [3,7]. Pituitary dysfunction, which slowly progresses, is thought to be due to an inflammatory or autoimmune cause [8]. This may occur because antigens released during pituitary necrosis trigger an autoimmune response that causes the progressive pituitary dysfunction, and autoantibodies have been detected in patients with Sheehan syndrome, but not consistently [8]. Some patients do not have a history of postpartum hemorrhage, which can make the diagnosis even more challenging; therefore, Sheehan syndrome should be considered for patients with hyponatremia, hypoglycemia, and hypotension. Screening patients for thyroid hormone deficiency with new-onset hyperlipidemia has been suggested. The present patient’s hyperlipidemia was likely attributable to hypothyroidism and resolved with treatment of her hypothyroidism [9,10]. Additionally, this patient had longstanding elevation of liver enzyme levels before the diagnosis of hypopituitarism. These abnormalities normalized after treatment for her hypopituitarism and could have been related to the hypothyroidism or adrenal insufficiency. Recognition of these endocrine abnormalities is vital to avoid long-term complications of hyperlipidemia and obesity, including higher cardiovascular risk and even cirrhosis related to nonalcoholic steatohepatitis [11,12]. Regarding specific strategies for preventing Sheehan syndrome, discouraging homebirths, which can be associated with increased blood loss, and giving early transfusions for postpartum hemorrhage may limit risk [4,12,13].
Conclusions
In conclusion, screening patients by using only TSH and morning cortisol testing will miss a diagnosis of central hypopituitarism [2]. Diagnosis can be especially challenging in developed countries because the incidence of cases is low, symptoms are often vague, and patients can have late crises and unusual presentations such as severe hyponatremia, pancytopenia, cardiac tamponade, psychosis, and even cardiac arrest [2,14,15]. Some of these abnormalities and conditions can resolve with hormone supplementation, which is reassuring. Clinicians must have a low threshold for screening for adrenal insufficiency with ACTH stimulation testing and for central hypothyroidism with free T4 levels in patients with suspected cases because of the high risk of mortality from an adrenal crisis (0.5 per 100 patients annually) [16] and increased risk of premature atherosclerosis [9], and therefore cardiovascular risk.
References:
1.. Tomlinson JW, Holden N, Hills RK, Association between premature mortality and hypopituitarism. West Midlands Prospective Hypopituitary Study Group: Lancet, 2001; 357(9254); 425-31
2.. Karaca Z, Laway BA, Dokmetas HS, Sheehan syndrome: Nat Rev Dis Primers, 2016; 2; 16092
