17 May 2021: Articles 
Anti-N-Methyl-D-Aspartate Receptor Encephalitis with Serum Anti-Thyroid Antibodies: A Case Report and Literature Review
Challenging differential diagnosis, Diagnostic / therapeutic accidents, Management of emergency care, Unexpected drug reaction, Rare disease, Educational Purpose (only if useful for a systematic review or synthesis)
Emilia Matera1ADEF*, Alessandra Gabellone1BF, Maria Giuseppina Petruzzelli2D, Lucia Marzulli1F, Flora Furente1DF, Lucia Margari1ADOI: 10.12659/AJCR.931104
Am J Case Rep 2021; 22:e931104
Abstract
BACKGROUND: Anti-N methyl D-aspartate receptor encephalitis (anti-NMDArE) is a disorder in which triggers such as infectious agents or neoplastic disease can lead to an autoimmune response against the nervous system, although this disorder is usually idiopathic. Some patients with anti-NMDArE have evidence of other autoimmune alterations. Here, we present a case of non-paraneoplastic anti-NMDArE with elevation of serum anti-thyroid antibodies and a literature review of this association.
CASE REPORT: A 16-year-old girl was admitted in the University Hospital of Bari for a new onset of tonic-clonic seizures. Progressively, the patient manifested also psychomotor agitation, language difficulties, memory impairment, psychotic symptoms, autonomic dysfunction, and psychomotor retardation. Blood evaluation revealed the presence of anti-thyroglobulin, anti-thyroperoxidase, and anti-NMDAr antibodies. Cerebrospinal fluid analysis confirmed the diagnosis of anti-NMDArE. No tumors were found. Treatment with intravenous immunoglobulin, steroids, and plasma exchange relieved symptoms and decreased levels of serum anti-NMDAr antibodies. After 12 months, the patient had full recovery of communicative capacity, with the persistence of slight difficulty of memory and mild tendency to irritability. Blood exams shown persistence of anti-NMDAr positivity and absence of anti-thyroid antibodies.
CONCLUSIONS: We report a rare case in which an autoimmune involvement of thyroid gland was concurrent with an anti-NMDArE. It would be useful for clinical practice to clarify whether the presence of anti-thyroid antibody an characterize the clinical course, prognosis, and response to treatment of the idiopathic type of anti-NMDArE.
Keywords: Thyroiditis, Anti-N-Methyl-D-Aspartate Receptor Encephalitis, Adolescent, Autoantibodies, Immunoglobulins, Intravenous, Receptors, N-Methyl-D-Aspartate, Seizures
Background
Anti-N-methyl-D-aspartate receptor encephalitis (anti-NMDArE), first described by Dr. Josep Dalmau and colleagues at the University of Pennsylvania in 2007 [1], is an autoimmune disorder with a wide spectrum of neuropsychiatric symptoms. This disorder usually occurs in young women [2–4] with a female-to-male ratio of approximately 4: 1 [5]. It is the second most common autoimmune encephalitis in children and adolescents following acute disseminated encephalomyelitis (ADEM) [6].
The NMDA receptor is ligand-gated cationic channel mainly located in the forebrain and hippocampus and activated by glutamate. It is involved in synaptic transmission and neuronal plasticity, and has a role in learning, judgment, perception of reality, memory, and autonomic functions [7]. In the anti-NMDArE, the immune system produces immunoglobulins, with the prevalence of G1 subclass, against the GluN1/NR1 subunit of the NMDA receptor [8,9].
These antibodies (Abs) are produced in response to an auto-immune reaction, but the cause of this process is not entirely understood. Previous infections from other agents, such as Herpes Simplex Virus (HSV), Epstein-Barr Virus (EBV) and neo-plastic disease with ectopic expression of neuronal proteins are thought to trigger a misdirected immune response against the nervous system [10]. The anti-NMDArE associated with a tumor is identified as a paraneoplastic encephalitis. The most common tumor associated with anti-NMDArE is ovarian teratoma [11], which is diagnosed in 6–50% of female patients with paraneoplastic encephalitis [12], while testicular germ cell tumors, lung cancer, thyroid cancer, breast cancer, colon tumors, mediastinal teratoma, neuroblastoma and Hodgkin’s lymphoma are less frequent [13–16]. Nevertheless, most cases of anti-NMDArE are idiopathic [7]. Possible risk factors for idiopathic anti-NMDArE are viral comorbidities, a family history for autoimmunity, and possible genetic and ethnic predisposition [10].
