13 October 2021: Articles 
Epstein-Barr Virus Causing Clinical Jaundice and Acute Acalculous Cholecystitis in a Previously Healthy 17-Year-Old Girl
Challenging differential diagnosis, Rare coexistence of disease or pathology
Kevin G. Harvey1ABCDEFG*, Joshua G. Tice2BCDF, Adam Sigal1ACDEGDOI: 10.12659/AJCR.932285
Am J Case Rep 2021; 22:e932285
Abstract
BACKGROUND: Infectious mononucleosis secondary to Epstein-Barr Virus is a common infection in young adults. Infection usually involves a self-limiting course of fevers, sore throat, malaise, and myalgias. Transaminitis is a relatively common complication; clinical jaundice, however, is rare. This case report highlights an uncommon complication of Epstein-Barr Virus infection in which hepatocellular injury led to clinical jaundice as well as radiologic evidence of gallbladder pathology mimicking acute calculous cholecystitis.
CASE REPORT: A 17-year-old girl with no prior medical history presented to our Emergency Department 1 week after being diagnosed with infectious mononucleosis. She was hemodynamically stable and her physical exam was notable for scleral icterus with right upper quadrant tenderness and positive Murphy’s sign. Multiple imaging modalities performed showed gallbladder wall thickening without common bile duct dilatation. A hepatobiliary iminodiacetic acid (HIDA) scan showed evidence of hepatocyte dysfunction with normal gallbladder filling. The imaging results obtained in conjunction with her laboratory testing and active infectious mononucleosis infection confirmed the patient’s presentation was a result of her Epstein-Barr virus infection and did not require surgical intervention for cholecystectomy.
CONCLUSIONS: This case report highlights a rare complication of Epstein-Barr Virus infection and demonstrates the utility of interpreting hepatic function testing in conjunction with relevant imaging modalities in cases of clinical jaundice. By doing so, we were able to conclude the patient’s gallbladder pathology was related to acute acalculous cholecystitis (AAC) and did not warrant surgical intervention. The patient was given supportive care measures and made a full recovery.
Keywords: Epstein-Barr Virus Infections, Infectious Mononucleosis, Jaundice, Acalculous Cholecystitis, Adolescent, Cholecystitis, Acute, Female, Herpesvirus 4, Human, Humans, young adult
Background
Infectious mononucleosis secondary to Epstein-Barr Virus is a common infection in young adults. Infection usually involves a self-limiting course of fevers, sore throat, malaise, and myalgias. Lab abnormalities such as transaminitis can be a relatively common complication of infection, but clinical jaundice is rare. This case report describes an uncommon complication of Epstein-Barr Virus infection which resulted in hepatocellular injury and subsequent clinical jaundice as well as radiologic evidence of gallbladder pathology manifested as acute acalculous cholecystitis (AAC).
Case Report
A 17-year-old girl presented with 8 days of generalized abdominal pain, body aches, sore throat, and fatigue. She was in no acute distress, with a pulse of 103 bpm, BP 113/71 mmHg, RR 18, and T 36.6°C, with 97% O2 saturation on room air. Her physical exam revealed generalized abdominal discomfort with no focality, guarding, or rigidity. Specifically, her abdominal exam demonstrated a negative clinical Murphy’s sign and no tenderness at McBurney’s point. Relevant laboratory studies from this initial visit included an aspartate aminotransferase (AST) level of 105 IU/L (reference range 13–39 IU/L), ala-nine aminotransferase (ALT) level of 80 IU/L (reference range 7–52 IU/L), alkaline phosphatase level of 174 IU/L (reference range 38–126 IU/L), total bilirubin level of 4.8 mg/dL (reference range 0.3–1.0 mg/dL), and positive anti-nuclear and anti-capsid antigen IgM antibodies against Epstein-Barr virus. A complete blood count (CBC) did not show any evidence of leukocytosis or leukopenia, anemia, or thrombocytopenia. Her urine pregnancy test was negative and urinalysis showed trace levels of urine bilirubin. An abdominal ultrasound (US) was performed and showed mild splenomegaly. She was discharged home with supportive care and instructions to refrain from sports/physical contact for 6 weeks.
