04 April 2022: Articles 
Management of an Extensive Intraparotid and Auricular Arteriovenous Malformation
Rare disease
Sze Ying Yee1EF*, Shuyi Guo1E, Chi Long Ho123EFDOI: 10.12659/AJCR.935337
Am J Case Rep 2022; 23:e935337
Abstract
BACKGROUND: Extracranial arteriovenous malformations (AVMs) of the parotid gland and auricle are rarely encountered. Management of these AVMs depends on the Schobinger stage and their flow characteristics. We present a rare case of an AVM involving the parotid and auricle concurrently. The clinical and imaging features of these high-flow vascular malformations and their treatment options are discussed and we provide a review of the literature.
CASE REPORT: A 40-year-old woman presented with a large 6.4×6.0×13.0 cm high-flow Schobinger stage II high-flow AVM of the parotid gland and auricle. Diagnostic imaging included magnetic resonance imaging (MRI) and conventional catheter angiogram, which defined the vascular anatomy and flow characteristics of the AVM. She was treated with preoperative endovascular embolization followed by surgical excision and free-tissue transfer reconstruction on the next day. The results were excellent, with no recurrence over 3.5 years of follow-up.
CONCLUSIONS: This is the second case reported in the literature of high-flow AVM concurrently involving the parotid gland and auricle, treated with perioperative embolization followed by surgical excision and grafting. Management of AVMs requires a multidisciplinary team approach and understanding of the natural history of the lesion. Although total surgical resection is the criterion standard for these AVMs, endovascular embolization is an alternative treatment that can be used as an adjunct to surgery. Furthermore, perioperative embolization can decrease the vascularity of the lesion and effectively reduce blood loss during AVM surgery.
Keywords: Arteriovenous Malformations, Ear Auricle, Embolization, Therapeutic, endovascular procedures, Adult, Angiography, Female, Humans, vascular malformations
Background
According to the International Society for Study of Vascular Anomalies (ISSVA), vascular anomalies can be categorized into vascular tumors and malformations [1]. Vascular tumors are soft-tissue growths that can be either benign or malignant, formed from blood vessels or lymph vessels (eg, hemangioendotheliomas, Kaposi’s sarcomas, and angiosarcoma) [1]. Vascular malformations are congenital vascular anomalies due to developmental error. They are further classified according to their vascular flow characteristics into low-flow (eg, hemangiomas, capillary, venous, and lymphatic malformations) and high-flow lesions, including arteriovenous malformation (AVM) and arteriovenous fistula (AVF) [1]. The fistulas are functionally-open embryological residues between the arteries and veins and are present at birth. Local trauma, partial surgery, psychological stress, and endocrine events (eg, puberty, pregnancy, and birth) can cause the fistulas to grow and form malformations [2].
The extracranial AVMs are classified according to Schobinger (Table 1) into 4 stages according to the patient’s symptoms: stage I (warm and discolored skin), II (pulsation, thrill, and swelling), III (pain, dystrophic skin, ulceration, bleeding), and IV (decompensation). These AVM can be further differentiated according to their flow rates into fast-flowing and slow-flowing types [4]. Fast-flowing in an existing vascular malformation can induce arteriovenous shunting, increasing flow demand and cascading enlargement of the malformation [5]. Early intervention can arrest or even reverse such changes [5]. Stage I AVMs are usually just observed, while stage II may need intervention based on symptoms and location; stage III and IV often require intervention [3].
AVMs of the parotid and auricle are rare malformations and are exceedingly rare when they occur concurrently in the same individual. Here, we report an exceedingly rare case of a Schobinger stage II fast-flowing AVM of the parotid gland and the left auricle, which were treated by endovascular embolization and surgical resection. The clinical and imaging features of these high-flow vascular malformations and their treatment options are discussed and we provide a review of the pertinent literature.