Several studies showed that patients with autoimmune encephalitis have contemporary evidence of other autoimmune alterations and syndromes (eg, anti-nuclear Abs (ANA), thyroid peroxidase (TPO) Abs, Graves’ disease, neuromyelitis optica, type I diabetes) [17–20], according to the hypothesis that an autoimmune disorder increases the risk of an additional autoimmune disorder [21]. Over the past decade, several authors have pointed out the coexistence of anti-thyroid (Thy) Abs in non-paraneoplastic anti-NMDArE [21], but the clinical and pathogenetic significance of this association needs to be further explored. In the context of this ongoing debate, we present the present case report of an adolescent girl affected by a non-paraneoplastic anti-NMDArE associated with positive anti-TPO and anti-thyroglobulin (TG) circulating Abs; then, we discuss this finding together with other case reports selected through a brief review of the literature on the association between anti-NMDArE and serum anti-Thy Abs.
Case Report
REVIEW OF ANTI-NMDARE WITH SERUM ANTI-THY ABS:
An electronic literature search was conducted for all articles published up to April 2020, with a range of databases searched including PubMed, Scopus, and Web of Science. The following combinations of keywords were used: “NMDAr/NMDA encephalitis”, “Thyroid”, “Thyroid Peroxidase/TPO”, “Thyroglobulin/ TG”. Research articles, case reports, and reviews in free full-text format and in English language were included.
We identified 35 records through the database search; after removing duplicates, there were 24 records. As inclusion criteria, papers needed to provide enough information about thyroid involvement in non-paraneoplastic anti-NMDArE cases, so 6 publications were selected for inclusion in this review.
Discussion
We described the case of an adolescent girl with a definite diagnosis of non-paraneoplastic anti-NMDArE and the coexistence of anti-TPO and anti-TG circulating Abs. The acute onset of epileptic seizures, psychotic symptoms, and abnormal speech and behavior and the progressive clinical worsening despite treatment with anti-epileptic and anti-psychotic drugs justified the Abs testing on CSF, confirming the diagnosis of anti-NMDArE. We observed good results with immunomodulatory therapy, with progressive improvement of clinical conditions and no episode of relapse over a 12-month follow-up.
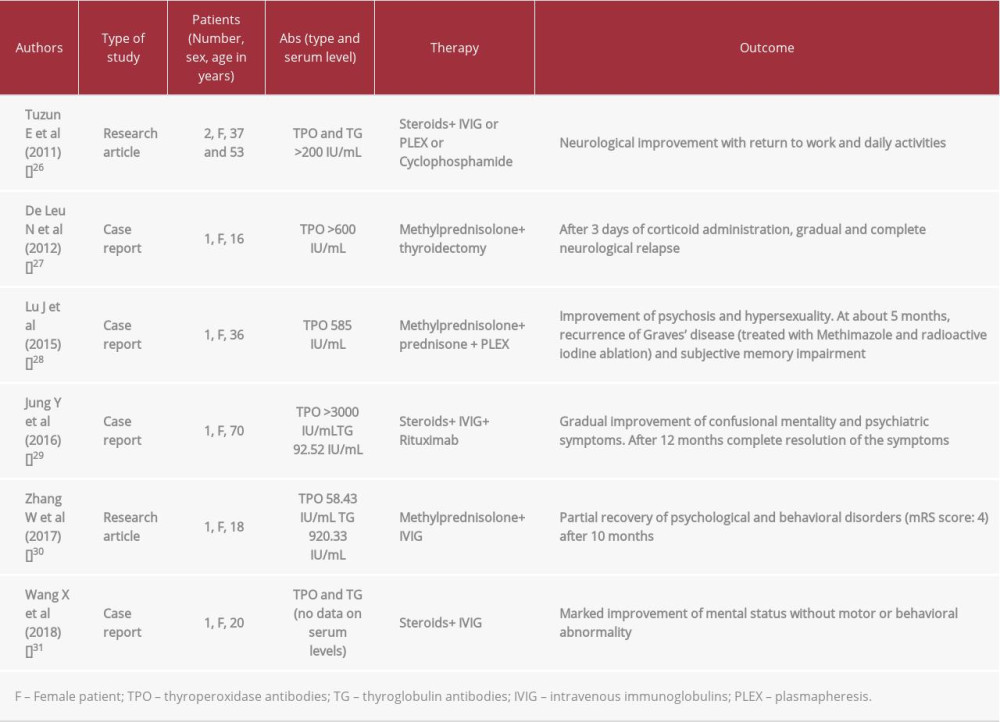
To our knowledge, this is one of the few cases reported in the literature of an autoimmune involvement of the thyroid gland concurrent with an anti-NMDArE. We know that Thy Abs are found in 10–12% of healthy populations [23], with different ranges according to age and sex [24], so the detection of anti-Thy Abs in patients with anti-NMDArE could be considered as an occasional finding. A recent retrospective cohort study of 517 patients with different types of antibody-positive auto-immune encephalitis (AE) showed that Hashimoto’s thyroiditis was the most commonly diagnosed autoimmune comorbidity, with a frequency of 5.42%, opposed to 1% in the general population [25]. This finding supported the hypothesis, previously suggested by Tuzun et al [26], that patients with Thy Abs are inclined to develop anti-neuronal-immune response and acute idiopathic encephalitis. A literature search of patients with the co-occurrence of anti-NMDArE and increased level of serum anti-Thy Abs is presented in Table 1 [26–31]. In particular, De Leu et al [27] and Lu J et al [28] described 2 patients with Graves’ disease; the remaining 5 patients had variable and different titers for Anti-Thy Abs, ranging from 58 IU/mL to 3000 IU/mL for TPO and from 92 IU/mL to 920 IU/mL for TG. In addition, our patient had a family history of Hashimoto’s thyroiditis.
