18 August 2022: Articles 
Post-COVID-19 Secondary Sclerosing Cholangitis: A Rare but Severe Condition with no Treatment Besides Liver Transplantation
Challenging differential diagnosis, Unusual setting of medical care, Rare disease
Marcel Cerqueira Cesar Machado1ABEF*, Roberto Kalil Filho2E, Ibrahim Ahmad Hussein el Bacha3BF, Irai Santana de Oliveira4CD, Cristiane Maria de Freitas Ribeiro5CD, Heraldo Possolo de Souza1DE, Edson Roberto Parise6CDDOI: 10.12659/AJCR.936250
Am J Case Rep 2022; 23:e936250
Abstract
BACKGROUND: The incidence of abnormal liver function, mainly aspartate aminotransferase and alanine aminotransferase elevations, in patients with COVID-19 is not uncommon, but persistent liver damage after the acute phase of the disease is uncommon and has been recently recognized as a new entity named post-COVID-19 cholangiopathy.
CASE REPORT: We report a clinical case with progressive cholestatic disease following severe COVID-19. AST and ALT peaked at hospital admission and while its serum concentration went down, bilirubin and cholestatic liver enzymes started to increase, reaching the maximum at day 122. Magnetic resonance imaging (MRI) revealed a diffuse irregularity of intra- and extrahepatic bile ducts, with multiple focal strictures alternating with mild focal dilations of the biliary tree, suggesting a sclerosing cholangiopathy. A transjugular liver biopsy showed a prominent bile ductular reaction, cholangiocyte injury, inflammatory infiltrate rich in neutrophils, biliary infarctions, marked cholestasis, and portal fibrosis, suggesting the diagnosis of post-Covid-19 secondary sclerosing cholangitis. The patient evolved with a continuous deterioration of liver functions, but liver transplantation was not performed due to his poor clinical condition.
CONCLUSIONS: Post-COVID-19 SSC is a severe disease with no effective clinical treatment and has liver transplantation as the only treatment for a few selected patients.
Keywords: Adult Multisystem Inflammatory Disease, Cholangitis, Sclerosing, Cholestasis, Intrahepatic, COVID-19 Related, Bile Ducts, Extrahepatic, COVID-19, Humans, Liver, Liver Transplantation
Background
The incidence of abnormal liver tests in patients with COVID-19 ranges from 14% to 76% [1,2]. However, persistent liver damage after the acute phase of the disease is uncommon and has recently been recognized as a new entity [3]. Liver disease usually seen in COVID-19 patients is related to hepatocellular damage, associated with elevation of aspartate aminotransferase (AST) and alanine aminotransferase (ALT). Nevertheless, the elevation of canalicular enzymes and bilirubin occurs in 12% of cases [1,4].
Moreover, a relationship between liver damage and disease severity has recently been observed [5]. In most of these cases, serum liver enzyme levels are within 1–2 times the upper limit of normal and regress to normal values with healing of the disease [1–3]. However, prolonged and severe cholestasis during recovery from severe COVID-19 is observed in some cases, and it is considered a novel entity, named post-COVID cholangiopathy [3], which may be severe enough to be treated by liver transplantation [6]. Here, we report a clinical case of progressive cholestatic disease following severe COVID-19.
Case Report
PATHOLOGICAL FINDINGS: LIVER BIOPSY:
A liver biopsy showed a prominent bile ductular reaction, cholangiocyte injury, inflammatory infiltrate rich in neutrophils, biliary infarctions, marked cholestasis, and portal fibrosis. The biopsy demonstrated a degenerative cholangiocyte injury with extreme cholangiocyte cytoplasmic vacuolization and degenerative changes (Figures 2–4).
Discussion
Secondary sclerosing cholangitis in critically ill patients (SSCCIP) has been reported in patients treated in an intensive care unit with hemodynamic instability due to infection, trauma, burns, and even cardiothoracic surgery [7]; however, the precise mechanism of this disease remains unknown. A combination of ductal ischemia, biliary infection, and bile composition alterations may interact to trigger the process [8,9].