3.. Ramiandrasoa C, Castinetti F, Raingeard I, Delayed diagnosis of Sheehan’s syndrome in a developed country: A retrospective cohort study: Eur J Endocrinol, 2013; 169(4); 431-38
4.. Diri H, Karaca Z, Tanriverdi F, Sheehan’s syndrome: New insights into an old disease: Endocrine, 2016; 51(1); 22-31
5.. Kilicli F, Dokmetas HS, Acibucu F, Sheehan’s syndrome: Gynecol Endocrinol, 2013; 29(4); 292-95
6.. Kovacs K, Sheehan syndrome: Lancet, 2003; 361(9356); 520-22
7.. Gei-Guardia O, Soto-Herrera E, Gei-Brealey A, Chen-Ku CH, Sheehan syndrome in Costa Rica: Clinical experience with 60 cases: Endocr Pract, 2011; 17(3); 337-44
8.. Goswami R, Kochupillai N, Crock PA, Pituitary autoimmunity in patients with Sheehan’s syndrome: J Clin Endocrinol Metab, 2002; 87(9); 4137-41
9.. Stamatouli A, Bedoya P, Yavuz S, Hypothyroidism: Cardiovascular endpoints of thyroid hormone replacement: Front Endocrinol (Lausanne), 2019; 10; 888
10.. Chait A, Brunzell JD, Acquired hyperlipidemia (secondary dyslipoproteinemias): Endocrinol Metab Clin North Am, 1990; 19(2); 259-78
11.. Malik R, Hodgson H, The relationship between the thyroid gland and the liver: QJM, 2002; 95(9); 559-69
12.. Loria P, Carulli L, Bertolotti M, Lonardo A, Endocrine and liver interaction: The role of endocrine pathways in NASH: Nat Rev Gastroenterol Hepatol, 2009; 6(4); 236-47
13.. Ajala MO, Ogunro PS, Fasanmade OA, Relationship between liver function tests and thyroid hormones in thyroid disorders: Niger Postgrad Med J, 2013; 20(3); 188-92
14.. Bouznad N, Mghari GE, Hattaoui ME, Ansari NE, Atypical and rare cardiac revelation about Sheehan’s syndrome: A report of three cases]: Ann Cardiol Angeiol (Paris), 2017; 66(4); 239-42 [in Japanese]
15.. Reddy MS, Nahar A, Thippeswamy H, Kumar CS, Psychosis as a late manifestation of Sheehan’s syndrome: Asian J Psychiatr, 2017; 25; 228-30
16.. Elshimy G, Alghoula F: StatPearls [Internet], 2021, Treasure Island (FL), StatPearls Publishing https://www.ncbi.nlm.nih.gov/books/NBK499968/
Tables
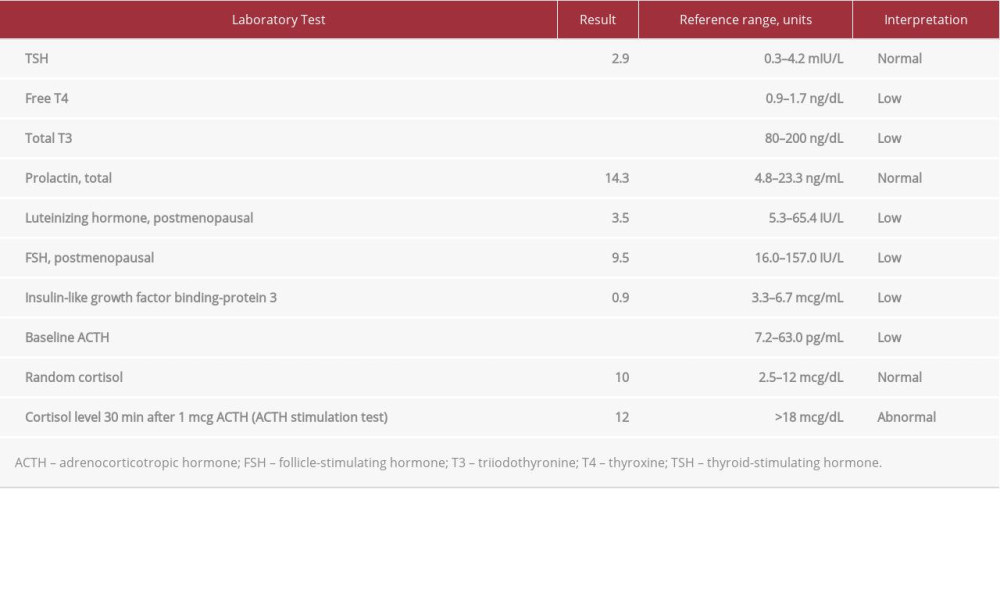 Table 1.. Results of endocrine evaluations.
Table 1.. Results of endocrine evaluations.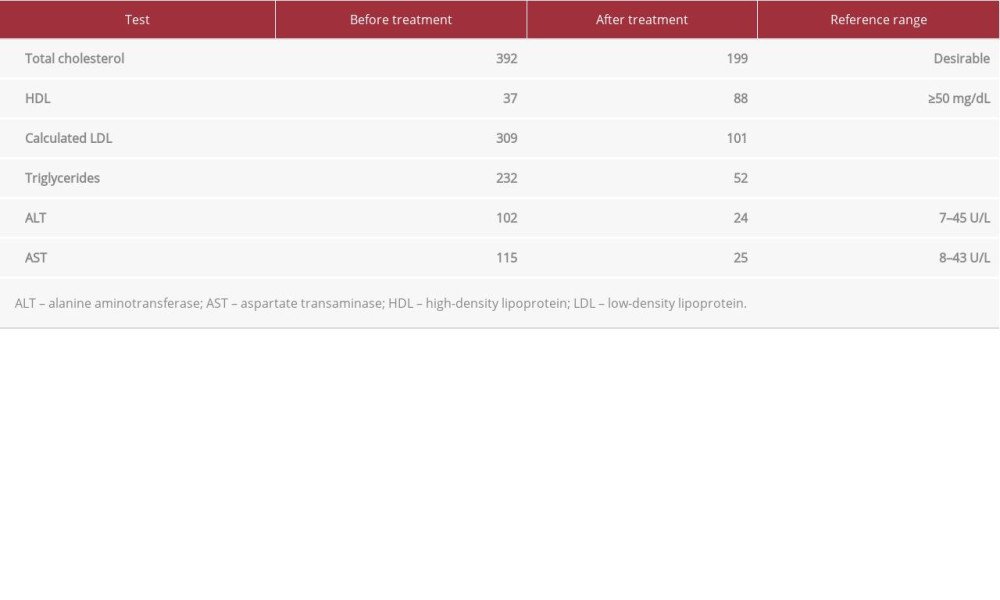 Table 2.. Results of lipid panel and liver enzyme levels before and 6 months after treatment of endocrine abnormalities.
Table 2.. Results of lipid panel and liver enzyme levels before and 6 months after treatment of endocrine abnormalities. Table 1.. Results of endocrine evaluations.
Table 1.. Results of endocrine evaluations. Table 2.. Results of lipid panel and liver enzyme levels before and 6 months after treatment of endocrine abnormalities.
Table 2.. Results of lipid panel and liver enzyme levels before and 6 months after treatment of endocrine abnormalities. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