Case Report
A 40-year-old woman presented with progressive swelling on the left side of the neck for more than 6 months. She has no significant past medical history. Physical findings showed a swelling over the left parotid gland and auricle, with skin discoloration. There was a palpable thrill and vascular murmur detected on auscultation. Magnetic resonance imaging (MRI) showed serpiginous vessels with “honeycomb” flow voids in the left parotid gland and the left auricle, indicating a large high-flow AVM (Figure 1). The large AVM measured approximately 6.4×6.0×13.0 cm (anteroposterior×transverse×craniocaudal dimensions). The presenting signs and symptoms of the patient correlated with the Schobinger stage II AVM. The AVM was primarily supplied by branches of the external carotid artery and drained into the external jugular vein (Figure 1). Preoperative embolization was performed with vascular access via the right femoral artery and insertion of a guiding catheter in the left external carotid artery. A conventional catheter angiogram showed a dilated intranidal aneurysm within the left parotid AVM with the main blood supply from the posterior auricular and superficial temporal branches of the left external carotid artery (Figure 2). A high-flow shunt with venous drainage into the dilated left external jugular vein was identified. Blood flow control was achieved using the proximal balloon occlusion technique. Coil embolization of the feeding arteries and shunts was performed under general anesthesia. As a result, there was a significant reduction in the vascularity of the AVM. The patient underwent surgical excision of the AVM on the next day, including left total parotidectomy and left total auriculectomy. Careful dissection allowed for retrograde identification and preservation of the left facial nerve with branches. There was further extension of the dissection down into the neck, allowing for surgical closure with a musculocutaneous flap with end-to-end vessel anastomosis. The postoperative course was uneventful, with no complications related to either the preoperative embolization or surgery. No facial palsy was detected. Histology confirmed an AVM of the parotid gland and auricular subcutaneous tissue with no evidence of atypical cells or malignancy. The patient was discharged on the fifth postoperative day. Follow-up MRI at 6 months after surgery showed no remnant or recurrent AVM (Figure 3). There was no clinical or radiological evidence of AVM recurrence over 3.5 years of follow-up after surgery.
Discussion
PATHOPHYSIOLOGY OF AVM:
Enlargement of AVM can be caused by increased blood flow secondary to collateralization, dilatation, and thickening of adjacent vessels [3]. Latent arteriovenous (AV) shunts can open and stimulate hypertrophy of surrounding vessels and even cause aneurysm formation, which further increases the size of the AVM [30]. Expansion of AVMs can be due to angiogenesis (growth of new blood vessels from pre-existing vasculature) or vasculogenesis (de novo formation of new vasculature) [3]. There are endothelial proliferation and elevated vascular endothelial growth factor (VEGF) in AVM tissue [31]. Increased tissue VEGF expression correlates with AVM recurrence [31]. Endothelial cells of AVMs can express high levels of VEG, which results in proliferation and rapid migration of cells, forming anomalous vascular channels [32]. Matrix metalloproteinases (MMPs) are elevated in AVM; conversely, MMPs inhibitors control the progression of MMPs by reducing their expression [33].
Another stimulus for AVM expansion is tissue hypoxia or ischemia, a potent stimulator of angiogenesis, particularly after proximal arterial ligation or trauma [8]. Increased blood flow caused by AV shunting can promote angiogenesis and stimulate VEGF production and endothelial proliferation [34]. There is a higher risk of AVM progression in puberty due to increased hormonal activity during this period, thus stimulating AVM growth by promoting angiogenesis [35]. Estrogen and testosterone stimulate VEGF production, endothelial proliferation, and angiogenesis [36], while growth hormone has pro-angiogenic activity [37].
In adults, the diagnosis of AVM is often made around the fourth decade of life, with a female predominance [4]. Pregnancy, like puberty, is thought to increase the risk of AVM expansion [2]. Approximately 60% of AVMs occur in the superficial lobe of the parotid gland, 20% in the deep lobe, and 20% within the masseter muscle, with no dominant side [4,29].
The most common clinical manifestation of the AVM is the presence of a pulsatile mass [29].
MRI and conventional angiogram are the preferred imaging modalities for diagnosis and surveillance of vascular malformations. These imaging modalities are paramount for understanding both the extent of the disease and the flow characteristics [20]. Typical MRI features of AVM includes “bag of worms” or “honeycomb” flow voids of the serpiginous vessels (Figure 1). Unlike the presence of a nidus in intracranial AVM, blood is shunted directly from the arteries into venous tributaries. The veins become engorged over time, resulting in skin ulceration and necrosis [4]. The blood-shunting effects of AVM can cause high-output heart failure (Schobinger stage IV) [28].