Biliary duct ischemia seems to play a critical role in this process. It is known that biliary ducts receive their blood supply solely from branches of the hepatic artery; therefore, they are more susceptible to ischemia than hepatocytes that receive double blood supply from the portal vein and hepatic artery. Biliary duct ischemia damages the biliary epithelium with necrosis and biliary cast formation, as observed in the present case (Figure 1) [8,10]. Bile duct damage with loss of connection to the central bile duct resulting in excluded bile ducts can make antibiotics ineffective, with prolonged sepsis and abscess formation, with high mortality [8].
Although this condition was initially related to long-term treatment in the intensive care unit, it seems that even a short-term stay in an intensive care unit can induce biliary duct damage [7]. Alterations in gamma-glutamyl transpeptidase (GGT) were the predominant enzyme abnormality, which occurs earlier and is more intense than changes in alkaline phosphatase (ALP). Hyperbilirubinemia occurred in later stages, as observed in the case presented here. These findings are not specific, but they are helpful in distinguishing this condition from other diseases, such as septicemia-associated cholestasis, when hyperbilirubinemia is an earlier and predominant event [11,12]. Rapid and extensive biliary duct destruction explains the intense fibrotic response and the need for liver transplantation.
Post-COVID-19 cholangiopathy is a special entity of liver injury that has been suggested as a variant of secondary sclerosing cholangitis in critically ill patients (SSC-CIP), but with unique histologic features [4]. This new entity was reported in patients recovering from a severe disease treated in intensive care units with vasopressor drugs, mechanical ventilation, and positive end-respiratory pressure, which increases the possibility of microcirculatory ischemia in the hepato-splanchnic vascular plexus [12]. Increased proinflammatory cytokine levels also contribute to cholangiocyte damage [7]. Prolonged prone positioning frequently used in COVID-19 patients also seems to increase the risk of SSC-CIP [13]. Biliary epithelium ulceration and hemorrhagic exudates in the bile ducts were also observed [9]. In the present case, we also observed intraductal bleeding with cast formation that induced retrograde chol-angiography exploration.
In the present case, it should be mentioned that, although the patient was chronically addicted to alcohol, no signs of chronic liver disease were detected on admission ultrasound or even in liver the biopsy, which also did not show histological signs of alcoholic hepatitis. The progression of cholestatic disease occurred later in during his hospital stay. AST and ALT peaked at hospital admission, and while serum concentrations decreased, bilirubin and cholestatic liver enzymes started to increase, reaching a maximum on day 122 of his hospital stay. This biphasic pattern with initial transaminase elevations followed by cholestatic liver enzymes could reflect systemic inflammatory response syndrome (SIRS)-induced cholestasis at the hepatocellular/canalicular level or more severe bile duct injury in the later stage of the disease [14].
In contrast to the histological findings from autopsy of patients dying from COVID-19 with mild and focal lobular cholestasis with no derangement in bile ducts [15], our patient’s liver specimen showed extensive ductular reaction and degenerative cholangiocyte injury with biliary ductular proliferation accompanied by neutrophils and portal fibrosis.
These histologic changes were described in direct hepatic injury from COVID-19 in critically ill patients with underlying secondary sclerosing cholangitis, although no clear signs of intrahepatic microangiopathy were found, which could be due to the fact that the liver specimen was obtained via transjugular needle biopsy [6].
Conclusions
Most patients with SSC-CIP present with irreversible and progressive liver disease, which requires liver transplantation [15]. Recently, it was reported that the first liver transplantation in a patient with post-COVID-19 SSC-CIP was performed [6], which may be followed by several cases in the future. In conclusion, post-COVID-19 SSC-CIP is a severe disease that usually has no effective clinical treatment, and liver transplantation in selected patients is the only treatment at the present time.