It should be noted that each anti-NMDArE case considered was the non-paraneoplastic form, as was the case we described. Although anti-NMDArE is often categorized as a paraneoplastic syndrome, more frequently it is a non-paraneoplastic condition, especially in children [7]. The co-occurrence of both anti-NMDAr-Abs and Anti-TPO/Anti-TgG Abs in idiopathic forms of anti-NMDArE could suggest that T cell activation and the loss of immune self-tolerance, probably as a consequence of a complex interaction between genetic and environmental factors, could contribute to development of autoimmune disorders [25]. Juvenile age and female sex could be considered 2 adjunctive factors which increase the risk of auto-Abs production against both Thy and the brain.
Our patient and the cases listed in the table were young women, with a mean age of 33.2 years. The high frequency of anti-NMDArE and autoimmune thyroiditis reported in reproductive age woman suggested that sex hormones could act as factors increasing risk to develop both of these autoimmune disorders [7,32].
In addition, the pathogenetic role of anti-Thy Abs in AE, which has already been established for Hashimoto’s encephalitis (HE), should be considered. It would be better to classify HE as a probable AE [33], because the underlying pathogenetic mechanism of HE is currently not clear. In fact, the theory that self-Abs against neural antigens cross-reacts with Thy antigens as the pathogenetic basis of HE needs further investigation. The following pathogenetic mechanisms have been suggested: a) a shared target antigen between the thyroid gland and central nervous system; b) a neurotoxic effect of Thy hormones and Abs interference on neurotransmission; c) an effect of other Abs as enolases, dimethylargininase-I, aldehyde reductase-I, myelin-oligodendrocyte glycoprotein, gangliosides, and a few onco-neuronal antigens; and d) a consequence of vasculitic processes, primary demyelination, and immune complex-mediated processes [34]. Because of these considerations, we are not able to exclude a direct effect of anti-Thy Abs on the brain or a second autoimmune mechanism in some patients with presumed HE. According to the diagnostic criteria for AE, if anti-Thy Abs and anti-neuronal Abs exist simultaneously, AE should be diagnosed with priority. Otherwise, before diagnosing HE, anti-neuronal Abs should be detected to avoid misdiagnosis. In line with these considerations, the case we reported had a definite diagnosis of anti-NMDArE with associated detection of anti-Thy Abs of unclear significance. The hypothesis that the association between anti-NMDAr and anti-Thy Abs could be suggestive of a co-shared pathogenetic mechanism of autoimmune encephalitis needs more intensive investigation.
We know of no specific clinical phenotype to discriminate NMDArE with serum anti-Thy Abs from no-serum Thy Abs ones. Guan et al [35], studying the clinical NMDArE evolution in several female patients, explored the hypothesis that the presence of serum anti-Thy Abs and their titers could predict a shorter disease duration and a better treatment response [36–38]. Because very little is known about this topic, further studies are required to determine the utility of anti-Thy Abs titers predicting clinical manifestations, prognosis, and eventual relapses [39]. Anti-NMDArE is certainly a severe disease in which the prognosis remains obscure, but early diagnosis and intervention could reduce the incidence of complications and relapses.