The patient returned to the Emergency Department 1 week later complaining of worsening abdominal pain, specifically in her right upper quadrant, as well as generalized itching and her “eyes turning yellow.” Her vital signs revealed a pulse of 117 bpm, BP 137/90 mmHg, RR 18, and T 36.8°C with 100% O2 saturation on room air. Her physical exam was notable for scleral icterus as well as right upper quadrant and left lower quadrant abdominal tenderness, including a positive clinical Murphy’s sign. Relevant laboratory studies during this subsequent encounter were significant for elevations in her hepatic function levels compared to her visit 1 week prior. During this second visit, the patient had an AST level of 169 IU/L, ALT level of 151IU/L, alkaline phosphatase level of 324 IU/L, and total bilirubin of 7.6 mg/dL. Her urine pregnancy test was again negative and urinalysis showed presence of bilirubin. The patient was admitted and additional laboratory tests were ordered, revealing an elevated gamma-glutamyl transferase (GGT) level of 214 IU/L (reference range 8–23 IU/L), lactate dehydrogenase (LDH) level of 534 IU/L (reference range 105–223 IU/L), and partial thromboplastin time (PTT) of 49.8 seconds (reference range 25–35 seconds). Her prothrombin time (PT) was normal at 12.5 seconds (reference 10–12.5 seconds) and her CBC did not reveal evidence of leukocytosis or leukopenia, anemia, or thrombocytopenia. A computed tomography (CT) scan of the abdomen and pelvis showed cholelithiasis with mild gall-bladder wall thickening and periportal edema within the liver (Figure 1). No hepatic lesions were noted. An abdominal ultra-sound (Figure 2) showed progressive splenomegaly as well as small cholelithiasis with gallbladder wall thickening of almost 4 mm (normal gallbladder wall thickness <3 mm) with common bile duct (CBD) diameter measuring 3mm (normal CBD diameter <4 mm). A magnetic resonance cholangiopancreatography (MRCP) showed periportal edema and fluid within the gallbladder fossa, which was thought to be more consistent with hepatocyte dysfunction than cholecystitis. The CBD was again non-dilated, consistent with the US findings. A hepatobiliary iminodiacetic acid (HIDA) scan was then performed on day 2 of admission and re-demonstrated the patient’s hepatocyte dysfunction with delayed hepatic clearance of tracer (Figure 3). There was no abnormal filling of the gallbladder noted, which would be seen in acute calculous cholecystitis. Further workup including human immunodeficiency virus (HIV) testing, viral hepatitis panels, and testing for diseases such as systemic lupus erythematosus (SLE) and alpha-1 antitrypsin deficiency were negative. The patient was observed with supportive care, including intravenous hydration and ursodiol for pruritus. Her transaminases and liver function tests began to trend downwards, and she was discharged home after a 3-day stay in the hospital. The patient had close follow-up with her primary care physician, and 3 months later was noted to have complete resolution of her symptoms and normal hepatic function test results.
Discussion
Epstein-Barr Virus, also known as EBV or HHV-4, is a member of the Herpesviridae family and is estimated to have infected over 90% of all people worldwide [1]. It is primarily transmitted via body fluids and although the symptoms of being infected may be unpleasant, it almost always involves a benign self-limiting course of body aches, sore throat, fatigue, and eventual recovery. Serious complications are rare, with the most common being upper airway obstruction (1–3.5%), splenic rupture (0.1–0.5%), and a wide range of lymphoproliferative cancers (accounting for roughly 1% of all cancers) [2,3].