Figures
References:
1.. Cai Q, Huang D, Yu H, COVID-19: Abnormal liver function tests: J Hepatol, 2020; 73; 566-74
2.. Brandão Neto RA, Marchini JF, Marino LO, Mortality and other outcomes of patients with coronavirus disease pneumonia admitted to the emergency department: A prospective observational Brazilian study: PLoS One, 2021; 16; e0244532
3.. Roth NC, Kim A, Vitkovski T, Post-COVID-19 cholangiopathy: A novel entity: Am J Gastroenterol, 2021; 116; 1077-82
4.. Fix OK, Hameed B, Fontana RJ, Clinical best practice advice for hepatology and liver transplant providers during the COVID-19 pandemic: AASLD Expert Panel Consensus Statement: Hepatol Baltim Md, 2020; 72; 287-304
5.. Hundt MA, Deng Y, Ciarleglio MM, Abnormal liver tests in COVID-19: A retrospective observational cohort study of 1,827 patients in a Major U.S. Hospital Network: Hepatology, 2020; 72; 1169-76
6.. Durazo FA, Nicholas AA, Mahaffey JJ, Post-COVID-19 cholangiopathy – a new indication for liver transplantation: A case report: Transplant Proc, 2021; 53; 1132-37
7.. Leonhardt S, Veltzke-Schlieker W, Adler A, Secondary sclerosing cholangitis in critically ill patients: Clinical presentation, cholangiographic features, natural history, and outcome: a series of 16 cases: Medicine (Baltimore), 2015; 94; e2188
8.. Leonhardt S, Veltzke-Schlieker W, Adler A, Trigger mechanisms of secondary sclerosing cholangitis in critically ill patients: Crit Care Lond Engl, 2015; 19; 131
9.. Laurent L, Lemaitre C, Minello A, Cholangiopathy in critically ill patients surviving beyond the intensive care period: A multicentre survey in liver units: Aliment Pharmacol Ther, 2017; 46; 1070-76
10.. Gelbmann CM, Rümmele P, Wimmer M, Ischemic-like cholangiopathy with secondary sclerosing cholangitis in critically ill patients: Am J Gastroenterol, 2007; 102; 1221-29