TREATMENT OPTIONS:
Management of these AVMs can be challenging and is best achieved by understanding the natural history of the lesion and the patient’s needs. Treatment is performed not only for aesthetic purposes but also to avoid complications such as skin ulceration/necrosis and post-traumatic hemorrhage [28]. The primary goal is to restore and preserve function, stop bleeding, and improve or restore cosmesis [5]. Total AVM excision is the criterion standard treatment because it allows a definitive diagnosis with histological confirmation [5]. There is little role for radiation therapy in the treatment of parotid and auricular AVMs [5]. The extent of the parotidectomy depends on the extent of involvement of the gland. The risks of surgery include neurovascular injuries, particularly involving the facial nerve.
Endovascular embolization is an adjunct or alternative treatment. By reducing the vascularity of the AVM, blood loss can be limited, and safe tissue planes can be identified during surgery, thus facilitating AVM excision. The selection of an embolization agent depends on the type of lesion, method of embolization, and the experience of the interventional radiologist [4]. Detachable balloons, coils, and embolic agents are some of the commonly used agents [29]. The use of embolic agents is, however, not advisable for high-flow AVMs, as migration of embolic agents in high-flow shunts can increase the risk of pulmonary embolism [28], and platinum coils can be employed in such cases [28]. Microcatheters can be placed distal to the shunt during the procedure, and blood flow within the feeding vessel can be controlled with a balloon-tip catheter. Platinum coils can then be used to occlude the feeding arteries and the AV shunts [4]. Accurate identification of these shunts is crucial during the procedure. Although less invasive than surgery, endovascular treatment may not completely occlude the AVM in a single attempt, and multiple attempts may be required [4].
Among the 82 patients reported with auricular AVMs (Table 2), the majority underwent endovascular embolization (37 patients) and embolization followed by excision (25 patients), while the minority were treated with excision (8 patients) and some had only observation without intervention (12 patients) [5–22]. Incomplete devascularization of the auricular AVMs has been reported in 16 patients (43%) following embolization [13,14]. There was no recurrence or re-expansion of auricular AVMs after treatment. Among the 21 patients with parotid AVMs (Table 3), the majority underwent surgical excision (8 patients) and embolization (5 patients), and embolization with sclerotherapy (4 patients), while a few patients underwent embolization followed by excision (3 patients), and only 1 had sclerotherapy [5,22–27]. Although no recurrence was detected in any of the AVM cases, there was incomplete involution in 3 cases (60%) of parotid AVMs following embolization [23].
PATIENT OUTCOMES:
Recurrence and re-expansion of AVMs following embolization have been described in other extracranial AVMs within 5 years of treatment [3]. This is because the AVM was not removed and perhaps partially occluded following embolization [3]. Embolization can effectively reduce the size of the AVM by slowing its expansion and reducing blood loss during AVM excision. Postembolization ischemia subsequently can lead to angiogenesis and collateralization [3]. This is consistent with the natural cause of progression and re-expansion of AVM following treatment due to collateralization, dilation of vessels, and angiogenesis [3].
According to some authors, favorable long-term outcomes can be achieved by AVM resection with or without preoperative embolization [3]. Some authors believe that AVM recurrence can be stimulated by treatment, as both surgery and embolization can cause local tissue trauma, producing a pro-angiogenic milieu that incites AVM expansion [8]. These treatment modalities resulted in local tissue hypoxia and increased the release of hypoxia-inducible factor-1α, MMP-2, and MMP-9 from platelets, neutrophils, and macrophages [38]. Furthermore, interventions result in a reduction of the antiangiogenic tissue inhibitor of MMP [38]. Other authors advocate free-tissue transfer reconstruction following AVM resection to minimize the incidence of recurrence by reducing local tissue hypoxia [39].
In our patient’s case, endovascular treatment was used to decrease the vascularity of the AVM. Surgical excision of the AVM followed by free-tissue transfer reconstruction was performed 24 h later, with an excellent outcome. To the best of our knowledge, this is the second case reported in the literature of a high-flow parotid and auricular AVM successfully treated by the aforementioned approach [5].