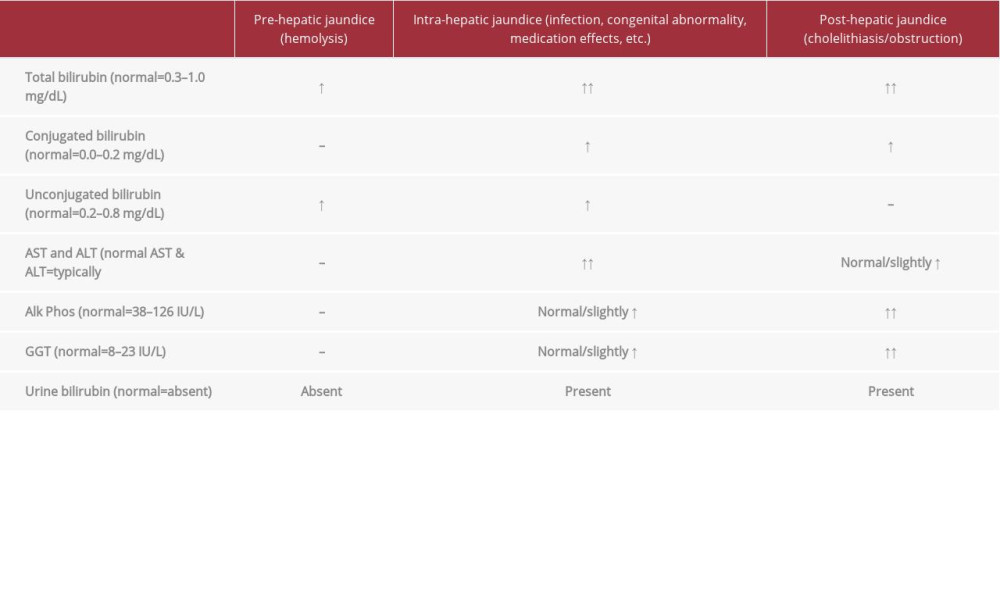
Transaminitis is relatively common in acute EBV infections, occurring in up to 80% of clinical presentations. However, clinical jaundice is rare and is present in only about 5% of infections [4]. There are 3 main types of jaundice: pre-hepatic, hepatocellular, and obstructive. Pre-hepatic jaundice usually involves predominantly elevated unconjugated bilirubin levels from some type of blood dyscrasia (such as hemolytic anemia), leading to hemolysis and subsequent increased bilirubin production. Hepatocellular jaundice typically has both elevated conjugated and unconjugated bilirubin levels and is the result of hepatic dysfunction such as from infection or medications. Post-hepatic or obstructive jaundice mainly involves an elevation in conjugated bilirubin levels and is due to faulty excretion of bile from the biliary tract, most commonly from a gallstone. The differences in laboratory values among these 3 types of jaundice are highlighted in Table 1. Our patient was noted to have a non-concerning complete blood count, with no evidence of hemolysis, making pre-hepatic jaundice unlikely and limiting the etiology of her jaundice to either hepato-cellular or obstructive in nature.
The HIDA scan is considered the most accurate imaging modality for the diagnosis of acute calculous cholecystitis, with a sensitivity of ~98% and specificity of ~95%, and was performed in this case to help determine the etiology of the patient’s gallbladder pathology and to subsequently rule-in or rule-out obstructive jaundice [5]. In this test, the patient is injected with a radiographic tracer labeled with technetium-99. The specific tracer used is normally metabolized by the liver and excreted in the bile. Photographs are intermittently taken after tracer injection with a scintillation camera to track the clearance of tracer. In cases of biliary obstruction, most commonly seen in acute calculous cholecystitis, we would expect there to be no filling of the gallbladder with tracer visualization in the CBD (representing an obstructing gallstone in the CBD). A gallbladder ejection fraction is also able to be calculated from the transit time of the tracer via the pictures taken; a value <35% is considered diagnostic for primary gallbladder disease. In our patient’s HIDA scan, there was no abnormal filling of the gallbladder, but there was delayed hepatic clearance of tracer. She was also noted to have a normal gallbladder ejection fraction above 35%. Given her findings of normal gallbladder filling with tracer and normal gallbladder ejection fraction, this made acute calculous cholecystitis an unlikely diagnosis, meaning her jaundice was likely due to hepatocellular injury as opposed to obstructive jaundice. Furthermore, the evidence of delayed hepatic clearing of tracer with normal visualization of the gallbladder helped confirm the hypothesis that her gall-bladder injury was in fact due to hepatocellular dysfunction as a result of her EBV infection.