Conclusions
The case we reported showed a classic presentation of anti-NMDArE, but with the presence of anti-Thy Abs. To date, the coexistence of anti-NMDAr Abs and anti-Thy Abs is still unclear. The detection of high titers of anti-TG and anti-TPO in an adolescent female with anti-NMDArE and a positive family history for Hashimoto’s thyroiditis we described, together with previous evidence reported by other authors, suggests the hypothesis that this association cannot be just occasional. Further studies about these mechanisms are needed to determine if anti-Thy Abs has a pathogenetic role in the context of idiopathic anti-NMDArE. Moreover, it would be useful for clinical practice to clarify, through longitudinal studies on a larger number of patients, whether the presence of anti-thyroid antibody can characterize the clinical course, prognosis, and response to treatment of the idiopathic type of anti-NMDArE.
References:
1.. Dalmau J, Tuzun E, Wu H, Paraneoplastic anti-N-methyl-D-aspar-tate receptor encephalitis associated with ovarian teratoma: Ann Neurol, 2007; 61(1); 25-36
2.. Dalmau J, Lancaster E, Martinez-Hernandez E, Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis: Lancet Neurol, 2011; 10(1); 63-74
3.. Florance NR, Davis RL, Lam C, Anti-N-methyl-D-aspartate receptor (NMDAR) encephalitis in children and adolescents: Ann Neurol, 2009; 66(1); 11-18
4.. Granerod J, Ambrose HE, Davies NWS, Causes of encephalitis and differences in their clinical presentations in England: A multicentre, population-based prospective study: Lancet Infect Dis, 2010; 10(12); 835-44
5.. Shi YC, Chen XJ, Zhang HM, Anti-N-methyl-D-aspartate receptor (NMDAR) encephalitis during pregnancy: Clinical analysis of reported cases: Taiwan J Obstet Gynecol, 2017; 56(3); 315-19
6.. Gurrera RJ, Recognizing psychiatric presentations of anti-NMDA receptor encephalitis in children and adolescents: A synthesis of published reports: Psychiatry Clin Neurosci, 2019; 73(5); 262-68
7.. Lazar-Molnar E, Tebo AE, Autoimmune NMDA receptor encephalitis: Clin Chim Acta, 2015; 438; 90-97
8.. Graus F, Titulaer MJ, Balu R, A clinical approach to diagnosis of auto-immune encephalitis: Lancet Neurol, 2016; 15(4); 391-404
9.. Dalmau J, Gleichman AJ, Hughes EG, Anti-NMDA-receptor encephalitis: Case series and analysis of the effects of antibodies: Lancet Neurol, 2008; 7(12); 1091-98
10.. Scheer S, John RM, Anti-N-methyl-D-aspartate receptor encephalitis in children and adolescents: J Pediatr Heal Care, 2016; 30(4); 347-58
11.. Leypoldt F, Titulaer MJ, Aguilar E, Clinical/Scientific Notes: Herpes simplex virus-1 encephalitis can trigger anti-nmda receptor encephalitis: Case report: Neurology, 2013; 81(18); 1637-39
12.. Armangue T, Titulaer MJ, Málaga I, Pediatric anti-N-methyl-D-aspar-tate receptor encephalitis – Clinical analysis and novel findings in a series of 20 patients: J Pediatr, 2013; 162(4); 850-56
13.. Dabner M, McCluggage WG, Bundell C, Ovarian teratoma associated with anti-n-methyl D-aspartate receptor encephalitis: A report of 5 cases documenting prominent intratumoral lymphoid infiltrates: Int J Gynecol Pathol, 2012; 31(5); 429-37
14.. Zandi MS, Irani SR, Follows G, Limbic encephalitis associated with antibodies to the nmda receptor in hodgkin lymphoma: Neurology, 2009; 73(23); 2039-40
15.. Padma S, Sundaram PS, Marmattom BV, PET/CT in the evaluation of anti-NMDA-receptor encephalitis: What we need to know as a NM physician: Indian J Nucl Med, 2011; 26(2); 99-101
16.. Eker A, Saka E, Dalmau J, Testicular teratoma and anti-N-methyl-D-aspartate receptor-associated encephalitis: J Neurol Neurosurg Psychiatry, 2008; 79(9); 1082-83
17.. Leypoldt F, Armangue T, Dalmau J, Autoimmune encephalopathies: Ann NY Acad Sci, 2015; 1338(1); 94-114