Conclusions
Management of these AVMs can be challenging and it is important to understand the natural history of the lesion. The pathophysiology and the natural progression, as well as the re-expansion of AVMs following treatment, involve collateralization, dilation of vessels and angiogenesis. Treatment requires a multidisciplinary team including physicians, surgeons, anesthetists, and diagnostic and interventional neuroradiologists. Diagnostic imaging is essential to define the AVMs’ vascular anatomy, regions of involvement, and flow characteristics. Management of parotid and auricular AVMs often depends on the Schobinger stage and the flow rates of the lesion. Although total surgical resection is the criterion standard for these AVMs, endovascular embolization is an alternative treatment that can be used as an adjunct to surgery. Furthermore, perioperative embolization can decrease the vascularity of the lesion and effectively reduce blood loss during AVM surgery.
Figures
References:
1.. Wassef M, Blei F, Adams D, Vascular anomalies classification: Recommendations from the International Society for the Study of Vascular Anomalies: Pediatrics, 2015; 136(1); e203-14
2.. Kohout MP, Hansen M, Pribaz JJ, Mulliken JB, Arteriovenous malformations of the head and neck: Natural history and management: Plast Reconstr Surg, 1998; 102; 643-54
3.. Liu AS, Mulliken JB, Zurakowski D, Extracranial arteriovenous malformations: Natural progression and recurrence after treatment: Plast Reconstr Surg, 2010; 125(4); 1185-94
4.. Achache M, Fakhry N, Varoquaux A, Management of vascular malformations of the parotid area: Eur Ann Otorhinolaryngol Head Neck Dis, 2013; 130(2); 55-60
5.. Anesti K, Moaveni Z, Wu HY, Management of extensive intraparotid vascular malformation: A case report: Plast Aesthet Res, 2014; 1; 33-36
6.. Ramadass T, Sridhar K, Krishnan G, Arteriovenous malformation with auricular hypertrophy: Indian J Otolaryngol Head Neck Surg, 2000; 52; 307-9