11.. Chand N, Sanyal AJ, Sepsis-induced cholestasis: Hepatol Baltim Md, 2007; 45; 230-41
12.. Talwalkar JA, Lindor KD, Primary biliary cirrhosis: Lancet Lond Engl, 2003; 362; 53-61
13.. Weig T, Schubert MI, Gruener N, Abdominal obesity and prolonged prone positioning increase risk of developing sclerosing cholangitis in critically ill patients with influenza A-associated ARDS: Eur J Med Res, 2012; 17; 30
14.. Edwards K, Allison M, Ghuman S, Secondary sclerosing cholangitis in critically ill patients: A rare disease precipitated by severe SARS-CoV-2 infection: BMJ Case Rep, 2020; 13; e237984
15.. Kirchner GI, Rümmele P, Update on sclerosing cholangitis in critically ill patients: Viszeralmedizin, 2015; 31; 178-84
Figures
Tables
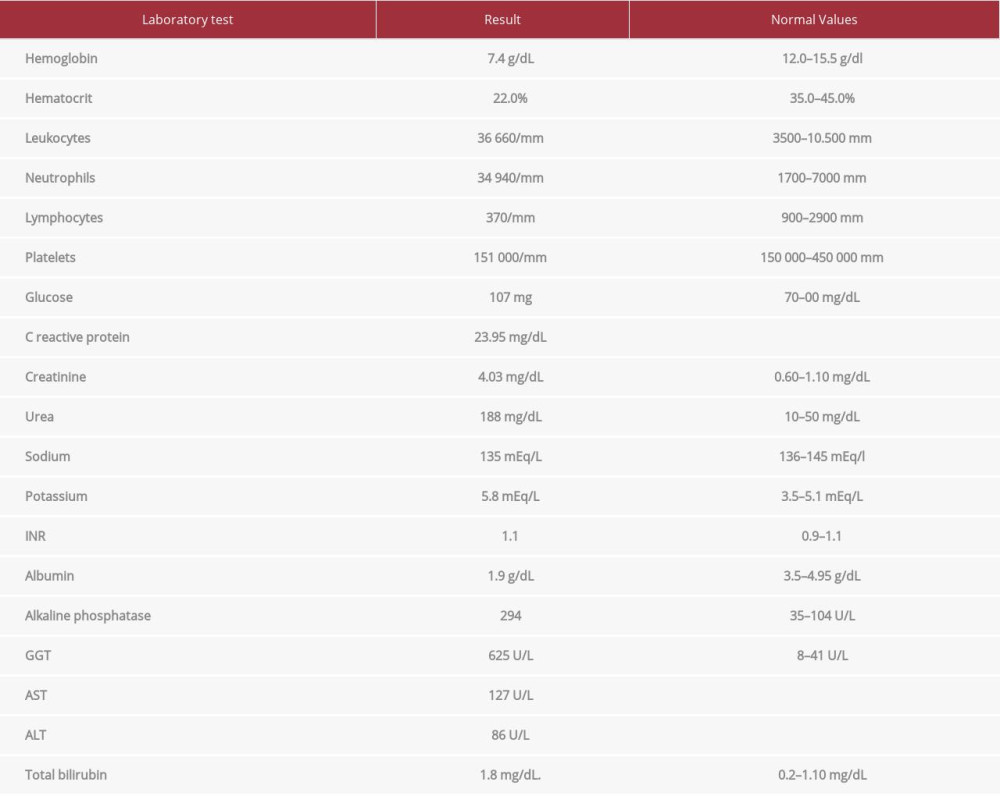 Table 1.. Laboratory tests at hospital admission.
Table 1.. Laboratory tests at hospital admission.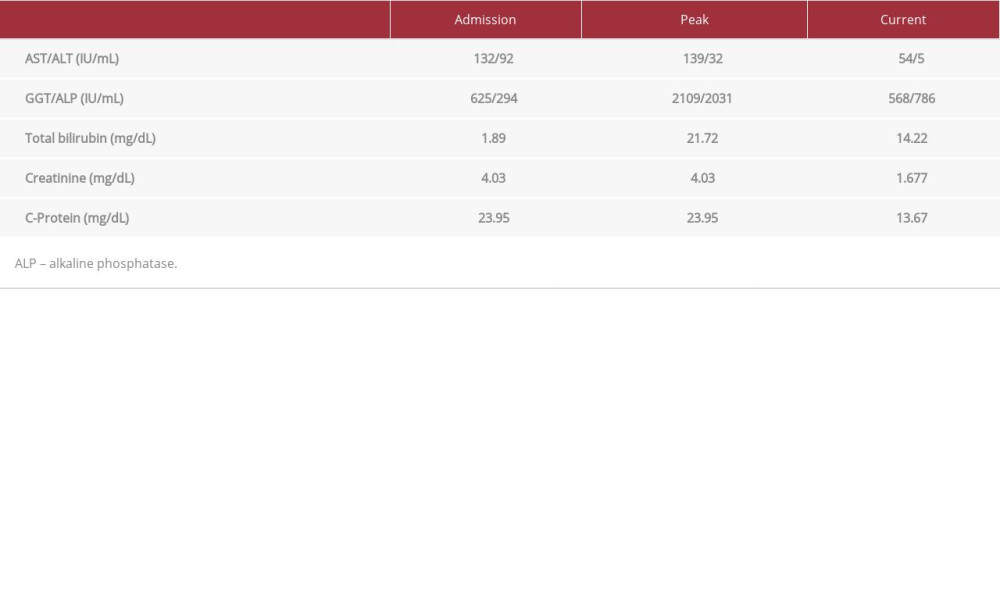 Table 2.. Laboratory tests during hospital evolution. Data obtained at hospital admission. Peak values and current data for these biochemical evaluations.
Table 2.. Laboratory tests during hospital evolution. Data obtained at hospital admission. Peak values and current data for these biochemical evaluations. Table 1.. Laboratory tests at hospital admission.
Table 1.. Laboratory tests at hospital admission. Table 2.. Laboratory tests during hospital evolution. Data obtained at hospital admission. Peak values and current data for these biochemical evaluations.
Table 2.. Laboratory tests during hospital evolution. Data obtained at hospital admission. Peak values and current data for these biochemical evaluations. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