18.. Frunza-Stefan S, Whitlatch HB, Rao GG, Malek R, Unusual case of anti-Nmethyl-D-aspartic acid-receptor (NMDA-R) encephalitis and autoimmune polyglandular syndrome (APS): BMJ Case Rep, 2018; 2018; bcr2018224821
19.. Lai M, Hughes EG, Peng X, AMPA receptor antibodies in limbic encephalitis alter synaptic receptor location: Ann Neurol, 2009; 65(4); 424-34
20.. Lancaster E, Lai M, Peng X, Antibodies to the GABAB receptor in limbic encephalitis with seizures: case series and characterisation of the antigen: Lancet Neurol, 2010; 9(1); 67-76
21.. Khoodoruth MAS, Chut-kai Khoodoruth WN, Alshawwaf MKM, Anti-N-methyl-D-aspartate receptor encephalitis in a young female with sub-clinical hypothyroidism associated with anti-thyroid peroxidase and anti-thyroglobulin antibodies: A case report: SAGE Open Med Case Reports, 2020; 8; 2050313 X20949780
22.. Rankin J, Cerebral vascular accidents in patients over the age of 60. I. General considerations: Scott Med J, 1957; 2(4); 127-36
23.. Vanderpump MPJ, The epidemiology of thyroid disease: Br Med Bull, 2011; 99; 39-51
24.. Zöphel K, Saller B, Wunderlich G, Autoantibodies to thyroperoxidase (TPOAb) in a large population of euthyroid subjects: Implications for the definition of TPOAb reference intervals: Clin Lab, 2003; 49(11–12); 591-600
25.. Zhao J, Wang C, Xu X, Coexistence of autoimmune encephalitis and other systemic autoimmune diseases: Front Neurol, 2019; 10; 1142
26.. Tüzün E, Erdağ E, Durmuş H, Autoantibodies to neuronal surface antigens in thyroid antibody-positive and-negative limbic encephalitis: Neurol India, 2011; 59(1); 47-50
27.. De Leu N, Unuane D, Poppe K, Velkeniers B, Seizures and postictal stupor in a patient with uncontrolled Graves’ hyperthyroidism: BMJ Case Rep, 2012; 2012; bcr0220125929
28.. Lu J, Samson S, Kass J, Ram N, Acute psychosis in a pregnant patient with Graves’ hyperthyroidism and anti-NMDA receptor encephalitis: BMJ Case Rep, 2015; 2015; bcr2014208052
29.. Jung Y, Park S, Son H-J, Thyroid autoantibody positive anti-N-methyl-D-aspartate receptor encephalitis: Dement Neurocognitive Disord, 2016; 15(1); 24-27
30.. Zhang W, Yan L, Jiao J, Repeated misdiagnosis of a relapsed atypical anti-NMDA receptor encephalitis without an associated ovarian teratoma: Neurosci Lett, 2017; 638; 135-38
31.. Wang X, Lai Y, Li P, Zhou K, Che G, Massive idiopathic spontaneous hemothorax complicating anti-N-methyl-d-aspartate receptor encephalitis: A case report: Medicine (Baltimore), 2018; 97(45); e13188
32.. , Patologie al femminile/Malattie autoimmuni c2016 [cited 2016 Apr 21]. [in Italian]https://salute.gov.it/home/Argomenti-Patologiealfemminile/Malattieautoimmune
33.. Walikonis JE, Lennon VA, Radioimmunoassay for glutamic acid decarboxylase (GAD65) autoantibodies as a diagnostic aid for stiff-man syndrome and a correlate of susceptibility to type 1 diabetes mellitus: Mayo Clin Proc, 1998; 73(12); 1161-66
34.. Churilov LP, Sobolevskaia PA, Stroev YI, Thyroid gland and brain: Enigma of Hashimoto’s encephalopathy: Best Pract Res Clin Endocrinol Metab, 2019; 33(6); 101364
35.. Guan W, Fu Z, Zhang H, Non-tumor-associated anti-N-methyl-d-aspartate (NMDA) receptor encephalitis in Chinese girls with positive antithyroid antibodies: J Child Neurol, 2015; 30(12); 1582-85
36.. Schiess N, Pardo CA, Hashimoto’s encephalopathy: Ann NY Acad Sci, 2008; 1142; 254-65
37.. Chong JY, Rowland RDU, Hashimoto encephalopathy: Syndrome or myth?: Arch Neurol, 2003; 60(2); 164-71
38.. Litmeier S, Prüss H, Witsch E, Witsch J, Initial serum thyroid peroxidase antibodies and long-term outcomes in SREAT: Acta Neurol Scand, 2016; 134(6); 452-57
39.. Lee J, Yu HJ, Lee J, Hashimoto encephalopathy in pediatric patients: Homogeneity in clinical presentation and heterogeneity in antibody titers: Brain Dev, 2018; 40(1); 42-48
In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133