7.. Pham TH, Wong BJ, Allison G, A large arteriovenous malformation of the external ear in an adult: Report of a case and approach to management: Laryngoscope, 2001; 111; 1390-94
8.. Wu JK, Bisdorff A, Gelbert F, Auricular arteriovenous malformation: Evaluation, management, and outcome: Plast Reconstr Surg, 2005; 115; 985-95
9.. Meher R, Varshney S, Pant HC, Arteriovenous malformation related to the pinna: Hong Kong Med J, 2008; 14; 157-59
10.. Saxena SK, Gopalakrishnan S, Megalamani SB, Arteriovenous malformation of the external ear: Indian J Otolaryngol Head Neck Surg, 2008; 60; 177-78
11.. Woo HJ, Sing SY, Kim YD, Bai CH, Arteriovenous malformation of the external ear: A case report: Auris Nasus Larynx, 2008; 35(4); 556-58
12.. Whitty LA, Murray JD, Null WE, An arteriovenous malformation of the external ear in the pediatric population: A case report and review of the literature: Can J Plast Surg, 2009; 17; e45-47
13.. Zheng LZ, Fan XD, Zheng JW, Su LX, Ethanol embolization of auricular arteriovenous malformations: preliminary results of 17 cases: Am J Neuroradiol, 2009; 30(9); 1679-84
14.. Jin YB, Lin XX, Chen H, Auricular arteriovenous malformations: Potential success of superselective ethanol embolotherapy: J Vasc Interv Radiol, 2009; 20(6); 736-43
15.. Prasad KC, Prasad SC, Shahul S, Spontaneous arteriovenous malformation of the ear: Indian J Otolaryngol Head Neck Surg, 2011; 63(Suppl. 1); 19-22
16.. Goal A, Arteriovenous malformation pinna: Review of literature: Otorhinolaryngology Clinics: An International Journal, 2011; 3(2); 75-78
17.. Meena BK, Meena S, Gupta A, A rare case of arteriovenous malformation of the pinna and review of the literature: Journal of Medical Science and Clinical Research, 2013; 1(2); 107-11
18.. Dixit SG, Abnormal vessel of the ear associated with congenital arteriovenous malformation in the postauricular region: Indian J Surg, 2013; 75(4); 334-35