This important distinction between hepatocellular dysfunction and an obstructive etiology influenced the decision to pursue a conservative management approach, although the clinical setting mimicked an acute surgical abdomen. The constellation of right upper quadrant abdominal pain with congruent tenderness, abnormal liver function tests, and cholelithiasis with gall bladder wall thickening on US is consistent with typical acute calculous cholecystitis. Transaminitis and elevations in unconjugated and conjugated bilirubin as well as alkaline phosphatase are seen in both hepatocellular and obstructive jaundice. The absence of CBD dilatation or obstruction on US and MRCP in conjunction with normal gallbladder visualization and hepatocyte dysfunction on HIDA scan helped rule-out biliary obstruction and subsequently confirm the hepatocellular etiology of the patient’s gallbladder pathology and jaundice.
Although our patient did not have acute calculous cholecystitis, she did have some type of gallbladder pathology, as evidenced by gallbladder wall thickening on her ultrasound and MRCP. Acute acalculous cholecystitis (AAC) occurs in up to 10% of cases of acute cholecystitis and can have multiple potential etiologies, such as severe infection or sepsis, trauma, surgery, or systemic diseases. As indicated by its name, AAC has no physical obstructing etiology, or calculous, causing cholecystitis. Treating the underlying illness or disease process that led to the development of AAC is seen as the best therapy in addressing this type of cholecystitis. The first reported case in Scandinavia of EBV infection complicated by AAC was described by Agergaard et al in a 34-year-old woman who also initially presented with symptoms typical of infectious mononucleosis and tested positive for EBV antibodies [6]. Their patient was found to have abnormal hepatic function testing, similar to our patient, and also underwent abdominal US, which showed evidence of acute cholecystitis with gallbladder wall thickening, but no cholelithiasis. She was thought to have AAC secondary to EBV infection. She was given antibiotics for a suspected gastroenteritis and pneumonia and made a full recovery with normalization of hepatic function testing and no surgical intervention. Agergaard et al performed a literature review of 26 cases of AAC and found no difference in clinical course between patients who received antibiotics and those who did not. Only 1 patient required surgery. We present a case similar to theirs in a younger female patient and also demonstrate how additional testing such as HIDA scanning can further aid in the potentially difficult diagnosis.
Conclusions
This case highlights an atypical complication of EBV infection and subsequently an atypical presentation of jaundice. In the presence of active EBV infection, elevations in liver function tests should prompt the physician to consider viral-induced hepatocellular injury. This hepatocellular injury can lead to gall-bladder pathology, causing acute acalculous cholecystitis and mimicking a surgical abdomen. Recognition and awareness of this by the bedside clinician as well as the surgeon can aid in the diagnosis and may avoid an unnecessary surgery.
Figures
References:
1.. Smatti MK, Al-Sadeq DW, Ali NH, Pintus G, Epstein-Barr virus epidemiology, serology, and genetic variability of LMP-1 oncogene among healthy population: An update: Front Oncol, 2018; 8; 211
2.. Fugl A, Andersen CL, Epstein-Barr virus and its association with disease – a review of relevance to general practice: BMC Fam Pract, 2019; 20; 62
3.. Bakkalci D, Jia Y, Winter JR, Risk factors for Epstein Barr virus-associated cancers: A systematic review, critical appraisal, and mapping of the epidemiological evidence: J Glob Health, 2020; 10(1); 010405
4.. Herold J, Grimaldo F, Epstein-Barr virus-induced jaundice: Clin Pract Cases Emerg Med, 2020; 4(1); 69-71
5.. Weismann HS, Frank MS, Bernstein LH, Freeman LM, Rapid and accurate diagnosis of acute cholecystitis with 99mTc-HIDA cholescintigraphy: Am J Roentgenol, 1979; 132(4); 523-28
6.. Agergaard J, Larsen CS, Acute acalculous cholecystitis in a patient with primary Epstein-Barr virus infection: A case report and literature review: Int J Infect Dis, 2015; 35; 67-72
Figures
In Press
14 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.942770
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943214
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943010
16 Mar 2024 : Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.943687
Most Viewed Current Articles
07 Mar 2024 : Case report 
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133
10 Jan 2022 : Case report 
DOI :10.12659/AJCR.935263
Am J Case Rep 2022; 23:e935263
19 Jul 2022 : Case report 
DOI :10.12659/AJCR.936128
Am J Case Rep 2022; 23:e936128
23 Feb 2022 : Case report 
DOI :10.12659/AJCR.935250
Am J Case Rep 2022; 23:e935250