19.. In ’t Veld M, Willems PW, Absence of skin discoloration after transarterial embolization of a subcutaneous auricular arteriovenous malformation with PHIL: Interv Neuroradiol, 2016; 22(5); 606-10
20.. Kim SH, Han SH, Song Y, Arteriovenous malformation of the external ear: A clinical assessment with a scoping review of the literature: Braz J Otorhinolaryngol, 2017; 83(6); 683-90
21.. Ishikawa K, Fujita M, Sasaki S, Auricular arteriovenous malformation with macrotia treated with transcatheter arterial embolization, polidocanol foam sclerotherapy and subsequent otoplasty following resection: J Craniofac Surg, 2021; 32(5); e489-90
22.. Hamdan AL, Hadi U, Moukarbel RV, Arteriovenous malformation of the parotid gland: Case report and review of the literature: Oto-Rhino-Laryngologia Nova, 2001; 11(3–4); 214-17
23.. Chen WL, Ye JT, Xu LF, A multidisciplinary approach to treating maxillofacial arteriovenous malformations in children: Oral Surg Oral Med Oral Pathol Oral Radiol Endod, 2009; 108; 41-47
24.. Shailaja SR, Manika , Manjula M, Kumar LV, Arteriovenous malformation of the mandible and parotid gland: Dentomaxillofac Radiol, 2012; 41(7); 609-14
25.. Bhatia C, Dalal S, Sattibabu V, Beniwal JP, Vascular malformation of the parotid gland: A rare case report: Int Surg J, 2017; 4; 2081-83
26.. John H, Padmashree S, Pandeshwar P, Innus S, Arteriovenous malformation of the parotid gland: diagnostic perspective – A case report: Indian J Dent Res, 2020; 31(1); 164-66
27.. Gupta M, Nijhawan VS, Kaur C, Kaur S, Gupta A, The rare cases of parotid gland arteriovenous malformations: Case Rep Otolaryngol, 2021; 2021; 6072155
28.. Yoshida K, Oishi H, Endovascular treatment of a patient with arteriovenous malformation in the parotid region: Ann Vasc Med Res, 2016; 3(3); 1036
29.. Gobin YP, Garcia de la Fuente JA, Herbreteau D, Endovascular treatment of external carotid-jugular fistulae in the parotid region: Neurosurgery, 1993; 33; 812-16
30.. Friedlander RM, Clinical practice: Arteriovenous malformations of the brain: N Engl J Med, 2007; 356; 2704-12
31.. Redondo P, Martinez-Cuesta A, Quetglas EG, Idoate M, Active angiogenesis in an extensive arteriovenous vascular malformation: A possible therapeutic target?: Arch Dermatol, 2007; 143; 1043-45
32.. Jabbour MN, Elder JB, Samuelson CG, Aberrant angiogenic characteristics of human brain arteriovenous malformation endothelial cells: Neurosurgery, 2009; 64; 139-46 ; discussion 146–48
33.. Hashimoto T, Matsumoto MM, Li JF, Lawton MT, Young WL, University of California, San Francisco, BACM Study Group. Suppression of MMP-9 by doxycycline in brain arteriovenous malformations: BMC Neurol, 2005; 5; 1
34.. Karunanyaka A, Tu J, Watling A, Storer KP, Endothelial molecular changes in a rodent model of arteriovenous malformation: J Neurosurg, 2008; 109; 1165-72
35.. Kayisli UA, Luk J, Guzeloglu-Kayisli O, Regulation of angiogenic activity of human endometrial endothelial cells in culture by ovarian steroids: J Clin Endocrinol Metab, 2004; 89; 5794-802
36.. Lissbrant IF, Hammarsten P, Lissbrant E, Ferrara N, Neutralizing VEGF bioactivity with a soluble chimeric VEGF receptor protein flt(1–3)IgG inhibits testosterone stimulated prostate growth in castrated mice: Prostate, 2004; 58; 57-65
37.. Thorey IS, Hinz B, Hoeflich A, Transgenic mice reveal novel activities of growth hormone in wound repair, angiogenesis, and myofibroblast differentiation: J Biol Chem, 2004; 279; 26674-68
38.. Kadirvel R, Dai D, Ding YH, Endovascular treatment of aneurysms: Healing mechanisms in a swine model are associated with increased expression of matrix metalloproteinases, vascular cell adhesion molecule-1, and vascular endothelial growth factor, and decreased expression of tissue inhibitors of matrix metalloproteinases: Am J Neuroradiol, 2007; 28; 849-56
39.. Hartzell LD, Stack BC, Yuen J, Free tissue reconstruction following excision of head and neck arteriovenous malformations: Arch Facial Plast Surg, 2009; 11; 171-77
Figures
Tables
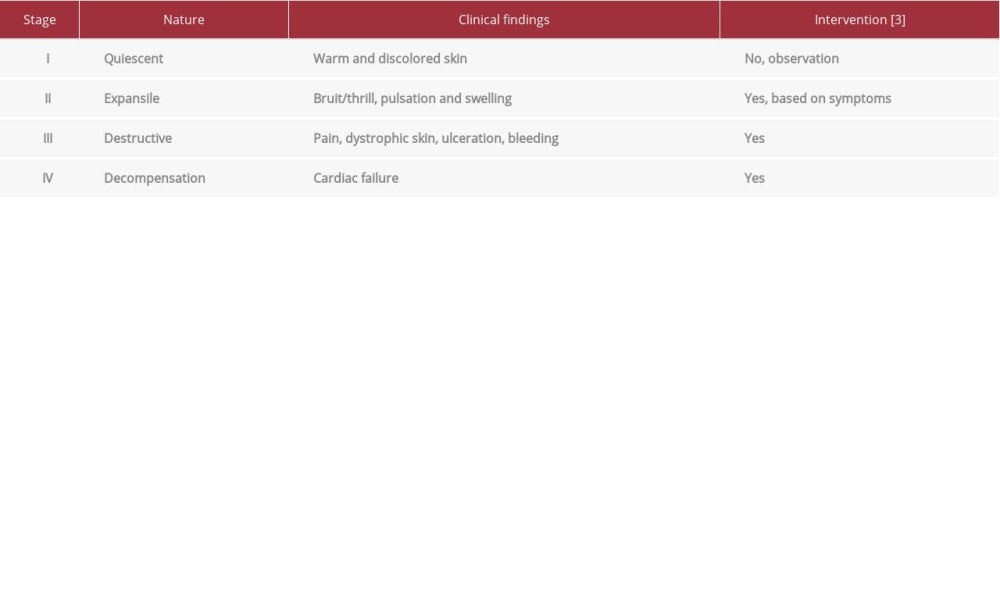 Table 1.. Schobinger staging of arteriovenous malformation.
Table 1.. Schobinger staging of arteriovenous malformation.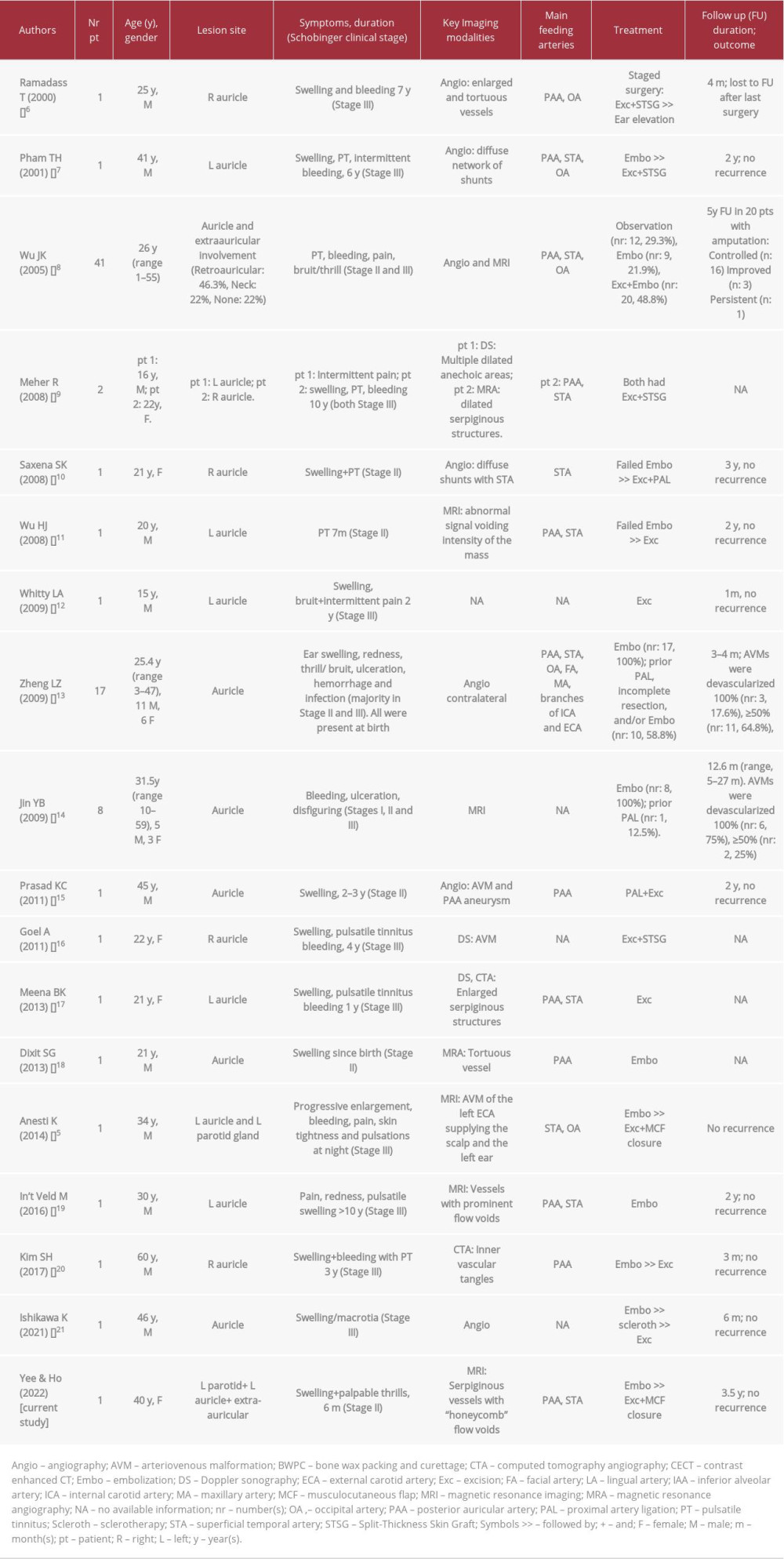 Table 2.. Summary of the reported cases of arteriovenous malformation of the auricle in the literature.
Table 2.. Summary of the reported cases of arteriovenous malformation of the auricle in the literature.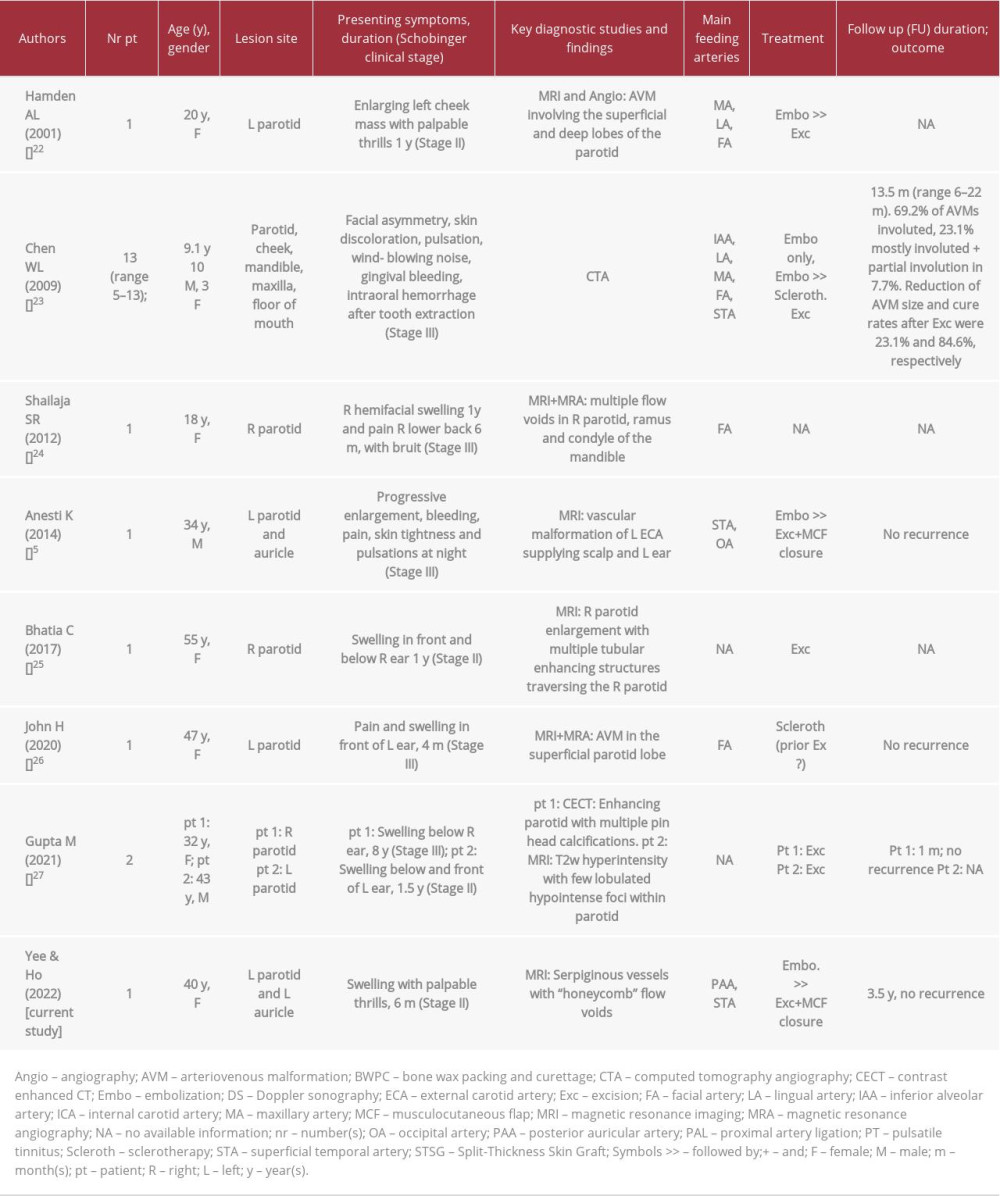 Table 3.. Summary of the reported cases of arteriovenous malformation of the parotid gland in the literature.
Table 3.. Summary of the reported cases of arteriovenous malformation of the parotid gland in the literature. Table 1.. Schobinger staging of arteriovenous malformation.
Table 1.. Schobinger staging of arteriovenous malformation. Table 2.. Summary of the reported cases of arteriovenous malformation of the auricle in the literature.
Table 2.. Summary of the reported cases of arteriovenous malformation of the auricle in the literature. Table 3.. Summary of the reported cases of arteriovenous malformation of the parotid gland in the literature.
Table 3.. Summary of the reported cases of arteriovenous malformation of the parotid gland in the literature. In Press
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.949976
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950290
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950607
Case report 
Am J Case Rep In Press; DOI: 10.12659/AJCR.950985
Most Viewed Current Articles
07 Dec 2021 : Case report  17,691,734
17,691,734
DOI :10.12659/AJCR.934347
Am J Case Rep 2021; 22:e934347
06 Dec 2021 : Case report  164,491
164,491
DOI :10.12659/AJCR.934406
Am J Case Rep 2021; 22:e934406
21 Jun 2024 : Case report  113,090
113,090
DOI :10.12659/AJCR.944371
Am J Case Rep 2024; 25:e944371
07 Mar 2024 : Case report  59,175
59,175
DOI :10.12659/AJCR.943133
Am J Case Rep 2024; 25:e943133








